Author Affiliations
Abstract
Trench foot, a non-freezing cold injury historically recognized in World War I, continues to affect vulnerable populations exposed to prolonged cold and wet environments. It is characterized by vascular and neuropathic damage that can progress to infection, necrosis, and amputation if not promptly addressed. Racial disparities have been reported, with Black and African-Caribbean individuals demonstrating a significantly higher risk of cold-related injuries in both military and civilian settings. We present a case of a 51-year-old African American male who developed bilateral trench foot after wearing wet socks and boots for several days and subsequently soaking his feet in warm water with salt. Despite early initiation of broad-spectrum antibiotics and wound care, his condition progressed rapidly, with necrosis and foul-smelling gangrene evident by day 9 of hospitalization. Imaging revealed soft tissue emphysema consistent with advanced infection, necessitating bilateral guillotine amputations to prevent systemic sepsis. This case highlights the unpredictable course of trench foot even under medical management and underscores the importance of early recognition, prevention, and timely surgical intervention. It also emphasizes the need for targeted public health strategies in high-risk populations, including individuals facing housing insecurity and racial groups disproportionately affected by cold injuries.
Keywords
Trench foot, Amputation, Gas gangrene, Cold exposure, Foot injury, Military personnel.
Introduction
Trench foot, a severe non-freezing cold injury (NFCI), was first widely recognized among soldiers during World War I. Prolonged exposure to cold, wet, and unsanitary conditions in the trenches led to significant foot injuries, often resulting in infection, gangrene, and amputations. Since then, trench foot has remained a concern in military and civilian populations exposed to extreme environmental conditions. Historically, inadequate footwear, prolonged immobility, and unsanitary conditions have been major contributors to its development.
The incidence of trench foot and related cold injuries varies across different populations. Research indicates that certain demographic groups, particularly Black soldiers, may be disproportionately affected. A study on United Kingdom (UK) service personnel found that African-Caribbean ethnicity was a statistically significant risk factor for NFCIs, with other contributing factors including shorter service duration and exposure to static duties in cold environments.[1] Similarly, data from the United States (U.S) military suggest that Black service members experience cold injuries, including frostbite and trench foot, at more than twice the rate of their White counterparts. A retrospective analysis of British Army personnel further supports these findings, revealing that African American soldiers had a 30-fold increased risk of peripheral cold injury compared to Caucasians, with more severe cases reported in this population.[2]
Beyond military settings, urban populations, particularly those with economic disadvantages, also face an elevated risk of cold-weather injuries. A study from Boston Medical Center found that 44% of cold-weather injury cases occurred in African Americans, highlighting racial disparities in environmental health risks for cold-weather injuries in urban populations from 2005 to 2015. These findings underscore the importance of targeted prevention efforts, especially for vulnerable populations exposed to extreme weather conditions.
Case Presentation & Management
A 51-year-old African American male presented to the emergency department (ED) with bilateral foot ulceration of the dorsum of the foot with accompanying swelling of the ankles and feet. His only past medical history was a brain tumor that he had removed with ventriculoperitoneal (VP) shunt placement when he was 3 years old. The patient explained that 2 weeks prior, he wore wet socks inside his boots for several days at a time, after getting his feet wet from shoveling snow. He would then heat up water on the stove and put Epsom salt in the water before soaking his feet with his shoes on. He stated that sometime after doing that and removing his shoes, his feet began to swell, and blisters formed. A day prior to admission, the blisters popped, exposing an erythematous dorsum with no overlying skin. He stated that his pain was 10/10 with nothing that could alleviate the pain, and he endorsed experiencing chills at that time. He was shown to have leukocytosis and a microcytic anemia. Infectious disease and dermatology were consulted, and peripheral blood cultures were taken. Bilateral foot x-rays were taken, showing only soft tissue swelling. With the nature of his presentation, he was treated for cellulitis and was started on empiric antibiotic coverage with linezolid 600 mg q12 and cefepime 2g q8.
