Author Affiliations
Abstract
Background: Permanent colostomy creates major life quality changes, which damage both patients’ bodily health and their mental condition while disrupting their social connections. Researchers aimed to evaluate quality of life (QoL) among permanent colostomy patients in a tertiary care hospital located in Swat to create focused interventions for population sub-groups.
Methodology: The study enrolled 70 participants aged 18 years or older who received a permanent colostomy at least three months ago. Structured questionnaires were used to gather data through direct interviews with the respondents. The research used the Statistical Package for the Social Sciences (SPSS) Version 26 to process data through descriptive and inferential statistics (chi-square tests), which investigated demographic characteristics and stoma-related and QoL variables.
Results: The reported stoma complications affected half of the patients through skin irritation, while leakage affected 40%, and odor affected 31.4%. Social adjustment demonstrated the greatest adverse effect as measured by QoL domain scores (2.5/5) that resulted in poor QoL for 51.4% of participants, ahead of physical comfort (2.8/5) and psychological well-being (3.1/5). Significant associations occurred between education levels and social QoL (χ² = 6.78, p = 0.009), gender and physical QoL (χ² = 4.32, p = 0.038), and complications showed an association with overall QoL (χ² = 8.15, p = 0.004).
Conclusion: Permanent colostomy patients from Swat demonstrate significant impacts on their quality of life due to financial constraints, together with inadequate education levels and restricted healthcare services. A combination of targeted educational initiatives, enhanced stoma care, and psychological support should be used to handle these difficulties.
Keywords
Permanent colostomy, Quality of life, Stoma complications, Social adjustment, Demographic characteristics.
Introduction
The surgical procedure of permanent colostomy produces a stoma opening through the abdominal wall to redirect fecal waste matter from patients whose lower colon or rectum requires removal because of colorectal cancer, inflammatory bowel disease, or trauma.[1] The life-changing surgery substantially affects QoL, involving the patient’s physical health, psychological state, and social relationships.[2] Stoma adaptation, psychosocial adjustment, stoma-related complications, and patient education determine long-term outcomes from this study. Identifying these elements by medical professionals leads to complete patient care delivery, which enhances postoperative health outcomes for patients with colostomies.[3,4]
The number of patients requiring permanent colostomy procedures keeps increasing as the incidence of colorectal cancer and pelvic surgeries for other diseases continues to rise. The global population of individuals with colostomy has reached 1 million, since 100,000 Americans receive such surgery each year.[5] Patients in regions with limited healthcare access develop their conditions at advanced stages before undergoing colostomy surgery and receive insufficient pre- and postoperative support.[6] A permanent colostomy delivers lifesaving benefits despite providing patients with lifelong challenges that affect QoL because they face difficulties with stoma care and body image concerns, as well as social stigma.[4,7]
Absence of self-esteem, together with disruptions in daily activities, results from physical limitations experienced by permanent colostomy patients, including peristomal skin irritation and leakage, alongside odor control issues.[8] Thirty to fifty percent of stomates face complications with their stoma within their first postoperative year, according to scientific studies, which leads to increased stress and reduced independence.[9] Adaptation becomes more complex because of unremitting medical supply needs and specialized care requirements, especially in regions with limited medical resources, such as rural areas and communities without adequate healthcare access. A colostomy’s physical weight and complications require specialized approaches to stoma care, which aim to prevent preventable medical challenges.[10]
Many individuals develop psychological distress after colostomy surgery since they experience anxiety as well as depression, along with post-traumatic stress symptoms.[9] The medical literature shows that depressive symptoms exist in 20-40 percent of colostomy patients because they worry about social isolation and sexual problems.[11] Younger colostomy patients often experience grief due to sudden changes in body function and appearance after surgery. Most healthcare systems need to improve their utilization of mental health support services because counseling and peer networking help minimize the adverse effects of these challenges, but remain underused.[12, 13]
The quality of life becomes negatively impacted by workplace challenges and social discrimination because of the difficulties colostomy patients face at work and in social settings. [14]. Exploring stoma patients through a survey revealed that it led 45% to avoid social events, while it caused employment problems for 30% of the responders. The public needs to receive educational initiatives about disability and incontinence because cultural attitudes tend to strengthen such obstacles.[15] The critical part in encouraging people to rejoin their professions and communities depends heavily upon family backing and health provider assistance.[16]
