Author Affiliations
Abstract
Background: Spirometry is a skilled procedure that relies heavily on the cooperation of the patient and the skillfulness of the person administering the procedure. Spirometry is one of the most widely used techniques in the evaluation of pulmonary function, particularly the volume of air that can be inhaled or exhaled, and the rate at which such air can be exhaled.
Aim: The study aimed to assess the level of nursing knowledge and perception towards spirometry, including their competence on the spirometry test in a clinical setting.
Methods: The quantitative cross-sectional study design was used, aimed to assess the level of knowledge of spirometry as well as the perception of 100 nurses in the Saidu Group of Teaching Hospital (SGTH) Swat, Pakistan. Through convenience sampling, the sample population was recruited based on some criteria for the nurses. The survey questionnaire, as the main data collection tool, was structured and administered, while data analysis was conducted using the Statistical package for the social sciences (SPSS) software version 27. Descriptive analysis of demographic variables, knowledge, and perceptions was done using the frequency and percentage distribution.
Results: The survey evaluated the awareness and attitude of 100 nurses towards spirometry at SGTH. Most of the nurses had an excellent understanding of knowledge to spirometry and its uses, 90% responded to spirometry’s purpose accurately. Most of those surveyed believed spirometry was necessary and performed regularly, but 30% admitted to limitations in spirometry and 70% would like to receive additional training.
Conclusion: The current study shows that nurses have a moderate amount of knowledge about spirometry and have positive attitudes towards it. However, specific barriers require training and resource commitment as key strategies for the successful implementation of ICP into nursing practice.
Keywords
Spirometry, Nursing knowledge, Respiratory care, Demographic characteristics, Hospitals.
Introduction
Spirometry is one of the most widely used techniques in the evaluation of pulmonary function, particularly the volume of air that can be inhaled or exhaled, and the rate at which such air can be exhaled.[1] This test is a critical tool in the assessment of asthma, the distinction between chronic obstructive pulmonary disease (COPD) and asthma, and pulmonary fibrosis, among other respiratory disorders.[2] The nurses, especially those working in care facilities, respiratory therapy, primary care, and hospitals, are most likely to be involved in the care of clients with respiratory disorders.[3] They help to perform and explain spirometry and adhere to therapies, educate customers.[4] Knowledge can be defined as the story held or believed to be true or a skill acquired through learning or personal experience. On the other hand, perception entails the manner or ways in which information is processed.[5]
Spirometry is a very skilled procedure that relies heavily on the cooperation of the patient and the skillfulness of the person administering the test.[6] However, despite such important services from nurses, few studies have been done to find out how many nurses have undergone spirometry and their preparedness to conduct it.[7]
However, the perception nurses have about spirometry can determine their attitude toward the use of spirometry in a clinical setting.[8] The nurses believe that spirometry is an important tool in the care of patients; they are more likely to recommend its use and explain to patients why the test is important.[9] However, low levels of knowledge or poor understanding of spirometry can result in low self-efficacy in performing the test. This may consequently decrease the quality of patient care.[10]
Methodology
To evaluate and compare spirometry knowledge and perception in nurses employed at SGTH in Swat Pakistan, a cross-sectional quantitative study was conducted. The study targeted 100 nurses from the hospital’s intensive care units (ICU), critical care units (CCU), pulmonology, surgical, and orthopedic departments. Only participants who had worked for at least six months in these departments were considered, and those willing to participate. The goal of the research was to identify the gaps in current knowledge and associated attitudes of the selected group of nurses to spirometry. Convenience sampling was effective in data collection, even though it may pose some restrictions to the results’ general applicability.
Data collection procedure: Information was gathered with the aid of a standard self-administered structured questionnaire containing closed-ended questions. The questionnaire developed aimed at evaluating the understanding and attitude of the nurses towards spirometry. It included three sections:
Demographic information: Concerning age, gender, experience, and work in the clinical area.
Knowledge of spirometry: A comprehensive knowledge assessment test comprising multiple-choice questions to test their knowledge of spirometry and the tests’ primary role, how it is done, and the results.
Perception of spirometry: Questions on a Likert scale regarding the nurses’ confidence when administering spirometry tests, regarding their view on how important the test is in diagnosing the patients, and any perceived obstacles to the integration of spirometry in practice.
