Author Affiliations
Abstract
Background: Polycystic ovary syndrome (PCOS) is an endocrine disorder that is the most common among women of reproductive age; global prevalence estimates range from 2% to 26%. The low-public-awareness level, despite its prevalence, may retard early diagnosis and adequate management. Objective: To assess the knowledge and health-related practices regarding PCOS among diagnosed young women attending the gynecology department in Muzaffarabad, Azad Jammu & Kashmir (AJK), Pakistan.
Methodology: This cross-sectional study was conducted prospectively at the Combined Military Hospital (CMH) Muzaffarabad from August to October 2024. Convenience sampling was used to recruit 200 patients. Data was collected through a structured questionnaire that included demographic information, knowledge regarding PCOS, and health behaviors. SPSS version 25 software facilitated data analysis with descriptive and inferential statistics for assessing knowledge and health habits related to PCOS.
Results: The mean knowledge score on PCOS was 9.8 (SD = 3.2). While participants demonstrated high awareness of core symptoms like ovarian cysts (90.5%), hirsutism (81.0%), and hair loss (80.0%), significant knowledge gaps were identified regarding metabolic risks (e.g., pre-diabetes, 18.5%) and the association with irregular menstruation (26.5%). The study also found that information gaps can lead to late diagnosis and higher health risk.
Conclusion: This study revealed that diagnosed young women in Muzaffarabad generally possess knowledge of core PCOS symptoms. However, significant deficits exist concerning the disorder’s full spectrum, particularly its metabolic complications and the fundamental link to irregular menstruation. Focused educational approaches, specifically tailored for diagnosed patients, are needed to improve comprehensive understanding and health outcomes.
Keywords
Polycystic ovarian syndrome, Knowledge, Symptoms, Women, Health-related practice.
Introduction
PCOS is one of the most common endocrine disorders in reproductive-aged women, affecting 2% to 26% of women worldwide.[1] Recent research in Pakistan has reported the prevalence of PCOS symptoms in 20.7% of women, and as such, PCOS is a major health issue. PCOS, initially described by Stein and Leventhal in 1935, is composed of a combination of hormonal disturbances that lead to ovarian dysfunction, hyperandrogenism, and metabolic disturbances. The clinical diagnosis can be confirmed using the Rotterdam criteria, as they require at least two of the following: oligo-anovulation, clinico/biochemical hyperandrogenism, or ultrasonographic presence of polycystic ovaries.[2-4]
The etiology of PCOS is multifactorial, including genetic, environmental, and lifestyle factors. Evidence signifies a strong hereditary tendency, with instances clustering and PCOS being particularly prevalent among first-degree relatives.[5] Environmental factors, particularly modern lifestyle changes, have contributed to the disorder. The increased consumption of processed foods and sugary beverages is a disruptive trend, as it incorporates obesity, a major risk factor for insulin resistance and metabolic issues related to PCOS.[6] PCOS symptoms vary and can have a substantial influence on quality of life. Common symptoms of PCOS include irregular menstrual cycles, infertility, hirsutism, acne, and obesity.[7,8] Studies show that around 70-80% of women with PCOS struggle with infertility due to anovulation.[9] Additionally, women with PCOS face a higher risk of developing serious health issues like type 2 diabetes, dyslipidemia, endometrial cancer, and cardiovascular disease. Research indicates that women with PCOS are three times more likely to develop type 2 diabetes compared to those who don’t have the condition.[10]
It is particularly alarming that even though PCOS is so prevalent and can be the trigger of serious health issues if left untreated, public awareness is still low. A study has revealed that more than 25% of the gynecologists and reproductive endocrinologists did not recognize PCOS diagnostic criteria, which indicates that there is a huge gap in knowledge among healthcare professionals. The fact that a significant number of women with PCOS feel their needs are unmet underscores the urgent need for more comprehensive and effective educational initiatives. Given the unique socio-cultural and healthcare access landscape of Muzaffarabad, AJK, the present research aims to investigate the level of knowledge and health behaviors among diagnosed young women presenting at a clinical setting. By identifying specific knowledge deficits and behavioral patterns within this context, this study seeks to provide targeted recommendations to improve proper management and patient education for PCOS in this particular cohort.
