Author Affiliations
Abstract
Introduction: Metal bezoars are a rare form of bezoar that are usually found in the stomach but may be found anywhere in the gastrointestinal tract (GIT). This condition is often seen in psychiatric patients and can even present with perforation and peritonitis. Only a few case reports of large metal bezoars have been reported to date.
Case presentation: An 18-year-old gentleman with psychiatric illness presented to the emergency department due to hollow viscus perforation peritonitis after intentionally ingesting multiple foreign bodies (metal bezoars). There was a history of head injury 2 years ago, resulting in disturbed mental status. Plain Radiograph of chest (erect view) showed multiple metallic objects with dilated stomach and free air under the diaphragm. Emergency exploratory laparotomy with gastrotomy and primary repair of gastric perforation was performed and post-operative period uneventful.
Conclusion: Metal bezoars have been associated with several gastrointestinal complications. Early diagnosis and treatment are important for the prevention of morbidity and mortality. Although emergency exploratory laparotomy is the treatment of choice in case of perforation peritonitis, pharmacotherapy and behavioral assessment play a vital role in the overall care of the patient to prevent recurrence.
Keywords
Bezoar, Gastrotomy, Laparotomy, Peritonitis, Blood investigations.
Introduction
Bezoars are accumulations of ingested foreign bodies forming a hard mass or concretion in the GIT, most commonly in the stomach.[1] This condition is rare and causes a wide variety of signs and symptoms. Patient can be asymptomatic and diagnosed incidentally during upper gastrointestinal endoscopy or imaging, and at times may present with obstruction or even perforation. Several types of bezoars are classified based on their composition. Phytobezoar is the most common type of gastric bezoar, composed of ingested vegetative materials. Other forms include trichobezoar (ingestion of hair), pharmacobezoar (medications), and lactobezoars. Metal bezoar, though rare, has also been reported in the literature. Majority of people with this disorder have associated psychiatric illnesses such as depression, anxiety, and psychosis, and they subsequently feel pleasure and gratification in doing so.[2,3] Here, we present a case of multiple gastric bezoars in a psychiatric patient who was operated on for gastric perforation and peritonitis.
Case Presentation
An 18-year-old male with a history of chronic psychosis and personality disorder presented to the emergency department with acute generalized, severe abdominal pain following ingestion of multiple foreign bodies (metals, nails, plastic stuff). He had a history of traumatic brain injury two years earlier, associated with neurological findings with impaired higher mental function, and had a history of ingestion of bezoars since then. On examination, he looked unwell, with blood pressure of 100/60 mmHg, pulse of 100/min, and respiratory rate of 22/min. His abdomen was distended with generalized tenderness and rebound tenderness, guarding, and rigidity. Bowel sounds were sluggish, liver dullness was obliterated, and bilateral hernial orifices were intact. Digital rectal examination findings were unremarkable. Higher mental status was not intact (poor judgment and memory). Based on these clinical findings, the patient was admitted with a provisional diagnosis of peritonitis secondary to bowel perforation.
Blood investigations showed total white blood cell counts of 17,300 mm3 with 90% neutrophils. Hemoglobin level was 9.1 g/dL, serum urea, creatinine, and electrolyte levels were normal. Erect chest radiograph showed multiple radiopaque foreign bodies in the epigastrium and right upper quadrant, a grossly dilated stomach, and both domes of the diaphragm showed free gas under the diaphragm (Figure 1).
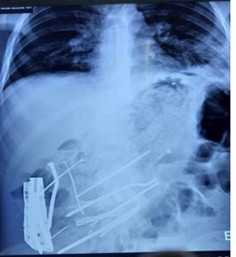
Figure 1: Radiograph showing multiple metal Bezoar
Case Management
The patient underwent emergency exploratory laparotomy. Intraoperative findings were a single perforation (0.7 x 0.7cm) on the anterior stomach wall (Figure 3) and multiple foreign bodies, including metals, plastic, and clothing fabric, in the stomach (Figure 2 ). A gastrotomy was required for removal of foreign bodies, followed by primary repair of gastric perforation with peritoneal lavage and intra-abdominal drain placement. The patient was managed in a post-operative ward for 3 days and then transferred to the general surgical ward. No intraoperative and immediate post-operative complications were noted. Regular dressing of the wound was done, and the patient was discharged on the 7th post-operative day. Psychiatric consultation was done before the discharge. |He was then followed up at 15th, 28th, 3 months, and 6 months periods and had no surgical complications, and his psychiatric complaints were well controlled with regular psychiatric medications.