Data analysis procedure: The data collected from the structured questionnaires were analyzed using SPSS software version 27. The frequency and percentage distributions were calculated for demographic variables, knowledge scores, and perceptions of spirometry.
Ethical consideration: Ethical clearance to conduct the study was sought from the medical superintendent of the hospital. All participants provided written informed consent. Thus, they volunteered themselves, and anonymity was also ensured.
Results
Demographic characteristics of study participants: The total number of participants in the study was 100, where the number of male participants was higher compared to female participants.
| Demographic variable | Frequency (n) | Percentage (%) |
| Age | ||
| 20-30 years | 40 | 40% |
| 31-40 years | 35 | 35% |
| 41-50 years | 15 | 15% |
| 51+ years | 10 | 10% |
| Gender | ||
| Male | 65 | 65% |
| Female | 35 | 35% |
| Years of experience | ||
| 1-5 years | 25 | 25% |
| 6-10 years | 45 | 45% |
| 11+ years | 30 | 30% |
| Clinical unit | ||
| ICU | 20 | 20% |
| CCU | 25 | 25% |
| Pulmonology | 20 | 20% |
| Surgical | 25 | 25% |
| Orthopedic | 10 | 10% |
Table 1: Demographic characteristics of the nurses (N = 100)
Most of the nurses were included in the study from the surgical unit and the CCU.
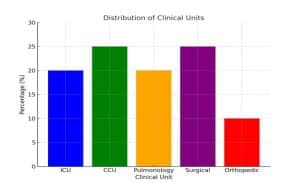
Figure 1: Working area of participants
The highest correct response (95%) was for the need to instruct deep inhalation before spirometry.
| Knowledge question | Correct response (%) | Incorrect response (%) |
| What is the primary purpose of spirometry? | 90% | 10% |
| Which of the following is measured by spirometry? | 85% | 15% |
| Which condition is commonly diagnosed using spirometry? | 80% | 20% |
| Can spirometry be used to assess lung volume? | 75% | 25% |
| Is it necessary to instruct the patient to inhale deeply before spirometry? | 95% | 5% |
Table 2: Knowledge of spirometry
Most respondents (95%) recognize spirometry as an essential diagnostic tool, with 85% feeling confident in performing the test.
| Perception statement | Strongly agree | Agree | Neutral | Disagree | Strongly disagree |
| Spirometry is an important diagnostic tool for respiratory conditions. | 75% | 20% | 5% | 0% | 0% |
| I feel confident in performing spirometry tests. | 55% | 30% | 10% | 5% | 0% |
| Spirometry is a routine part of patient care in my clinical unit. | 60% | 25% | 10% | 5% | 0% |
| There are barriers to using spirometry effectively in clinical practice. | 30% | 40% | 20% | 10% | 0% |
| I believe further training in spirometry would be beneficial. | 70% | 25% | 5% | 0% | 0% |
Table 3: Perception of spirometry
Discussion
The research sample comprised 100 nurses, out of which a higher percentage of participants were male (65%) and a lesser percentage of female participants (35%). These findings align with a study that showed that 65 percent of participants were male. To instruct deep inhalation before spirometry.[11] This disparity in gender could be a result of the demography of its human resources, although gender might not influence the level of awareness and perception towards spirometry, as shown in the study findings.[12]
Knowledge of spirometry: According to the findings of the study, the nurses were assumed to have a moderate amount of knowledge regarding spirometry. Most respondents provided correct answers to questions related to the primary use of spirometry: 90%, correct answers concerning the assessment of lung volume: 75%, and diagnosis of respiratory disorders: 80%. These outcomes are opposite to the study finding, which showed only 52% correct responses relating to the primary use of spirometry.[13]
Still, some areas had a large gap. Knowledge about the applicability of spirometry in concrete cases was answered by only 80 percent. These findings are parallel to the study findings.[14] This implies that as much as the nurses have knowledge, they may not have the exact detailed knowledge of how spirometry is useful, especially in the diagnosis of certain respiratory diseases. This shows a potential for additional training and education to improve their clinical use of the test.[15]