Methodology
The cross-sectional survey was carried out in the Gynaecology department of CMH, Muzaffarabad, from October 2023 to August 2024. We recruited 200 women using a convenience sampling method, primarily contacting patients already attending the department. This approach allowed for efficient data collection within the timeframe. However, it is crucial to acknowledge that this convenience sampling, focusing on a clinical population (88% of participants were already diagnosed with PCOS), inherently introduces selection bias. Therefore, the findings of this study are specific to this diagnosed patient cohort and may not be generalizable to the broader population of young women in Muzaffarabad. While statistical significance was achieved for various correlations within this sample, this does not negate the external validity limitations posed by the sampling method.
We used a well-designed questionnaire, derived from previous studies, to collect our data. The questionnaire was neatly divided into four segments.3 Each segment had a clear focus, and the overall title of the four segments addressed the awareness of participants concerning PCOS and their health behavior. The first segment had 20 well-crafted questions concerning the knowledge base of the participants. The questions were all direct and solicited clear answers. There was no room for the participants to misunderstand what was being asked. The questions themselves had good face validity; they appeared to measure what they were supposed to measure (knowledge of PCOS). The second segment had 12 questions that were essentially a checklist for the participants to indicate whether they had certain clinical symptoms associated with PCOS. The third segment had 10 direct behavior-based questions. These questions solicited participants’ health behavior concerning a few areas that are known to impact the health of individuals with PCOS.
Results
This study included a survey of 200 young women whose health behaviors and understanding of PCOS were being investigated. Demographic data showed that 72% of respondents were unmarried and 65% were unemployed. Surprisingly, about 91% of them lived in urban areas, and the majority had at least one degree. In addition, a significant portion of respondents reported being exempt from any chronic ailments, which indicates that this population is generally healthy.
| Demographic characteristics | Frequency (N = 200) | Percentage |
| Age group (years) 17-20 21-29 31-39 > 40 |
28 124 32 16 |
14% 62% 16% 8% |
| Marital status Unmarried Married Widow Divorced |
144 50 3 3 |
72% 25% 1.5% 1.5% |
| Employment Employed Unemployed |
70 130 |
35% 65% |
| Education Primary High school Graduation Post-graduation |
24 38 132 10 |
12% 19% 66% 5% |
| Residence Rural Urban |
18 182 |
9% 91% |
| BMI (kg/m2) <18.518.5–24.9 25.0–29.9 |
39 108 53 |
19.5% 54% 26.5% |
| Chronic disease Yes No |
47 153 |
23.5% 76.5% |
| Diagnosed PCOS Yes No |
176 24 |
88% 12% |
Table 1: Sociodemographic factors and Background of the participants
Participants’ understanding of PCOS was assessed using a 20-item questionnaire (Table 2). The mean knowledge score was 9.8 (SD = 3.2), with scores ranging from 2 to 16. This distribution was nearly normal (skewness = -0.2, kurtosis = -0.5). While the overall mean score suggests a moderate level of knowledge, a more detailed analysis reveals important nuances among this largely diagnosed population. Many participants demonstrated high awareness of core concepts and symptoms, for instance, the presence of ovarian cysts (90.5%), hirsutism (81.0%), the link to hair loss (80.0%), and the risks of diabetes (72.5%) and heart disease (77.5%). However, significant knowledge gaps were identified regarding more complex associations, such as between PCOS and pre-diabetes (18.5% correct). Furthermore, a surprisingly low percentage (26.5% correct) identified irregular or absent menstrual cycles as a symptom, a fundamental characteristic of PCOS, warranting further investigation into the reasons for this specific deficit.