The wounds were wrapped with betadine, petroleum dressing, kerlix, and Coban wrap and topical clotrimazole. He was having a relatively stable hospital course with a down-trending white blood cell (WBC) count and negative blood cultures. A bilateral lower extremity computed tomography (CT) with and without contrast was obtained, showing bilateral soft tissue emphysema and phalangeal and multi-digit interosseous emphysema consistent with osteomyelitis. Once these results came back, the patient started on clindamycin. On day 9 of his hospital stay (Figure 1), his feet began to look gangrenous, with black discoloration of toes and on all surfaces of bilateral feet, stopping at the mid ankle and an accompanying foul smell. Also, the sensation in his feet was becoming more diminished. At this time, vascular surgery was consulted for concern of trench foot. After surgical evaluation, it was determined that his condition would best benefit from bilateral guillotine amputation at the ankle. A few days later, that procedure was performed to prevent sepsis, especially considering his past medical history.
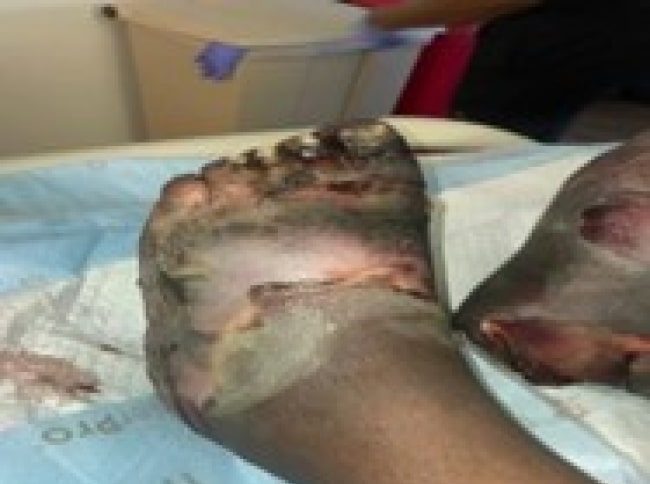
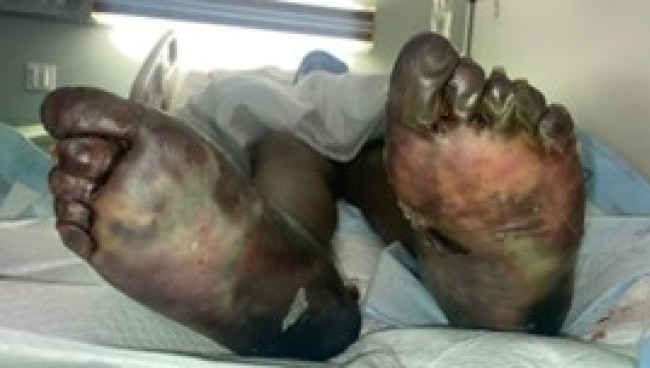
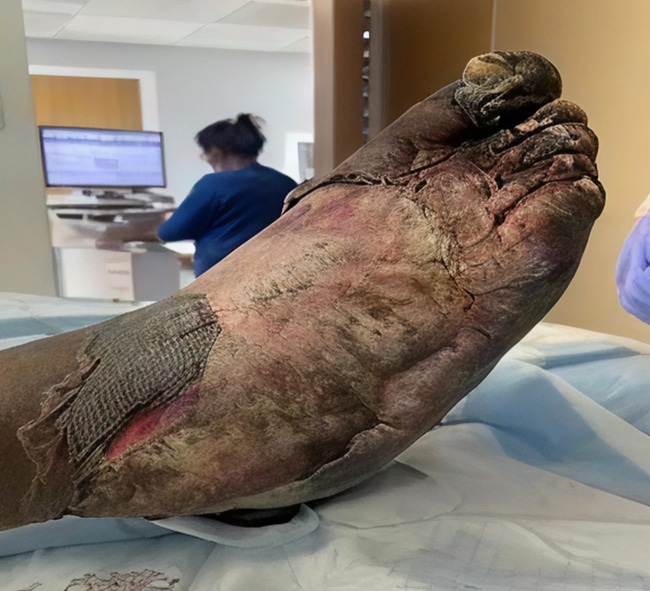
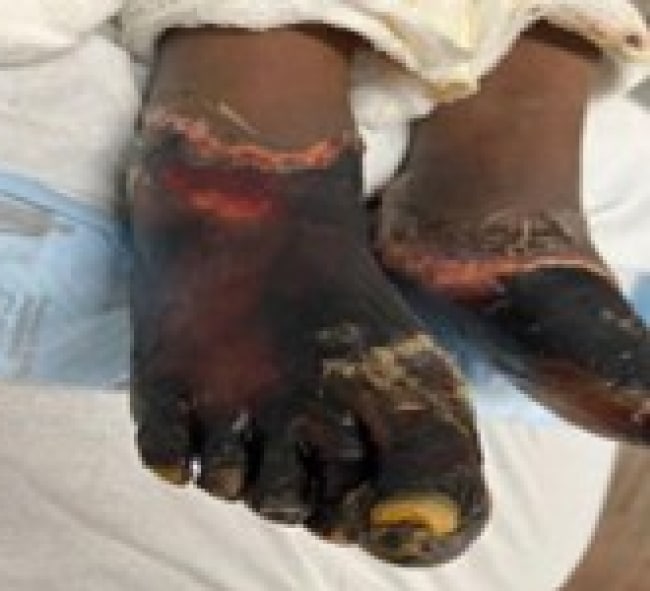
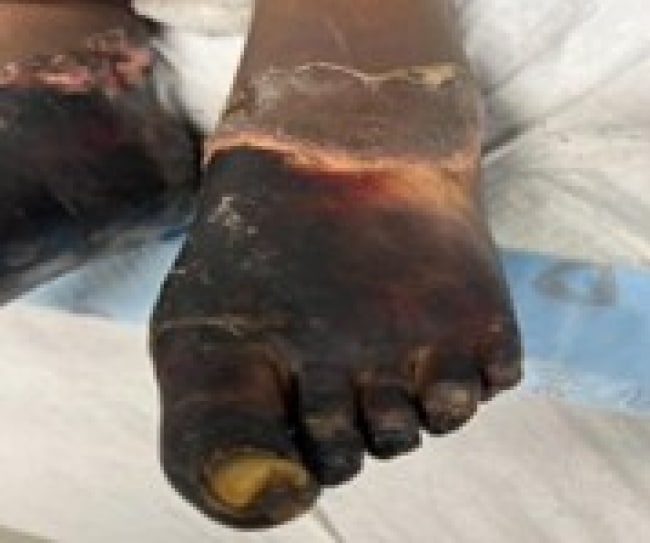
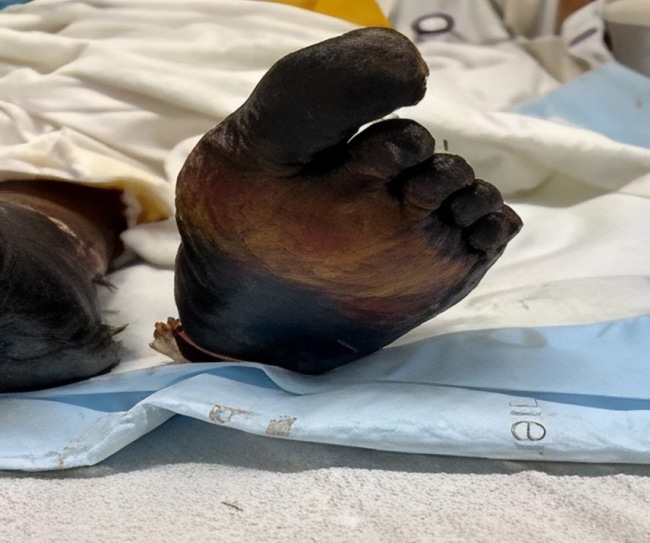
Figure 1: Bilateral foot discoloration progressing to black necrosis on day 9 of admission
Discussion
The pathophysiology of trench foot involves an interconnection of vascular and neuropathic mechanisms that combine to produce tissue damage and inflammation. Unlike frostbite, trench feet can occur without freezing temperatures. The feet can be affected in temperatures up to 16 °C (60 °F), and the disease can develop in as little as 10 to 14 hours.[3] Initially, as in our patient, exposure to a cold and wet environment produces vasoconstriction, which greatly reduces blood flow to the extremities. This is a protective mechanism that helps maintain the core body temperature, but with prolonged exposure, it can lead to tissue hypoxia and ischemia. In the setting of cold exposure, vascular changes resulting in poor blood flow can result in the feet becoming erythematous or cyanotic. In later stages, as the extremity is rewarmed, hyperesthesia is often noted.