Author Affiliations
Abstract
This study introduces a minimally invasive percutaneous technique for partial wrist denervation, targeting the posterior interosseous nerve (PIN) to alleviate chronic wrist pain. Traditional methods, including non-steroidal anti-inflammatory drugs (NSAIDs), bracing, proximal row carpectomy, and total wrist fusion, present limitations such as long recovery times, discomfort, and aesthetic concerns. The proposed technique employs a radiofrequency probe for selective PIN ablation, offering a less invasive alternative with no incisions, minimal scarring, and outpatient applicability. Diagnostic nerve blocks are used preoperatively to determine patient candidacy. Clinical outcomes demonstrate significant pain relief and functional improvement, with rapid return to work. Case studies highlight success in treating conditions such as scaphoid nonunion advanced collapse (SNAC), Kienbock’s disease, and dynamic carpal instability. This approach avoids complications associated with open surgeries and preserves options for further treatment if needed. The findings suggest that percutaneous wrist denervation is a promising solution for managing chronic wrist pain effectively and efficiently.
Keywords
Joint denervation, Percutaneous, Posterior interosseous nerve, Wrist pain, Joint denervation.
Introduction
Wrist pain for non-tendinous and non-carpal tunnel type pathology, i.e., related to primary problems in the wrist, particularly scapholunate dissociation (dynamic or static), scaphoid fracture with or without scaphoid non-union advanced collapse (SNAC), and Kienbock’s disease, can be quite disabling due to pain and reduced motion, resulting in weakness of grip strength. Over the years, five choices for the treatment of this primary wrist pain have evolved. Ultimately, one is treating arthritis from instability, spontaneous decay, or avascular necrosis.[1-3]
| NSAID |
| Bracing |
| Denervation (PIN or PIN+anterior interosseous neurectomy (AIN) |
| Proximal row carpectomy |
| Limited or total wrist fusion |
| Total joint replacement |
Table 1: Treatment choices for primary wrist pain
NSAIDs are not tolerated by all. Gastritis or the development of an ulcer occurs in about 2% to 4%. NSAIDs are an excellent choice for many people. If they work after being taken for about six weeks or less, then they must be continued indefinitely. Plus, there is the question of cardiovascular disease that goes unresolved. Wrist bracing can be cumbersome, unsightly, and inconvenient, but it may result in complete relief. However, it obviously gets in the way of gripping. More aggressive treatments such as proximal row carpectomy (PRC) have been quite good over the years, but involve a larger operation, discomfort, and longer time away from employment. Before NSAIDs were widely available in the mid-1960s, denervation or removal of the nerve from a joint to eliminate pain by stopping the signal that would otherwise be sent from the nerve ending to the brain was developed.[2]
Anatomic dissection by Rudinger et al.[1] and other anatomists many years before him led to the testing of denervation as a treatment option. This was first reported for the hip (30 patients, 65% to 75% good result), and later reports of denervation were given for the heel, ankle, knee, elbow, shoulder, jaw, and ultimately the base of the thumb and small joints of the
hand.[2]
| Authors | Joint denervation | Year |
| Nyakas et al.[3] | Heel | 1955 |
| Arenas-Prat J.[4] | Ankle | 2014 |
| Casagrande et al.[5] | Ankle | 1951 |
| Bateman JE.[6] | Global elbow | 1948 |
| Kaplan EB.[7] | Lateral elbow | 1959 |
| Dellon AL.[8] | Medial elbow | 2014 |
| Wilhelm A.[9] | Wrist | 1966 |
| Loréa P et al.[10] | Shoulder | 2005 |
| Foucher G et al.[11] | Proximal interphalangeal joint (PIP) of the finger | 1998 |
| Arenas-Prat JM.[12] | Distal interphalangeal joint (DIP) | 2012 |
| Patil V et al.[13] | Metacarpophalangeal (MP) joint | 2016 |
Table 2: Joint denervation origin
Joint denervation may be offered as an isolated procedure or it may be done in conjunction with other procedures, as an insurance policy for pain relief, when doing open reduction with internal fixation of fracture, excision of painful ganglion, radial osteotomy, etc. Wilhelm first reported his “total wrist denervation” in 1966, but he had been doing it since 1959.[9] This involved the deletion of 10 nerve branches through a series of incisions, both dorsal and palmar, on the wrist. It has been relatively popular, particularly in Germany. Results of isolated posterior interosseous nerve ablation versus a more comprehensive denervation.[14] It is now being promoted by different authors.