| Question | Response | Frequency | Percentage |
| 1. Have you heard about the term called “polycystic ovary syndrome (PCOS)”? | Correct | 148 | 74.0% |
| Incorrect | 32 | 16.0% | |
| Don’t Know | 20 | 10.0% | |
| 2. Have you heard about the androgen (male) hormone? E.g. testosterone | Correct | 175 | 87.5% |
| Incorrect | 25 | 12.5% | |
| 3. In PCOS, there is an increased level of androgens level | Correct | 148 | 74.0% |
| Incorrect | 18 | 9.0% | |
| Don’t Know | 34 | 17.0% | |
| 4. Patients suffering from PCOS have multiple small cysts in their ovaries | Correct | 181 | 90.5% |
| Incorrect | 19 | 9.5% | |
| 5. Obesity may cause PCOS | Correct | 164 | 82.0% |
| Don’t Know | 36 | 18.0% | |
| 6. Pre-diabetes condition (due to decreased insulin action in the body) may cause PCOS | Correct | 37 | 18.5% |
| Incorrect | 123 | 61.5% | |
| Don’t Know | 40 | 20.0% | |
| 7. Irregular or absence of menstrual (periods) cycle is a symptom of PCOS | Correct | 53 | 26.5% |
| Incorrect | 111 | 55.5% | |
| Don’t Know | 36 | 18.0% | |
| 8. An unusual amount of hair growth on different body parts (upper lip, chin, abdomen, breast, thighs, etc.) is a symptom of PCOS | Correct | 162 | 81.0% |
| Don’t Know | 38 | 19.0% | |
| 9. Severe acne problem during the menstrual (periods) cycle is a symptom of PCOS | Correct | 86 | 43.0% |
| Incorrect | 61 | 30.5% | |
| Don’t Know | 53 | 26.5% | |
| 10. Hair loss from the scalp more than normal is a symptom of PCOS | Correct | 160 | 80.0% |
| Incorrect | 6 | 3.0% | |
| Don’t Know | 34 | 17.0% | |
| 11. PCOS diagnosis can be confirmed by vaginal ultrasound | Correct | 149 | 74.5% |
| Incorrect | 13 | 6.5% | |
| Don’t Know | 38 | 19.0% | |
| 12. A specific blood test can be used for the diagnosis of PCOS | Correct | 159 | 79.5% |
| Incorrect | 5 | 2.5% | |
| Don’t Know | 36 | 18.0% | |
| 13. PCOS may lead to diabetes (long-term high blood sugar level) | Correct | 145 | 72.5% |
| Incorrect | 12 | 6.0% | |
| Don’t Know | 43 | 21.5% | |
| 14. PCOS may lead to heart disease | Correct | 155 | 77.5% |
| Incorrect | 23 | 11.5% | |
| Don’t Know | 22 | 11.0% | |
| 15. PCOS may lead to infertility (inability to have children) or reduced fertility (reduced chance of getting pregnant) | Correct | 136 | 68.0% |
| Incorrect | 16 | 8.0% | |
| Don’t Know | 48 | 24.0% | |
| 16. PCOS may lead to anxiety and depression | Correct | 128 | 64.0% |
| Incorrect | 66 | 33.0% | |
| Don’t Know | 6 | 3.0% | |
| 17. Hormonal therapy (oral contraceptives, hormone intrauterine device, etc.) may be used to treat PCOS | Correct | 108 | 54.0% |
| Don’t Know | 92 | 46.0% | |
| 18. Anti-diabetic medications (metformin) may be used to treat PCOS | Correct | 67 | 33.5% |
| Don’t Know | 133 | 66.5% | |
| 19. Symptomatic treatment (clomiphene, letrozole, acne topical cream, spironolactone, etc.) may be given to relieve the symptoms of PCOS | Correct | 148 | 74.0% |
| Incorrect | 6 | 3.0% | |
| Don’t Know | 46 | 23.0% | |
| 20. Surgery may be used to remove ovarian cysts | Correct | 128 | 64.0% |
| Incorrect | 21 | 10.5% | |
| Don’t Know | 51 | 25.5% |
Table 2: Knowledge of PCOS
Health practices were evaluated using a separate scale (Table 3), yielding a mean score of 32.5 (SD = 5.8) and indicating generally moderate health behaviors. The categorization revealed that 70% of participants had moderate practices, 18% had good practices, 10% had poor practices, and 2% had very poor practices. While a high percentage (84%) reported incorporating fruits and vegetables into their diet, other positive behaviors were less common, such as regular exercise, which 61% of participants reported doing rarely.