Perception of spirometry: From the perception point of view, the study revealed that the modality of the nurses viewed spirometry as an essential modality for diagnosing respiratory diseases, with 31 respondents strongly agreeing or agreeing with the statement. This finding is opposite to the study, which showed that 80 % of respondents agree that spirometry is essential for diagnosis.[16] Study participants had moderate levels of confidence in spirometry and reported moderate levels of perceived barriers to using spirometry.[17]
The study showed that 55% of the respondents expressed their self-confidence in performing spirometry tests, with 30% agreeing to some extent, while the rest remained in the neutral zone. These findings are opposite to the study,which showed that 40% of the respondents expressed their self-confidence in performing spirometry tests.[18]
The survey also found that 30 % of the nurses strongly endorsed it and 40 % partially endorsed the idea that there are limitations in the practice of spirometry.[19] This observation agrees with earlier studies that mention several limitations: patients do not have access to spirometers or equipment, healthcare workers are not trained to perform spirometry, or have limited time for this activity. Of note, when considering the potential for future implementation of spirometry in clinical settings, 70% of the surveyed nurses claimed that they would like to receive further training: taken at face value, this represents a positive perception of the role of professional development; nonetheless, the perception of barriers indicates that more support for spirometry implementation may still be needed.[20]
Conclusion
In this study, the authors found that although most nurses at the SGTH know why spirometry is used, and how it is done, they are not fully knowledgeable about its specific practice areas. Despite awareness of spirometry among most nurses, a proportion stated low self-efficacy, while nearly a third of the sample reported challenges towards effective spirometry use. These results underscore the importance of specific educational and material support for the enhancement of spirometry in clinical practice.
To promote the confidence and competence of nurses, it is suggested that frequent and broadly based training programs on spirometry should be initiated. Furthermore, such factors as lack of equipment and time could also be other modifiable factors that, should they be optimized, help in the practical application of spirometry. Subsequent research should establish the efficacy of the training interventions; it should also determine possible ways of dealing with the challenges facing the nurses while implementing spirometry in the caregiving process.
References
- Gefter WB, Lee KS, Schiebler ML, et al. Pulmonary functional imaging: Part 2-state-of-the-art clinical applications and opportunities for improved patient care. Radiology. 2021;299(3):524-538. doi:10.1148/radiol.2021204033
PubMed | Crossref | Google Scholar - Townsend MC. Spirometry in occupational health, 2020. J Occup Environ Med. 2020;62(5):e208-230. doi:10.1097/JOM.0000000000001851 PubMed | Crossref | Google Scholar
- Kouri A, Dandurand RJ, Usmani OS, Chow CW. Exploring the 175-year history of spirometry and the vital lessons it can teach us today. Eur Respir Rev. 2021;30(162):210081. doi:10.1183/16000617.0081-2021 PubMed | Crossref | Google Scholar
- Whitmer KH. Assessment of pulmonary function. In: A Mixed Course-Based Research Approach to Human Physiology. 2021. Assessment of Pulmonary Function – A Mixed Course-Based Research Approach to Human Physiology
- Ng DT, Luo W, Chan HM, Chu SK. Using digital story writing as a pedagogy to develop AI literacy among primary students. Comput Educ Artif Intell. 2022;3:100054. doi:10.1016/j.caeai.2021.100054 Crossref | Google Scholar
- Ghibu S, Juncan AM, Rus LL, et al. The particularities of pharmaceutical care in improving public health service during the COVID-19 pandemic. Int J Environ Res Public Health. 2021;18(18):9776. doi:10.3390/ijerph18189776
PubMed | Crossref | Google Scholar - Perry AG, Potter PA, Ostendorf WR, Laplante N. Clinical Nursing Skills and Techniques. eBook. Elsevier Publishing; 2024. Clinical Nursing Skills and Techniques
- Desjardins A, Boulay MÈ, Gagné M, Simon M, Boulet LP. Family medicine physician teachers and residents’ intentions to prescribe and interpret spirometry: A descriptive cross-sectional study. J Asthma. 2020;57(2):149-159. doi:10.1080/02770903.2019.1571097 Google Scholar
