Author Affiliations
Abstract
Background: Patients with esophageal cancer often require percutaneous endoscopic gastrostomy (PEG) tube feeding due to dysphagia and malnutrition. This treatment presents several physical, emotional, and socioeconomic challenges for caregivers. Despite their critical role, particularly in resource-limited settings, caregivers’ experiences with PEG tube management remain underexplored. This study aims to examine the multifaceted experiences of caregivers, focusing on their knowledge, emotional responses, caregiving practices, and the support systems available to them.
Methodology: The research used a phenomenological qualitative design to study 12 primary caregivers at Saidu Teaching Hospital in Swat through in-depth interview sessions. Participants were selected purposively, having provided PEG tube care for more than one month. Data were collected through in-depth interviews and analyzed thematically using Braun and Clarke’s (2006) framework.
Results: Most caregivers (75%) were women aged 31–50. Many reported emotional distress, particularly grief over the loss of shared meals and guilt rooted in their collectivist culture (67%). Challenges included a lack of formal training and the demanding nature of care. Religious coping was prevalent (58%), while 83% expressed the need for clearer instructional methods, and 75% highlighted the necessity of psychological counseling.
Conclusion: Multiple stressors affecting caregivers emerge from their cultural background and broader institutional influences. Because of the existing challenges, the framework for interventions needs to combine practical training with faith-based counseling and financial safety measures. Certain healthcare assistance programs need immediate cultural adaptation because it will benefit caregivers and their patients.
Keywords
Percutaneous endoscopic gastrostomy tube feeding, Esophageal cancer, Caregivers, Qualitative research, Low-resource settings.
Introduction
Esophageal cancer manifests as an aggressive tumor that causes dysphagia alongside malnutrition and significant weight reduction, thus requiring alternative nutrition through percutaneous endoscopic gastrostomy (PEG) tube feeding.[1] The flexible feeding tube, known as a PEG tube, enables nutrition delivery into the stomach through the abdominal wall for patients who cannot tolerate oral feeding.[2] The primary responsibility for handling PEG tube nutrition, nutritional management, preventing issues, and keeping patients healthy belongs to caregivers who are usually relatives.[3] PEG tube feeding requires caregivers to handle various demands that researchers have not sufficiently addressed.[4]
Esophageal cancer exists as the eighth most common cancer in the world, based on annual reports indicating 604,000 new cases and 544,000 deaths.[5] The disease shows aggressive behavior because of its high mortality rate. When patients receive late-stage diagnoses, dysphagia affects 60-80% of them, which requires the placement of PEG tubes for nutritional support.[6] Researched data shows that thirty to fifty per cent of patients with advanced esophageal cancer need a PEG tube for proper nutrition and hydration support, which establishes its vital significance for palliative management.[7] The rising need for PEG tube feeding has created an escalating challenge for caregivers because most healthcare providers lack enough training and support resources to handle this complicated treatment method properly.[8]
Esophageal cancer shows an increasing global trend that produces poor survival outcomes, together with high mortality among patients in advanced disease stages.[9] The disease progression results in debilitating swallowing problems, so PEG tube feedings serve as a vital method to maintain patient nutrition and fluid levels. PEG tubes provide life-prolonging benefits, but healthcare providers must follow strict hygiene maintenance and feed administration procedures and identify complications during usage.[10] Those without medical training who care for patients must learn these essential medical procedures rapidly because professional support remains minimal. Unstandardized caregiver training programs alongside inadequate emotional assistance lead caregivers to experience work-related stress, which creates anxiety and burnout that adversely affect patient care quality.[11]
Most PEG tube feeding research examines clinical results, including infection statistics, patient survival duration, and tube maintenance, but fails to consider the caregiver’s experience.[12] Detecting the substantial physical and psychological impact on caregivers from multiple chronic diseases like dementia and stroke shows symptoms of depression and isolation, while creating financial difficulties.[13] The specific demands of caring for an esophageal cancer patient through rapid disease progression and numerous hospital visits while managing a life-sustaining intervention have not received sufficient exploration in research.[14] The researchers recognize the importance of filling this knowledge gap since caregiver well-being directly impacts patient feeding implementation success and health results.[15]
Emotional and technical factors involving PEG tube maintenance difficulties worsen the overall caregiving difficulties for families.[16] Caregivers should learn skills to address tube complications, including blockages, as well as infections and dislodgement, without rapid access to medical help. Caregivers and patients may experience emotional distress when the patient transitions to tube feeding because it represents the disease progression, and they lose their ability to eat normally.[17] Caregivers who experience psychological distress from viewing their loved one deteriorate while continuously dealing with caregiving duties develop fatigue that hampers their care quality. Healthcare providers must fully comprehend these challenges to deliver proper training, suitable resources, and psychosocial support.[18]
Medical experts acknowledge escalating caregiver strain in oncology, yet they need systematic support systems for individuals who perform PEG tube feeding tasks.[19] Most health systems dedicate their resources to treating patients while neglecting caregiver welfare, forcing caregivers to handle sophisticated care procedures without guidance.[20] Positive impacts on caregiver burdens are possible through peer support groups, educational programs, and respite care services, although these services remain scarce in availability and accessibility.[21] The study investigates lived caregiver experiences to find crucial intervention points by developing better training systems, emotional support methods, and community support resources, which will benefit patient and caregiver outcomes.[22]
Scientists behind this research work to address current gaps in knowledge about the diverse phenomena within caregiver tasks while managing PEG tube feedings for esophageal cancer patients.[23] The study investigates the practical challenges along with emotional problems and unmet requirements of this demographic using quantitative and qualitative research methods. This research will guide healthcare policies to create cancer care systems incorporating extensive caregiver support mechanisms. Improving quality of life for patients and their families depends on caregivers receiving knowledge and developing skills and emotional resilience for continuous, compassionate disease trajectory care.[24]
Methodology
The study adopted a phenomenological qualitative approach to investigate the lived experiences and challenges encountered by caregivers who conducted PEG tube feeding for their patients with esophageal carcinoma at Saidu Teaching Hospital, Swat, which treats numerous esophageal cancer patients who require PEG tube feeding. The research selected 12 primary caregivers (relative family members) through purposive sampling for analysis. These caregivers supported patients with esophageal carcinoma through PEG tube feeding for at least one month until data saturation occurred for thematic analysis. The research included primary caregivers responsible for tube feeding management of confirmed esophageal carcinoma patients who met the criteria of having at least one month of experience and providing consent. This feature strengthened the quality of data collection by giving authentic perspectives about their healthcare experiences.
