Author Affiliations
Abstract
Background: Critical care nurses (CCNs) routinely experience multiple ethical dilemmas that force them to test their ability to make decisions while respecting their professional duties. Nurses working in critical care need to resolve difficulties stemming from contradictory issues in end-of-life patient care, self-determination, resource distribution, and professional ethical standards.
Aim: This study explores the ethical challenges faced by CCNs at Saidu Teaching Hospital while examining their professional tactics for addressing these issues.
Methodology: This study employed a mixed-method approach, integrating quantitative and qualitative data collection. A structured questionnaire was used to survey 50 CCNs regarding their ethical challenges. The study conducted ten in-depth interviews with nurses who shared their procedures for dealing with problems, along with their techniques for making ethical decisions. Quantitative data were analyzed using SPSS, while thematic analysis was applied to qualitative data.
Results: The study showed that staff members frequently encounter ethical conflicts, which mainly include end-of-life decisions, together with the withholding of life-prolonging care and family-related disputes. Stress levels among nurses reached extremely high points according to their self-reported observations, and 16% were registered in this category. Most nurses face these ethical situations through peer collaboration (80%) while using their own moral guidelines (60%). However, participants expressed dissatisfaction with institutional ethics committees and training, citing inadequate support.
Conclusion: CCNs at Saidu Teaching Hospital frequently encounter ethical dilemmas. Nurses need support from institutions, together with practical ethical training and well-defined guidelines, to properly address their professional situations.
Keywords
Ethical dilemmas, Critical care nurses, Decision-making, Patient autonomy, Nursing ethics.
Introduction
Working in critical care environments creates multiple ethical challenges for nurses, which occur when patient autonomy, beneficence, and justice conflict with medical realities [1]. These situations compel healthcare professionals, especially nurses, to make difficult choices between competing values or conflicting responsibilities.[2] Nurses within intensive care units (ICUs) operate in critical locations that possess high consequences and intense pressure requirements, necessitating immediate life-changing choices.[3] In critical nursing scenarios, professional ethics compete against legal duties together with personal beliefs as nurses attempt to provide necessary care to life-threatening patients.[4] Such professional dilemmas require thorough examination to build nursing abilities for making sound decisions in challenging environments.[5]
Research consistently highlights ethical dilemmas as a serious problem in critical care areas since nurses encounter these situations frequently.[6] Studies show that about 60% of ICU nurses face ethical problems with their daily work responsibilities.[7] Nurses encounter ethical scenarios stemming from the various situations that involve end-of-life choices, along with resource distribution decisions or medical treatment limitations for patients with poor prognoses. Nurses must understand how they handle these challenges since their decision-making power determines patient welfare and their career development.[8] The high rates of ethical dilemmas in nursing practice emphasize the necessity of creating institutional training programs that support nurses when handling complex ethical situations.