Figure 2 : Plastic and metallic items retrieved from patient’s stomach
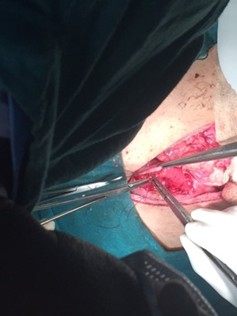
Figure 3: Perforation on anterior Wall of stomach
Discussion
Metal bezoars are extremely rare. Several cases have been reported.[1-6] with different types of presentations (acute, chronic, and asymptomatic). Majority of them presented with an acute abdomen. However, very few cases have been reported for multiple bezoars in the stomach with perforation and peritonitis.
Bezoars are usually intentionally ingested by patients. However, certain risk factors predispose to gastric bezoars, such as decreased gastric motility, history of previous gastrectomy, hypothyroidism, and drugs (laxatives, antipsychotics, calcium channel blockers).[4,7] Composition of the ingested material plays an important role in the pathogenesis. In the past, it was thought to be due to delayed gastric emptying. However, studies showed normal or accelerated gastric emptying in many patients.
Metal bezoars, which are radiopaque, are usually diagnosed on abdominal radiographs. However, the investigation of choice in non-perforated cases to confirm gastric bezoars includes upper GI endoscopy, which in some uncomplicated cases can also be therapeutic. Diagnostic modalities like ultrasound and computerized tomography (CT) scan are available. CT scans are more accurate methods for the diagnosis of gastric bezoars.[8] GI endoscopic techniques are considered the diagnostic methods for gastric bezoars and have some therapeutic value.[9]
The main goals of bezoar treatment are the removal of the bezoar and the prevention of its recurrence. There are different treatment methods based on presentation: chemical dissolution, endoscopic removal, or surgery. Recent study regarding endoscopic removal for upper GI bezoars showed a success rate of 86.5% as compared to 13.5% in open surgery.[10] Several agents have been used for chemical dissolution, such as Coca-Cola, cellulase, and papain. Endoscopic removal has been tried for trichobezoar and small metal bezoar.[11]
Laparotomy is indicated in cases of large metal bezoars and those presenting with perforation peritonitis, and it has shown good results in most of the bezoars, including our case. Recurrent bezoar has been reported in up to 14% of cases, which is associated with psychiatric illness as well as conditions related to gastric emptying.[12,13] Dietary modification and increased water intake to prevent recurrence in cases of altered gastric motility. The management of existing psychiatric illness can help prevent relapses.
Conclusion
Bezoars, though rare, are a potentially serious problem. Although laparotomy is frequently required to manage bezoars and their complications, the role of pharmacotherapy and psychological interventions is crucial.
