Author Affiliations
Abstract
Background: Postoperative delirium (POD) commonly affects elderly patients (>65 years), leading to longer hospital stays, increased mortality, and higher healthcare costs. While surgical nurses play a vital role in POD prevention through risk assessment, non-pharmacological strategies, and environmental improvements, their efforts are often limited by inadequate training and resources.
Aim: This study aimed to assess surgical nurses’ knowledge, attitudes, and practices regarding POD prevention in elderly patients and examine the relationship between protocol adherence and POD incidence.
Methodology: A descriptive quantitative study was conducted at a tertiary hospital in Swat. Sixty surgical nurses completed structured questionnaires, and medical records of 100 elderly surgical patients were reviewed using the confusion assessment method (CAM). Data were analyzed using the Statistical Package for the Social Sciences (SPSS) v27, including descriptive statistics and chi-square tests.
Results: Ninety percent of nurses recognized sedation reduction as helpful, and 85% supported early mobilization. However, only 60% routinely implemented cognitive orientation strategies. Although 92% had positive attitudes, only 40% felt adequately trained. The overall POD incidence was 20%. Notably, nurses with high adherence to preventive protocols had significantly lower POD rates (only 8%).
Conclusion: Surgical nurses possess good knowledge and strong motivation to prevent POD, but gaps in consistent practice remain. Strengthening training, especially in cognitive orientation and reinforcing adherence to evidence-based protocols, is essential for improving outcomes in elderly postoperative patients.
Keywords
Postoperative delirium, Surgical nurses, Elderly patients, Delirium prevention, Nursing practices.
Introduction
After surgery, elderly patients are especially likely to have POD, even though it is common and often misunderstood.[1] It refers to a quick disturbance in a person’s awareness, attention, thinking, and perception, usually seen shortly after surgery. Surgical nurses care for patients before, during, and after surgical procedures by carefully watching for and dealing with complications.[2] Most elderly patients, who are distinguished by their age (65 or older), often have weaker body function and, thus, face greater chances of adverse outcomes.[3] In these conditions, prevention focuses on taking steps ahead of surgery to lessen the chances or severity of POD by interventions, teaching patients, and organizing the environment.[4]
How often POD happens depends on what surgery is done and who receives it, but it is most common among elderly people. Between 10% and 50% of elderly patients have delirium after having significant surgery.[5] The presence of traumatic brain injury (TBI) in such surgeries as orthopedic, cardiac, and abdominal can lead to anesthesia-related deaths in more than 60% of patients. Having POD is linked to a longer stay in the hospital, higher total healthcare costs, a greater possibility of impacting cognitive health, and higher rates of illness and death. POD does a lot of damage, but it is either mistaken for dementia, anxiety, or confusion due to pain, making the prevention of POD essential in surgery.[6]
Regular contact with patients allows surgical nurses to spot cognitive changes early and use preventive steps before any real concern arises. They must complete postoperative monitoring, pain relief, early mobilization, medication administration, teach patients, talk with families, and communicate that these activities include many ways to avoid delirium after surgeries.[7] Surgical nurses help create a calm and well-organized environment and ensure that patients are well-fed and hydrated, which reduces the risk of cognitive disturbances.[8]
Delirium in this group is caused by several factors that can sometimes be controlled and others that cannot be changed.[9] Age, comorbid conditions, if dementia already exists, and any sensory impairments cannot be changed, but factors that can be improved include drugs, inability to move, poor sleep, and health issues involving infection and hydration.[10] Surgical nurses may offer suggestions, for example, by keeping psychoactive drug needs low, promoting early movement, and ensuring a patient gets enough rest and good pain management. The importance of physicians increases tremendously in places where formal geriatric care is hard to get.[11]
Though physicians are primarily involved with diagnosing and treating patients, nurses can more easily see the first signs of delirium by changes in behavior.[12] Early steps such as proper orientation, often assessment, prevention of restraints, and motivating families to be involved, can reduce the occurrence and duration of POD.[13] Experts agree that nurse-led interventions not involving drugs are very effective for delirium prevention, though these methods are not widely used because of a lack of knowledge, proper training, and hospital policies.[14]
According to the literature, both practice and policy fail to address several aspects linked to the role nurses have in preventing delirium. Several studies researching medicines or physician guidelines exist, but many fewer deal with structured, nurse-led protocols.[15] Besides, not much data exists from these regions, where both the number of older surgical patients is going up, and nurses often lack focused geriatric training.[16] This points out that there needs to be more in-depth research about the work, obstacles, and opportunities of surgical nurses when preventing POD in these circumstances.[17]
The study aims to find out the current information, work, and positions surgical nurses have when it comes to delaying POD in elderly people. The study works to highlight strengths, gaps, and challenges, which helps provide evidence for policy, training, and nursing guidelines. Emphasizing how nursing care can prevent problems can result in better overall outcomes for patients, fewer complications, and better use of medical resources.