| Author | Year | Follow up (months) | Patients | Results | RTW (days) |
| Dellon et al.[15] | 1984 | 12 | 29
30 hands |
92% good to excellent | 83 |
| Fukumoto K et al.[16] | 1993 | 12 | 17 | 94% success | N/M |
| Ferreres A et al.[17] | 1995 | 60 | 50 | 74% success | N/M |
| Weinstein LP et al.[18] | 2002 | 30 | 19 | 85% | 73 |
| Hofmeister EP et al.[19] | 2006 | 28 | 48
50 wrists |
68% success | N/M |
| Giesen et al.[20] | 2017 | 12 | 30
31 wrists |
83% success | 18 |
| Sgromolo NM et al.[21] | 2018 | 12.5 | 13 | 31% success | 2/13 |
Table 3: Partial wrist denervation (N/M = Not mentioned)
| Author | Year | Follow up (months) | Wrists | Results | RTW
(days) |
| Rostlund et al.[22] | 1980 | 22 | 9 | 89% success | 56 |
| Ekerot, L et al.[23] | 1983 | 3-48 | 56% success | 14 | |
| Grechenig W et al.[24] | 1998 | 1998 | 11-1/2 | 22 | 77% success |
| Wilhelm A.[25] | 2001 | 126 | 48 | 81% success @ 14 mos
77% @ 26 mos 63% @ 16 mos |
N/M |
| Loréa P et al.[26] | 2002 | 5 | 14 | 84% success | N/M |
| Schweizer A et al.[27] | 2006 | 70 | 66-87% success | 61 or 70 | |
| Braga-Silva J et al.[28] | 2011 | 72 | 49 | 79% success | 35 |
| Storey PA et al.[29] | 2011 | 18 | 47 | 78% success | N/M |
| Fuchsberger T et al.[30] | 2018 | 206 | 68% success | N/M | |
| Simon E et al.[31] (France) | 2012 | 77 | 27 | 85% success | N/M |
| Foucher G et al.[11] | 1998 | 60 | 56 | 74% success | N/M |
| Patil V et al.[13] | 2016 | 36 | 21 | 95% success | N/M |
Table 4: Complete wrist denervation
In 1991, Cozzi first discussed denervation of the base of the thumb and reported a large series on a large series in which branches of the superficial radial nerve (SRN) were eliminated with 87% success in relieving pain. Though this is not utilized or reported on as extensively as wrist denervation per se, it appears to be gaining traction.
Discussion
Results reported have been contingent on the surgeon’s skill in performing the procedure, the number of nerves removed, and the completeness. The means and criteria for reporting outcomes, along with the duration of the follow-up, have been quite variable. In 1985, Dellon A proposed limiting denervation to the posterior interosseous nerve (PIN) at the wrist via a tiny dorsal incision, claiming that most of the nerve fibers contributing to the pain of the wrist would be eliminated.[8] As Nyakas and Wilhelm before him, he also recommended determining candidates for denervation dependent on their response to specific nerve blocks to each joint.[3,9] He reported 92% good-to-excellent results with short-term follow-up of only a year. Some others have felt that pre-denervation nerve blocking is beneficial, while others, Weinstein, Berger, Sgromolo, and Rostlund, have not found this beneficial.[18,21,22] Ferreres, et al.[17] retrospectively reported on a series of 30 isolated PIN ablations versus 22 total denervation via the Wilhelm technique. They disagreed with Dellon’s results for isolated PIN denervation. In their hands, PIN denervation resulted in inferior results to total wrist denervation. Eighty-six percent good-to-excellent and 14% failures were reported for total denervation versus 70% good-to-excellent and 30% failure in the isolated PIN denervation group with a mean follow-up of 4.7 years. They concluded that their results of pain relief were not dependent on the patient’s age or diagnosis. They felt that the initial relief of pain in the first few months of treatment decreased by about 10% in 12 months’ time and then stabilized. Upon review of their data, only pain and not grip or range of motion were parameters useful in grading the results. However, there has been variable success using this as a prognostic factor reported by other clinical researchers.
