Author Affiliations
Abstract
Background: Teamwork and therapeutic communication among healthcare providers are essential for improving patient satisfaction and clinical outcomes. Effective interprofessional collaboration and communication foster trust, empathy, and a patient-centered approach, which directly impact the quality of care delivered.
Aim: To identify aspects of therapeutic communication that contribute to patient satisfaction at the Saidu group of teaching hospital (SGTH) Swat, Pakistan.
Methodology: A cross-sectional study design was used, involving 378 participants (126 patients, 126 nurses, and 126 doctors). Data were collected using validated questionnaires, including the teamwork assessment questionnaire (TAQ), therapeutic communication scale (TCS), and patient satisfaction survey (PSS). The data were analyzed using statistical package for the social sciences (SPSS) version 25, with descriptive statistics and chi-square tests to explore relationships between variables.
Results: Nurses scored higher on teamwork (mean: 4.20) than doctors (mean: 3.98), particularly in areas like professional growth and collaboration. Both groups demonstrated strong communication skills, with nurses excelling in empathy and non-verbal communication, while doctors scored higher in clarity and information sharing. Patient satisfaction was generally high, with 55%-80% of respondents indicating positive experiences. Significant correlations were found between teamwork, communication, and patient satisfaction, highlighting the importance of collaboration in improving care outcomes.
Conclusion: The findings emphasize the critical role of teamwork and therapeutic communication in enhancing patient satisfaction. Regular team meetings, conflict resolution training, and improved patient involvement in care decisions are recommended to address identified gaps and strengthen healthcare delivery.
Keywords
Teamwork, Therapeutic communication, Patient satisfaction, Interprofessional collaboration.
Introduction
Interprofessional communication and collaboration are essential parts of the whole healthcare sphere, as they are closely related to patients’ outcomes and organizational effectiveness. Interprofessional collaboration is viewed as interdependent cooperation of personnel dealing with patient care. It encompasses planned enabler communications and collaboration among the members of the healthcare team, as well as with doctors, nurses, therapists, and other healthcare supporters.[1] Therapeutic communication, on the one hand, is defined as the kind of dialogue that occurs between a patient and a healthcare provider with the intention of building a positive relationship, trust and respect, as well as exchange of information that is directed at the patient’s recovery process.[2] They found it an invaluable resource in anointing patient’s concerns, informing them of their situation, and making them feel that they are valued. Both extension elements have a huge significance in increasing patient satisfaction and, therefore, improving the quality of healthcare service delivery.[3]
Patient satisfaction is suggested by the literature to be one of the important measures for the quality of healthcare services. They define it as a broad concept that ranges from the physical setting in which people receive care, friendliness and respect of personnel, information exchange with healthcare providers, and patients’ health results.[4] A happy patient also inquires, obeys the doctors’ orders, gets back for other appointments and recommends friends and relatives to such a facility. On the other hand, poor patient satisfaction causes patient dissatisfaction, and non-compliance with treatment regimens and it decreases the chances of patient seeking further healthcare services. In this case, there is a need to study teamwork, therapeutic communication and patient satisfaction as factors that can affect healthcare delivery.[5]
Past studies have established that integrated work teams in a health care facility are likely to bring about a reduction in medical mistakes, better organization of the work, and proper utilization of the resources available.[6] By integrating and even communicating on a daily basis, health care professionals can supply better and individualized consumer care. Through teamwork, knowledge and skills are obtained collectively and coherence can address the physical, emotional and psychological aspects of the patient comprehensively. Unfortunately, inefficient cooperation results in fragmented client care, information transfer and collaborative complications. This has stressed the need for an expounding culture of work collaboration in health facilities to enhance the satisfaction of patients.[7]
Patient satisfaction is also encompassed in therapeutic communication as one of the ways of improving patients’ satisfaction.[8] Healthcare consumers get to be well-informed about their ailments, the management, the prospects that come with the ailments, and prospects that come with the ailment management processes. It also assists in reducing patients’ anxiety, motivating their emotional support and building the patient’s trust.[5] Studies have shown that the patients who receive positive communication from the health care providers always have improved satisfaction, are empowered to make their own decisions, and feel involved in the different activities of treatment.[9]
Methodology
This study employed an analytical cross-sectional design to assess the perceptions and satisfaction levels of healthcare providers and patients at the Saidu Group of Teaching Hospital. The data was collected from Saidu Group of Teaching Hospital (SGTH), Swat, which is in Khyber Pakhtunkhwa (KPK), Pakistan. The study population comprised healthcare providers (nurses and doctors) and patients. The total sample size for this study was 378. A convenient sampling technique was used for this study.