Methodology
The role of surgical nurses in preventing POD among elderly patients was examined in this study by using a cross-sectional descriptive quantitative approach. The study was conducted at a tertiary care hospital in Swat. The population consisted of nurses working in the general surgery and orthopedic units and adults 65 years of age or older admitted for elective or emergency procedures within the study period. To achieve this objective, 60 surgical nurses with at least a year of experience, plus 100 elderly patients who fit the study criteria, were recruited.
Data collection: We gathered information from nurses using a questionnaire with questions about their knowledge, attitudes, and delirium prevention practices. Before launching the questionnaire, it was developed using expert research and was validated (Content validity index (CVI) 0.88, and Cronbach alpha 0.82) by experts in surgical nursing and geriatric care. The medical records of all patients were reviewed to look for instances of POD diagnosed with the CAM.
Data analysis: Data analysis was done in SPSS version 27, and statistics such as frequencies, percentages, means, and standard deviations were calculated. Chi-square was used to explore the relationship between nurses’ preventive measures and the likelihood of POD in patients.
Results
Demographic characteristics: In the study, 60 surgical nurses took part, and 63.3% were female, while the remaining 36.7% were male. Many nurses were in the age category of 35–44 (46.7%), compared to the 45+ group (28.3%). There were 41.7% who had worked between 6 and 10 years, and 33.3% who had at least 1–5 years. This shows that most nurses currently working are in the middle or later stages of their careers (Table 1).
| Characteristic | Frequency (n) | Percentage (%) |
| Gender | ||
| Male | 22 | 36.7 |
| Female | 38 | 63.3 |
| Age (years) | ||
| 25–34 | 15 | 25.0 |
| 35–44 | 28 | 46.7 |
| 45 and above | 17 | 28.3 |
| Years of experience | ||
| 1–5 years | 20 | 33.3 |
| 6–10 years | 25 | 41.7 |
| More than 10 years | 15 | 25.0 |
Table 1: Demographic characteristics of surgical nurses (N = 60)
Knowledge of delirium prevention strategies for nurses: Results from the knowledge assessment indicated that many surgical nurses are knowledgeable about strategies for preventing delirium. 90% recognized that not giving unnecessary sedation helps prevent delirium, and 88% knew that monitoring for early warning signs is essential. About 85% of the nurses were aware of the importance of early mobilization, and 78% understood the need to keep patients well-hydrated. Two out of three organizations mentioned regularly orienting patients, confirming they are aware of the issue, but want to learn more (Figure 1).