In the study of military patients treated in San Antonio, Sgromolo, NM et al.[21] put forth a rather bizarre study on soldiers with ill-defined wrist pain. Without saying so, they essentially were looking at patients with posterior interosseous nerve syndrome, wherein they treated 13 patients for whom no diagnosis could be confirmed as to the cause of wrist pain, despite all patients having undergone plain x-rays and magnetic resonance imaging (MRI) scans that were normal. For no specified reason, isolated PIN neuroctomy vs. anterior interosseous nerve (AIN) plus PIN were performed at the whim of one of four different hand surgeons. Only 2 of 13 soldier patients returned to work at their level of function prior to the onset of wrist pain, though 4 patients were said to have had complete resolution of their pain and were allowed to return to active duty four weeks postop. None of the 13 had been deployed following their procedure at the time of final follow-up, due to either permanent duty restrictions (N=6) or ongoing medical discharge (N=5) or no need for deployment mobilization (N=2). Of course, what does one expect with the huge secondary gain possible in this unusual workers’ compensation patient group. They failed in their study to show a difference between PIN neurectomy versus AIN plus PIN neurectomy or to make a case for it in treating patients with non-diagnosed, vague wrist pain.
Kadiyala, et al.[32] though finding pre-op nerve block useful, suggested the greatest use may be the negative response, i.e., the person not responding to this, someone who would probably be considered a poor candidate for an attempt at denervation, even though a positive result from the block does not guarantee a commensurate result with nerve ending deletion. The use of the nerve block may explain the small size of Dellon’s series, the superior success reported, and the largely excellent results reported by Donato et al.[33] who described meticulous surgical techniques and similar results to Dellon.
American surgeons have tended to seek tiny incisions to decrease surgical pain, improve the rate of recovery, and improve aesthetics in patients being treated for shoulder, knee, elbow, hand, hip, and even spine problems, among others. It seems natural, therefore, that trying to limit the denervation approach to the wrist to one or two small incisions or perhaps no incision if a percutaneous technique is available would be a desirable option. Weinstein et al.[34] in 2002, adding to Dellon’s approach, advocated including AIN ablation with the PIN via a single dorsal incision just proximal to the distal radioulnar joint (DRUJ) as proposed 17 years earlier but perhaps missed by many. Of Weinstein and Berger’s 19 patients, 85% reported pain relief with a 2-1/2-year follow-up. Notably, there is no good indication that taking out the anterior interosseous in Berger’s patients added anything to the outcome in terms of results in comparison to a partial denervation via isolated PIN ablation.[35]
Grafe MW et al.[36] in a smaller series of only 9 patients, both a dorsal and palmar longitudinal incision to include some innervation coming through the adventitia of the radial artery via the lateral antebrachial cutaneous nerve (nerve of Cruveilhier). He, however, reported only a 75% success rate in his small series. Bekler H et al.[37] pointed out the detailed anatomy of innervation existing with perivascular fibers and intraosseous fibers in the Haversian canals of the bone. Also, periosteal fibers and subchondral fibers exist. Thus, it is very hard to completely denervate around a joint.
Notably, concern over neuropathic joint decay after doing partial or total wrist denervation has never been justified. Complications have been mostly limited to temporary hypoesthesia occurring enough that it should probably just be considered routine for the procedure, along with rare neuromata in total wrist denervation. Kadiyala RK et al.[32] felt that denervating the nerve endings around the radial side of the wrist, i.e., radial artery, etc., from the lateral antebrachial cutaneous nerve (LABC) and superficial radial nerve (SRN), etc., should be done a few centimeters proximal to the wrist to avoid neuromatous pain. They are the only authors who reported a specific problem with that. Interpretation of results may also be influenced strongly by socioeconomic considerations and cultural influences.