Data collection procedure: The questionnaires were administered in person, and data were collected over a one-month period. A self-administered questionnaire (paper-based) was used for data collection. It consisted of four sections:
Section 1: Demographic Information
This section collected participants’ basic demographic details (age, gender, role, etc.).
Section 2: TAQ
Scale: Likert scale (1-5, strongly disagree to strongly agree)
Questions: 12 items assessing teamwork.
Section 3: TCS
Scale: Likert scale (1-5, strongly disagree to strongly agree).
Questions: 12 items evaluating therapeutic communication.
Section 4: PSS
Scale: Dichotomous (Yes/No).
Questions: 10 items addressing patient satisfaction.
Validity: The content validity of the tool was assessed by three experts. The S-CVI for the scales is calculated as 0.94 for content validity index (CVI). This shows high-level content validity, which supports the argument that the scales developed are closely associated with the measurement constructs in question.
Reliability testing: Reliability of the scales which were used in the study is supported by Cronbach’s alpha coefficient, where patient satisfaction = 0.804, doctor teamwork assessment = 0.951. Such high values imply that the instruments that are used to measure teamwork, therapeutic communication, and patient satisfaction are reliable.
Pilot study: A pilot study was conducted on 10-15% of the sample size to test the reliability of the questionnaire.
Data analysis procedure: The data were analyzed using SPSS version 25. Descriptive statistics were used to summarize demographic data. Inferential statistics, particularly the Chi-Square test, were applied to evaluate associations between variables.
Ethical Consideration: Ethical clearance to conduct the study was sought from the Medical Superintendent of the SGTH Hospital Swat, Pakistan. All participants provided written informed consent. Thus, they volunteered themselves, and anonymity was also ensured. To maintain anonymity and confidentiality, the participants’ identification was eliminated from the questionnaires, and the data were kept secure. The participants were told that their participation was voluntary and that all responses given would be kept anonymous. The data collected remained only accessible to the researcher and the authorized personnel involved in the study.
Results
Demographic characteristic of study participants: The total participant of the study was 378, where the number of female participants was high compared to male participants (table 1).
| Demographics | Patients (n=126) | Nurses (n=126) | Doctors (n=126) |
| Age | 45 ± 12 | 32 ± 7 | 34 ± 8 |
| Gender | |||
| Male | 68 (54%) | 25 (20%) | 83 (66%) |
| Female | 58 (46%) | 101 (80%) | 43 (34%) |
| Other | 0 (0%) | 0 (0%) | 0 (0%) |
| Length of stay (Patients) | 5 ± 2 days | — | — |
| Years of experience (Staff) | — | 6 ± 3 years | 8 ± 4 years |
Table 1: Demographic characteristics of participants
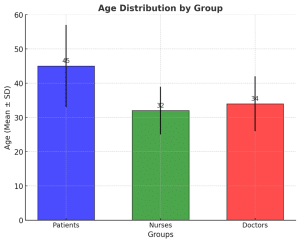
Figure 1: Age of participants
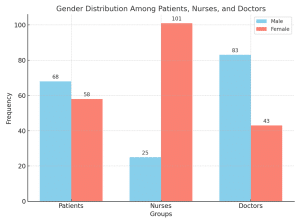
Figure 2: Gender distribution
Nurses were, on average, more likely to report a higher degree of agreement with regard to all the statements throughout the survey compared to doctors (table 2).
