Author Affiliations
Abstract
Hemorrhagic shock is a critical emergency condition affected by severe blood loss, leading to inadequate tissue perfusion and oxygen delivery. This report highlights the management of hemorrhagic shock in a 32-year-old female following an automobile accident with suspected femoral artery injury. Upon arrival in the emergency department, she presented with hypotension, tachycardia, and signs of significant blood loss. Immediate interventions included securing the airway, administering oxygen, and performing volume resuscitation with Ringer’s lactate solution. A type and crossmatch for blood transfusion was conducted, and packed red blood cells were given to replace lost blood. The patient underwent urgent vascular surgical intervention for femoral artery control, followed by stabilization in the ICU. Postoperative care focused on monitoring complications and rehabilitation, including gradual mobilization and physical therapy. This case underscores the importance of early hemorrhage control, rapid surgical intervention, and a multidisciplinary approach in improving outcomes for patients with traumatic vascular injuries.
Keywords
Hemorrhagic shock, Arterial Bleeding, Trauma, Vascular surgery, Oxygen therapy, Emergency management.
Introduction
Hemorrhagic shock is a critical and life-threatening condition that is caused by severe blood loss, leading to inadequate tissue perfusion and oxygen delivery to vital organs. Losing more than 30% of circulating blood volume is considered critical in adults. Globally, hemorrhagic shock accounts for up to 8% of all deaths, resulting in around 1.9 million deaths annually due to massive bleeding. It is responsible for 40% of all trauma-related deaths and 27% of deaths during childbirth.[1]
Trauma is a leading cause of death, with hemorrhage responsible for nearly half of these fatalities. Hemorrhagic shock is common in trauma cases; one trauma center found that 62.2% of massive transfusions were trauma-related, using over 75% of blood products. Older adults face higher risks due to reduced physiological reserves, increased comorbidities, and frequent anticoagulant use, making them more vulnerable to rapid decompensation during hemorrhagic shock.[2,3]
Hemorrhagic shock results from severe blood loss, reducing oxygen delivery below tissue demand and forcing cells into anaerobic metabolism, which produces lactic acid. The body compensates by increasing heart rate, vasoconstriction, and redirecting blood to vital organs, but prolonged hypoperfusion worsens acidosis and leads to hemodynamic collapse. Shock responses vary based on age, comorbidities, and medications.[4] An important factor of hemorrhagic shock is the onset of trauma-induced coagulopathy. This is caused by early coagulation dysfunction, hemorrhage, fluid dilution, acidosis, and hypothermia. This coagulopathy, present in many before resuscitation, significantly worsens outcomes and highlights the need for early and targeted intervention.[5]
Hemorrhagic shock treatment has evolved to “damage control resuscitation,” focusing on permissive hypotension, hemostatic resuscitation, and rapid hemorrhage control to address coagulation, acidosis, and hypothermia. Permissive hypotension, which targets 90 mmHg systolic, aims to limit rebleeding before hemorrhage is controlled, though outcomes vary by injury type and trauma center access. Current strategies favor early use of blood products over crystalloids to reduce coagulopathy and metabolic derangements. A 1:1:1 plasma: platelets: Red blood cells (RBC) ratio improves early hemostasis and reduces death from bleeding. Antifibrinolytics like tranexamic acid, especially when given within 3 hours of post-injury, have been shown to reduce mortality. Timely hemorrhage control remains critical alongside resuscitation
efforts.[6,7]
This case report aims to highlight the critical steps involved in the emergency management of hemorrhagic shock due to major arterial bleeding following blunt trauma.
Case Presentation
A 32-year-old female was brought to the emergency department following an automobile accident with major arterial bleeding. Emergency medical services reported a significant bleeding suspected from a severed femoral artery. She was conscious, appeared pale and weak. Emergency medical services (EMS) reported about 600 mL of blood loss. They applied a tourniquet to the right leg to control the bleeding and started an intravenous (IV) line of normal saline.
