Author Affiliations
Abstract
Postpartum mothers attending the neuropsychiatric hospital Remigio have suffered silently from puerperal psychosis in previous years and even now, due to certain sociodemographic factors, which are neglected and usually not reported. Although rare, it’s one of the most common psychiatric disorders experienced during postpartum. This study investigated the sociodemographic determinants of the prevalence of puerperal psychosis among postpartum mothers attending the neuropsychiatric hospital Remigio Port Harcourt. A retrospective research design was adopted. Three research questions and hypotheses guided the study. Data was collected using an Inventory from the daily client register; The population consisted of one hundred and sixty-six (166) reported cases of puerperal psychotic women who attended the hospital from January 2005 to December 2020. Instrument was validated by t-test statistical package, the hypothesis was tested using Chi Square in statistical package for the social sciences (SPSS) version 21. Results revealed that the prevalence of puerperal psychosis was 6 in 1000 women per year, and sociodemographic determinants such as lower maternal age, being married, having no form of education, and residing in rural areas were significantly associated with the prevalence of puerperal psychosis. The study showed that there is evidence of a low report rate of postpartum psychosis and recommended that identified cases should be reported early enough for prompt assessment, diagnosis, and proper treatment.
Keywords
Socio-demographic determinants, Prevalence, Puerperal psychosis, Postpartum mothers, Maternal age.
Introduction
Globally, the health and well-being of postpartum mothers have been an issue of concern for the world health bodies. Ensuring that postpartum mothers enjoy maximal physical, psychological, and social good health and well-being has received huge attention on a global scale. Postpartum mothers experience psychological turberance in pregnancy, especially during the puerperal period.[1] In Nigeria, it has been reported that many postpartum women suffer mental health problems in silence, which is unrecognized and also not reported, making it a contributory factor that affects the quality of maternal health shortly after childbirth.[2] The most common mental health disorder that occurs during this postpartum period is puerperal psychosis, and this disorder refers to a serious psychological disorder episode that starts abruptly days or weeks after delivery. The diagnosis is often difficult to identify due to its masked nature, and it is frequently confused with other aberrant behaviors because it is frequently concealed as general misbehavior. Worldwide, the prevalence of puerperal psychosis has been reported to be between 12 million and 352.3 million births yearly that’s 1-2 per every 1000 live births this is approximately for high-income countries.[3] In Nigeria, studies have also reported that the prevalence of postpartum psychosis is estimated to be 1.1 per 1000 deliveries; this does not include cases that are not identified or reported.[4]
Poor understanding of the factors and patterns leading to puerperal psychosis has delayed prevention, early detection, and correct care of patients with puerperal psychosis. Although the risk factors for postpartum psychosis is not really known, quite a few number of factors that could possibly lead to this condition have been identified and these includes primiparity, family-related history of psychosis, a history of mood disorder, pregnancy and obstetric complications, caesarean section, sex of the baby especially female child, lack of social support, history of affective disorder, stressful life circumstances, estrogen withdrawal, and difficulty sleeping during the postpartum period were few of the factors cited.[5-7]. Some studies stated that women are more susceptible to postpartum psychosis due to a variety of biological and psychological factors. Meanwhile, the knowledge of the impact of sociodemographic determinants on the risk of puerperal psychosis is not explicitly stated and is scarce because it has proven to be a significant risk factor for developing puerperal psychosis. Given the dangerous effects of puerperal psychosis in Nigeria and the few sociodemographic risk factors of postpartum psychosis identified, it is necessary that more studies be carried out to evaluate the socio demographic factors associated with the prevalence of puerperal psychosis. In a study conducted in the North-Western Nigerian context of a hospital of higher learning, primiparity was discovered as a factor for the occurrence of puerperal psychosis, and it frequently occurs in unbooked cases with unsupervised deliveries.[8] In a separate study conducted in a general hospital in Wushishi, Niger State, Nigeria, family care and the financial status of the family (social and economic standing) were reported to be predictors of puerperal psychosis. Few studies have been conducted on sociodemographic determinants and their association in the prevalence of puerperal psychosis; the number of these studies is quite limited, and the results are to some degree inconsistent.[9]