References
- Chahine E, El Khoury L, Baghdady R, Chouillard E. Recurrent gastric metal bezoar: a rare cause of gastric outlet obstruction. BMJ Case Rep. 2017;2017:bcr2017221928. doi:10.1136/bcr-2017-221928 Pubmed | Crossref | Google Scholar
- Guze SB. Diagnostic and Statistical Manual of Mental Disorders, 4th ed. (DSM-IV). Am J Psychiatry.1995;152(8):1228. doi:10.1176/ajp.152.8.1228 Crossref | Google Scholar
- Siddiqui ZU. Metal bezoars causing upper gastrointestinal obstruction in a schizophrenic. APSP J Case Rep. 2011;2(2):14 Metal bezoars causing upper gastrointestinal obstruction in a schizophrenic
- Eng K, Kay M. Gastrointestinal bezoars: history and current treatment paradigms. Gastroenterol Hepatol (N Y). 2012;8(11):776-778 Pubmed | Google Scholar
- Kumar GS, Amar V, Ramesh B, Abbey RK. Bizarre metal bezoar: a case report. Indian J Surg. 2013;75(Suppl 1):356-358. doi:10.1007/s12262-012-0706-2 Pubmed | Crossref | Google Scholar
- Márquez-Rojas J, Roldán-Baños S, López-Guerra D, Onieva-González FG, Jiménez-Redondo JL, Leal-Macho A. Bezoar por ingestión de cuerpos extraños metálicos (Bezoar after ingestion of metallic foreign bodies). Cir Cir. 2011;79(5):464-467 Pubmed | Google Scholar
- Mehta HM, Mehta MN. Pharmacobezoars: A rare entity. Am J Pharmacol Pharmacother. 2016;3(3):25-27 Pharmacobezoars: A Rare Entity
- Ripollés T, García-Aguayo J, Martínez MJ, Gil P. Gastrointestinal bezoars: sonographic and CT characteristics. AJR Am J Roentgenol. 2001;177(1):65-69. doi:10.2214/ajr.177.1.1770065 Pubmed | Crossref | Google Scholar
- Wang YG, Seitz U, Li ZL, Soehendra N, Qiao XA. Endoscopic management of huge bezoars. Endoscopy. 1998;30(4):371-374. doi:10.1055/s-2007-1001285 Pubmed | Crossref | Google Scholar
- Gökbulut V, Kaplan M, Kaçar S, Akdoğan Kayhan M, Coşkun O, Kayaçetin E. Bezoar in upper gastrointestinal endoscopy: A single center experience. Turk J Gastroenterol. 2020;31(2):85-90. doi:10.5152/tjg.2020.18890 Pubmed | Crossref | Google Scholar
- Saeed ZA, Ramirez FC, Hepps KS, Dixon WB. A method for the endoscopic retrieval of trichobezoars. Gastrointest Endosc. 1993;39(5):698-700. doi:10.1016/s0016-5107(93)70226-6 Pubmed | Crossref | Google Scholar
- Robles R, Parrilla P, Escamilla C, et al. Gastrointestinal bezoars. Br J Surg. 1994;81(7):1000-1001. doi:10.1002/bjs.1800810723 Pubmed | Crossref | Google Scholar
- Calabuig R, Navarro S, Carrió I, Artigas V, Monés J, Puig LaCalle J. Gastric emptying and bezoars. Am J Surg. 1989;157(3):287-290. doi:10.1016/0002-9610(89)90552-7 Pubmed | Crossref | Google Scholar
Acknowledgments
We would like to acknowledge our patient and the Bir Hospital Surgery team for the successful surgery.
Funding
None
Informed consent
We obtained an informed consent form from the patient and his father.
Author Information
Corresponding Author:
Archana KC
Department of General Surgery
Bir Hospital, Kathmandu, Nepal
Email: kcarchana0511@gmail.com
Co-Authors:
Kishor K Deo
Department of General Surgery
Bir Hospital, Kathmandu, Nepal
Binod Dangal
Department of General Practice
Medical Director
Tsho-Rolpa General Hospital, Dolokha, Nepal
Authors Contributions
All authors contributed to the conceptualization, investigation, and data curation by acquiring and critically reviewing the selected articles. They were collectively involved in the writing – original draft preparation, and writing – review & editing to refine the manuscript. Additionally, all authors participated in the supervision of the work, ensuring accuracy and completeness. The final manuscript was approved by all named authors for submission to the journal.
Conflict of Interest Statement
None
Guarantor
None
DOI
Cite this Article
Archana K, Kishor KD, Binod D. Multiple gastrointestinal bezoars—An unusual cause of perforation peritonitis. medtigo J Med. 2024;2(4):e30622442. doi:10. 63096/medtigo30622442 Crossref