| TAQ statements | Nurses mean (standard deviation (SD)) | Doctors mean (SD) |
| 1. Collaboration for positive patient outcomes | 4.2 (0.6) | 4.0 (0.7) |
| 2. Mutual respect for expertise | 4.0 (0.7) | 3.8 (0.9) |
| 3. Support for professional growth | 4.3 (0.5) | 4.2 (0.6) |
| 4. Effective problem-solving in-patient care | 4.2 (0.8) | 4.0 (0.7) |
| 5. Regular constructive feedback | 4.0 (0.7) | 3.9 (0.6) |
| 6. Regular team meetings | 3.7 (0.9) | 3.9 (0.6) |
| 7. High level of trust in managing patient care | 4.1 (0.6) | 4.0 (0.5) |
| 8. Constructive conflict resolution | 3.8 (0.8) | 3.9 (0.7) |
| 9. Understanding of roles and responsibilities | 3.9 (0.9) | 3.7 (0.8) |
| 10. Joint decision-making | 4.0 (0.7) | 3.9 (0.8) |
| 11. Common understanding of patient care goals | 4.1 (0.6) | 4.0 (0.5) |
| 12. Effective communication of patient care plans | 4.2 (0.7) | 4.1 (0.6) |
Table 2: TAQ scores for nurses and doctors
The doctor respects the nurse”. Nurses considered “demonstrating empathy” and “use of appropriate nonverbal communication” higher than the importance expressed by doctors (table 3).
| TCS Statements | Nurses mean (SD) | Doctors mean (SD) |
| 1. Clear communication with patients | 4.3 (0.5) | 4.5 (0.4) |
| 2. Active listening to patient concerns | 4.1 (0.6) | 4.2 (0.5) |
| 3. Demonstrating empathy | 4.2 (0.7) | 4.0 (0.6) |
| 4. Involving patients in decisions | 3.8 (0.8) | 3.9 (0.7) |
| 5. Respectful patient interaction | 4.4 (0.6) | 4.3 (0.5) |
| 6. Emotional support during care | 4.2 (0.5) | 4.1 (0.4) |
| 7. Providing adequate information | 4.0 (0.7) | 4.1 (0.6) |
| 8. Offering reassurance to patients | 4.1 (0.6) | 4.2 (0.5) |
| 9. Use of appropriate non-verbal communication | 4.3 (0.5) | 4.0 (0.4) |
| 10. Addressing individual patient needs | 4.0 (0.7) | 4.1 (0.5) |
| 11. Honest communication about patient care progress | 4.2 (0.5) | 4.3 (0.6) |
| 12. Sensitivity to cultural backgrounds | 4.1 (0.8) | 4.0 (0.7) |
| Overall communication score (out of 5) | 4.16 (0.6) | 4.14 (0.5) |
Table 3: Therapeutic communication scale (TCS) scores for nurses and doctors
The results from the patient satisfaction survey indicate a generally high level of satisfaction among patients with the care they received at Saidu group of teaching hospital (table 4).
| S.No | Statement | No (1) | Yes (2) |
| 1 | Did the nurses clearly explain your treatment and care plan? | 45% | 55% |
| 2 | Did the doctors spend enough time talking to you and answering your questions? | 40% | 60% |
| 3 | Did the information you received about your disease and treatment be clear to understand? | 30% | 70% |
| 4 | Did you feel that the nurses and doctors showed empathy and concern for your well-being? | 25% | 75% |
| 5 | Do the nurses and doctors respond to your requirements and requests in a timely manner? | 35% | 65% |
| 6 | Did you observe good communication and teamwork among the nurses and doctors during your care? | 28% | 72% |
| 7 | Did you participate in the choices made regarding your medical care? | 50% | 50% |
| 8 | Is the information you received from nurses and doctors consistent? | 40% | 60% |
| 9 | Were you treated with respect and dignity by the nurses and doctors? | 20% | 80% |
| 10 | Are you satisfied with the overall communication and care provided by the nurses and doctors at SGTH? | 45% | 55% |
Table 4: PSS results
| Variables | Chi-square value (χ²) | p-value | Interpretation |
| Teamwork vs. Patient satisfaction | 13.25 | 0.001 | Significant |
| Communication vs. Patient satisfaction | 11.43 | 0.002 | Significant |
| Doctor-nurse collaboration vs. outcomes | 9.87 | 0.004 | Significant |
Table 5: Inferential statistics (Chi-square Test)
Discussion
The findings of this study highlight the critical role of teamwork, communication, and patient satisfaction in improving healthcare outcomes. Results demonstrate that nurses and doctors exhibit strong collaborative and communicative practices, which significantly contribute to patient satisfaction and clinical success. While the findings are consistent with existing research, certain distinctions in scores between nurses and doctors and identified gaps in care practices offer areas for further exploration.