The study of the sociodemographic determinants of the prevalence of puerperal psychosis among postpartum mothers in neuropsychiatric hospital Remigio, Port Harcourt, was imperative due to an observed increase in the number of puerperal psychotic cases from audit in the records during a period of crisis in this geographical area and also as a result of the alarming existing gap in understanding the nuanced factors contributing to this severe postpartum mental health condition as efforts are only directed towards the genetic causes of this disorder. The scarcity of localized studies addressing the prevalence and determinants of puerperal psychosis in Port Harcourt, particularly within the specified timeframe from 2005 to 2020, underscores the need for a targeted investigation. Current literature has provided a general understanding of the condition; however, there is a dearth of in-depth exploration into the sociodemographic factors specific to the local population attending the neuropsychiatric hospital Remigio. This research aims to bridge this gap by examining and analyzing the sociodemographic determinants, thereby contributing valuable insights for tailored interventions and strategies to address the unique challenges posed by puerperal psychosis in this healthcare setting.[10]
Psychopathology of puerperal psychosis: The pathophysiology of puerperal psychosis involves a complex interplay of various factors, each contributing to the manifestation of psychotic symptoms in postpartum women. Understanding how these causes connect provides insights into the development of this severe mental health condition. Hormonal fluctuations, a central element in postpartum physiology, can trigger significant changes in neurotransmitter systems. These alterations in neurotransmitter function are linked to mood regulation, and their imbalance can contribute to the onset of psychotic symptoms such as hallucinations and delusions. Genetic predisposition reveals that individuals with a familial history of mood disorders may inherit genetic variants associated with neurotransmitter regulation and hormonal response systems. Neurotransmitter imbalance, particularly involving serotonin, dopamine, and gamma-aminobutyric acid (GABA), is implicated in the development of psychotic symptoms. Some studies suggest that disruptions in these neurotransmitter systems may contribute to the mood disturbances observed in postpartum psychiatric disorders.[11]
Immunological factors, the study introduces the concept of immune dysregulation playing a role in the vulnerability to puerperal psychosis. Inflammatory processes associated with immune dysfunction may impact the brain, influencing neurotransmitter function and contributing to the emergence of psychotic symptoms. Psychosocial stressors, including high levels of stress, lack of social support, and sleep disturbances, contribute to the overall vulnerability of women to puerperal psychosis. Meltzer-Brody et al.[5] emphasize the importance of considering these stressors in the context of perinatal mental health. Stress-induced changes in the hypothalamic-pituitary-adrenal (HPA) axis can further exacerbate hormonal imbalances and neurotransmitter dysfunction, fostering a conducive environment for psychotic symptoms. Dysregulation instress response systems can exacerbate mood disturbances and contribute to the emergence of psychotic symptoms. Finally, neuroimaging studies, such as those discussed by Friedman et al.[4] indicate structural and functional changes in the brain during the postpartum period. Alterations in regions like the amygdala and prefrontal cortex, crucial for emotional regulation, may directly contribute to the psychotic symptoms observed in puerperal psychosis.
Methodology
The study adopted a retrospective research design, the design was deemed appropriate because Shehu et al.[12] used it in their research work to investigate the association between socio-demographic variables and postpartum psychosis and the Obstetric characteristics and management of patients with postpartum psychosis.
The study was carried out in the neuropsychiatric hospital Remigio, Port Harcourt, Rivers State, Nigeria. The facility has the highest catchment population in the south region, so the researcher felt it would have the number of people needed for the study. The study’s target population included all reported inpatient and outpatient postpartum women who were diagnosed with puerperal psychosis from January 2005 to December 2020, and the total number was 166 postpartum women. These included 166 reported inpatients and outpatient postpartum women who attended the Hospital Port Harcourt from January 2005 to December 2020.
The instrument used for the study was an “inventory checklist from the daily clients register (DCR)” designed by the researcher, which was deemed appropriate because Shehu and Yunusa used the same instrument in their study for data collection.[12] The inventory was split into two parts; the first portion was used to determine the patient’s typical socio-demographic information from the reported cases of women who could have predisposed them to puerperal psychosis from hospital records, and the second part was used to determine the typical prevalence of puerperal psychosis.
The information acquired for this study was sorted and coded into the computer software using the statistical package for social sciences SPSS for analysis to indicate the frequencies and relationship between variables. All data were analyzed using inferential statistics; the data for prevalence of puerperal psychosis was analyzed using percentages, the various socio-demographic determinants information was analyzed using frequencies, while the research questions and null hypothesis were answered and analyzed using chi-square.