Research provides insufficient attention to how nurses handle ethical dilemmas, even though these situations occur frequently.[9] Nurses identify most ethical issues that develop in critical care, yet physicians, together with other medical team members, often block the visibility of nurse voices concerning these matters.[10] The research lack creates a problem, since nurses, as frontline caregivers, can shape ethical choices because of their patient-family interaction. Such moral dilemmas impact both the psychological state and emotional well-being of nurses who show considerable job satisfaction.[11] Knowledge about how nurses experience and handle ethical situations demands a fundamental approach to supporting nursing staff in workplace settings.[12]
People who encounter ethical dilemmas frequently experience extensive psychological and emotional pressure. Nurses develop stress-related reactions and moral distress and experience burnout when they make challenging decisions at their workplaces.[13] Moral distress impacts nurses when they become helpless because they feel unable to follow their ethical principles or meet their patients’ best care requirements.[14] Fast and deadly medical choices within critical care units create additional ethical challenges because of the elevated temporal demands. Research demonstrates how stressful professional decisions at work cause nurse dissatisfaction and increased turnover rates, which emphasizes the requirement of institutional programs supporting ethical decisions and emotional healthcare for nurses.[15]
The ethical problems confronting nurses in critical care facilities affect personal well-being and result in enhanced quality of care for patients.[16] Nurses must successfully handle these challenges due to their direct influence on the quality of critical illness care they provide to patients. Guidance for complex moral decisions arises from learning programs combined with practical teaching and professional help systems.[17] Further research into nurses’ experiences with ethical dilemmas can help healthcare institutions refine professional development initiatives and allocate resources to strengthen ethical decision-making frameworks in critical care settings. [18]
Methodology
Study design and setting: The research combination of quantitative data collection with qualitative methods enabled a holistic understanding of critical care nurses’ ethical challenges. The mixed data collection design integrates multiple information types, leading to the enhancement of interpretation through both numerical statistics and personal testimony. The research design used structured surveys to analyze ethical dilemmas but added semi-structured interviews to understand critical care nurses’ entire spectrum of experiences and their ways of coping with dilemmas and institutional support reviews. The research site was Saidu Teaching Hospital, based in a substantial urban area where its critical care unit deals with both high-acuity and active patient load. The research site is an optimal setting because this hospital provides crucial services equally to adult and pediatric patients from different demographics. Nurses in the critical care unit (CCU) at the hospital administer care to patients in ICU settings and high-dependency units (HDUs) because they frequently encounter situations requiring moral decisions and managing complex technological equipment and end-of-life quality of care.
Study population and sampling: Saidu Teaching Hospital served as the research setting for critical care nurses working in both the ICU and the HDU. All study participants belonged to the group of registered nurses, nurse practitioners, and senior nurses who actively managed patients. An appropriate representation of participants for the quantitative study was obtained by selecting them through convenient sampling methods. The survey included fifty CCNs who worked in the ICU and HDU and volunteered for the study according to their availability. Since the research required immediate data collection, the researchers chose convenient sampling because it provided a chance to survey those participants who were available during the designated time window. Research on healthcare professionals commonly utilizes this method because practitioners often have different work shifts.
The research adopted purpose sampling to choose 10 critical care nurses with a significant work history in intensive care areas. The research selects nurses because they possess significant experience with the diverse ethical issues that arise in ICU/HDU practice. Researchers included nurses with different levels of proficiency, ranging from new registrants to seasoned practitioners, to obtain diverse insights. The selected participants showed readiness to participate and prove their understanding of ethical challenges experienced in their clinical work. Through purposive sampling, the researchers collect in-depth interview findings that answer their research questions specifically from sources that have directly experienced the issue.
Data collection tools
Questionnaire: A structured questionnaire was used to collect quantitative data. The research instrument consisted of questions that aimed to record how often nurses faced ethical dilemmas, as well as the variety of these ethical situations that presented themselves. A pristine questionnaire adopted closed-response questions to explore distinct ethical scenarios such as end-of-life choices, disputes with families, and allocation of resources, along with life-saving utilization measures. The participants evaluated the occurrence of their ethical dilemmas through a Likert rating scale, which spanned from “never” to “always.” The survey collected statistical information about nurses’ ages and experience levels, as well as their academic qualifications, to evaluate if these variables affect their ethical dilemma situations. A preliminary review of the survey took place with critical care nurses to verify accuracy and appropriateness for full distribution to the research subjects.
Semi-structured Interviews: A total of ten carefully chosen nurses participated in purposeful semi-structured interviews as part of this research investigation. The interviewer-maintained flexibility through the semi-structured format, which granted him or her freedom to delve further into interview responses and follow new topics that emerged naturally. The interview guide encompassed essential areas for inquiry by assessing nurses’ ethical challenges and their approaches to moral distress, along with their institutional support experiences and ethical decision-making views in the critical care environment. Each question had an open format to obtain elaborate responses from participants. The research design sought direct responses about ethical dilemma situations they encountered, alongside descriptions of their resolution methods and access to any available support.
The dual approach to data collection occurred simultaneously to establish a complete understanding of nurses’ ethical challenges. The data collection methods used together enabled researchers to perform data triangulation through survey and interview methods.
