Author Affiliations
Abstract
Background: Central Line-Associated Bloodstream Infections (CLABSIs) are a considerable source of increased mortality and morbidity during intensive care unit stays. As there has been a difference in the use of the above preventive measures, nonadherence to protocols still continues to be an issue. Since nurses are direct caregivers, they are in a central position to implement the recommended measures to minimize CLABSI rates.
Aim: To determine the knowledge and performance of nurses towards CLABSI prevention in a tertiary care Hospital in Peshawar, Pakistan.
Methods: In a cross-sectional study, 100 nurses from the tertiary care hospital participated. Data was collected through the structured questionnaire tool. The survey targeted three major areas: knowledge of CLABSI prevention and control measures by the nurses, their compliance with the infection prevention and control measures, and their perception of the effect of change on patient outcome. Quantitative descriptive and inferential statistical analysis was done to measure the results.
Results: When evaluating the nurses’ conformity to the research questions, 85% of the nurses maintained hand hygiene strictly, and 75% were aware of chlorhexidine’s use for skin antisepsis. However, central line removal was evident only 60% of the time. They removed unnecessary central lines promptly. Data analysis revealed that there is a very small knowledge gap. They are adherent to protocol and showed a correlation between knowledge: adherence to protocols, and/or patient health (p < 0.05). Challenges faced were related to workload, staffing, and resources.
Conclusion: In our study, even though the knowledge of and the actual behavior regarding CLABSI manifested a relatively impressive level among the nurses, there are systematic barriers that do not allow them to avoid inconsistent actions. To surmount these challenges, strict training, institutional backing, and promotion of interdisciplinary cooperation will improve compliance and, in the process, patient safety.
Keywords
Central Line-Associated Bloodstream Infection, Nursing practices, Infection control, Patient safety, Tertiary care hospital.
Introduction
Bloodstream-associated infection from the Central Line (CLABSI) poses a great concern to healthcare organizations all over the world.[1] A central line, often referred to as a central venous catheter, is an intravenous line that is placed into the large vessels to deliver medication and/or fluids or to withdraw a specimen. This occurs when pathogens enter the blood through these lines, making complications like sepsis very likely to develop.[2] Nurses are viable in the fight against CLABSIs by being the first line of defense and having a detailed understanding of the best practices.[3] It’s necessary that they strictly observe infection control measures with a view to protecting the health of these patients. It is crucial for CLABSI care improvements that the knowledge and practices nurses have about CLABSI prevention are described and explained.[4]
CLABSIs are among the endemic healthcare-associated infections (HAIs), as well as represent a significant risk factor for patients’ safety. Such infections lead to higher hospital charges, longer lengths of stay, and increased mortality.[5] Observational research on CLABSI has revealed that the infection may be fatal in up to 25% of intensive care unit (ICU) patients. Nurses’ knowledge and compliance with CLABSI prevention practices are dependent on available training and educational programs for the nurses.[6] The programs, including workshops, simulations, and e-modules, have proved beneficial as a way of improving the end product of the nurses as well as their awareness.[7]
Nurses are currently becoming involved in these monitoring efforts because their frontline involvement with patients affords a unique perspective.[8] Prescribing a competent monitoring system enhances the performance of the health organizations, and it is a confirmation of responsibility towards patients by correcting the errors that might be made by health practitioners.[9] The efficiency of continuing education for practicing registered nurses (RNs) can be demonstrated by using organization-wide educational campaigns to promote awareness and understanding of CLABSIs and the precautions to prevent them. Such campaigns can focus on the effects of CLABSIs on individual patients, organizational performance, and financial implications.[10]
Methodology
The current research applied a cross-sectional survey design in order to assess the knowledge and practices of nursing professionals with concerns regarding CLABSI. It was conducted on 100 participants at the Peshawar Institute of Cardiology, Peshawar, Pakistan, through purposive sampling. Only registered nurses with more than one year’s working experience in the critical care area of practice, including intensive care units and high dependency units, were considered. Participants with less than one year’s experience or who did not wish to participate were excluded.
Data collection procedure: Data collection was done in consultation with the supervisor and with approval from the pediatric intensive care (PIC) hospital administration. Informed consent was obtained from each participant whose data was collected through a structured questionnaire. The areas of questioning were demographic details, knowledge, and practice concerning CLABSI prevention. The questionnaires were administered in person, and data were collected over a one-month period. A self-administered questionnaire (paper-based) was used for data collection. Data was collected using a five-point Likert scale.