Results and Discussion
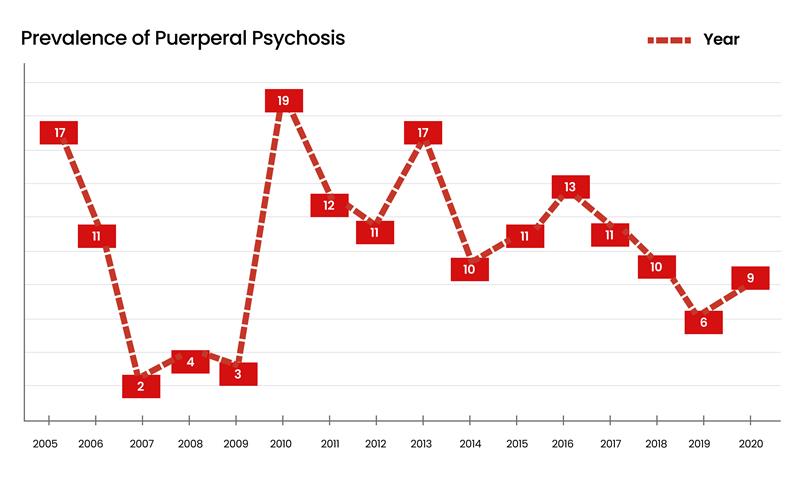
Figure 1: Prevalence of puerperal psychosis
The table above reveals that the prevalence of puerperal psychosis has varied over time. This further explains why, from 2009 to 2019, the incidence rate did not exceed 6 people per year, indicating that, in large part, the incidence rate trend has not been as strong in recent years.
| Variable | Mean | Standard deviation (SD) | Frequency statistics |
| Age | |||
| Greater than 30 | 1.25 | .931 |
12.366
|
| 30-20 | 3.25 | 1.693 | |
| less than 20 | 5.38 | 3.575 | |
| Marital status | |||
| Single | 3.00 | 1.751 |
14.012 |
| Married | 5.13 | 3.284 | |
| Divorced | 1.13 | 1.204 | |
| Separated | 1.25 | .856 | |
| Parity | |||
| Primigravida | 4.25 | 2.463 | 3.255 |
| Multigravida | 5.94 | 2.816 | |
| Level of education | |||
| Primary | 1.50 | 1.033 | 7.590 |
| Secondary | 1.44 | 1.556 | |
| Tertiary | 3.69 | 2.243 | |
| None | 3.81 | 2.536 | |
| Residence | |||
| Rural area | 7.13 | 3.897 | 14.852 |
| Urban area | 3.06 | 1.611 | |
Table 1: Socio-demographic determinants of puerperal psychosis common among postpartum mothers attending the neuropsychiatric hospital Remigio, Port Harcourt
The table shows the common sociodemographic factors among postpartum mothers attending the neuropsychiatric hospital Remigio, Port Harcourt. The table reveals that most of the postpartum mothers were aged less than 20 (mean 5.38), which shows that puerperal psychosis affected this age group more. The table also revealed that most of the women were married (mean 5.13), multiparous (mean 5.94). The study also revealed that these mothers had no form of education (mean 3.81), and area of residence was a significant predictor of puerperal psychosis, especially among women who lived in rural areas and were represented by (mean 7.13).
| Variable | Mean | SD | Frequency statistics | P-value |
| Greater than 30 | 1.25 | 0.931 | 12.366 | 1.000 |
| 30-20 | 3.25 | 1.693 | ||
| Less than 20 | 5.38 | 3.575 |
Table 2: Chi Square table showing the influence of age on the prevalence of puerperal psychosis among postpartum mothers in the neuropsychiatric hospital Remigio, Port Harcourt
The table reveals that the age of the postpartum mothers had a significant influence on the prevalence of puerperal psychosis (P = 1.000), as the women with a maternal age of less than 20 (5.38). This was because these mothers were not ready and mature enough to deal with the postpartum challenges, and that under 20-year-olds were the most childbearing age for postpartum.
| Variable | Mean | SD | Frequency statistics | P-value |
| Single | 3.00 | 1.751 | 14.012 | 1.000 |
| Married | 5.13 | 3.284 | ||
| Divorced | 1.13 | 1.204 | ||
| Separated | 1.25 | 0.856 |
Table 3: Chi Square table showing the influence of marital status on the prevalence of puerperal psychosis among postpartum mothers attending the neuropsychiatric hospital Remigio, Port Harcourt
The data above shows that the marital status of these women was a significant socio-demographic predictor of the occurrence of puerperal psychosis among these postpartum mothers, especially among the married women (5.13) undergoing treatment at the neuropsychiatric hospital Remigio, Port Harcourt (P = 1.000).