Data analysis
Quantitative data analysis: The surveys received statistical analysis through the commonly used statistical package for the social sciences (SPSS). Descriptive statistics were used to analyze demographic characteristics (age, gender, work experience) and the frequency of ethical dilemmas encountered. Descriptive statistics were used to analyze demographic characteristics (age, gender, work experience) and the frequency of ethical dilemmas encountered. The research strategy used frequency distribution to establish common patterns among encountered ethical dilemmas, including decisions about end-of-life care, consent-related dilemmas, and ethical tension between nurses and other healthcare providers. The researchers utilized quantitative approaches to determine consent-related nurse encounters with ethical matters and establish the most difficult ethical situations faced by nurses.
Qualitative data analysis: Thematic analysis served as the method for analyzing semi-structured qualitative interview data. The researchers decided to utilize thematic analysis since it enables them to notice recurring ideas together with patterns and themes found within textual data. The majority of interview data is received in full transcription and then read multiple times by the researcher to deeply connect with the information. The researchers conducted coding and combined matching codes into distinct themes. The researchers divided themes into categories that linked to their research inquiries and the fundamental elements of participant experiences. Through thematic analysis, researchers gained profound insights regarding how nurses described ethical challenges they encountered as well as their emotional responses when handling moral distress and the coping mechanisms they employed. The researchers used information from key themes extracted through interviews to enhance their analysis of numeric data.
Results
Demographic characteristics of survey participants: A total of 50 CCNs participated in the quantitative survey. The following table presents the demographic characteristics of the participants (Table 1).
| Demographic factor | Frequency | Percentage |
| Age group | ||
| 20–29 years | 15 | 30 |
| 30–39 years | 20 | 40 |
| 40–49 years | 10 | 20 |
| 50+ years | 5 | 10 |
| Gender | ||
| Female | 35 | 70 |
| Male | 15 | 30 |
| Years of experience in critical care | ||
| Less than 5 years | 10 | 20 |
| 5–10 years | 15 | 30 |
| 11–20 years | 15 | 30 |
| More than 20 years | 10 | 20 |
| Highest educational qualification | ||
| Diploma | 20 | 40 |
| Bachelor’s degree | 25 | 50 |
| Master’s degree | 5 | 10 |
Table 1: Demographic characteristics of survey participants (N = 50)
Frequency of Ethical dilemmas encountered by nurses: The survey examined the frequency of various ethical dilemmas faced by critical care nurses. Respondents were asked to rate the frequency of specific ethical dilemmas on a 5-point Likert scale (1 = Never, 5 = Always). The following table summarizes the results.
| Ethical dilemma | Never (%) | Rarely (%) | Sometimes (%) | Often (%) | Always (%) |
| End-of-life decision-making | 2 (4%) | 3 (6%) | 18 (36%) | 14 (28%) | 13 (26%) |
| Withholding life-sustaining treatment | 5 (10%) | 7 (14%) | 15 (30%) | 12 (24%) | 11 (22%) |
| Conflicts with family members about treatment decisions | 6 (12%) | 8 (16%) | 20 (40%) | 9 (18%) | 7 (14%) |
| Resource allocation (e.g., ICU bed availability) | 4 (8%) | 6 (12%) | 18 (36%) | 12 (24%) | 10 (20%) |
| Ethical conflicts with other healthcare providers | 8 (16%) | 10 (20%) | 15 (30%) | 9 (18%) | 8 (16%) |
| Obtaining consent for treatment in critical situations | 7 (14%) | 12 (24%) | 14 (28%) | 11 (22%) | 6 (12%) |
Table 2: Frequency of ethical dilemmas encountered by nurses (N = 50)
Coping mechanisms employed by nurses: The research examined the methods that nurses use to deal with moral conflicts in their practice. The interview and survey data showed which methods nurses use to manage their challenges.