Scientific evidence shows that QoL improvement results from preoperative education combined with follow-up care, although these practices lack standardization in healthcare settings. Stoma education programs delivered before surgical procedures lead patients to acquire better self-care techniques and reduce anxiety compared to unprepared patients.[17] The quantity of time and differing nursing skills available during clinical care restrict the delivery of quality educational resources. Research must investigate how telehealth and digital resources help different populations through their effectiveness.[18]
Social and cultural differences between particular population groups affect the quality-of-life outcomes.[19] Frequent complications alongside poor adaptation occur when low-income countries lack sufficient access to specialized care providers and affordable medical supplies for their patients with stomas.[20] Even in developed countries, population groups with limited resources, such as older people and the uninsured, must overcome more obstacles to achieve quality of life. Measures that combine affordable surgical supplies with neighborhood-based care systems need to become standard practice because they help eliminate health care inequalities between groups of people while providing fair treatment.[19]
The research initiative seeks to provide a detailed assessment of permanent colostomy effects on QoL while establishing modifiable risk factors for clinical and policy use. Research results examining patient physical health status, psychological resilience, social integration, and systemic barriers will lead to strategies to enhance patient-centered care. Developing an integrated medical-psychological-social support structure is essential for maximum QoL improvement of colostomy patients.[21, 22]
Methodology
The research utilized a quantitative cross-sectional approach to measure QoL in permanent colostomy patients found in the surgical wards of a tertiary health facility in Swat, Pakistan, because it serves a sizable colostomy patient pool and represents a wide array of demographics. The research included participants aged 18 or above who received a permanent colostomy at least three months ago and demonstrated decision-making capabilities and consent to participate after passing inclusion criteria that excluded people with temporary colostomies alongside mental disabilities or psychiatric conditions. The research team employed convenient sampling to find 70 participants whose recruitment followed calculations from the Raosoft Sample Size Calculator at a 95% confidence threshold, utilizing a 5% error tolerance corresponding to the hospital’s annual colostomy patient demographic.
Data collection procedure: Before starting the study, the hospital gained ethical approval from its institutional review board (IRB), Ref No SGTH/ IRB/2025/ 03. After obtaining written consent, participating patients were contacted in person during their hospital stays or follow-up appointments. The questionnaire delivery involved trained research assistants who conducted face-to-face interviews to guarantee participant understanding while minimizing missing information. The data collection took place across three months.
Data analysis procedure: The researchers utilized SPSS (Version 26) statistical software to evaluate the obtained data. Statistics for demographic variables and QoL data were calculated using descriptive measures such as frequencies, percentages, means, and standard deviations. The study used inferential statistics to analyze data through chi-square tests, which evaluated the connection between gender categories and QoL measurement results.
Results
Demographic characteristics of participants: The total number of participants reached 70, with middle-aged adults between 31 and 45 comprising 40% of the group and males comprising 60% of this demographic. The educational level of the participants was limited because 35.7% completed secondary education, and 21.4% did not receive formal schooling. Almost two-thirds of respondents (64.3%) were unemployed due to potential socioeconomic hardships. The distribution revealed declining participant numbers across age groups above sixty years (11.4% of the total sample).
| Variable | Category | Frequency (n) | Percentage (%) |
| Age (years) | 18-30 | 12 | 17.1 |
| 31-45 | 28 | 40.0 | |
| 46-60 | 22 | 31.4 | |
| >60 | 8 | 11.4 | |
| Gender | Male | 42 | 60.0 |
| Female | 28 | 40.0 | |
| Education | No formal | 15 | 21.4 |
| Primary | 20 | 28.6 | |
| Secondary | 25 | 35.7 | |
| Tertiary | 10 | 14.3 | |
| Occupation | Employed | 25 | 35.7 |
| Unemployed | 45 | 64.3 |
Table 1: Demographic characteristics of participants (N=70)
Stoma-related characteristics: Results showed that 45.7% of the study participants kept their colostomy active for 7-12 months, followed by 25.7% between 3-6 months. The study confirmed that skin irritation affected 50.0% of participants, with leakage occurring in 40.0% and odors reported by 31.4%. When surveyed, 21.4% of patients had no complications due to the stoma. Long-term follow-up research seems necessary because 28.6% of participants have had a colostomy for over twelve months. The data demonstrate that colostomy patients endure considerable physical barriers, which become more prominent in their initial post-surgery year (Figure 1).