[4] This is also true in our patient case, as he noticed swelling and blister formation following heating his feet. Prolonged ischemia results in endothelial damage and increased vascular permeability, leading to edema at the site, which further compromises blood flow to the site of injury. This is also known as the hyperemic phase of trench foot, which is characterized by a paradoxical increase in blood flow that exacerbates tissue damage and inflammation. These ischemic changes cause damage to myelinated and unmyelinated nerve fibers, leading to sensory and motor deficits. One study suggests that an increase in blood vessels following tissue ischemia/hypoxia could be associated with disproportionate and abnormal nerve fibers (irritable nociceptors) and may lead to NFCI as “painful vaso-neuropathy.[5] Clinical and histological studies have shown trench foot can cause damage to large and small diameter nerves, with deficits in pinprick and thermal thresholds. Immunohistochemistry has demonstrated decreased intraepidermal nerve fiber density and increased markers of nerve regeneration and vascularity, further indicating ongoing nerve damage and repair.
The diagnosis of trench foot is entirely clinical. A good history and physical exam should allow a clinician to differentiate trench foot from frostbite, cellulitis, and other localized processes because it greatly affects the management. Inflammatory markers such as a C-reactive protein (CRP) or erythrocyte sedimentation rate might prove helpful, as will a radiograph or bone scan if underlying osteomyelitis is suspected.
The best treatment for trench foot is prevention. By keeping the feet warm, dry, and clean, trench feet can be avoided. Historically, regular foot inspections were found to decrease the incidence of the disease. The soldiers were paired up and were instructed to watch the feet of their partner. It was found that a soldier was more likely to remove his boots and dry his socks and feet if he was reminded to do so by his fellow soldier. Whale oil was also provided to the soldiers to rub on their feet after they were dry to help prevent trench foot.[6]