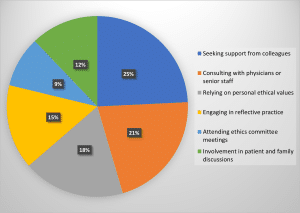
Figure 1: Coping mechanisms employed by nurses
Emotional and psychological impact of ethical dilemmas: The researchers evaluated emotional ethical stress through questions about challenging ethical scenarios that nurses encounter. This table presents the overall stress scores that nurses reported during the study.
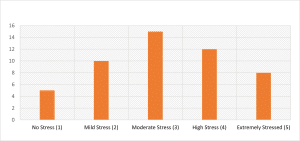
Figure 2: Emotional and psychological impact of ethical dilemmas (N = 50)
Institutional support for handling ethical dilemmas: Alternative forms allowed the researchers to evaluate what nurses thought about their organization’s support for resolving ethical dilemmas. Study participants evaluated their involvement with institutional resources that included ethics committees, together with training programs and mentorship opportunities.
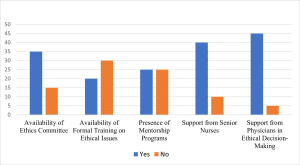
Figure 3: Institutional support for handling ethical dilemmas (N = 50)
Key themes from qualitative interviews: The thematic analysis of collected qualitative interview data delivered multiple major themes that depict nurses’ personal situations and challenges during ethical dilemmas in critical care environments. The summarized analysis of essential topics appears in the following table.
| Theme | Description | Frequency (%) |
| Moral Distress and Emotional Impact | Nurses expressed feelings of stress, guilt, and anxiety when making difficult ethical decisions, particularly related to end-of-life care. | 9 (90%) |
| Institutional Support and Resources | Nurses reported that formal institutional support, such as ethics committees, was available but often felt insufficient to address the complexities of dilemmas. | 7 (70%) |
| Communication with Families | Nurses emphasized the need for clear, compassionate communication with families but also noted challenges, especially in cases of conflicting opinions. | 8 (80%) |
| Ethical Decision-Making Autonomy | Nurses had mixed experiences with decision-making autonomy, with some feeling empowered and others constrained by hospital policies or medical hierarchy. | 6 (60%) |
| Coping with Moral Conflicts | Nurses often relied on personal values, peer support, and reflective practices to cope with ethical dilemmas, but some felt isolated in dealing with complex issues. | 7 (70%) |
Table 3: Key themes from qualitative interviews (N = 10)
Discussion
The research investigated the ethical issues that critical care nurses at Saidu Teaching Hospital experience, as well as the recurring patterns and specific situations that result in emotional effects on their coping approaches. Ethical dilemmas commonly occur in critical care areas because nurses frequently experience problems regarding end-of-life care decisions, life-support withholding, and family-patient conflicts. Nurses have developed major emotional and psychological harm from their daily ethical challenges, although existing institutional support systems failed to meet their needs adequately.[19]
Ethical dilemmas in critical care: The study highlights the wide occurrence of ethical dilemmas that nurses must handle. A representative number of nurses (26%) experienced end-of-life decision-making difficulties on a consistent basis, according to survey results, with equal proportions (22%) reporting problems related to withholding life-sustaining treatment, along with 14% facing conflicts with family members. Research data from other studies indicates that critical care staff experience these exact ethical problems. Critical care nurses face ethical problems when managing life-supporting treatment and guiding end-of-life care decisions in their clinical practice. Many ICU staff find disagreement with families about treatment approaches to be one of the most important ethical challenges they face.[20]
The nurses in this research faced ethical problems mainly because they needed to balance respecting patient choice against acting in accordance with the principle of beneficence that underlies nursing ethics. Critical care nurses develop moral distress through conflicts they notice between what patients want and their professional judgment regarding essential care decisions for critical patients.[21] Young nursing professionals showed signs of moral distress by expressing guilt and experiencing anxiety, together with stress, while deciding not to sustain patients with critical treatments.[22]
Emotional and psychological impact: The emotional and psychological burden from ethical dilemmas proved extensive by survey results because 16% of nurses disclosed having “extremely high” stress levels when making such choices. Of the respondents, 30% described their stress levels as moderate. The study results match previous research that showed critical care nurses experience severe moral distress, together with emotional strain, during ethical conflicts.[23] The intricate, high-consequence patient care environment at critical care units worsens the emotional burden nurses face when they need to combine their technical skills with emotional intelligence for decision-making.[24]