On arrival, her blood pressure was 90/60 mmHg, heart rate of 120 bpm, respiratory rate of 22 breaths per minute, and temperature of 36.5 °C. The patient is pale, diaphoretic, and anxious. The patient is otherwise healthy and has no other significant past medical history. The central nervous system (CNS) examination reveals a Glasgow coma scale (GCS) score of 15, and the patient is alert and oriented. Cardiovascular examination indicates tachycardia with a regular rhythm, weak peripheral pulses, and delayed capillary refill. On auscultation, the patient is tachypneic, but the breath sounds are clear bilaterally. A complete blood count indicates hemoglobin of 10 g/dL, hematocrit of 30%, and other parameters within normal range. Blood coagulation shows prothrombin time (PT), activated partial thromboplastin time (aPTT), and international normalized ratio (INR) within normal range. An X-ray of the affected lower limb reveals no fractures but soft tissue swelling (Figure 1).
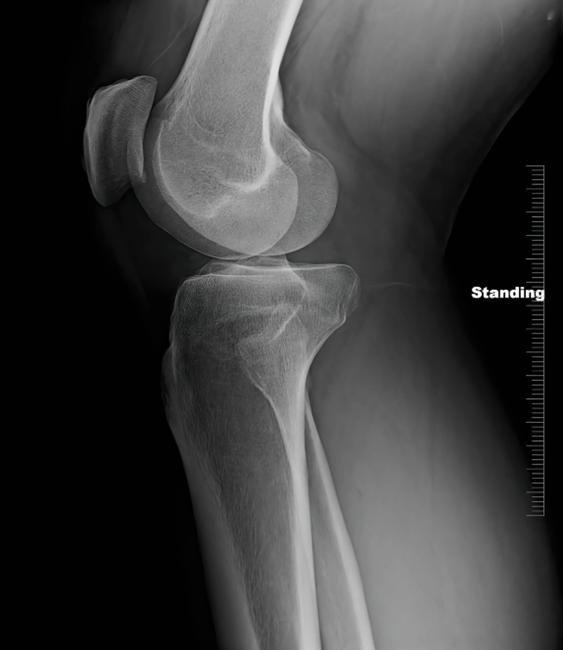
Figure 1: X-ray of the Knee Joint showing normal bony alignment and joint space
Case Management
Close monitoring of vital signs and physiological responses was conducted due to the patient’s low blood volume. A type and crossmatch for blood transfusion was performed immediately, and packed red blood cells were administered to replace blood loss. The patient was monitored hourly for improvements in blood pressure and heart rate. The airway was secured to ensure adequate ventilation, and oxygen therapy continued to maintain oxygen saturation above 94%. Two large-bore intravenous lines were established, and rapid infusion of 1–2 liters of Ringer’s lactate solution was initiated for volume resuscitation.
A surgical consultation was obtained for definitive control of the bleeding artery. Given the high suspicion of femoral artery involvement, urgent vascular surgical intervention was planned. The patient was stabilized, and temporary hemorrhage control was achieved before transfer to the intensive care unit (ICU) for continued monitoring.
In the ICU, the patient remained hemodynamically stable, with ongoing assessments of hemoglobin levels, electrolyte balance, and vigilance for potential complications such as compartment syndrome or infection. Pain management was optimized, and normothermia was maintained to reduce the risk of coagulopathy. Postoperative care included vascular imaging to confirm successful arterial repair, diligent wound care, and functional assessment of the affected limb. The patient’s recovery was closely monitored, with gradual mobilization and physical therapy initiated as appropriate. Long-term follow-up was arranged through outpatient vascular surgery and trauma services to ensure optimal healing and functional recovery.
Discussion
Hemorrhage remains the most common cause of shock in trauma patients, and a significant proportion of these individuals present to the hospital with severe physiological derangements resulting from acute circulatory collapse. Dr. Samuel D. Gross, one of the most influential and forward-thinking surgeons of the 19th century, famously described shock as “…a rude unhinging of the machinery of life.” This vivid and timeless description continues to resonate, capturing the profound systemic disruption caused by hemorrhagic shock, just as powerfully today as it did more than 175 years ago.[8]
Long D and Hessel M reported the case of traumatic aortic transection presenting with hemorrhagic shock. A 61-year-old man was brought to the emergency department after being struck by a vehicle, presenting with hypotension and signs of hemorrhagic shock. The image revealed a traumatic thoracic aortic transaction with a pseudoaneurysm. The patient underwent thoracic endovascular aortic repair (TEVAR) and recovered. Traumatic aortic injuries require high suspicion, especially in high-velocity impacts. Rapid imaging and endovascular repair can be lifesaving.[9]
Imamoto T et al.[10] explained the case report of a 7-year-old boy suffering an open skull fracture after being hit by a car, leading to hemorrhagic shock due to bleeding from an anterior cerebral artery pseudoaneurysm. The bleeding was controlled via endovascular embolization. While this case involves a pediatric patient, it highlights the importance of considering intracranial vascular injuries in open head traumas and the role of endovascular techniques in managing such bleeding.