Data collection process: Ethical approval was obtained from Saidu Teaching Hospital, Swat, Ref No SGTH/IRB/2025/27. The research data were gathered by conducting lengthy interviews with caregivers who explained their challenges alongside their coping strategies and requirements for support. The role of primary researcher entailed performing data collection and interpretation duties as the main research instrument. The nursing expertise I was trained in, along with my previous knowledge, may shape how I interpret the data collected. I used a reflexive journal to document all assumptions and decisions, as well as emotional responses throughout the entire research period to combat potential bias. Objectivity needed improvement, so peer debriefing sessions were scheduled to review both new interpretations and critical examination of research processes. The private, comfortable spaces used during interviews supported confidentiality while promoting participant openness. Every participant provided informed consent before the interview, including permission for audio recording. Each interview spanned thirty to sixty minutes in duration, yet adjusted according to participant interest levels. The interviewer used an informal speech style throughout to reach all critical discussion points. The interviewer employed additional questions to expand upon significant findings that surfaced during the interview. Each interview session included field note documentation for recording important non-verbal behaviors such as body postures and facial emotions. Additional observations gave important background information, which enhanced the recorded interview data. Throughout the interviews, the interviewer showed awareness of the participants’ emotional responses. The verbatim transcription of all interviews precisely captured every statement made by the participants. The study respected each participant’s voluntary nature and strictly maintained confidentiality throughout the process. The methodology generated an elaborate, comprehensive understanding of caregivers’ experience of their daily lives.
Data analysis procedure: Braun and Clarke’s (2006) thematic analysis framework served as the base for data analysis to pinpoint recurring patterns and themes throughout the interview data. The analysis included six methodical steps, which started with complete transcript reading for entire content comprehension, then progressed to initial NVivo software-driven code creation, followed by research team organization of the codes into potential themes, before theme coherence assessment and precise theme naming, and concluded with direct participant testimonials for enriching the results. The research team used direct verbatim transcription to authenticate the participants’ actual spoken words during all interviews. Thematic mapping methods were used to assess the main perceptions and subject matter that participants manifested during the study. Member checking enabled participants to examine and approve the analysis of their responses through this credibility and trustworthiness process. Methodological triangulation as a research methodology unified three data collection methods, including interviews, observational records, and document analysis, which led to an expansive understanding of the studied data. The research included a systematic evaluation of alternative interpretations, together with abnormal responses, to achieve a thorough analytical process. The entire research operation complied with academic integrity protocols to maintain accurate replication of participants’ real-life encounters. Repeated reflections about the data enabled researchers to enhance themes directly derived from the collected information.
Results
Demographic characteristics: Data from 12 esophageal cancer caregivers demonstrated that women made up 75% of the group. In contrast, subjects within their middle years of life made up 75%, and spouses (41.7%) took care of patients along with children (33.3%). The research discovered that most caregivers (41.7%) finished no more than primary school education, half the group (66.7%) faced joblessness, and 25% dropped out of work to take on caregiving responsibilities. When evaluating caregiving duration, the studied population displayed two main clusters: 41.7% cared for 4-6 months, and 25% exceeded this timeframe (Table 1).