Hofmeister, et al.[19] reporting on their results of denervation of the 50 wrists of 48 predominantly active military patients who had normal x-rays and abnormalities only identifiable on arthroscopy at 28-month follow-up reported only 25 excellent and 6 complete failures. Along the same lines, Ishida O et al.[38] reported terrible results of 29 patients and an overall 71% failure rate. Notably, these were large military contingents with wrist pain and normal x-ray and MRI exams. Equally bad results were reported by Sgromolo,et al.[21] with their 13 workers comp patients in the Texas military clinic. Thes studies suggest quite strongly a supratentorial factor, i.e., malingering, symptom magnification, i.e., secondary gain.[39]
Overall, the literature on partial and total wrist denervation reflects about an 80% to 90% success rate in treating patients with arthritis or wrist instability or Kienbock’s disease in people with objectively confirmed damage to the wrist who are not involved in the U.S. military. The fact that both the poor results in Sgromolo’s report and those of Hofmeister also involved doctors from the same institution, unfortunately, may impugn surgical technique. Single and double-incision techniques appear to achieve a good or better response than Wilhelm’s “total wrist denervation.” Newer anatomic research also shows that even though Wilhelm thought he was achieving total wrist denervation, he was missing several nerve branches, which could account for the less-than-optimal results reported.
Lorea et al.[40,41] first noted the sensory fibers entering the carpometacarpal CMC) of the thumb via tiny branches coming through the thenar motor branch of the median nerve. Researchers also demonstrated branches of the LABC going into the adventitia of the radial artery. Ulnar motor fibers have been identified, which could only be eliminated by very extensive dissection into the palm, which is not feasible due to the morbidity of the same. Not only does wrist denervation cause little discomfort perioperatively, but it is also an outpatient procedure. Depending on how it is done, there doesn’t have to be a noticeable scar. Most importantly, denervation doesn’t burn any bridges to further treatment. There is always proximal row carpectomy, partial or total wrist fusion, or, ultimately, in a selected patient, total joint replacement if denervation fails to get adequate pain relief.[42]
One of the concerns when looking at wrist denervation outcomes in those reported is whether the patients really achieve partial or total pain relief. In Buck-Gramcko’s enormous, non-randomized series reported with 4-year follow up, data being derived from about seven European surgeons, it is notable that only half of the 400 wrists, i.e., 195, were able to give outcome, i.e., not lost to follow up, and of that portion of the total that did give follow up, 69% were said to be “practically pain free” and only 5% were failures, i.e., no benefit at all.[43]
Feasibility of percutaneous denervation: In order to minimize pain and any visible scarring, in denervation limited to the PIN, I developed a technique of denervation using a single puncture wound with a Radionics radiofrequency probe. I had gained experience with the percutaneous technique for lumbar facet denervation on patients with lumbar facet syndrome and applied it to the wrist.[44]. Grutter, et al.[45] used injection techniques to test fresh frozen cadavers with methylene blue and confirmed that 100% of the time, they were able to inject the posterior interosseous nerve using anatomic landmarks for both the posterior interosseous and the anterior interosseous nerves. This validated the premise that I should be able to partially denervate the wrist, i.e., ablate the posterior interosseous nerve, using a percutaneous technique with the radiofrequency lesion probe.
Introduction of new technique: First, test the patient’s response to PIN nerve block using 1% lidocaine with epinephrine in the office, then the patient is taken to surgery.