| Question | Response | Frequency | Percentage |
| 1. How often do you read nutrition labels? | Never | 99 | 49.5% |
| Rarely | 26 | 13.0% | |
| Sometimes | 5 | 2.5% | |
| Usually | 50 | 25.0% | |
| Always | 20 | 10.0% | |
| 2. I incorporate low-fat foods into my diet | Never | 41 | 20.5% |
| Rarely | 7 | 3.5% | |
| Sometimes | 94 | 47.0% | |
| Usually | 42 | 21.0% | |
| Always | 16 | 8.0% | |
| 3. I incorporate low-salt foods into my diet | Never | 6 | 3.0% |
| Rarely | 40 | 20.0% | |
| Sometimes | 121 | 60.5% | |
| Usually | 27 | 13.5% | |
| Always | 6 | 3.0% | |
| 4. I eat five servings of fruits and vegetables per day | Never | 36 | 18.0% |
| Rarely | 12 | 6.0% | |
| Sometimes | 52 | 26.0% | |
| Usually | 78 | 39.0% | |
| Always | 22 | 11.0% | |
| 5. I decrease the amount of refined sugar in my diet | Never | 10 | 5.0% |
| Rarely | 13 | 6.5% | |
| Sometimes | 126 | 63.0% | |
| Usually | 51 | 25.5% | |
| 6. I eat more high-fiber foods | Never | 5 | 2.5% |
| Rarely | 6 | 3.0% | |
| Sometimes | 168 | 84.0% | |
| Usually | 11 | 5.5% | |
| Always | 10 | 5.0% | |
| 7. I eat smaller portions at dinner | Never | 6 | 3.0% |
| Rarely | 19 | 9.5% | |
| Sometimes | 135 | 67.5% | |
| Usually | 24 | 12.0% | |
| Always | 16 | 8.0% | |
| 8. I exercise 30 minutes 5 days a week | Never | 19 | 9.5% |
| Rarely | 122 | 61.0% | |
| Sometimes | 11 | 5.5% | |
| Usually | 20 | 10.0% | |
| Always | 28 | 14.0% | |
| 9. I control my eating on weekends | Never | 26 | 13.0% |
| Rarely | 122 | 61.0% | |
| Sometimes | 28 | 14.0% | |
| Usually | 11 | 5.5% | |
| Always | 13 | 6.5% | |
| 10. It is easy for me to eat a healthy diet | Rarely | 126 | 63.0% |
| Sometimes | 54 | 27.0% | |
| Usually | 19 | 9.5% | |
| Always | 1 | 0.5% |
Table 3: Health-related practice statements
The clinical evaluation (Table 4) revealed a high prevalence of PCOS-related symptoms. A family history of PCOS was reported by 37.0% of participants. Common symptoms included abnormal scalp hair loss (86.5%), hirsutism (60.5%), and continuous abnormal weight gain (55.5%). Menstrual irregularities were also prominent, with 39.5% experiencing heavy menstruation, 38.0% a complete absence of menstruation, and 26.0% prolonged menstrual cycles. Furthermore, 32.0% reported a personal history of diabetes, and 41.0% had a family history of diabetes, highlighting the significant metabolic risk in this cohort.
| Question | Response | Frequency | Percentage |
| 1. History of PCOS in your mother or sister | Yes | 74 | 37.0% |
| No | 90 | 45.0% | |
| I don’t know | 36 | 18.0% | |
| 2. Very heavy periods (more than two pads per day) | Yes | 79 | 39.5% |
| No | 110 | 55.0% | |
| I don’t know | 11 | 5.5% | |
| 3. Prolonged periods (more than 7 days) | Yes | 52 | 26.0% |
| No | 116 | 58.0% | |
| I don’t know | 32 | 16.0% | |
| 4. Complete absence of periods (not at all) | Yes | 76 | 38.0% |
| No | 116 | 58.0% | |
| I don’t know | 12 | 6.0% | |
| 5. Partial absence of periods (not after 28 days) | Yes | 32 | 16.0% |
| No | 74 | 37.0% | |
| I don’t know | 94 | 47.0% | |
| 6. Acne problem during the menstrual cycle | Yes | 45 | 22.5% |
| No | 78 | 39.0% | |
| I don’t know | 77 | 38.5% | |
| 7. Unusual amount of hair loss from the scalp | Yes | 173 | 86.5% |
| I don’t know | 27 | 13.5% | |
| 8. Unusual amount of hair growth at different parts of your body (upper lip, chin, abdomen, breast, thighs, etc.) | Yes | 121 | 60.5% |
| No | 38 | 19.0% | |
| I don’t know | 41 | 20.5% | |
| 9. Discoloration or dark color patches on skin | Yes | 66 | 33.0% |
| No | 96 | 48.0% | |
| I don’t know | 38 | 19.0% | |
| 10. Continuous abnormal weight gain | Yes | 111 | 55.5% |
| No | 71 | 35.5% | |
| I don’t know | 18 | 9.0% | |
| 11. Diabetes | Yes | 64 | 32.0% |
| No | 78 | 39.0% | |
| I don’t know | 58 | 29.0% | |
| 12. Family history of diabetes | Yes | 82 | 41.0% |
| No | 91 | 45.5% | |
| I don’t know | 27 | 13.5% |
Table 4: Clinical evaluation of PCOS
Correlation analysis was used to investigate the association between PCOS knowledge and health practice. The findings were statistically significant, with a positive correlation as r=0.25, r=0.25, r=0.25 and p=0.001, p=0.00, p=0.001. The result shows that increased knowledge about PCOS has a positive association with practicing healthy habits. As participants gained knowledge regarding PCOS, they also tended to adopt healthier behaviors, highlighting the value of education interventions in the promotion of improved health outcomes.