Data analysis: The data analysis was done using the statistical package for the social sciences (SPSS) software. Frequency distributions and percentages were used to analyze demographic data and participants’ awareness and behavior related to CLABSI prevention. Chi-square test analysis was conducted to analyze how nurses applied the identified infection control measures to patients and the perceived effects. As for statistical significance, the results were given a p-value of less than 0.05 for all the studies.
Ethical consideration: Ethical approval was taken from the institutional review board (IRB) Peshawar institute of cardiology Peshawar, Pakistan (Ref No IRC/24/92). All participants provided written informed consent. Thus, they volunteered themselves, and anonymity was also ensured. To maintain anonymity and confidentiality, the participants’ identification was eliminated from the questionnaires, and the data were kept secure. The participants were told that their participation was voluntary and that all responses given would be kept anonymous.
Results
Demographic characteristics of participants: The total number of participants in the study was 100, where the number of female participants was higher compared to male participants (Table 1).
| Variable | Category | Frequency (n) | Percentage |
| Gender | Male | 45 | 45 |
| Female | 55 | 55 | |
| Age | 20-30 years | 60 | 60 |
| 31-40 years | 25 | 25 | |
| 41-50 years | 10 | 10 | |
| 51+ years | 05 | 05 | |
| Years of Experience | 1-5 years | 70 | 70 |
| 6-10 years | 20 | 20 | |
| 11+ years | 10 | 10 | |
| Department | ICU | 50 | 50 |
| High dependency unit (HDU) | 30 | 30 | |
| Pediatric intensive care unit (PICU) | 20 | 20 |
Table 1: Demographic characteristics of participants
Knowledge of CLABSI prevention protocols: A significant proportion of the nurses in the study had good knowledge and practice concerning CLABSI prevention. Only 20% disagreed with the practice of hand hygiene, and 30% disagreed with knowledge regarding appropriate aseptic techniques applicable during central line insertion (Table 2).
| Knowledge Item | Strongly Agree | Agree | Disagree | Strongly Disagree |
| Nurses understand the importance of hand hygiene in preventing CLABSI. | 80% | 15% | 5% | 0% |
| Nurses are familiar with proper aseptic techniques for central line insertion. | 70% | 20% | 5% | 5% |
| Nurses use chlorhexidine for skin antisepsis during central line insertion. | 75% | 20% | 3% | 2% |
| Nurses regularly assess the necessity of central lines for patients. | 65% | 25% | 7% | 3% |
| Nurses consistently follow PPE protocols when handling central lines. | 85% | 10% | 3% | 2% |
Table 2: Knowledge of CLABSI prevention protocols
Nurses practice CLABSI prevention: nurses have a commitment to infection prevention. Before and after touching the central line, 85% of participants complied with hand hygiene, and 78% were also compliant with aseptic measures adopted during dressing change (Figure 1).
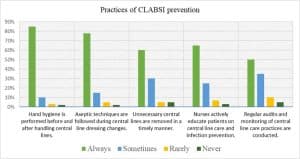
Figure 1: Practices of nurses on CLABSI prevention
Relationship between knowledge, practices, and perceived impact on patient health: The result shown here indicated that there was a high level of correlation between the level of knowledge on CLABSI prevention and infection control practice knowledge comprehension (Table 3).