With the patient supine and the upper extremity on the procedure table after giving a small dose of intravenous midazolam (1-3 mg), several cc’s of 3% chloroprocaine are infiltrated into the skin directly ulnar to Lister’s tubercle in the pronated forearm.[45] A 14-gauge intracath needle and sheath are then introduced down to the periosteum of the radius, radial to the ulnar, to the Lister’s tubercle, into the floor of the fourth extensor compartment. The patient is asked to flex and extend his thumb to make sure that the extensor pollicis longus tendon (EPL) is not being impaled. A sterile radiofrequency (RF) lesion electrode, a 5-cm needle with a 5-mm active tip, is inserted to selectively cauterize the PIN.[46] The electrode tip is positioned and repositioned, and an electric stimulus is administered until the painful stimulus recreates the patient’s symptoms or nerve-like pain is encountered. At this point, the cautery from the NT 100 Radiofrequency generator is turned on and kept at 85 degrees for 90 seconds. The procedure is repeated about two additional times, slightly distal or proximal to the first insertion. After completing this procedure, the surgeon stresses the patient’s wrist, and the patient is questioned as to whether there is any significant discomfort at that point. A Band-Aid™ is applied over the puncture wound. The patient is discharged from home. Return to work (RTW) is possible as soon as the sedative has worn off, i.e., the same day or the next day. NSAID is used exclusively, and/or acetaminophen may be supplemented. No opioids are necessary. The procedure takes between 5 and 20 minutes, depending on the patient’s medication requirements.[47-50]
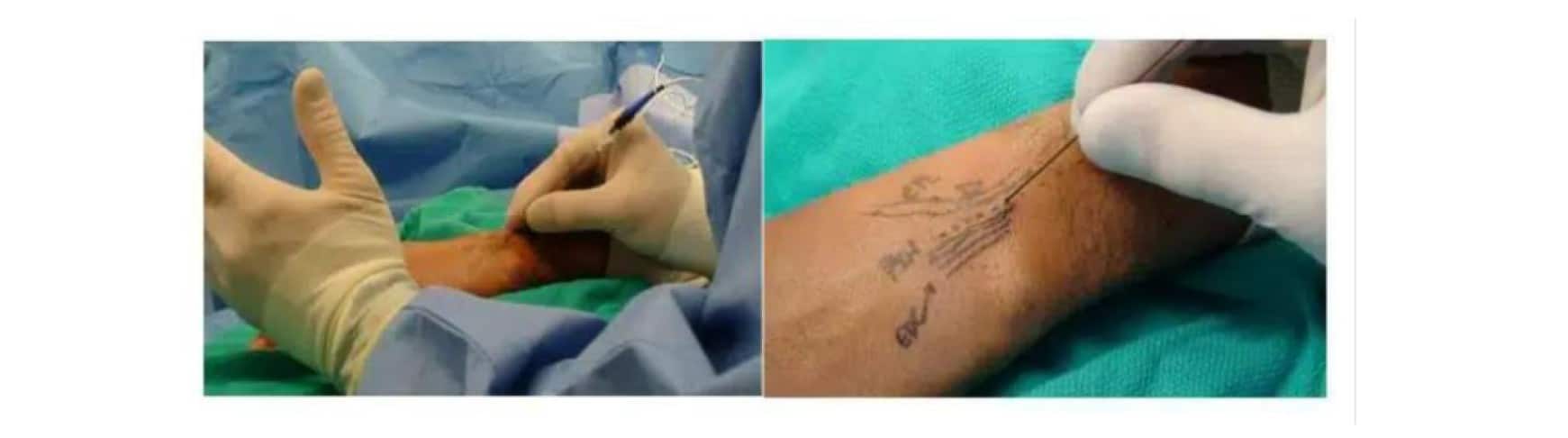
Figure 1: Electrode inserted into PIN
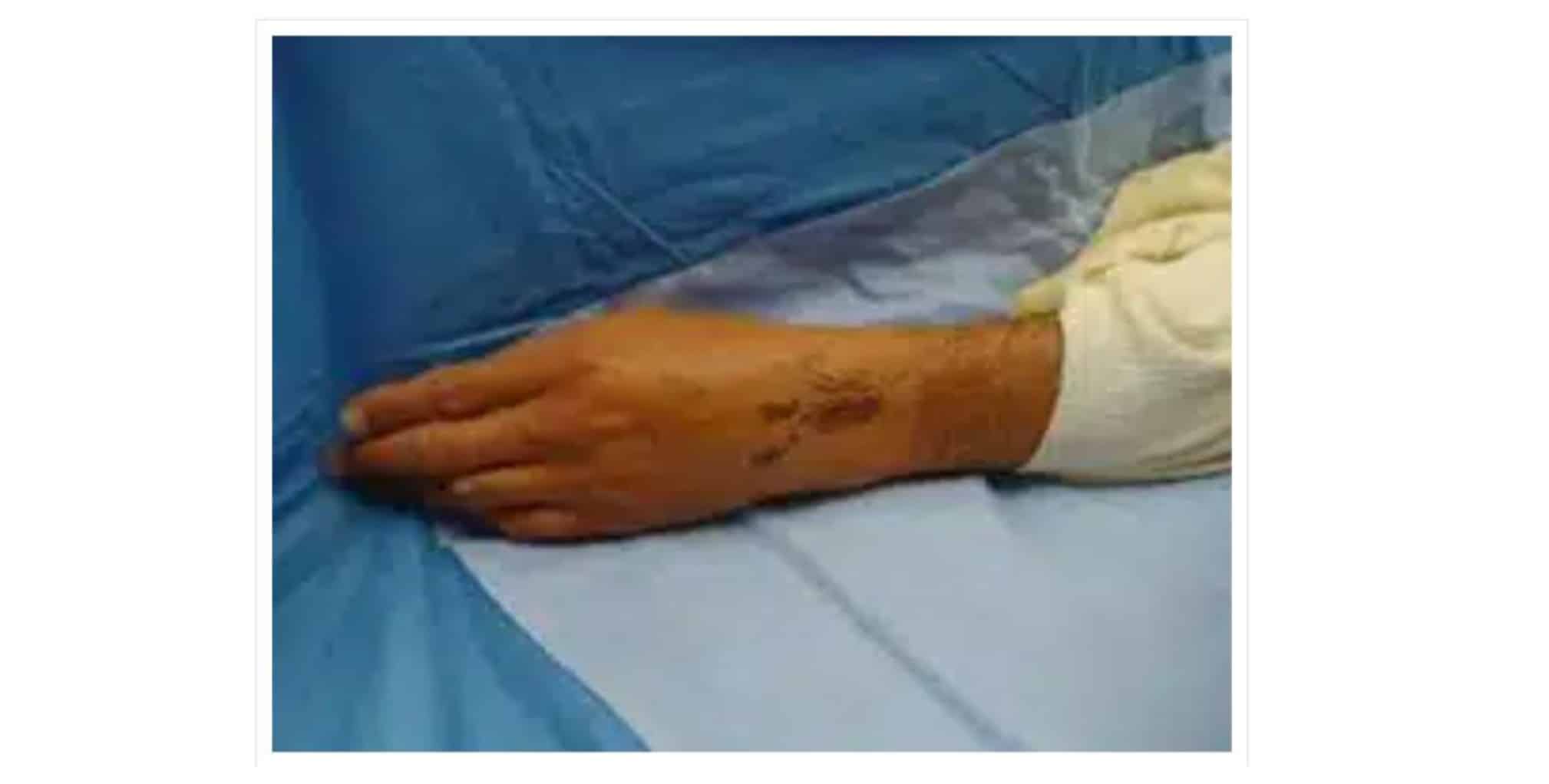
Figure 2: Hand sterilely prepped and draped
Case examples:
- A 60-year-old right-hand-dominant Caucasian electrician with a chronically untreated left scaphoid fracture non-union resulting in a Scaphoid nonunion advanced collapse SNAC wrist with radiocarpal, midcarpal, as well as capitolunate arthritis. Preoperatively, he had full flexion and extension of the wrist but limited radial and ulnar deviation with crepitation, but no swelling. The grip was 140 lbs. on the compared with 80 lbs. on the involved wrist. After failing a diagnostic nerve block in the office, a percutaneous wrist denervation was performed, as He was off work at the time of treatment. He did not miss any additional time off work to recuperate. However, he returned to work a few days after the treatment. He exhibited no pain from the arthritis during the 1-1/2-year follow-up. Grip strength at final follow-up was 135 lbs. right vs. 70 lbs. left, and with key pinch, right 31 and left 23 lbs.