The study participants demonstrated moral distress symptoms that also surfaced in different research reports. Moral distress develops primarily in nursing staff who participate in end-of-life choices, especially when they receive insufficient support from physicians and hospital guidelines during decision-making processes. Staff members experienced distress at elevated levels, especially when deciding either to withhold or withdraw life-sustaining medical treatments.[25] Ethical dilemmas encountered by nurses frequently produce a state of moral conflict while causing emotional distress due to their obligation to support patients while following medical protocols.[26]
Coping mechanisms: The nurses in this study managed their ethical issues through numerous different coping methods. Nurses stated they used the most frequent coping strategies, which included asking colleagues for help at 80% and receiving support from senior staff or medical team at 70%, as well as using their individual ethical values at 60%. The respondents used reflective practice (50%), followed by attendance at ethics committee meetings (30%), as their coping strategies. Studies from the past have validated peer support and reflective practice as primary coping strategies nurses utilize to handle moral distress during critical care shifts.[27]
Nurses depend heavily on peer interaction to manage their emotional responses towards ethical conflicts encountered at work. When nurses openly communicate with colleagues and their senior staff, they have chances to review complicated cases or obtain guidance and manage their emotional strain. The nurses emphasized reflective practice as a crucial tool because it enables them to process complex ethical situations, thus minimizing their emotional distress. The findings support healthcare ethics research showing that supportive work areas and team-based decision processes reduce ethical work-related pressures.[28]
Although a considerable number of nurses relied on coping measures, research indicates that institutional structures failed to supply adequate support for nurses. The study revealed insufficient ethical training access, since only 40% of nurses possessed this training, whereas 30% noted that ethics committees lacked accessibility or were not employed effectively. Research evidence shows that critical care institutions should strengthen their support structures for nursing staff.[29] Ethics committees exist in most hospitals, yet their practical utilization remains inconsistent. Nurses typically experience professional isolation in complex ethical situations because of insufficient institutional training and commitment.[30]
Institutional support and training: The nurses surveyed revealed different amounts of institutional support for ethical decision-making, since 70% declared the availability of ethics committees, but their assistance was inconsistent. The survey results showed that 40% of nurses believed their institution lacked adequate education on ethical matters. The reported support data reveals that critical care units require stronger backing from their institutions.[31] The regular training and active participation of ethics committee members help reduce moral distress and provide framework-based ethical decision-making resources for nurses. The proposed improvements function to decrease nurses’ emotional strain while simultaneously improving their ethical judgments in critical situations.[32]
The research evidence shows that ethical training alongside institutional backing is fundamental to critical care nursing environments. Nurses require access to training programs about ethical challenges they encounter in their work, which should be combined with frequent contact between nurses and ethics committee members for support.[33] Institutions that develop their resources to support ethical practice will create better ethical environments and lessen nurses’ emotional turmoil when making decisions in critical care.
Recommendations: The following strategies enable healthcare institutions to help critical care nurses produce ethical decisions, which in turn enhance patient care results in ICU settings.
- Implementation of Regular Ethics Training: Nursing programs at hospitals need to establish essential ethics training for all students to develop effective ethical choices.
- Formation of Ethical Support Committees: The creation of ethical committees inside hospitals provides medical staff with systematic procedures to solve difficult ethical medical matters.
- Encouraging Open Communication: The healthcare facility must encourage interdisciplinary team discussions and debrief sessions as a fundamental strategy to handle ethical dilemmas properly.
- Institutional Policy Development: The institution should create definitive policies together with practical guidelines to help nurses resolve ethical problems safely.