| Variable | Mean | SD | Frequency statistics | P-value |
| Primigravida | 4.25 | 2.468 | 3.255 | 0.081 |
| Multigravida | 5.94 | 2.816 |
Table 4: Chi Square table showing the influence of parity on the prevalence of puerperal psychosis among postpartum mothers in the neuropsychiatric hospital Remigio, Port Harcourt
Findings from the above table revealed that parity was not a likelihood for the prevalence of puerperal psychosis among these postpartum mothers (P = 0.081), its p-value is negligible as shown in the table above.
| Variable | Mean | SD | Frequency statistics | P-value |
| Primary | 1.50 | 1.033 | 7.590 | 0.000 |
| Secondary | 3.69 | 2.243 | ||
| Tertiary | 1.44 | 1.459 | ||
| None | 3.81 | 2.816 |
Table 5: Chi Square table showing the influence of level of education on the prevalence of puerperal psychosis among postpartum mothers in the neuropsychiatric hospital Remigio, Port Harcourt
The table above demonstrates that level of education was a significant socio-demographic determinant for the presence of puerperal psychosis (P = 0.000), especially among those who had no form of school education (3.81).
| Variable | Mean | SD | Frequency statistics | P-value |
| Rural area | 7.13 | 3.897 | 14.852 | 0.001 |
| Urban area | 3.06 | 1.611 |
Table 6: Chi-square table showing the influence of area of residence on the prevalence of puerperal psychosis among postpartum mothers attending the neuropsychiatric hospital Remigio, Port Harcourt
The findings from the table revealed that the area of residence was a significant factor that influenced the occurrence of puerperal psychosis (P = 0.001), and this was seen mostly among the mothers residing in villages (7.13).
Conclusion
The study was undertaken to determine the sociodemographic factors that account for the prevalence of puerperal psychosis among postpartum mothers who attended the neuropsychiatric hospital, Remigio, Port Harcourt, from January 2005 to December 2020. This study was necessitated by the limited literature and reports on the sociodemographic factors that predispose postpartum mothers to coming down with puerperal psychosis and the devastating effects on the mother, child, and family. It even gets to the extent of admitting the woman who is at risk for suicide and possible infanticide, all these are due to poor sensitization of potential mothers and family members on triggers to this disorder, and ensuring a good family support system right from the antenatal period.
Postpartum psychosis is a terrible and disabling condition that affects postpartum women, it requires early recognition of warning signs right from the antenatal period by identifying at risk mothers, ensuring adequate family support systems for both married and single mothers and also ensuring that identified cases are reported early for proper psychiatric care; furthermore, already reported and identified cases should be properly managed to prevent relapse. It is clear from the findings of this study that puerperal psychosis cases are rare and factors such as lower maternal age, being married, living in rural/low socioeconomic status, not being well educated were the common factors and variable found among these postpartum mothers that contributed to the occurrence of puerperal psychosis among them. The study also revealed that these variables had a likelihood of having a direct connection to most first-time admissions due to postpartum psychosis. However, through early detection of the disorder’s signs and symptoms, psychiatric nurses who have received specialized training and education in postpartum mental illnesses can significantly contribute to the recovery of women who are experiencing puerperal psychosis. Based on these findings, suggestions and recommendations were formulated. Health practitioners should make sure that nursing mothers are informed about certain socio-demographic characteristics, like marital status, age, housing, and occupation, during the prenatal and post-natal periods, and how they influence the occurrence of the disorder. These factors have been identified as some of the factors contributing to puerperal psychosis.