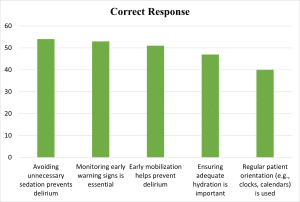
Figure 1: Nurses’ knowledge of delirium prevention strategies (N = 60)
Attitudes of nurses toward delirium prevention: The results showed that about 92% of surgical nurses consider preventing delirium a necessary duty, demonstrating their commitment. A significant 95% response reflected their belief that preventing delirium results in better patient outcomes. Still, more than half of the respondents believed that their delirium prevention training was not extensive enough, with around a third agreeing or disagreeing, showing that enhancing their training might be necessary (Table 2).
| Statement | Agree (%) | Neutral (%) | Disagree (%) |
| Preventing delirium is an essential nursing role | 92 | 5 | 3 |
| Training in delirium prevention is adequate | 60 | 20 | 20 |
| Delirium prevention improves patient outcomes | 95 | 3 | 2 |
Table 2: Attitudes of nurses toward delirium prevention (N = 60)
Nurses’ preventive practices: It is shown in the data that most surgical nurses follow essential strategies to prevent delirium. Most of the time, surgeons brought up the need to walk early and watched that patients remained well-hydrated (75% and 80%, respectively). Seventy percent of nurses always assessed preoperative delirium risk, and 68% tried to use less sedation during surgery. Even so, only a little more than half (60%) of participants showed a consistent use of cognitive orientation (e.g., using clocks or calendars), making this area worth highlighting as a priority in practice (Table 3).
| Practice | Always (%) | Sometimes (%) | Rarely/Never (%) |
| Assessing patients for delirium risk preoperatively | 70 | 25 | 5 |
| Encouraging early postoperative mobilization | 80 | 18 | 2 |
| Ensuring adequate hydration | 75 | 20 | 5 |
| Minimizing the use of sedative medications | 68 | 22 | 10 |
| Providing cognitive orientation (e.g., clocks, calendars) | 60 | 30 | 10 |
Table 3: Nurses’ preventive practices (N = 60)
Incidence of POD among elderly patients: POD was observed in 20 of the 100 elderly patients who had surgery, while 80 of them did not have delirium. Since only a limited number of patients experienced this issue, it demonstrates why pre-emptive actions are vital for surgical nurses (Figure 2).
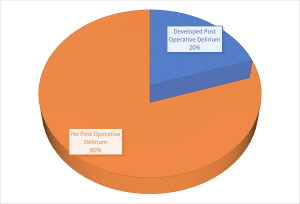
Figure 2: Incidence of POD among elderly patients (N = 100)
Association between nurses’ preventive practices and incidence of delirium: Data shows there is a major relationship between levels of follow-up for these guidelines and the occurrence of delirium. Delirium was less likely to happen in high adherence patients (8%), but much more so in low adherence patients (38%). Statistical analysis proves the connection (χ² = 12.34, p = 0.001), revealing that people who follow better practice have fewer delirium cases (Table 4).
| Practice level | Delirium developed (n, %) | No delirium (n, %) | Chi-square (χ²) | p-value |
| High adherence | 5 (8%) | 55 (92%) | 12.34 | 0.001 |
| Low adherence | 15 (38%) | 25 (62%) | – | – |
Table 4: Association between nurses’ preventive practices and incidence of delirium
Discussion
The research demonstrates that surgical nurses are vital in helping to prevent delirium in elderly people following surgery. According to the demographic data, there were considerably more senior female nurses, a finding that agrees with literature showing experienced nurses contribute significantly to delivering quality patient care.[18] Since many of the nurses in the study had adequate on-the-job knowledge, it may have contributed to what they reported about delirium prevention.
The extensive knowledge about delirium prevention strategies found in the nurses is reassuring and supported by a study, which shows that focused education raises nurses’ awareness of delirium. Concretely, not using too much sedation and walking early are important to reduce the risk of delirium, in line with clinical guidelines.[19] The basic focus on patient orientation points to another area that could be enhanced, which other research has shown to be a frequent shortcoming in delirium education.[20]
Nurses’ strong focus on preventing delirium is a positive sign and is consistent with research from other countries, where nurses also feel strongly that reducing delirium is essential for patient care.[21] Nevertheless, over half of the participants considered the training they received to be insufficient, against the findings which stress that nurses should get ongoing training in delirium prevention. This research points out that nurses want to prevent delirium but might have uncertainty and need to retrain, making it less likely they will always rely on consistent practices.[22]
Most nurses indicated they regularly rely on important preventive actions such as getting patients moving and encouraging them to drink, which is consistent with evidence-based standards.[23] It should be noted that cognitive orientation is less likely to be used than some other interventions in studies.[24] It is possible that practical or resource problems prevent delirium bundles from being used at full strength, making it important to introduce actions to raise awareness and usage of these packages.