| Variable | PCOS knowledge | Health practices |
| PCOS knowledge | 1.00 | |
| Health practices | 0.25** | 1.00 |
| N | 200 | 200 |
Table 5: Correlations between PCOS knowledge and health practices
Additional analysis involved group comparisons using demographic variables. The residency coefficient was 0.7940.7940.794 with a p-value of less than 0.000, indicating that urban residency increases education levels by 0.794 units significantly. Likewise, the employment coefficient was 0.2460.2460.246, which indicates that employment leads to an increase in education levels by 0.246 units. These results point to the influence of socioeconomic factors on the knowledge and health practices of PCOS.
| Variable | B | SE(B) | β | t | p |
| (Constant) | 20.50 | 3.20 | – | 6.41 | <0.001 |
| PCOS knowledge | 0.20 | 0.05 | 0.24 | 4.00 | <0.001 |
| Residency | 0.794 | 0.087 | 0.484 | 9.108 | <0.001 |
| Employment | 0.246 | 0.055 | 0.250 | 4.464 | <0.001 |
| R<sup>2</sup> | 0.432 |
Table 6: Linear regression predicting health practices from PCOS knowledge, residency, and employment
B = Unstandardized regression coefficient, SE(B) = Standard error of the unstandardized coefficient, β = Standardized regression coefficient (Beta weight), t = t-statistic, p = p-value
The visual depiction demonstrates the conceptual model for appreciating the interrelations among knowledge of PCOS, health-related practices, and health outcomes. It demonstrates the ways that demographic and psychosocial variables intersect with knowledge and practices and, in turn, affect the treatment of PCOS. The model is a guide for examining the interrelatedness of the factors in subsequent studies. As can be seen from Figure 1, the conceptual model identifies the interrelations between knowledge of PCOS and health-related practices.
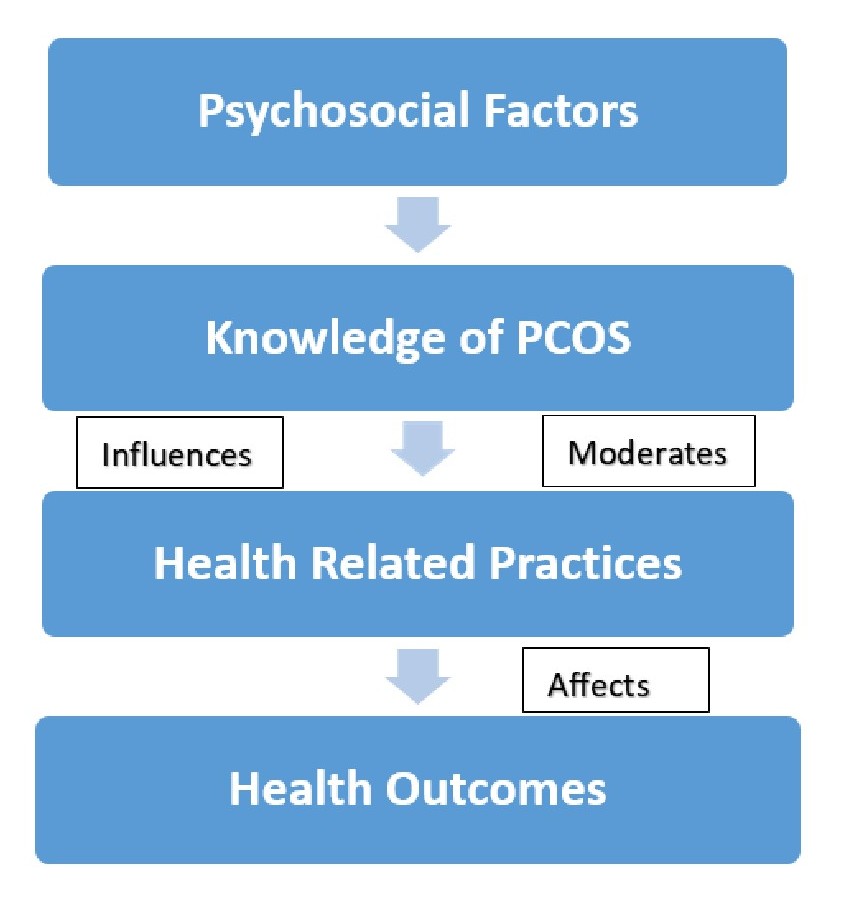
Figure 1: Framework of influences on PCOS health practices
Overall, the findings of this study offer valuable information on knowledge and health practices about PCOS in young women. Although participants exhibited a basic level of knowledge about PCOS, notable areas of knowledge gaps were evident, especially in relation to long-term complications of PCOS, such as the association between prediabetes and PCOS. The positive relationship between knowledge and health practices indicates that increased awareness and comprehension of PCOS may result in healthier behaviors. These results identify a need for specifically directed educational interventions to address knowledge gaps and encourage healthier behaviors among young women in the area.