- Dueñas PS. An evidence-based educational presentation on spirometry in the pediatric primary care setting. Doctoral dissertation. The University of Arizona; 2020. An Evidence-Based Educational Presentation on Spirometry in the Pediatric Primary Care Setting
- Lim R, Smith T, Usherwood T. Barriers to spirometry in Australian general practice: A systematic review. 2023;52(9):585-593. doi:10.31128/AJGP-09-22-6568 PubMed | Crossref | Google Scholar
- Sampaio F, Sequeira C, Teixeira L. Impact of COVID-19 outbreak on nurses’ mental health: A prospective cohort study. Environ Res. 2021;194:110620. doi:10.1016/j.envres.2020.110620 PubMed | Crossref | Google Scholar
- Deng Z, Dong B, Guo X, Zhang J. Impact of indoor air quality and multi-domain factors on human productivity and physiological responses: A comprehensive review. Indoor Air. 2024;2024(1):5584960. doi:10.1111/ina.13038 Impact of indoor air quality and multi-domain factors on human productivity and physiological responses: A comprehensive review
- Dombkowski KJ, Hassan F, Wasilevich EA, Clark SJ. Spirometry use among pediatric primary care physicians. 2010;126(4):682-687. doi:10.1542/peds.2010-0301 PubMed | Crossref | Google Scholar
- Harvanová G, Csanády A, Duranková S. Impact of pollen season and viral disease COVID-19 on respiratory function of the adult population in Eastern Slovakia: Analysis of spirometric data and results of a questionnaire survey. J Asthma. 2024;61(7):745-753. doi:10.1080/02770903.2024.2303762 PubMed | Crossref | Google Scholar
- Townsend MC. Spirometry in occupational health. J Occup Environ Med. 2020;62(5):e208-230. doi:10.1097/JOM.0000000000001847 PubMed | Crossref
- Graham SS. The Doctor and the Algorithm: Promise, Peril, and the Future of Health AI. eBook. Oxford University Press; 2022. The Doctor and the Algorithm: Promise, Peril, and the Future of Health AI
- Dombkowski KJ, Hassan F, Wasilevich EA, Clark SJ. Spirometry use among pediatric primary care physicians. Pediatrics. 2010;126(4):682-687. doi:10.1542/peds.2010-0301 PubMed | Crossref | Google Scholar
- Pramod P. Street Vendors in Kerala—Vulnerability, Capability, and Potentials. Doctoral dissertation. University of Calicut Libraries; 2023. Street vendors in Kerala – vulnerability, capability, and potentials
- Saunders C. Evidence-Based Training for Nurses: Improving Incentive Spirometry Usage, Documentation, and Patient Education, While Decreasing Postoperative Pulmonary Complications in Coronary Artery Bypass Graft Patients. Doctoral dissertation. The University of North Carolina at Charlotte; 2024. Evidence-Based Training for Nurses: Improving Incentive Spirometry Usage, Documentation, and Patient Education, While Decreasing Postoperative Pulmonary Complications in Coronary Artery Bypass Graft Patients
- Johnson B, Steenbruggen I, Graham BL, Coleman C. Improving spirometry testing by understanding patient preferences. ERJ Open Res. 2021;7(1):00093-2020. doi:10.1183/23120541.00093-2020 PubMed | Crossref
Acknowledgments
I would like to express my sincere gratitude to all who supported me during the writing of this article. Special thanks to my mentor, Dr. Shah Hussain, for his guidance. I’m deeply thankful to my family and friends for their understanding, especially my parents and my wife, whose unwavering support made this work possible. I also appreciate my colleagues and the staff of SGTH for their assistance throughout this journey.
Funding
The work had no special funding.
Author Information
Kainat Nadeem
Department of Nursing
Al-Harmain Institute of Health Sciences, Pakistan
Email: nadeemkainat707@gmail.com
Author Contribution
I would like to express my sincere gratitude to all who supported me during the writing of this article. Special thanks to my mentor, Dr. Shah Hussain, for his guidance. I’m deeply thankful to my family and friends for their understanding, whose unwavering support made this work possible. I also appreciate my colleagues and the staff of SGTH for their assistance throughout this journey.
Conflict of Interest Statement
The author declares no conflicts of interest.
Guarantor
None
DOI
Cite this Article
Kainat N. Knowledge and Perception of Spirometry Among Nurses: A Cross-Sectional Study. medtigo J Med. 2025;3(1):e30623117. doi:10.63096/medtigo30623117 Crossref