The 20% prevalence of POD in these elderly patients is consistent with figures from other studies that show about 15–25% of elderly patients after surgery develop delirium. The high rate of delirium in surgery shows that taking active steps is necessary and can help nurses respond to this challenge. This link between good adherence and fewer cases of delirium proves that regular nursing care plays an important role in reducing this risk.[25]
Also, the fact that delirium was less common in patients managed by highly compliant nurses supports the need to implement prevention protocols strongly. In line with this, the study showed that proper nursing programs can substantially decrease cases of delirium. Because of this, hospital administration must offer frequent training, ensure resources are provided, and track the use of guidelines.[26]
This research provides significant information about surgical nurses’ knowledge, attitudes, and practices regarding delirium prevention and indicates areas where further improvement is needed, mainly training and cognitive orientation. Researchers should study what keeps people from following guidelines fully and assess the impact of special education programs on compliance. Increasing the education and care given by nurses can decrease the likelihood of POD, leading to improved outcomes and ensuring global best practices are applied.
Recommendations
- It is important for nursing education programs to include in-depth and regular training about preventing delirium, especially through a focus on cognitive orientation and early detection.
- Healthcare organizations should adopt consistent procedures and ongoing monitoring to encourage nurses to follow proper steps in preventing delirium.
- It is important to carry out further research to find out what gets in the way of nurses using delirium prevention guidelines in practice.
- Hospital staff should be given resources to support nurses in preventing delirium by offering them clocks, calendars, and reminders to stay hydrated, all designed to improve cognitive orientation.
- Working together with various medical teams helps ensure a complete plan for delirium prevention and uniform care as the patient moves through different treatment phases.
Conclusion
The findings suggest that surgical nurses are well informed and have a positive view on delirium prevention, which is reflected in how they handle the issue. Implementing effective delirium strategies greatly decreases the prevalence of delirium in older patients after an operation. Yet, there are still some areas, like using special tools for diagnosing or treating delirium, that need more attention. The data underlines how important it is for nurses to help prevent delirium and suggests they need further support to do so effectively.
References
- Ho MH, Nealon J, Igwe E, et al. Postoperative delirium in older patients: a systematic review of assessment and incidence of postoperative delirium. Worldviews Evid Based Nurs. 2021;18(5):290-301. doi:10.1111/wvn.12536 PubMed | Crossref | Google Scholar
- Igwe EO, Nealon J, O’Shaughnessy P, et al. Incidence of postoperative delirium in older adults undergoing surgical procedures: a systematic literature review and meta‐analysis. Worldviews Evid Based Nurs. 2023;20(3):220-237. doi:10.1111/wvn.12599 PubMed | Crossref | Google Scholar
- Damluji AA, Forman DE, Wang TY, et al. Management of acute coronary syndrome in the older adult population: a scientific statement from the American Heart Association. Circulation. 2023;147(3):e93-e621. doi:10.1161/CIR.0000000000001123 PubMed | Crossref | Google Scholar