- Psychosocial Support for Nurses: Nurses should receive access to counseling services combined with peer support groups that assist their ability to manage moral distress.
Conclusion
This study demonstrates vital information about the moral challenges experienced by critical care nurses, combined with their resulting emotional and psychological impact. The exam’s ethical challenges in critical care nursing matched findings from other research concerning end-of-life decisions, family disagreements, and resource distribution dilemmas. The nursing staff adopts peer support together with reflective practice as coping mechanisms, but they feel their workplace does not provide sufficient support. Healthcare facilities must develop strong ethical training programs while enhancing their ethics commissions’ accessibility and efficiency to minimize nurses’ moral distress. The resolution of identified ethical problems should decrease emotional strain among critical care nurses and improve ethical decision-making within high-risk hospital wards.
References
- Alshahrani IHF. Ethical considerations in respiratory therapy and nursing practice: Balancing patient autonomy and care. Tuijin Jishu. 2024;45(04):2369-2376 Ethical Considerations in Respiratory Therapy and Nursing Practice: Balancing Patient Autonomy and Care
- Barakat-Johnson M, Barnett C, Wand T, White K. Knowledge and Attitudes of Nurses Toward Pressure Injury Prevention: A Cross-Sectional Multisite Study. J Wound Ostomy Continence Nurs. 2018;45(3):233-237. doi:10.1097/WON.0000000000000430 PubMed | Crossref | Google Scholar
- Huerta-González S, Caro-Alonso PÁ, Rodríguez-Martín B, et al. Nurses’ perceptions of the performance of nurse managers and senior hospital management during the COVID-19 pandemic. BMC Nurs. 2024;23(1):455. doi:10.1186/s12912-024-02123-4 PubMed | Crossref | Google Scholar
- Mwirigi PK. Doctors’ and Nurses’ Experiences of Ethical Challenges in End of Life Decisions in Critical Care Unit at Kenyatta National Hospital. Doctoral dissertation. University of Nairobi; 2020. Doctors’ and Nurses’ Experiences of Ethical Challenges in End of Life Decisions in Critical Care Unit at Kenyatta National Hospital (doctoral dissertation)
- Cherry B, Jacob SR. Contemporary Nursing E-Book: Issues, Trends, & Management. Elsevier Health Sciences; 2021. Contemporary Nursing Elsevier eBook on VitalSource, 9th Edition
- Kalaycioglu O, Sert-Ozen A, Yeşildağ A. To stay or leave? Consequences of ethical dilemma experienced by nurses in the intensive care units. J Bus Ethics. 2024. doi:10.1007/s10551-024-05915-5 Crossref | Google Scholar
- Atashzadeh-Shoorideh F, Tayyar-Iravanlou F, Chashmi ZA, Abdi F, Cisic RS. Factors affecting moral distress in nurses working in intensive care units: A systematic review. Clin Ethics. 2021;16(1):25-36. doi:10.1177/1477750920927174 Crossref | Google Scholar
- Khanal A, Franco-Correia S, Mosteiro-Diaz MP. Ethical conflict among critical care nurses during the COVID-19 pandemic. Nurs Ethics. 2022;29(4):819-832. doi:10.1177/09697330211066574 PubMed | Crossref | Google Scholar
- Ricciardelli R, Johnston MS, Bennett B, Stelnicki AM, Carleton RN. “It Is Difficult to Always Be an Antagonist”: Ethical, Professional, and Moral Dilemmas as Potentially Psychologically Traumatic Events among Nurses in Canada. Int J Environ Res Public Health. 2022;19(3):1454. doi:10.3390/ijerph19031454 PubMed | Crossref | Google Scholar