Discussion
PCOS is increasingly common among women and a leading cause of infertility. Characterized by chronic anovulation, hyperandrogenism, and symptoms like hirsutism, alopecia, irregular menstrual cycles, and acne, PCOS poses significant health risks.[11,12] It is linked to impaired glucose tolerance, increasing the risk of type 2 diabetes, hypertension, dyslipidemia, cardiovascular diseases, and even endometrial cancer. The physical symptoms can negatively impact women’s self-esteem and quality of life.[13,14] Therefore, it is essential to examine awareness and management of PCOS among affected women, particularly in clinical populations, and healthcare providers, as well as to address cultural factors that influence these experiences.[15]
Our study’s findings, indicating specific knowledge gaps alongside areas of high awareness, align with international research that often reveals varied levels of understanding about PCOS. A study in Klang Valley, Malaysia, by Goh et al. found that nearly half of the participants had poor knowledge (47.30%) and poor health-related practices (47.60%) regarding PCOS.[12] These parallels underscore the widespread need for targeted educational interventions, especially for diagnosed populations, to address persistent knowledge deficits.
Several studies from Pakistan corroborate our results, indicating a persistent national challenge. Research by Arif et al. among nurses in Lahore revealed low awareness, with a mean knowledge score of just 1.75.[2] Similarly, Kiran et al. found poor knowledge among nursing students in Lahore.[13] Another study in Lahore by Aslam et al. reported that 20% of women were unaware of their PCOS symptoms despite exhibiting them.[14] These findings collectively mirror the knowledge gaps observed in our Muzaffarabad cohort and underscore the urgent need for enhanced education, not only for the general public but also for healthcare professionals who are pivotal for early diagnosis.
The barriers to seeking information and care are also a critical factor. Rizvi et al. found that while undergraduate students in Pakistan felt comfortable discussing PCOS, 67.3% had never talked about it with a doctor, citing a lack of self-knowledge and shyness as primary reasons.[15] This resonates with our study’s findings that even among diagnosed individuals*, specific knowledge deficits (e.g., regarding pre-diabetes or, notably, the low awareness of irregular menstruation as a symptom) persist, which could indirectly impact ongoing proactive management behaviors. Even among medical students, as shown by Khalfe et al., awareness does not always translate to a complete understanding of PCOS and its long-term implications, further strengthening the case for comprehensive, in-depth education, even in clinical settings.[16]
Jahangir focused on non-medical female students and emphasized that PCOS is a common hormonal disorder affecting women of reproductive age. The study discussed the role of androgens and insulin in the condition, highlighting symptoms like irregular menstrual cycles and infertility. While this research underscored the hormonal aspects of PCOS, our study complements it by showcasing broader social perceptions and attitudes, indicating that awareness is influenced by both medical knowledge and societal factors.[17,18]
Overall, the findings of this study offer valuable information on knowledge and health practices about PCOS among diagnosed young women presenting in a clinical setting in Muzaffarabad. While this cohort demonstrated a good understanding of core PCOS symptoms, notable knowledge gaps were evident, particularly concerning long-term complications such as the association between prediabetes and PCOS, and surprisingly, the fundamental link to irregular menstruation. The positive relationship between knowledge and health practices indicates that increased awareness and comprehension of PCOS can result in healthier behaviors. These results identify a need for specifically directed educational interventions to address persistent knowledge gaps and encourage healthier behaviors among diagnosed young women in the region.[19]
The results of this study underscore the critical need to improve PCOS awareness among young women in Muzaffarabad, AJK. The prevalent unawareness of symptoms and long-term risks, such as infertility and metabolic syndrome, likely contributes to delayed diagnosis and management. This situation is potentially exacerbated by regional factors such as limited access to specialized healthcare and cultural barriers that may discourage open discussion of reproductive health issues. Therefore, this study highlights the immediate need for targeted educational initiatives tailored to the cultural and social context of AJK. Such programs, aimed at both young women and healthcare providers, are essential for bridging knowledge gaps, promoting early intervention, and ultimately improving health outcomes for women with PCOS in this region.