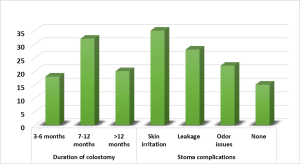
Figure 1: Stoma-related characteristics
QoL domains: According to study findings, social adjustment was the most problematic quality of life domain for permanent colostomy patients (2.5±0.8). Most participants displayed poor social quality of life (51.4%) while physical comfort and psychological wellbeing scores (mean = 2.8±0.9 and mean = 3.1±1.1) indicated moderate results. Of all patients, 45.7% had poor quality of life according to the composite QoL score (2.9±0.7), but good QoL existed for only 17.2% of respondents. Results validate significant psychosocial consequences of having a permanent colostomy, which primarily affect social relationships and physical ability in everyday life (Table 2).
| QoL domain | Mean score (SD) | Range (1-5) | Poor QoL (%) | Fair QoL (%) | Good QoL (%) |
| Physical comfort | 2.8 (0.9) | 1.2-4.5 | 42.9 | 38.6 | 18.5 |
| Psychological | 3.1 (1.1) | 1.5-4.8 | 35.7 | 42.9 | 21.4 |
| Social adjustment | 2.5 (0.8) | 1.0-4.2 | 51.4 | 32.9 | 15.7 |
| Overall QoL | 2.9 (0.7) | 1.3-4.3 | 45.7 | 37.1 | 17.2 |
Table 2: Quality of Life Domains (SQOLS Scores) Poor QoL = scores ≤2.5; Fair = 2.6-3.5; Good = ≥3.6
Chi-square test results for associations: QoL statistical findings showed multiple meaningful relationships between individual patient characteristics. Significant results indicated differences in physical adaptation to colostomy between male and female patients (χ² = 4.32, p = 0.038). Higher levels of education led to improved social QoL, according to statistical results (χ² = 6.78, p = 0.009).
| Variables compared | χ² value | p-value | Significance |
| Gender × Physical QoL | 4.32 | 0.038 | Significant |
| Education × Social QoL | 6.78 | 0.009 | Significant |
| Complications × Overall QoL | 8.15 | 0.004 | Significant |
| Age × Psychological QoL | 2.97 | 0.085 | Non-significant |
Table 3: Chi-square test results for associations
Discussion
This research presents critical understandings about permanent colostomy patients’ QoL difficulties in Swat, Pakistan, but its findings overlap with and depart from previous research outcomes. Our study participants demonstrate an unemployment rate of 64.3%, with limited educational attainment, including 35.7% secondary education and 21.4% without formal schooling. Middle-aged groups with male dominance at 60% accurately represent the local socioeconomic conditions, impacting QoL results. The research results indicate differences because colostomy patients in Western studies typically possess better educational attainment and higher employment rates.[23] Yet, these characteristics diverge from those of patients in Pakistan.
Research supports our discovery that social adjustment suffered the worst consequences for QoL among patients with colostomies, since patients reported poor QoL in this domain at 51.4%, with a mean score of 2.5 out of 5.[24] The level of social dysfunction among our population surpasses European population levels (mean = 3.2/5).[25] Because our culture shows higher disability stigma. The physical QoL score of 2.8 matched Nigerian findings. [26] Yet, it lies below Western populations, most likely because of supply and expert support deficits in stoma care.
The strong relationship between education level and social QoL (χ² = 6.78, p = 0.009) confirms global research, which shows that education enables better coping mechanisms.[27] The study proves that education in resource-limited healthcare environments creates stronger associations between training level and navigation ability within constrained health systems. Physical QoL shows gender distinctions (χ² = 4.32, p = 0.038). This contradicts Western findings that display no gender differences [28], since traditional gender roles in our region impose different physical requirements after colostomy surgery.