Matsumoto N et al.[11] A patient with multiple displaced rib fractures and a traumatic head injury developed hemorrhagic shock due to an intercostal artery injury during initial trauma care. The bleeding was managed successfully using resuscitative thoracotomy (RT) and transcatheter arterial embolization (TAE). This case underscores the necessity of considering vascular injuries in patients with rib fractures and the effectiveness of combining surgical and endovascular techniques for hemorrhage control.
Negahi A et al.[12] Conducted a randomized controlled clinical trial to assess the effectiveness of intravenous tranexamic acid (TXA) in 68 patients with acute bleeding and hemorrhagic shock presentation due to blunt trauma of the abdomen, pelvis, and thorax, randomly assigned into two groups: TXA and placebo. TXA administration was associated with reduced blood product consumption and a shorter hospital stay. However, there was no significant difference in mortality rates between the TXA and placebo groups. This study concluded that early TXA use may reduce transfusion needs and hospital stay length in trauma-induced hemorrhagic shock.
Johansson PI et al.[13] carried out a multicenter, randomized, blinded clinical trial involving 229 trauma patients with hemorrhagic shock. Patients were randomized to receive a 72-hour infusion of the prostacyclin analog iloprost or placebo. While iloprost did not significantly increase the number of ICU-free days within 28 days, it was associated with a statistically significant reduction in hospital length of stay. This study concluded that iloprost was safe and reduced hospital stay duration, suggesting potential benefits in managing hemorrhagic shock in trauma patients.
The control of major bleeding after trauma (COMBAT) trial investigated the feasibility and effectiveness of plasma-based resuscitation in the prehospital setting for patients with traumatic hemorrhagic shock. The trial aimed to assess whether early plasma administration could improve outcomes by addressing trauma-induced coagulopathy promptly. Early plasma resuscitation in the field may offer benefits in managing traumatic hemorrhagic shock, warranting further investigation.[14]
Conclusion
This case report of a young adult female with a suspected femoral artery injury following a motor vehicle accident highlights the critical importance of rapid assessment, early hemorrhage control, and prompt initiation of resuscitative measures in the management of traumatic vascular injuries. Timely surgical consultation and definitive intervention were essential to achieving hemostasis and preserving limb function. This case also underscores the value of a coordinated, multidisciplinary approach, including intensive care support and postoperative rehabilitation, in optimizing patient outcomes and minimizing long-term morbidity associated with life-threatening arterial trauma.