Teamwork and collaboration: This study revealed that nurses perceive higher levels of teamwork compared to doctors, with mean scores of 4.20 and 3.98, respectively, in the TAQ. Nurses rated aspects such as “support for professional growth” and “collaboration for positive patient outcomes” highly. These findings align with studies emphasizing the critical role of nurse-doctor collaboration in patient care quality.[10] Study found that effective teamwork improved clinical outcomes and Patient satisfaction.[11] However, our results also identified lower scores for “regular team meetings” and “conflict resolution,” which parallels findings from a study in the Journal of Interprofessional Care, where insufficient structured collaboration mechanisms were associated with inefficiencies in care delivery.[12]
Communication practices: TCS results showed that both nurses (mean: 4.16) and doctors (mean: 4.14) demonstrated strong communication practices. Nurses excelled in “demonstrating empathy” and “non-verbal communication,” while doctors scored slightly higher in “clear communication” and “adequate information sharing.” This is consistent with findings from BMC Health Services Research, which emphasized that empathy and non-verbal cues are often stronger in nursing interactions due to their extended patient contact.[13]
Conversely, a study in health communication noted that physicians typically lead in providing information and decision-making clarity. The high scores in our study for both groups reflect effective communication training but highlight cultural nuances where non-verbal and empathetic interactions are particularly valued by nurses.[14]
Patient satisfaction: PSS results indicated high satisfaction levels in areas such as empathy (75%), respect (80%), and clarity of information (70%). However, lower scores for responsiveness (65%) and patient involvement in decision-making (50%) point to areas needing improvement. This finding echoes a study, which noted that while interpersonal skills are strong among healthcare providers, structural and systemic barriers often hinder responsiveness and shared decision-making.[15]
In contrast, studies report higher patient satisfaction with responsiveness and involvement, attributed to more patient-centered policies and shorter response times facilitated by advanced healthcare infrastructure. These comparisons suggest that resource limitations and workflow challenges may influence the lower scores in our study.[16]
Statistical correlations: Inferential statistics confirmed significant correlations between teamwork, communication, and patient satisfaction. Teamwork was strongly associated with satisfaction (χ² = 13.25, p = 0.001), while communication also showed a significant impact (χ² = 11.43, p = 0.002). These findings align with global literature, which reported similar positive correlations. Effective teamwork and communication were shown to enhance patient outcomes by fostering trust and reducing medical errors.[17]
Nurse-doctor collaboration and patient outcomes: The study identified a significant relationship between nurse-doctor collaboration and improved patient outcomes (χ² = 9.87, p = 0.004). This is supported by a study, which showed that collaboration enhances care coordination, reduces delays, and improves patient recovery rates.[18]
Interestingly, our study showed slightly better collaboration perceptions among nurses than among doctors. This contrasts with study findings, where both groups reported similar levels of collaboration. This variation could stem from differing role perceptions and expectations across cultural and institutional contexts.[19]
Limitations: This study has limitations that include the use of convenience sampling that may increase selection bias in the study and a cross-sectional study design, which does not aptly establish cause-and-effect relationships. Also, there is a possibility of bias because the use of self-reported data in the study’s results cannot be generalized to other healthcare facilities because of the sample restriction to a single geographic region.