Current treatment recommendations are with slow passive rewarming of the affected extremity with adequate pain control with amitriptyline or other modalities for neuropathic pain.[7] It is important to assess for signs of hypothermia and to remove the affected extremity from any inciting environmental causes. Soft tissue skin infections, such as cellulitis or gangrene, are possible in later stages of presentation and should be managed with appropriate antibiotics or antifungal treatments. Subacute or chronic neuropathic pain is more common and can be managed with various modalities to treat neuropathic pain. In rare circumstances and if not managed/treated appropriately, permanent sensory changes may be seen, and amputation may be required. However, once the disease progressed to a severe case, the mainstay of treatment was surgical, like the treatment of gangrene. Many times, the patient ended up with an amputation.[8] This is what happened with our patient: he had severe pain and infection, which was evident both clinically and by X-ray. He was started on linezolid 600 mg q12 and cefepime 2g q8 empirically at the same time he was getting wound care management. It was wrapped with betadine, petroleum dressing, kerlix, and Coban wrap and topical clotrimazole.
Prevention: The prevention strategies for trench feet primarily focus on maintaining good foot hygiene, dryness, and circulation. Regularly changing damp or wet socks, wearing moisture-wicking socks and insulated footwear, avoiding tight shoes, and maintaining adequate foot ventilation are essential preventive measures. Waterproof but breathable boots help prevent prolonged moisture exposure, while rotating footwear and applying drying agents, such as foot powders, further help to reduce risk. Public health initiatives that provide shelter, dry socks, and shoes are also essential in prevention, particularly in populations affected by home insecurity. Additionally, educating at-risk populations and raising awareness of early signs and symptoms of trench foot, such as pain, numbness/tingling, and discoloration, helps to ensure that timely medical intervention can occur, mitigating the risk of severe tissue damage and other associated complications.