- Russell CD, Lone NI, Baillie JK. Comorbidities, multimorbidity, and COVID-19. Nat Med. 2023;29(2):334-343. doi:10.1038/s41591-022-02156-9 PubMed | Crossref | Google Scholar
- Yang Y, Zhao X, Gao L, et al. Incidence and associated factors of delirium after orthopedic surgery in elderly patients: a systematic review and meta-analysis. Aging Clin Exp Res. 2021;33:1493-1506. doi:10.1007/s40520-020-01674-1 PubMed | Crossref | Google Scholar
- Pal N, Abernathy JH III, Taylor MA, et al. Dexmedetomidine, delirium, and adverse outcomes: analysis of the Society of Thoracic Surgeons Adult Cardiac Surgery Database. Ann Thorac Surg. 2021;112(6):1886-1892. doi:10.1016/j.athoracsur.2021.03.056 Crossref | Google Scholar
- Hussain AK, Kakakhel MM, Ashraf MF, et al. Innovative approaches to safe surgery: a narrative synthesis of best practices. Cureus. 2023;15(11):e48387. doi:10.7759/cureus.48387 PubMed | Crossref | Google Scholar
- Dilmen OK, Meco BC, Evered LA, Radtke FM. Postoperative neurocognitive disorders: a clinical guide. J Clin Anesth. 2024;92:111320. doi:10.1016/j.jclinane.2023.111320 PubMed | Crossref | Google Scholar
- Kleinfelder LD. Implementation of Evidenced Based Practice Guidelines for Reducing Emergence Delirium in Elderly Patients Undergoing a Total Hip Replacement. Doctor of Nursing Practice Scholarly Project. Otterbein University; 2026. Implementation of Evidenced Based Practice Guidelines for Reducing Emergence Delirium in Elderly Patients Undergoing a Total Hip Replacement
- Moody E, McDougall H, Weeks LE, et al. Nursing interventions to improve care of people living with dementia in hospital: a mixed methods systematic review. Int J Nurs Stud. 2024;104838. doi:10.1016/j.ijnurstu.2024.104838 PubMed | Crossref | Google Scholar
- Stollings JL, Kotfis K, Chanques G, Pun BT, Pandharipande PP, Ely EW. Delirium in critical illness: clinical manifestations, outcomes, and management. Intensive Care Med. 2021;47(10):1089-1103. doi:10.1007/s00134-021-06503-1 PubMed | Crossref | Google Scholar
- Bellelli G, Brathwaite JS, Mazzola P. Delirium: a marker of vulnerability in older people. Front Aging Neurosci. 2021;13:626127. doi:10.3389/fnagi.2021.626127 PubMed | Crossref | Google Scholar
- Mart MF, Roberson SW, Salas B, Pandharipande PP, Ely EW. Prevention and management of delirium in the intensive care unit. In: Semin Respir Crit Care Med. 2021;42(1):112-126. doi:10.1055/s-0040-1710572 PubMed | Crossref | Google Scholar
- Krupa S, Friganović A, Oomen B, Benko S, Mędrzycka-Dąbrowska W. Nurses’ knowledge about delirium in the group of intensive care units patients. Int J Environ Res Public Health. 2022;19(5):2758. doi:10.3390/ijerph19052758 PubMed | Crossref | Google Scholar
- Eagles D, Cheung WJ, Avlijas T, et al. Barriers and facilitators to nursing delirium screening in older emergency patients: a qualitative study using the theoretical domains framework. Age Ageing. 2022;51(1):afab256. doi:10.1093/ageing/afab256 PubMed | Crossref | Google Scholar
- Swarbrick CJ, Partridge JS. Evidence‐based strategies to reduce the incidence of postoperative delirium: a narrative review. Anaesthesia. 2022;77:92-101. doi:10.1111/anae.15584 PubMed | Crossref | Google Scholar
- Liang S, Chau JP, Lo SH, Zhao J, Liu W. Non-pharmacological delirium prevention practices among critical care nurses: a qualitative study. BMC Nurs. 2022;21(1):235. doi:10.1186/s12912-022-01019-5 PubMed | Crossref | Google Scholar
- Alanazi FK, Sim J, Lapkin S. Systematic review: Nurses’ safety attitudes and their impact on patient outcomes in acute‐care hospitals. Nurs Open. 2022;9(1):30-43. doi:10.1002/nop2.1043 PubMed | Crossref | Google Scholar