| Variable | Chi-Square Value (X²) | p-value | Significance |
| Knowledge of CLABSI prevention and adherence to infection control practices. | 24.5 | 0.002 | Significant |
| Knowledge of CLABSI prevention and perceived impact on patient health outcomes. | 18.3 | 0.009 | Significant |
| Adherence to CLABSI prevention protocols and patient satisfaction. | 20.8 | 0.004 | Significant |
| Timely central line removal and patient health outcomes. | 15.6 | 0.023 | Significant |
Table 3: Relationship between knowledge, practices, and perceived impact on patient health
Discussion
One of the surprising facts that the present study revealed was the high level of awareness that the nurses have about infection control measures, particularly handwashing, use of gloves, masks, and other barrier tools, and use of gowns. These findings are parallel to the results of the study, which showed a high level of awareness that the nurses have about infection control measures.[11] The survey shows that 85% of nurses maintain hand hygiene before and after touching the central line, and 75% of nurses know how to use chlorhexidine during central line insertion. This finding aligns with the result of the research.[12] Similar to past investigations, the findings of the studies support the direct link between handwashing and correct aseptic practice to ward off CLABSI.[13] Nurses are, of course, knowledgeable, but our work indicates that in deploying this knowledge and enhancing the practice, it does not always translate because local factors such as work pressure and time limitations get in the way, which was evident from other studies as well.[14]
One area of contrast between our findings and other studies lies in the issue of central line removal. In this study, only 60% of nurses reported always removing central lines in a timely manner when no longer needed, with 30% indicating that they sometimes fail to remove lines promptly. This finding is consistent with those of other studies, which highlighted that delayed removal of central lines remains a significant risk factor for CLABSI.[15,16] However, our study also showed that the importance of timely line removal was recognized by most nurses, with 72% agreeing that this practice significantly impacts patient health outcomes. This suggests a gap between knowledge and practice, which can be attributed to challenges in clinical settings such as high patient-to-nurse ratios, staff shortages, and time pressures.[17]
Limitations: This study has limitations that include the use of purposive sampling, which may increase selection bias in the study, and a cross-sectional study design, which does not aptly establish cause-and-effect relationships. Also, there is a possibility that biases in using self-reported data in the study’s results cannot be generalized to other healthcare facilities because of the sample restriction to a single Hospital.
Conclusions
The findings in this study examined the current level of knowledge, compliance by the nurses, and perceived effectiveness of the implemented infection control measures in the prevention of CLABSI. Despite the nurses showing good practices knowledge and good implementation of key practices, system challenges such as workload and lack of adequate staffing reduce practice uniformity. These barriers must be overcome by gaining institutional support, which can entail continuing education and encouraging interdisciplinary cooperation to advance the infection prevention initiative and save the patients’ lives. Other potential strategies of healthcare institutions to prevent CLABSI should focus on eliminating system causes by increasing staffing, elaborating training programs, and increasing resources. Continued promotion of interdisciplinary staff collaboration among nurses, physicians, and infection control specialists may enhance infection prevention activity. Other factors which should also be incorporated specifically in relation to practices include template audit, feedback systems, and leadership support to enhance the applications of evidence-based practice (EBP).
References
- Gaonyatsege-Thankane R. Critical care nurses’ knowledge of evidence–based guidelines for the management of central venous catheters. Master’s thesis. University of the Witwatersrand; 2021. Critical care nurses’ knowledge of evidence–based guidelines for the management of central venous catheters
- Gadala A. A model to forecast central-line–associated bloodstream infection rates in acute care hospital units. Doctoral dissertation. The State University of New Jersey; 2021. A model to forecast central-line-associated bloodstream infection rates in acute care hospital units
- Alkhawaja S, Saeed NK, Rosenthal VD, et al. Impact of International Nosocomial Infection Control Consortium’s multidimensional approach on central line-associated bloodstream infection rates in Bahrain. J Vasc Access. 2020;21(4):481-489. doi:10.1177/1129729819888426 PubMed | Crossref | Google Scholar