- A 27-year-old right-handed Hispanic tile setter developed stage 2 Kienbock’s at age 25, and ultimately, after failed chiropractic, physical therapy, and NSAIDs along with wrist bracing, he was no longer able to use a hammer. The pain was present dorsally, ulnarly, and palmarly. The grip on the right-hand was 60 lbs. vs. 120 on the left. There was restricted motion in each direction. After a good response to a diagnostic posterior interosseous nerve block in the office, he underwent percutaneous wrist denervation. Sixteen days postoperatively, he reported an 85% reduction in pain. His grip had increased to 75 lbs., and he was given a release to regular work. At follow-up seven months post-op, he continued to do unrestricted duties with minimal discomfort in his wrist, and grip strength had increased to 100 lbs. vs. 110 on the left uninjured side. He did not require any NSAIDs or analgesics.
- A 28-year-old Caucasian deputy sheriff developed right ulnar wrist pain persisting for five months after restraining an enormous, combative He had pain with lifting and felt unable to use his firearm, a necessary requirement for his occupation. X-rays were normal. Grip strength was 94 lbs. on the right vs. 110 on the left, non-dominant side. There was pain in axial compression, ulnar deviation, and rotation of the wrist. Subtle dynamic carpal instability was diagnosed, and an arthrogram confirmed triquetrolunate deficiency. He responded well to a diagnostic posterior interosseous nerve injection. He had percutaneous needle cryo initially to freeze the nerve for three months. Pain returned, and after this wore off, he wanted to just have a formal open denervation rather than radiofrequency lesioning, which I believe would have worked in this case. He has continued to work in law enforcement without any restrictions, with follow-up six years after the procedure, and no subsequent treatment was required.
Conclusion
Limited wrist denervation with elimination of the PIN may give very good to complete pain relief. Literature on formal open partial denervation, in essence, serves as the control. A randomized study has not been performed and is not believed to be necessary based on supportive literature to date. Results with patients may be much better if limited to patients in whom a positive response to proximal PIN nerve block has been identified, though this issue is controversial.[49] Pre-denervation proximal nerve block, though not conclusive, is useful in determining the candidacy for the procedure. The injections can be made minimally uncomfortable by the use of chloroprocaine or buffered lidocaine. In some patients, both PIN and AIN deletion may be a better option than an isolated PIN ablation. PIN RF lesioning may be done percutaneously using the simple technique under wide-awake local anesthesia, no tourniquet (WALANT) outlined here.[50,51] It may be useful for AIN denervation, though the author has not yet attempted this option. Percutaneous PIN ablation is low cost, does not result in a scar, and is done as an outpatient with or without a sedative. In the eventthat the amount of benefit desired or expected after a positive PIN nerve block is not achieved, a more aggressive traditional procedure appropriate to the underlying pathology may be offered. The patient in whom considerable improvement is achieved but not complete pain relief, some patients may need to continue taking supplemental NSAID to avoid some of the bigger, and higher morbidity procedures.
References
- Rudinger N. Die Gelenknerven des Menschlichen Kopers. Erlangen: Verlag von Ferdinand Enke; 1857 Die Gelenknerven des menschlichen Körpers / von N. Rüdinger
- Saberi Hosnijeh F, Zuiderwijk ME, Versteeg M, et al. Cam Deformity and Acetabular Dysplasia as Risk Factors for Hip Osteoarthritis. Arthritis Rheumatol. 2017;69(1):86-93. doi:10.1002/art.39929 PubMed | Crossref | Google Scholar
- Nyakas A, Kiss T. Von Schultergelenks arthrosen stammende Schmerzen; heilung durch Denervation (Pains caused by arthrosis of the shoulder joint; treatment by denervation). Zentralbl Chir. 1955;80(24):955-958 Pains caused by arthrosis of the shoulder joint; treatment by denervation
- Arenas-Prat J. Denervation of the metacarpophalangeal joint. Tech Hand Up Extrem Surg. 2014;18(4):158-159. doi:10.1097/BTH.0000000000000057 PubMed | Crossref | Google Scholar
- Casagrande PA, Austin BP, Indeck W. Denervation of the ankle joint. J Bone Joint Surg Am. 1951;33-A(3):723-730 Denervation of the ankle joint
- Bateman JE. Denervation of the elbow joint for the relief of pain; a preliminary report. J Bone Joint Surg Br. 1948;30B(4):635-641 Denervation of the elbow joint for the relief of pain; a preliminary report
- Kaplan EB. Treatment of tennis elbow (epicondylitis) by denervation. J Bone Joint Surg Am.