- Munkeby H, Moe A, Bratberg G, Devik SA. ‘Ethics Between the Lines’ – Nurses’ Experiences of Ethical Challenges in Long-Term Care. Glob Qual Nurs Res. 2022;8:23333936211060036. doi:10.1177/23333936211060036
PubMed | Crossref | Google Scholar - Kelley MM, Zadvinskis IM, Miller PS, et al. United States nurses’ experiences during the COVID-19 pandemic: A grounded theory. J Clin Nurs. 2022;31(15-16):2167-2180. doi:10.1111/jocn.16032 PubMed | Crossref | Google Scholar
- Madni A, Levine DR, Sawyer KE, et al. Impacts of ethical dilemmas and moral distress in pediatric hematology oncology nurses. Pediatr Blood Cancer. doi:10.1002/pbc.31546 PubMed | Crossref | Google Scholar
- Sanderson C, Sheahan L, Kochovska S, et al. Re-defining moral distress: A systematic review and critical re-appraisal of the argument-based bioethics literature. Clin Ethics. 2019;14(4):195-210. doi:10.1177/1477750919886088 Crossref | Google Scholar
- Voget U. Professional nurses’ lived experiences of moral distress at a district hospital. 2017. Professional nurses’ lived experiences of moral distress at a district hospital
- Silverman HJ, Kheirbek RE, Moscou-Jackson G, Day J. Moral distress in nurses caring for patients with Covid-19. Nurs Ethics. 2021;28(7-8):1137-1164. doi:10.1177/09697330211003217 PubMed | Crossref | Google Scholar
- Rushton CH, Swoboda SM, Reller N, et al. Mindful Ethical Practice and Resilience Academy: Equipping Nurses to Address Ethical Challenges. Am J Crit Care. 2021;30(1):e1-11. doi:10.4037/ajcc2021359
PubMed | Crossref | Google Scholar - Halvorsen K, Jensen JF, Collet MO, et al. Patients’ experiences of well‐being when being cared for in the intensive care unit—An integrative review. J Clin Nurs. 2022;31(1-2):3-19. doi:10.1111/jocn.15910
PubMed | Crossref | Google Scholar - Morley G, Copley DJ, Field R, Zelinsky M, Albert NM. RESPONDER: A qualitative study of ethical issues faced by critical care nurses during the COVID-19 pandemic. J Nurs Manag. 2022;30(7):2403-2415. doi:10.1111/jonm.13792
PubMed | Crossref | Google Scholar - Nikbakht Nasrabadi A, Wibisono AH, Allen KA, Yaghoobzadeh A, Bit-Lian Y. Exploring the experiences of nurses’ moral distress in long-term care of older adults: a phenomenological study. BMC Nurs. 2021;20(1). doi:10.1186/s12912-021-00675-3 PubMed | Crossref | Google Scholar
- Guttormson JL, Calkins K, McAndrew N, Fitzgerald J, Losurdo H, Loonsfoot D. Critical Care Nurses’ Experiences During the COVID-19 Pandemic: A US National Survey. Am J Crit Care. 2022;31(2):96-103. doi:10.4037/ajcc2022312
PubMed | Crossref | Google Scholar - St Ledger U, Reid J, Begley A, et al. Moral distress in end-of-life decisions: A qualitative study of intensive care physicians. J Crit Care. 2021;62:185-189. doi:10.1016/j.jcrc.2020.12.019 PubMed | Crossref | Google Scholar
- De Brasi EL, Giannetta N, Ercolani S, et al. Nurses’ moral distress in end-of-life care: A qualitative study. Nurs Ethics. 2021;28(5):614-627. doi:10.1177/0969733020964859 PubMed | Crossref | Google Scholar
- Romero-García M, Delgado-Hito P, Gálvez-Herrer M, et al. Moral distress, emotional impact and coping in intensive care unit staff during the outbreak of COVID-19. Intensive Crit Care Nurs. 2022;70:103206. doi:10.1016/j.iccn.2022.103206 PubMed | Crossref | Google Scholar
- Beheshtaeen F, Torabizadeh C, Khaki S, Abshorshori N, Vizeshfar F. Moral distress among critical care nurses before and during the COVID-19 pandemic: A systematic review. Nurs Ethics. 2024;31(4):613-634. doi:10.1177/09697330231221196 PubMed | Crossref | Google Scholar