- Richemond RP. An Educational Intervention to Promote a Shift in Attitude in Using Dexmedetomidine to Prevent Pediatric Emergence Delirium. DNP Project. Florida International University; 2021. An Educational Intervention to Promote a Shift in Attitude in Using Dexmedetomidine to Prevent Pediatric Emergence Delirium
- Bellido D, García-García C, Talluri A, Lukaski HC, García-Almeida JM. Future lines of research on phase angle: strengths and limitations. Rev Endocr Metab Disord. 2023;24(3):563-583. doi:10.1007/s11154-023-09803-7 PubMed | Crossref | Google Scholar
- Liang S, Chau JP, Lo SH, Zhao J, Liu W. Non-pharmacological delirium prevention practices among critical care nurses: a qualitative study. BMC Nurs. 2022;21(1):235. doi:10.1186/s12912-022-01019-5 PubMed | Crossref | Google Scholar
- Hwang DY, Oczkowski SJ, Lewis K, et al. Society of Critical Care Medicine guidelines on family-centered care for adult ICUs: 2024. Crit Care Med. 2025;53(2):e465-e482. doi:10.1097/CCM.0000000000006286 PubMed | Crossref | Google Scholar
- Hakvoort L, Dikken J, van der Wel M, Derks C, Schuurmans M. Minimizing the knowledge-to-action gap: identification of interventions to change nurses’ behavior regarding fall prevention, a mixed method study. BMC Nurs. 2021;20(1):1-3. doi:10.1186/s12912-021-00598-z PubMed | Crossref | Google Scholar
- Van Dierendonck D, Lam H. Interventions to enhance eudaemonic psychological well‐being: a meta‐analytic review with Ryff’s Scales of Psychological Well‐Being. Appl Psychol Health Well Being. 2023;15(2):594-610. doi:10.1111/aphw.12429 PubMed | Crossref | Google Scholar
- Ho MH, Nealon J, Igwe E, et al. Postoperative delirium in older patients: a systematic review of assessment and incidence of postoperative delirium. Worldviews Evid Based Nurs. 2021;18(5):290-301. doi:10.1111/wvn.12536 PubMed | Crossref | Google Scholar
- Cortés-Beringola A, Vicent L, Martín-Asenjo R, et al. Diagnosis, prevention, and management of delirium in the intensive cardiac care unit. Am Heart J. 2021;232:164-176. doi:10.1016/j.ahj.2020.11.009 PubMed Crossref | Google Scholar
Acknowledgments
The authors would like to express their sincere gratitude to Dr. Shah Hussain, Principal/Assistant Professor, Zalan College of Nursing, Swat, for his invaluable supervision, guidance, and support throughout this study.
Funding
This research did not receive any specific grant from funding agencies in the public, commercial, or not-for-profit sectors.
Author Information
Corresponding Author:
Rifat Latif
Department of Nursing
Sharif College of Nursing, Lahore, Pakistan
Email: rifatlatif842@gmail.com
Co-Authors:
Firdos Kausar
Department of Nursing
Sharif College of Nursing, Lahore, Pakistan
Naheed Akhtar
Department of Nursing
Sina Institute of Nursing & Allied Health Science, Quetta, Pakistan
Shah Hussain
Department of Nursing
Zalan College of Nursing, Swat, Pakistan
Authors Contributions
Rifat Latif contributed to data collection and analysis; Firdos Kausar was involved in data analysis; Naheed Akhtar assisted with data collection; and Shah Hussain contributed to analysis and interpretations.
Ethical Approval
Ethical approval was obtained from the Institutional Review Board of Saidu Teaching Hospital, Swat (Ref. No. SGTH/IRB/2025/52).
Conflict of Interest Statement
The authors declare no conflict of interest.
Guarantor
Rifat Latif is the guarantor of this study and takes full responsibility for the integrity of the data and the accuracy of the data analysis.
DOI
Cite this Article
Latif R, Kausar F, Akhtar N, Hussain S. Surgical Nurses’ Role in Preventing Postoperative Delirium in Elderly Patients Undergoing Surgery. medtigo J Neurol Psychiatr. 2025;2(2):e3084224. doi:10.63096/medtigo3084224 Crossref