The presence of stoma complications proved to have the most damaging effect on QoL (χ² = 8.15, p = 0.004), which agrees with research conducted worldwide.[29] Our patients reported skin irritation in 50% of cases. In comparison, leakage occurred in 40% of patients, which exceeds the 20-30% reported in high-income countries, due to differences in preoperative stoma site marking and postoperative care quality. Results showed no psychological differences between young and elderly patients based on the χ² = 2.97, p = 0.085 analysis, which contests.[30] Findings that youthful patients suffer more frequently from body image problems. Patient psychological responses differ more based on universal poverty and healthcare problems than age-related psychological factors in our study area.
Recommendations: The implementation of tailored education programs should focus on improving stoma self-care for patients with limited educational backgrounds. Preoperative stoma site marking combined with post-surgery follow-up should be strengthened to minimize complications that cause skin issues and leakage. As per local cultural practices, establishing peer support groups should focus on psychosocial support for isolated patients. The development of rehabilitation programs should specifically focus on addressing the different physical needs of male and female patients.
Conclusion
The research illustrates the significant physical, psychological, and social difficulties that Swat’s permanent colostomy patients endure in Pakistan. The study demonstrates that 45.7% of participants faced subpar life quality because social adaptation suffered the most (51.4% reported negative QoL results). Education level and stoma complications, along with gender, made significant differences in outcome results, yet age did not play any role in patients’ psychological adaptation.
The study outcomes match worldwide research about quality-of-life disturbances in colostomy patients, yet demonstrate different patterns emerging from the local environment, specifically through increased complications alongside more severe social limitations observed relative to high-income nations. The region faces limitations in healthcare resources combined with socioeconomic factors and a cultural fear of disability as the primary cause for its differential outcomes.
References
- Parker JM, Feldmann TF, Cologne KG. Advances in Laparoscopic Colorectal Surgery. Surg Clin North Am. 2017;97(3):547-560. doi:10.1016/j.suc.2017.01.005. PubMed | Crossref | Google Scholar
- Davis BR, Valente MA, Goldberg JE, et al. The American Society of Colon and Rectal Surgeons Clinical Practice Guidelines for Ostomy Surgery. Dis Colon Rectum. 2022;65(10):1173-1190. doi:10.1097/DCR.0000000000002498. PubMed | Crossref | Google Scholar
- Barbosa I, Morais P, Torres H, Fonseca JC, Vilaça JL. Body Fluid Collection Devices for Ostomy Patients: A Review. Healthcare (Basel). 2024;12(21):2175. doi:10.3390/healthcare12212175 PubMed | Crossref | Google Scholar
- Hilleren IHS, Christiansen B, Bjørk IT. Learning practical nursing skills in simulation centers – A narrative review. Int J Nurs Stud Adv. 2022;4:100090. doi:10.1016/j.ijnsa.2022.100090 PubMed | Crossref | Google Scholar
- D’Ambrosio F, Pappalardo C, Scardigno A, Maida A, Ricciardi R, Calabrò GE. Peristomal Skin Complications in Ileostomy and Colostomy Patients: What We Need to Know from a Public Health Perspective. Int J Environ Res Public Health. 2022;20(1):79. doi:10.3390/ijerph20010079 PubMed | Crossref| Google Scholar
- Davis BR, Valente MA, Goldberg JE, et al. The American Society of Colon and Rectal Surgeons Clinical Practice Guidelines for Ostomy Surgery. Dis Colon Rectum. 2022;65(10):1173-1190. doi:10.1097/DCR.0000000000002498 PubMed | Crossref | Google Scholar