Conclusion
In conclusion, our study among *diagnosed young women attending the gynecology department in Muzaffarabad revealed a high prevalence of PCOS symptoms. While these participants generally exhibited good awareness of core PCOS manifestations like ovarian cysts and hirsutism, significant knowledge deficits were identified, particularly regarding metabolic risks such as pre-diabetes and, surprisingly, the fundamental symptom of irregular menstruation. This emphasizes the critical need for targeted and individualized patient education. Healthcare practitioners must focus on comprehensive education that not only reinforces understanding of core symptoms but also specifically addresses the long-term metabolic complications and clarifies all diagnostic criteria. By focusing educational interventions on these specific gaps, we can empower diagnosed patients to more effectively manage their symptoms, engage in healthier practices, and ultimately improve their overall well-being.
References
- Ajmal N, Khan SZ, Shaikh R. Polycystic ovary syndrome (PCOS) and genetic predisposition: A review article. Eur J Obstet Gynecol Reprod Biol X. 2019;3:100060. doi:10.1016/j.eurox.2019.100060
PubMed | Crossref | Google Scholar - Arif NA, Khawaja S, Iqbal Q. Awareness of polycystic ovarian disease: knowledge and presence of presenting symptoms. Pak J Med Health Sci. 2020;14(2):627-30.
Awareness of Polycystic Ovarian Disease: Knowledge and Presence of Presenting Symptoms - Srour I, Salhab S, Skaiki H, Sakr S, Sheet I. Assessment of prevalence, knowledge of polycystic ovary syndrome and health-related practices among female nurses in Lebanon. Open Public Health J. 2024;17:1-10. doi:10.2174/0118749445299594240430054249
Crossref | Google Scholar - Collée J, Mawet M, Tebache L, Nisolle M, Brichant G. Polycystic ovarian syndrome and infertility: overview and insights of the putative treatments. Gynecol Endocrinol. 2021;37(10):869-874. doi:10.1080/09513590.2021.1958310
PubMed | Crossref | Google Scholar - Cunha A, Póvoa AM. Infertility management in women with polycystic ovary syndrome: a review. Porto Biomed J. 2021;6(1):e116. doi:10.1097/j.pbj.0000000000000116
PubMed | Crossref | Google Scholar - Zehravi M, Maqbool M, Ara I. Polycystic ovary syndrome and infertility: an update. Int J Adolesc Med Health. 2021;34(2):1-9. doi:10.1515/ijamh-2021-0073
PubMed | Crossref | Google Scholar - Chaudhuri A. Polycystic ovary syndrome: Causes, symptoms, pathophysiology, and remedies. Obesity Medicine. 2023;39:100480. doi:10.1016/j.obmed.2023.100480
Crossref | Google Scholar - Islam H, Masud J, Islam YN, Haque FKM. An update on polycystic ovary syndrome: A review of the current state of knowledge in diagnosis, genetic etiology, and emerging treatment options. Womens Health (Lond). 2022;18:17455057221117966. doi:10.1177/17455057221117966
PubMed | Crossref | Google Scholar - Rashid R, Mir SA, Kareem O, et al. Polycystic ovarian syndrome-current pharmacotherapy and clinical implications. Taiwan J Obstet Gynecol. 2022;61(1):40-50. doi:10.1016/j.tjog.2021.11.009
PubMed | Crossref | Google Scholar - Armanini D, Boscaro M, Bordin L, Sabbadin C. Controversies in the Pathogenesis, Diagnosis and Treatment of PCOS: Focus on Insulin Resistance, Inflammation, and Hyperandrogenism. Int J Mol Sci. 2022;23(8):4110. doi:10.3390/ijms23084110
PubMed | Crossref | Google Scholar - Li M, Ruan X, Mueck AO. Management strategy of infertility in polycystic ovary syndrome. Glob Health J. 2022;6(2):70-74. doi:10.1016/j.glohj.2022.03.002
Crossref | Google Scholar - Goh JE, Farrukh MJ, Keshavarzi F, et al. Assessment of prevalence, knowledge of polycystic ovary syndrome and health-related practices among women in klang valley: A cross-sectional survey. Front Endocrinol (Lausanne). 2022;13:985588. doi:10.3389/fendo.2022.985588