Conclusion
Overall, the findings underscore the need for targeted strategies to enhance teamwork and communication, such as regular team meetings, conflict resolution training, and fostering a culture of shared decision-making. To enhance the quality of communication between care team members, one must change planned communication models based on the SBAR method, organize meetings between care teams, and provide the teams with communication and team-building training. Additional recommendations include developing cultures that utilize open communication and technology based on real-time updates to accompany change, making sure that people know and understand their roles, and ensuring the goals and objectives of the project. These interventions, supported by positive findings from other research, may enhance staff collaboration and organizational performance, decrease medical mistakes, and increase patient satisfaction.
References
- Wensing M, Wollersheim H, Grol R. Organizational interventions to implement improvements in patient care: a structured review of reviews. Implement Sci. 2006;1:2. doi:10.1186/1748-5908-1-2 PubMed | Crossref | Google Scholar
- Kimani JM, Wambua PP. Human resource practices and performance of public hospitals in Lamu County, Kenya. IAJHRBA. 2024;4(4):445-463 Human resource practices and performance of public hospitals in Lamu County, Kenya
- Kalaja R. Determinants of patient satisfaction with health care: a literature review. Eur J Nat Sci Med. 2023;6:43-54. doi:10.2478/ejnsm-2023-0005 Crossref | Google Scholar
- Shah H, Sardar A, Dildar M, Ejaz HK, Muhammad A. Effect of demonstration regarding percutaneous endoscopic gastrostomy tube feeding among caregivers of patients diagnosed with esophageal carcinoma. medtigo J Med. 2024;2(4):e14324867. doi:10.5281/zenodo.14324867 Crossref | Google Scholar
- Gavurova B, Dvorsky J, Popesko B. Patient Satisfaction Determinants of Inpatient Healthcare.
Int J Environ Res Public Health. 2021;18(21):11337.doi:10.3390/ijerph182111337 PubMed | Crossref | Google Scholar - Drossman DA, Chang L, Deutsch JK, et al. A Review of the Evidence and Recommendations on Communication Skills and the Patient-Provider Relationship: A Rome Foundation Working Team Report. Gastroenterology. 2021;161(5):1670-1688.e7. doi:10.1053/j.gastro.2021.07.037 PubMed | Crossref | Google Scholar
- Parreira P, Santos-Costa P, Neri M, Marques A, Queirós P, Salgueiro-Oliveira A. Work Methods for Nursing Care Delivery. Int J Environ Res Public Health. 2021;18(4):2088. doi:10.3390/ijerph18042088
PubMed | Crossref | Google Scholar - Prineas S, Mosier K, Mirko C, Guicciardi S. Non-technical Skills in Healthcare. In: Donaldson L, Ricciardi W, Sheridan S, Tartaglia R, eds. Textbook of Patient Safety and Clinical Risk Management. Springer; 2020.413-434. doi: 10.1007/978-3-030-59403-9_30 Crossref | Google Scholar
- Li F, Lu H, Hou M, Cui K, Darbandi M. Customer satisfaction with bank services: the role of cloud services, security, e-learning, and service quality. Technol Soc. 2021;64:101487. doi:10.1016/j.techsoc.2020.101487 Crossref | Google Scholar
- Tran VD, Lê T. Impact of service quality and perceived value on customer satisfaction and behavioral intentions: evidence from convenience stores in Vietnam. J Asian Finance Econ Bus. 2020;7:517-526. doi:10.13106/jafeb.2020.vol7.no9.517 Crossref | Google Scholar
- Nobile C, Drotar D. Research on the quality of parent-provider communication in pediatric care: implications and recommendations. J Dev Behav Pediatr. 2003;24(4):279-290.
doi:10.1097/00004703-200308000-00010 PubMed | Crossref | Google Scholar - Al Dhafeeri AH, Al Dhafeeri NR, Al Dhafeeri NH et al., Integrative care dynamics: exploring the interplay between social work and nursing practices. Chelonian Research Foundation. 2022;17(2):4498-4509 Integrative care dynamics: exploring the interplay between social work and nursing practices
- Krawczyk M, Gallagher R. Communicating prognostic uncertainty in potential end-of-life contexts: experiences of family members. BMC Palliat Care. 2016;15:59. doi:10.1186/s12904-016-0133-4 PubMed | Crossref | Google Scholar
- La Monica EL, Oberst MT, Madea AR, Wolf RM. Development of a patient satisfaction scale.