- Aryeetey L, Hinkle AJ, Huerta S, Sambandam S. The Impact of Colostomy on Inpatient Outcomes Following Primary Total Knee Arthroplasty. Cureus. 2024;16(7):e65900. doi:10.7759/cureus.65900 PubMed | Crossref | Google Scholar
- Babakhanlou R, Larkin K, Hita AG, Stroh J, Yeung SC. Stoma-related complications and emergencies. Int J Emerg Med. 2022;15(1):17. doi:10.1186/s12245-022-00421-9 PubMed | Crossref | Google Scholar
- Wiesler B, Hirt L, Guenin MO, et al. Stoma associated complications after diverting loop ileostomy, end ileostomy or split stoma formation after right sided colectomy-a retrospective cohort study (StoComSplit Analysis). Tech Coloproctol. 2024;28(1):68. doi:10.1007/s10151-024-02945-z PubMed | Crossref | Google Scholar
- Campos MOB, Monteiro AKDC, Mendes IAC, Avelino FVSD, Andrade JX, Andrade EMLR. Students’ knowledge on intestinal ostomies before and after an online educational platform intervention. Rev Bras Enferm. 2021;74(5):e20201313. doi:10.1590/0034-7167-2020-1313 PubMed | Crossref | Google Scholar
- Tang WSW, Chiang LLC, Kwang KW, Zhang MWB. Prevalence of depression and its potential contributing factors in patients with enterostomy: A meta-analytical review. Front Psychiatry. 2022;13:1001232. doi:10.3389/fpsyt.2022.1001232. PubMed | Crossref | Google Scholar
- Stavropoulou A, Vlamakis D, Kaba E, et al. “Living with a Stoma”: Exploring the Lived Experience of Patients with Permanent Colostomy. Int J Environ Res Public Health. 2021;18(16):8512. doi:10.3390/ijerph18168512 PubMed | Crossref | Google Scholar
- Black P, Notter J. Psychological issues affecting patients living with a stoma. Br J Nurs. 2021;30(6):S20-32. doi:10.12968/bjon.2021.30.6.S20 PubMed | Crossref | Google Scholar
- Petersén C, Carlsson E. Life with a stoma-coping with daily life: Experiences from focus group interviews. J Clin Nurs. 2021;30(15-16):2309-2319. doi:10.1111/jocn.15769 PubMed | Crossref | Google Scholar
- Ranjit S, Kissoon N. Challenges and Solutions in translating sepsis guidelines into practice in resource-limited settings. Transl Pediatr. 2021;10(10):2646-2665. doi:10.21037/tp-20-310 PubMed | Crossref | Google Scholar
- Anderson DM, Cronk R, Fejfar D, Pak E, Cawley M, Bartram J. Safe Healthcare Facilities: A Systematic Review on the Costs of Establishing and Maintaining Environmental Health in Facilities in Low- and Middle-Income Countries. Int J Environ Res Public Health. 2021;18(2):817. doi:10.3390/ijerph18020817 PubMed | Crossref | Google Scholar
- Bitton A, Fifield J, Ratcliffe H, et al. Primary healthcare system performance in low-income and middle-income countries: a scoping review of the evidence from 2010 to 2017. BMJ Glob Health. 2019;4(Suppl 8):e001551. doi:10.1136/bmjgh-2019-001551 PubMed | Crossref | Google Scholar
- Shah H, Sardar A, Dildar M, Ejaz HK, Muhammad A. Effect of Demonstration Regarding Percutaneous Endoscopic Gastrostomy Tube Feeding among Caregivers of Patients Diagnosed with Esophageal Carcinoma. medtigo J Med. 2024;2(4):e30622465. doi:10.63096/medtigo30622465 Crossref | Google Scholar
- Ranjit S, Kissoon N. Challenges and Solutions in translating sepsis guidelines into practice in resource-limited settings. Transl Pediatr. 2021;10(10):2646-2665. doi:10.21037/tp-20-310 PubMed | Crossref | Google Scholar
- Deshmukh V, John S, Arora NK. Utilization of Postnatal Healthcare Services Delivered through Home Visitation and Health Facilities for Mothers and Newborns: An Integrative Review from Developing Countries. Indian J Pediatr. 2020;87(3):207-216. doi:10.1007/s12098-019-03101-4. PubMed | Crossref | Google Scholar