Conclusion
This case underscores the unpredictable and potentially severe progression of trench foot, highlighting the necessity for early recognition and intervention. Despite initial broad-spectrum antibiotic therapy, our patient experienced rapid deterioration, leading to bilateral guillotine amputations. This outcome shows the importance of timely surgical intervention in preventing life-threatening sepsis. Furthermore, the observed racial disparities in cold injury incidence call for targeted prevention strategies and heightened awareness within vulnerable populations. Enhanced education on modern causes and preventative measures is essential to mitigate severe complications associated with trench foot.
References
- Kuht JA, Woods D, Hollis S. Case series of non-freezing cold injury: epidemiology and risk factors. J R Army Med Corps. 2019;165(6):400-404. doi:10.1136/jramc-2018-000992
PubMed | Crossref | Google Scholar - Mistry K, Ondhia C, Levell NJ, et al. A review of trench foot: a disease of the past in the present. Clin Exp Dermatol. 2020;45(1):10-14. doi:10.1111/ced.14031
PubMed | Crossref | Google Scholar - Zafren K. Nonfreezing cold injury (trench foot). Int J Environ Res Public Health. 2021;18(19):10482. doi:10.3390/ijerph181910482
PubMed | Crossref | Google Scholar - Ingram BJ, Raymond TJ, et al. Recognition and treatment of freezing and nonfreezing cold injuries. Curr Sports Med Rep. 2013;12:125-130. doi:10.1249/JSR.0b013e3182877454
PubMed | Crossref | Google Scholar - Anand P, Privitera R, Yiangou Y, et al. Trench foot or non-freezing cold injury as a painful vaso-neuropathy: clinical and skin biopsy assessments. Front Neurol. 2017;8:514. doi:10.3389/fneur.2017.00514
PubMed | Crossref | Google Scholar - Bennett BL, Holcomb JB. Battlefield trauma-induced hypothermia: transitioning the preferred method of casualty rewarming. Wilderness Environ Med. 2017;28(suppl 2):S82-S89. doi:10.1016/j.wem.2017.03.010
PubMed | Crossref | Google Scholar - Imray CH, Richards P, Greeves J, Castellani JW. Nonfreezing cold-induced injuries. J R Army Med Corps. 2011;157(1):79-84. doi:10.1136/jramc-157-01-14
PubMed | Crossref | Google Scholar - Johnston AM, Singleton J. Cold feet. BMJ. 2016;354:i4584. doi:10.1136/bmj.i4584
PubMed | Crossref | Google Scholar
Acknowledgments
Not reported
Funding
This case report received no specific grant.
Author Information
Corresponding Author:
Mekdem Bisrat
Department of Internal Medicine
Howard University, Washington DC, USA
Email: mekdembisrat21@gmail.com
Co-Authors:
Ryan Mitchell, Sean Parker, Wesley Oliver, Damon Ross Jr, Davon Lee, Kamron Rashid, Jordan Young
Howard University School of Medicine, Washington DC, USA
Samrawit Zinabu, Elizabeth Beyene, Miriam Michael
Department of Internal Medicine
Howard University, Washington DC, USA
Authors Contributions
All authors contributed to the conceptualization, investigation, and data curation by acquiring and critically reviewing the selected articles. They were collectively involved in the writing, original draft preparation, and review & editing to refine the manuscript. Additionally, all authors participated in the supervision of the work, ensuring accuracy and completeness. The final manuscript was approved by all named authors for submission to the journal.
Informed Consent
Patient consent for participation and publication (including the use of clinical details and images) was obtained. All identifying information has been removed to protect patient anonymity.
Conflict of Interest Statement
The authors declare no conflict of interest.
Guarantor
None
DOI
Cite this Article
Mitchell R, Parker S, Oliver W, et al. When the Cold Takes Hold – The Devastating Progression of Severe Trench Foot. medtigo J Emerg Med. 2025;2(3):e30922312. doi:10.63096/medtigo30922312 Crossref