1959;41-A(1):147-151 Treatment of tennis elbow (epicondylitis) by denervation - Dellon AL. Relief of pitcher’s elbow by denervation of medial humeral epicondyle. J Sports Med Doping 2014;3(1):1-3. doI:10.4172/2161-0673.1000135 Crossref | Google Scholar
- Wilhelm A. Articular denervation and its anatomical foundation: A new therapeutic principle in hand surgery. On the treatment of the later stages of lunatomalacia and navicular pseudoarthrosis (in German). Hefte Unfallheikd. 1966; 86: 1-109 Articular denervation and its anatomical foundation: A new therapeutic principle in hand surgery. On the treatment of the later stages of lunatomalacia and navicular pseudoarthrosis (in German)
- Loréa P, Foucher G. Dénervations articulaires en chirurgie de la main: Un plaidoyer. Ann Chir Plast Esthet.2005;50(2):154-160. doi:10.1016/j.anplas.2004.11.015 PubMed | Crossref | Google Scholar
- Foucher G, Long Pretz P, Erhard L. La dénervation articulaire, une réponse simple à des problèmes complexes de chirurgie de la main (Joint denervation, a simple response to complex problems in hand surgery). Chirurgie. 1998;123(2):183-188. doi:10.1016/s0001-4001(98)80104-9 Crossref | Google Scholar
- Arenas-Prat JM. Denervation of the distal interphalangeal joint. Tech Hand Up Extrem Surg. 2012;16(1):12-13. doi:10.1097/BTH.0b013e3182296e68 PubMed | Crossref | Google Scholar
- Patil V, Arenas-Prat J. Radical Wrist Denervation and Preliminary Results. Tech Hand Up Extrem Surg. 2016;20(3):96-98. doi:10.1097/BTH.0000000000000124 PubMed | Crossref | Google Scholar
- Kadiyala RK, Lombardi JM. Denervation of the Wrist Joint for the Management of Chronic Pain.
J Am Acad Orthop Surg. 2017;25(6):439-447. doi:10.5435/JAAOS-D-14-00243 PubMed | Crossref | Google Scholar - Dellon AL, Mackinnon SE, Daneshvar A. Terminal branch of anterior interosseous nerve as source of wrist pain. J Hand Surg Br. 1984;9(3):316-322. doi:10.1016/0266-7681(84)90051-2 PubMed | Crossref | Google Scholar
- Fukumoto K, Kojima T, Kinoshita Y, Koda M. An anatomic study of the innervation of the wrist joint and Wilhelm’s technique for denervation. J Hand Surg Am. 1993;18(3):484-489. doi:10.1016/0363-5023(93)90096-L
PubMed | Crossref | Google Scholar - Ferreres A, Suso S, Ordi J, Llusa M, Ruano D. Wrist denervation. Anatomical considerations. J Hand Surg Br. 1995;20(6):761-768. doi:10.1016/s0266-7681(95)80043-3 PubMed | Crossref | Google Scholar
- Weinstein LP, Berger RA. Analgesic benefit, functional outcome, and patient satisfaction after partial wrist denervation. J Hand Surg Am. 2002;27(5):833-839. doi:10.1053/jhsu.2002.35302
Acknowledgments
Not reported
Funding
None
Author Information
Dolf R. Ichtertz
Department of Orthopedic Surgery
Nebraska Hand & Shoulder Institute, PC, United States
Email: drichtertz@icloud.com
Ethical Approval
Not applicable
Conflict of Interest Statement
Not reported
Guarantor
None
DOI
Cite this Article
Ichtertz DR. Percutaneous Wrist Denervation, A New Technique: No Need for X-Ray or Ultrasound. medtigo J Med. 2025;3(1):e30623111. doi:10.63096/medtigo30623111 Crossref