- Yenet A, Nibret G, Tegegne BA. Challenges to the Availability and Affordability of Essential Medicines in African Countries: A Scoping Review. Clinicoecon Outcomes Res. 2023;15:443-458. doi:10.2147/CEOR.S413546. PubMed | Crossref | Google Scholar
- Beran D, Ewen M, Lipska K, Hirsch IB, Yudkin JS. Availability and Affordability of Essential Medicines: Implications for Global Diabetes Treatment. Curr Diab Rep. 2018;18(8):48. doi:10.1007/s11892-018-1019-z. PubMed | Crossref | Google Scholar
- Ellina P, Middleton N, Lambrinou E, Kouta C. Social gradient in health-related quality of life among urban middle-age residents in Limassol, Cyprus: research article. BMC Public Health. 2021;21(1):608. doi:10.1186/s12889-020-10027-6 PubMed | Crossref | Google Scholar
- Cochrane BS, Ritchie D, Lockhard D, Picciano G, King JA, Nelson B. A culture of compassion: How timeless principles of kindness and empathy become powerful tools for confronting today’s most pressing healthcare challenges. Healthc Manage Forum. 2019;32(3):120-127. doi:10.1177/0840470419836240 PubMed | Crossref | Google Scholar
- Panisset MG, Kilpatrick T, Cofré Lizama LE, Galea MP. Implementing education: Personal communication with a healthcare professional is a critical step to address vaccine hesitancy for people with multiple sclerosis. Mult Scler Relat Disord. 2022;63:103933. doi:10.1016/j.msard.2022.103933 PubMed | Crossref | Google Scholar
- Ahmed Z, Ellahham S, Soomro M, Shams S, Latif K. Exploring the impact of compassion and leadership on patient safety and quality in healthcare systems: a narrative review. BMJ Open Qual. 2024;13(Suppl 2):e002651. doi:10.1136/bmjoq-2023-002651 PubMed | Crossref | Google Scholar
- Sharma D, Cotton M. Overcoming the barriers between resource constraints and healthcare quality. Trop Doct. 2023;53(3):341-343. doi:10.1177/00494755231183784 PubMed | Crossref | Google Scholar
- Witter S, Hamza MM, Alazemi N, Alluhidan M, Alghaith T, Herbst CH. Human resources for health interventions in high- and middle-income countries: findings of an evidence review. Hum Resour Health. 2020;18(1):43. doi:10.1186/s12960-020-00484-w PubMed | Crossref | Google Scholar
- Kugler CM, Breuing J, Rombey T, et al. The effect of preoperative stoma site marking on risk of stoma-related complications in patients with intestinal ostomy-protocol of a systematic review and meta-analysis. Syst Rev. 2021;10(1):146. doi:10.1186/s13643-021-01684-8. PubMed | Crossref | Google Scholar
- Ambe PC, Kugler CM, Breuing J, et al. The effect of preoperative stoma site marking on risk of stoma-related complications in patients with intestinal ostomy – A systematic review and meta-analysis. Colorectal Dis. 2022;24(8):904-917. doi:10.1111/codi.16118 PubMed | Crossref | Google Scholar
Acknowledgments
Not reported
Funding
Not reported
Author Information
Corresponding Author:
Shah Hussain
Department of Nursing
Lincoln University College, Malaysia
Email: shahhussain.phdscholer@lincoln.edu.my
Co-Author:
Regidor III Poblete Dioso
Department of Nursing
Lincoln University College, Malaysia
Authors Contributions
Shah Hussain contributed to data collection, organization, analysis, and manuscript writing.
Dr. Regidor III Poblete Dioso contributed to data analysis.
Ethical Approval
The study received ethical approval from the hospital’s institutional review board (IRB), Ref No SGTH/IRB/2025/03. Written informed consent was obtained from all participating patients prior to their involvement in the study.
Conflict of Interest Statement
Not reported
Guarantor
None
DOI
Cite this Article
Hussain S, Dioso RPIII. Quality of Life in Patients with Permanent Colostomy: A Cross-Sectional Study at the Tertiary Care Hospital in Swat. medtigo J Med. 2025;3(2):e30623218. doi:10.63096/medtigo30623218 Crossref