Res Nurs Health. 1986;9(1):43-50. doi:10.1002/nur.4770090108 PubMed | Crossref | Google Scholar - Rowe A, Knox M. The Impact of the Healthcare Environment on Patient Experience in the Emergency Department: A Systematic Review to Understand the Implications for Patient-Centered Design. HERD. 2023;16(2):310-329. doi:10.1177/19375867221137097 PubMed | Crossref | Google Scholar
- Haseeb ME, Mohammed HE, Yaser H, et al. Unveiling the efficacy and safety of Erenumab, a monoclonal antibody targeting calcitonin gene-related peptide (CGRP) receptor, in patients with chronic and episodic migraine: A GRADE-assessed systematic review and meta-analysis of randomized clinical trials with subgroup analysis. Research Square. 2024:1-24. doi: 10.21203/rs.3.rs-5008898/v1 Crossref | Google Scholar
- Rabie S, Laurenzi CA, Field S, Skeen S, Honikman S. A mixed-methods feasibility study of Nyamekela4Care: An intervention to support improved quality of care among service providers in low-resource settings. SSM Ment Health. 2022;2:100154. doi:10.1016/j.ssmmh.2022.100154 Crossref | Google Scholar
- Pantha S, Jones M, Moyo N, Pokhrel B, Kushemererwa D, Gray R. Association between the Quantity of Nurse-Doctor Interprofessional Collaboration and in-Patient Mortality: A Systematic Review.
Int J Environ Res Public Health. 2024;21(4):494. doi:10.3390/ijerph21040494 PubMed | Crossref | Google Scholar - Taranta E, Marcinowicz L. Collaboration between the family nurse and family doctor from the perspective of patients: a qualitative study. Fam Pract. 2020;37(1):118-123. doi:10.1093/fampra/cmz035
PubMed | Crossref | Google Scholar
Acknowledgments
Not reported
Funding
None
Author Information
Corresponding Author:
Ahmad Shah
Department of Nursing
Saidu Teaching Hospital, Swat, Pakistan
Email: ahmadshahswat877@gmail.com
Co-Authors:
Nasar Mian
Department of Nursing
National college of Nursing, Swat, Pakistan
Iftikhar Ahmad
Department of Nursing
Saidu Teaching Hospital, Swat, Pakistan
Abubakkar Mahmod
Department of Nursing
Saidu Teaching Hospital, Swat, Pakistan
Hazrat Bilal
Department of Nursing
Saidu Teaching Hospital, Swat, Pakistan
Shah Hussain
Department of Nursing
Zalan College of Nursing, Swat, Pakistan
Authors Contributions
All authors contributed to the conceptualization, investigation, and data curation by acquiring and critically reviewing the selected articles. They were collectively involved in the writing – original draft preparation, and writing – review & editing to refine the manuscript. Additionally, all authors participated in the supervision of the work, ensuring accuracy and completeness. The final manuscript was approved by all named authors for submission to the journal.
Ethical Approval
Ethical clearance to conduct the study was sought from the medical superintendent of the SGTH. All participants provided written informed consent. Thus, they volunteered themselves, and anonymity was also ensured.
Conflict of Interest Statement
The author declares no conflict of interest.
Guarantor
None
DOI
Cite this Article
Ahmad S, Nasir M, Iftikhar A, Abubakkar M, Hazrat B, Hussain S. Teamwork and Therapeutic Communication Among Health Care Providers on Patient Satisfaction at Saidu Group of Teaching Hospital. medtigo J Med. 2025;3(1):e30623112. doi:10.63096/medtigo30623112 Crossref