PubMed | Crossref | Google Scholar - Kiran S, Sarwar H, Masih S. The Knowledge and Awareness on Polycystic Ovarian Syndrome among Lady Health Visitors in Public Health Nursing School Lahore: Knowledge and Awareness on PCOSs. Pakistan Journal of Health Sciences. 2023;4(05):140-4. doi:10.54393/pjhs.v4i05.707
Crossref | Google Scholar - Aslam M, Batool M, Tahir M, Asmat A, Naeem S, tul Wusqa U, Haneef Y, Sabir U. An explanatory research to undermine the knowledge related attributes of polycystic ovary syndrome among adult females: Polycystic ovary syndrome among adult females. Pakistan BioMedical Journal. 2022;5(3):73-77. doi:10.54393/pbmj.v5i3.179
Crossref | Google Scholar - Rizvi M, Islam MA, Aftab MT, et al. Knowledge, attitude, and perceptions about polycystic ovarian syndrome, and its determinants among Pakistani undergraduate students. PLoS One. 2023;18(5):e0285284. doi:10.1371/journal.pone.0285284
PubMed | Crossref | Google Scholar - Khalfe SA, Rafi U, Fatima B. Prevalence and awareness of polycystic ovarian syndrome among medical students of Karachi, Pakistan. Journal of Shifa Tameer-e-Millat University. 2023;6(2):78-82. doi:10.32593/jstmu/Vol6.Iss2.260
Crossref | Google Scholar - Kabel AM, Alghubayshi AY, Moharm FM. The impact of polycystic ovarian syndrome, a potential risk factor to endometrial cancer, on the quality of sleep. J Cancer Res Treat. 2016;4(6):96-98. doi:10.12691/jcrt-4-6-1
Crossref | Google Scholar - Jahangir S. A Study on Knowledge & Awareness of Polycystic Ovarian Syndrome among Female Non-Medical Undergraduate Students. Doctoral dissertation. East West University; 2013.
A Study on Knowledge & Awareness of Polycystic Ovarian Syndrome among Female Non-Medical Undergraduate Students - Khurshid F, Chatta AN, Zain M, Aziz H, Dar TK, Saghir I. A cross-sectional study to explore depression in postmenopausal women. Journal of Shifa Tameer-e-Millat University. 2024;7(1):61-7. doi.org/10.32593/jstmu/Vol7.Iss1.299
Crossref | Google Scholar
Acknowledgments
None
Funding
None
Author Information
Corresponding Author:
Fatima Khurshid
Department of Radiation Oncology
Medical Officer, Shifa International Hospital, Ltd., Islamabad, Pakistan
Email: fatimakhurshid61@yahoo.com
Co-Authors:
Isha Arshad
Department of Medicine
Azad Jammu Kashmir Medical College, Muzaffarabad, Pakistan
Hira Ali Zafar
Department of Medicine
DHQ Hospital Mirpur, AJK, Pakistan
Samina Qayyum
Department of Gynae and Obstetrics
Cantonment General Hospital, Rawalpindi, Pakistan
Abdul Hadi
Department of Medicine
Pakistan Airforce Hospital Lahore, Pakistan
Ayesha Khurshid
Department of Physiotherapy
Mirpur University of Science and Technology, Mirpur, AJK
Sana Tariq
Department of Emergency Medicine
Holy Family Hospital, Pakistan
Authors Contributions
Fatima Khurshid conceptualized the study design and prepared the initial manuscript draft. Isha Irshad and Sana Tariq were responsible for data collection. Hira Ali Zafar and Abdul Hadi contributed to the writing of the manuscript. Ayesha Khurshid carried out the data analysis, while Samina Qayum interpreted the data and provided a critical review of the manuscript. All authors reviewed and approved the final version of the manuscript.
Ethical Approval
The study received approval from the institutional ethics committee under reference number 17/Academics Block Trauma Center/Surgery/2024.
Conflict of Interest Statement
None
Guarantor
Fatima Khurshid serves as the guarantor for this study and takes full responsibility for the integrity of the work, including the accuracy of the data and analysis.
DOI
Cite this Article
Khurshid F, Arshad I, Zafar HA, et al. Knowledge of Polycystic Ovary Syndrome and Health Related Practice among Young Women in Muzaffarabad, AJK, Pakistan: A Survey Analysis. medtigo J Med. 2025;3(3):e3062338. doi:10.63096/medtigo3062338 Crossref