- Lutufyo TE, Qin W, Chen X. Central line associated bloodstream infection in adult intensive care unit population—changes in epidemiology, diagnosis, prevention, and addition of new technologies. Adv Infect Dis. 2022;12(02):252-280. doi:10.4236/aid.2022.122022 Crossref | Google Scholar
- Alqalah TAH. Mitigating risks in central line-associated bloodstream infection: a comprehensive insight into critical care nurses’ knowledge, attitudes, barriers, and compliance. BMC Nurs. 2024;23(1):497. doi:10.1186/s12912-024-02168-5
PubMed | Crossref | Google Scholar - Sham F, Huda Sulaiman N, Seman A, Akma Shohor N, Yao Mun C. Intensive care nurses’ knowledge, practice and attitude in prevention of central line-associated bloodstream infection (CLABSI). J Health Transl Med. 2023;(special issue 2):102-110. doi:10.22452/jummec.sp2023no2.12 Crossref | Google Scholar
- Manzo BF, Dittz Duarte E, Joice de Abreu Felizardo M, et al. Knowledge and Practices for Central Line Infection Prevention Among Brazilian Nurses: A Mixed-Methods Study. Adv Neonatal Care. 2022;22(2):180-187. doi:10.1097/ANC.0000000000000893 PubMed | Crossref | Google Scholar
- Al-Yateem ISA. Knowledge, behavior and attitude of nurses regarding prevention of Central Line Associated Blood Stream Infections. Master’s thesis. Royal College of Surgeons in Ireland; 2021. doi:10.25419/RCSI.13567523.V1
Google Scholar - Goldman J, Rotteau L, Shojania KG, et al. Implementation of a central-line bundle: a qualitative study of three clinical units. Implement Sci Commun. 2021;2(1):105. doi:10.1186/s43058-021-00204-y PubMed | Crossref | Google Scholar
- Beville ASM, Heipel D, Vanhoozer G, Bailey P. Reducing Central Line Associated Bloodstream Infections (CLABSIs) by Reducing Central Line Days. Curr Infect Dis Rep. 2021;23(12):23. doi:10.1007/s11908-021-00767-w PubMed | Crossref | Google Scholar
- Drews FA, Bakdash JZ, Gleed JR. Improving central line maintenance to reduce central line-associated bloodstream infections. Am J Infect Control. 2017;45(11):1224-1230. doi:10.1016/j.ajic.2017.05.017 PubMed | Crossref | Google Scholar
- Hannum SM, Oladapo-Shittu O, Salinas AB, et al. Controlling the chaos: Information management in home-infusion central-line-associated bloodstream infection (CLABSI) surveillance. Antimicrob Steward Healthc Epidemiol. 2023;3(1):e69. doi:10.1017/ash.2023.134 PubMed | Crossref | Google Scholar
- Wang C, Jiang W, Yang K, et al. Electronic Monitoring Systems for Hand Hygiene: Systematic Review of Technology.
J Med Internet Res. 2021;23(11):e27880. doi:10.2196/27880 PubMed | Crossref | Google Scholar - Wu F, Wu T, Zarate DC, et al. An autonomous hand hygiene tracking sensor system for prevention of hospital associated infections. IEEE Sens J. 2021;21(13):14308-14319. doi:10.1109/jsen.2020.3041331 Crossref | Google Scholar
- Iversen AM, Kavalaris CP, Hansen R, et al. Clinical experiences with a new system for automated hand hygiene monitoring: A prospective observational study. Am J Infect Control. 2020;48(5):527-533. doi:10.1016/j.ajic.2019.09.003 PubMed | Crossref | Google Scholar
- Ascaño FA. Tiered centralized education in the transition-to-practice program to improve nurses’ level of confidence on nursing-sensitive indicators outcomes. Doctoral projects. San Jose State University; 2022. doi:10.31979/etd.r2bf-fdac Crossref | Google Scholar
- Drews FA, Bakdash JZ, Gleed JR. Improving central line maintenance to reduce central line-associated bloodstream infections. Am J Infect Control. 2017;45(11):1224-1230. doi:10.1016/j.ajic.2017.05.017 PubMed | Crossref | Google Scholar
Acknowledgments
None
Funding
None
Author Information
Corresponding Author:
Sidra Iqbal
Department of Nursing
Service Institute of Medical Sciences Lahore, Pakistan
Email: salmansidra15@gmail.com
Co-Author:
Aqsa Iqbal
Department of Nursing
Service Institute of Medical Sciences Lahore, Pakistan
Authors Contributions
All authors contributed to the conceptualization, investigation, and data curation by acquiring and critically reviewing the selected articles. They were collectively involved in the writing – original draft preparation, and writing – review & editing to refine the manuscript. Additionally, all authors participated in the supervision of the work, ensuring accuracy and completeness. The final manuscript was approved by all named authors for submission to the journal.
Ethical Approval
Ethical approval was taken from the institutional review board (IRB) Peshawar institute of cardiology Peshawar, Pakistan (Ref No IRC/24/92). All participants provided written informed consent.
Conflict of Interest Statement
Not reported
Guarantor
None
DOI
Cite this Article
Sidra I, Aqsa I. Knowledge and Practices of the Nurses Regarding Central Line Associated Infection at Tertiary Care Hospital, Peshawar, Pakistan. medtigo J Med. 2025;3(1):e30623116. doi:10.63096/medtigo30623116 Crossref