- Choi HR, Ho MH, Lin CC. Navigating tensions when life‐sustaining treatment is withdrawn: A thematic synthesis of nurses’ and physicians’ experiences. J Clin Nurs. 2024;33(6):2337-2356. doi:10.1111/jocn.17059
PubMed | Crossref | Google Scholar - Gristina GR. Withholding or withdrawing life-sustaining treatments. In: Palliative Care in Cardiac Intensive Care Units. Springer International Publishing; 2021:99-112 Withholding or Withdrawing Life-Sustaining Treatments
- Mutschler C, Bellamy C, Davidson L, Lichtenstein S, Kidd S. Implementation of peer support in mental health services: A systematic review of the literature. Psychol Serv. 2022;19(2):360-374. doi:10.1037/ser0000531
PubMed | Crossref | Google Scholar - Tsarouha E, Preiser C, Weltermann B, et al. Work-Related Psychosocial Demands and Resources in General Practice Teams in Germany. A Team-Based Ethnography. Int J Environ Res Public Health. 2020;17(19):7114. doi:10.3390/ijerph17197114 PubMed | Crossref | Google Scholar
- Göbert P, Blanckenburg P von, Maier RF, Seifart C. Utilization and evaluation of ethics consultation services in neonatal intensive care. Children (Basel). 2024;11(11):1349. doi:10.3390/children11111349 PubMed | Crossref | Google Scholar
- Schulz I, O’Neill J, Gillam P, Gillam L. The scope of ethical dilemmas in paediatric nursing: a survey of nurses from a tertiary paediatric centre in Australia. Nurs Ethics. 2023;30(4):526-541. doi:10.1177/09697330231153916
PubMed | Crossref | Google Scholar - Smith HAB, Besunder JB, Betters KA, et al. 2022 Society of Critical Care Medicine Clinical Practice Guidelines on Prevention and Management of Pain, Agitation, Neuromuscular Blockade, and Delirium in Critically Ill Pediatric Patients With Consideration of the ICU Environment and Early Mobility. Pediatr Crit Care Med. 2022;23(2):e74-110. doi:10.1097/PCC.0000000000002873 PubMed | Crossref | Google Scholar
- Chemali S, Mari-Sáez A, El Bcheraoui C, Weishaar H. Health care workers’ experiences during the COVID-19 pandemic: a scoping review. Hum Resour Health. 2022;20(1):27. doi:10.1186/s12960-022-00724-1
PubMed | Crossref | Google Scholar - Haahr A, Norlyk A, Martinsen B, Dreyer P. Nurses experiences of ethical dilemmas: A review. Nurs Ethics. 2020;27(1):258-272. doi:10.1177/0969733019832941 PubMed | Crossref | Google Scholar
Acknowledgments
Not reported
Funding
Not reported
Author Information
Corresponding Author:
Shah Hussain
Department of Nursing
Zalan College of Nursing Swat, Pakistan
Email: shahpicu@gmail.com
Co-Authors:
Atta Ullah
Department of Nursing
Janbar College of Nursing and Allied Health Sciences, Swat, Pakistan
Arif Ullah
Department of Quality Improvement & Patient Safety
Lady Reading Hospital, Peshawar, Pakistan
Authors Contributions
Shah Hussain was responsible for data collection, data analysis, and manuscript write-up. Atta Ullah contributed to data collection and statistical analysis. Arif Ullah handled data collection and thematic analysis.
Ethical Approval
Ethical approval was obtained from the ethical committee of Saidu Teaching Hospital Ref. No SGTH/ 2024/45, verbal consent was obtained from the head of the department of the critical area and participants.
Conflict of Interest Statement
Not reported
Guarantor
None
DOI
Cite this Article
Shah H, Atta U, Arif U. Nurses’ experiences with ethical dilemmas in critical care settings: A mixed-method study at Saidu Teaching Hospital. medtigo J Med. 2025;3(1):e30623135. doi:10.63096/medtigo30623135 Crossref