References
- Ajibade BL, Akinpelu AO, Ibrahim J, Adeniran G. Evaluation of perceived causes of puerperal psychosis among post-cesarean section patients in General Hospital, Wushishi, Niger State, Nigeria. Int J Nurs Midwife Health Relat Cases. 2018;4(4):1-21 Evaluation of perceived causes of puerperal psychosis among post-cesarean section patients in General Hospital, Wushishi, Niger State, Nigeria
- Haohao Y, Yudan D, Wenbin G. Mental health of pregnant and postpartum women during the coronavirus disease 2019 pandemic: A systematic review and meta-analysis. Front Psychol. 2020;11:617001. doi:10.3389/fpsyg.2020.617001 PubMed | Crossref | Google Scholar
- Jones I, Craddock N. Familiality of the puerperal trigger in bipolar disorder: results of a family study. Am J Psychiatry. 2001;158(6):913-917. doi:10.1176/appi.ajp.158.6.913 PubMed | Crossref | Google Scholar
- Friedman SH, Reed E, Ross NE. Postpartum Psychosis. Curr Psychiatry Rep. 2023;25(2):65-72. doi:10.1007/s11920-022-01406-4 PubMed | Crossref | Google Scholar
- Meltzer-Brody S, Larsen JT, Petersen L, et al. Adverse life events increase risk for postpartum psychiatric episodes: A population-based epidemiologic study. Depress Anxiety. 2018;35(2):160-167. doi:10.1002/da.22697 PubMed | Crossref | Google Scholar
- Nager A, Johansson LM, Sundquist K. Neighborhood socioeconomic environment and risk of postpartum psychosis. Arch Womens Ment Health. 2006;9(2):81-86. doi:10.1007/s00737-005-0107-7 PubMed | Crossref |
Google Scholar - Perry A, Gordon-Smith K, Jones L, Jones I. Phenomenology, Epidemiology and Aetiology of Postpartum Psychosis: A Review. Brain Sci. 2021;11(1):47. doi:10.3390/brainsci11010047 PubMed | Crossref | Google Scholar
- Raza SK, Raza S. Postpartum Psychosis. eBook. StatPearls Publishing; 2023 Postpartum Psychosis
- Jackson CL, Ciciolla L, Crnic KA, Luecken LJ, Gonzales NA, Coonrod DV. Intimate partner violence before and during pregnancy: related demographic and psychosocial factors and postpartum depressive symptoms among Mexican American women. J Interpers Violence. 2015;30(4):659-679. doi:10.1177/0886260514535262 PubMed | Crossref | Google Scholar
- Saleh el-S, El-Bahei W, Del El-Hadidy MA, Zayed A. Predictors of postpartum depression in a sample of Egyptian women. Neuropsychiatr Dis Treat. 2013;9:15-24. doi:10.2147/NDT.S37156 PubMed | Crossref | Google Scholar
- Sharma V, Mazmanian D. Sleep loss and postpartum psychosis. Bipolar Disord. 2003;5(2):98-105. doi:10.1034/j.1399-5618.2003.00015.x PubMed | Crossref | Google Scholar
- Shehu CE, Yunusa MA. Obstetric Characteristics and Management of Patients with Postpartum Psychosis in a Tertiary Hospital Setting. Obstet Gynecol Int. 2015;2015:386409. doi:10.1155/2015/386409 PubMed | Crossref |
Google Scholar - ShifaMwesigye. Mental Health,a Silent Burden for Women/ Giving Birth In Nigeria. Nigerian Health Watch. 2020 Mental Health,a Silent Burden for Women/ Giving Birth In Nigeria
- Topiwala A, Hothi G, Ebmeier KP. Identifying patients at risk of perinatal mood disorders. Practitioner. 2012;256(1751):15-2 Identifying patients at risk of perinatal mood disorders
- World Health Organisation. WHO urges quality care for women and newborns in critical first weeks after childbirth. 2022 WHO urges quality care for women and newborns in critical first weeks after childbirth
Acknowledgments
Special thanks to my supervisor, Dr Isabu, Dean of Nursing Faculty, HOD of Mental/Psychiatric Health Nursing, Faculty Lecturers, fellow students, and my family members.
Funding
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
Author Information
Corresponding Author:
Ogu A. Gracious
Department of Mental Health/Psychiatric Nursing
Faculty of Nursing, Niger Delta University, Nigeria
Email: graciousogu48@gmail.com
Co-Author:
Isabu C. Augustina
Department of Mental Health/Psychiatric Nursing
Faculty of Nursing, Niger Delta University, Nigeria
Authors Contributions
All authors contributed to the conceptualization, investigation, and data curation by acquiring and critically reviewing the selected articles. They were collectively involved in the writing – original draft preparation, and writing – review & editing to refine the manuscript. Additionally, all authors participated in the supervision of the work, ensuring accuracy and completeness. The final manuscript was approved by all named authors for submission to the journal.
Guarantor
None
DOI
Cite this Article
Ogu AG, Isabu CA. Socio-Demographic Determinants of Prevalence of Puerperal Psychosis Among Postpartum Mothers Attending Neuropsychiatric Hospital Remigio, Portharcourt. medtigo J Neurol Psychiatry. 2024;1(1):e3084119.
doi:10.63096/medtigo3084119 Crossref