References
- Faria I, Thivalapill N, Makin J, Puyana JC, Raykar N. Bleeding, Hemorrhagic Shock, and the Global Blood Supply. Crit Care Clin. 2022;38(4):775-793. doi:10.1016/j.ccc.2022.06.013 PubMed | Crossref | Google Scholar
- Eastridge BJ, Holcomb JB, Shackelford S. Outcomes of traumatic hemorrhagic shock and the epidemiology of preventable death from injury. Transfusion. 2019;59(S2):1423-1428. doi:10.1111/trf.15161 PubMed | Crossref | Google Scholar
- Bonanno FG. Management of Hemorrhagic Shock: Physiology Approach, Timing and Strategies. J Clin Med. 2022;12(1):260. doi:10.3390/jcm12010260 PubMed | Crossref | Google Scholar
- Jones AR, Miller JL, Jansen JO, Wang HE. Whole Blood for Resuscitation of Traumatic Hemorrhagic Shock in Adults. Adv Emerg Nurs J. 2021;43(4):344-354. doi:10.1097/TME.0000000000000376 PubMed | Crossref | Google Scholar
- Salvo N, Charles AM, Mohr AM. The Intersection of Trauma and Immunity: Immune Dysfunction Following Hemorrhage. Biomedicines. 2024;12(12):2889. doi:10.3390/biomedicines12122889 PubMed | Crossref | Google Scholar
- Hooper N, Armstrong TJ. Hemorrhagic Shock. eBook. StatPearls Publishing; 2022. Hemorrhagic Shock
- Fecher A, Stimpson A, Ferrigno L, Pohlman TH. Pathophysiology and Management of Hemorrhagic Shock in the Polytrauma Patient. J Clin Med. 2021;10(20):4793. doi:10.3390/jcm10204793 PubMed | Crossref | Google Scholar
- Bonanno FG. Management of Hemorrhagic Shock: Physiology Approach, Timing and Strategies. J Clin Med. 2022;12(1):260. doi:10.3390/jcm12010260 PubMed | Crossref | Google Scholar
- Long D, Hessel M. A Case of Traumatic Aortic Transection Presenting With Hemorrhagic Shock. J Emerg Med. 2020;58(4):e201-205. doi:10.1016/j.jemermed.2020.02.004 PubMed | Crossref | Google Scholar
- Imamoto T, Sawano M, Murase M. Hemorrhagic Shock Due to Traumatic Anterior Cerebral Artery Aneurysm: A Case Report. Cureus. 2023;15(5):e39801. doi:10.7759/cureus.39801 PubMed | Crossref | Google Scholar
- Matsumoto N, Hayashi N, Morita C, et al. A case of hemorrhagic shock due to intercostal artery injury that occurred during initial trauma care with multiple displaced rib fractures and traumatic head injury. Trauma Case Rep. 2022;40:100658. doi:10.1016/j.tcr.2022.100658 PubMed | Crossref | Google Scholar
- Negahi A, Teimoury T, Alimohamadi Y, Vaziri M, Khaleghian M. The effect of early tranexamic acid on bleeding, blood product consumption, mortality and length of hospital stay in trauma cases with hemorrhagic shock: a randomized clinical trial. J Prev Med Hyg. 2022;62(4):E958-965. doi:10.15167/2421-4248/jpmh2021.62.4.2186 PubMed | Crossref | Google Scholar
- Johansson PI, Fenger Eriksen C, Bovbjerg PE, et al. Prostacyclin in trauma patients with hemorrhagic shock: A randomized clinical trial. J Trauma Acute Care Surg. 2024;96(3):476-481. doi:10.1097/TA.0000000000004150 PubMed | Crossref | Google Scholar
- Chapman MP, Moore EE, Chin TL, et al. Combat: Initial Experience with a Randomized Clinical Trial of Plasma-Based Resuscitation in the Field for Traumatic Hemorrhagic Shock. Shock. 2015;44 Suppl 1(01):63-70. doi:10.1097/SHK.0000000000000376 PubMed | Crossref | Google Scholar
Acknowledgments
Not reported
Funding
Not applicable
Author Information
Corresponding Author:
Raziya Begum Sheikh
Independent Researcher, Department of Content
medtigo India Pvt Ltd, Pune, India
Email: raziya.pharma@gmail.com
Co-Authors:
Rabia Akram, Sonam Shashikala BV, Mansi Srivastava, Shubham Ravindra Sali
Independent Researcher, Department of Content
medtigo India Pvt Ltd, Pune, India
Samatha Ampeti
Department of Pharmacology
Kakatiya University, University College of Pharmaceutical Sciences, Warangal, TS, India
Authors Contributions
All patient-related data were collected by Rabia Akram. The initial draft of this case report/review was compiled by Raziya Begum Sheikh. The final review and editing were completed by Samatha Ampeti. All authors reviewed and approved the final version of the manuscript.
Informed Consent
Not applicable
Conflict of Interest Statement
This case report is based on a clinical case published in the “Cases” section of medtigo.com. The authors declare no conflicts of interest related to this publication.
Guarantor
None
DOI
Cite this Article
Raziya BS, Rabia A, Samatha A, Sonam SBV, Mansi S, Shubham RS. Prompt Management of Major Injured Artery in a Young Adult Trauma Patient. medtigo J Emerg Med. 2025;2(2):e3092221. doi:10.63096/medtigo3092221 Crossref