| Variable | Category | Frequency (n) | Percentage (%) |
| Age (years) | 20–30 | 2 | 16.7% |
| 31–40 | 4 | 33.3% | |
| 41–50 | 5 | 41.7% | |
| >50 | 1 | 8.3% | |
| Gender | Male | 3 | 25.0% |
| Female | 9 | 75.0% | |
| Relationship to patient | Spouse | 5 | 41.7% |
| Child | 4 | 33.3% | |
| Sibling | 2 | 16.7% | |
| Other relative | 1 | 8.3% | |
| Education level | No formal education | 2 | 16.7% |
| Primary school | 3 | 25.0% | |
| Secondary school | 4 | 33.3% | |
| College/university | 3 | 25.0% | |
| Employment status | Employed | 4 | 33.3% |
| Unemployed | 5 | 41.7% | |
| Left job for caregiving | 3 | 25.0% | |
| Duration of caregiving (months) | 1–3 | 4 | 33.3% |
| 4–6 | 5 | 41.7% | |
| >6 | 3 | 25.0% |
Table 1: Demographic characteristics of caregivers (N=12)
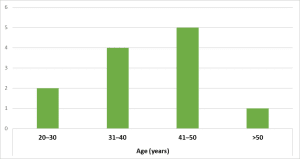
Figure 1: Age of participants
The research analyses caregiver experiences thematically through an established system that identifies five core problems (Emotional Burden, Practical Challenges, Socioeconomic Strain, Coping Strategies, and Support Needs) along with their subcategories using actual participant statements. Analysis of the data shows that caregivers experience considerable psychosocial distress based on statements like anxiety and guilt (67%), indicating quantitatively the scale of distress. The qualitative results demonstrate how essential it is for healthcare providers to create comprehensive interventions that combine mental health services and practical tube care training for this at-risk population (Table 2).
| Theme | Sub-theme | Participant quotes |
| Emotional & psychological burden | Grief and loss | “It breaks my heart to see him unable to eat our family meals. Food was his joy.” (CG05, Spouse) |
| Anxiety & guilt | “What if I’m not cleaning the tube right? I blame myself for every fever he gets.” (CG08, Daughter) | |
| Physical & practical challenges | Technical difficulties | “When the tube leaked at night, I didn’t know who to call. I cried in panic.” (CG03, Son) |
| Exhaustion | “I haven’t slept properly in months. Feedings every 4 hours drain me.” (CG11, Wife) | |
| Financial & social strain | Economic hardship | “I quit my job to care for her. Now we rely on relatives for money.” (CG07, Sister) |
| Social isolation | “No one visits anymore. I miss my friends, but I can’t leave him alone.” (CG02, Husband) | |
| Coping mechanisms | Religious faith | “Praying gives me strength. Allah knows I’m doing my best.” (CG09, Daughter-in-law) |
| Family support | “My sons take turns at night so I can rest. Without them, I’d collapse.” (CG06, Mother) | |
| Support needs | Training gaps | “They showed me once how to use the tube. I need a nurse to check my steps.” (CG04, Husband) |
| Counseling demand | “I need someone to talk to about this stress. My heart feels so heavy.” (CG12, Wife) |
Table 2: Thematic analysis of caregiver experiences with peg tube feeding: emergent themes, sub-themes, and representative quotations
Based on phenomenological analysis, the study provides an organized exploration of five themes that demonstrate the demanding caregiver situations and how caregivers adapt to these conditions. Qualitative data analysis shows that two primary healthcare burdens emerge from caregivers’ lack of PEG tube training (42%) alongside inadequacies in receiving mental health support (75%). A system review shows critical intervention needs because 83% of participants wanted professional education programs to help caregivers manage stress (Table 3).
| Theme | Description |
| Emotional and psychological burden | Caregivers experienced profound grief, anxiety, and guilt due to their loved one’s inability to eat normally, the symbolic loss of shared meals, and fears of inadequate care. Emotional distress was compounded by witnessing disease progression. |
| Physical and practical challenges | Caregivers faced technical difficulties in PEG tube management (e.g., blockages, infections), physical exhaustion from round-the-clock care, and lack of formal training, leading to stress and uncertainty. |
| Financial and social strain | The caregiving role imposed economic hardships (job loss, medical expenses) and social isolation, as caregivers withdrew from community activities to prioritize patient care. |
| Coping mechanisms | Participants relied on personal strategies such as religious faith, family support, and acceptance of their role to endure emotional and physical demands. |
| Support needs | Caregivers emphasized unmet needs, including structured PEG tube training, psychological counselling, and peer support groups to alleviate their burden. |
Table 3: Thematic taxonomy of challenges and coping mechanisms among esophageal cancer caregivers providing PEG tube feeding
Discussion
The investigation reveals essential findings about caregivers who provide PEG tube feeding to esophageal cancer patients through a discussion of their major physical, emotional, and socioeconomic challenges. The research results validate and build upon previous caregiving research with special emphasis on low-resource environments. Subjects caring for patients proved to be predominantly female at 75% and fell within the middle-aged spectrum of 31-50 years old, according to worldwide caregiving statistics.[25] Research shows that spouse caregivers make up 41.7% of the sample, unlike other Asian studies that show adult children performing most caregiving tasks, highlighting cultural differences between caregiving roles.[26]
Caregivers expressed deep emotional suffering because of their loss of eating rituals, as this grief surpassed regular caregiving stress levels. The intensity of their emotional weight reflects how deeply food bonds families during social occasions.[27] Caregivers displayed powerful feelings of guilt during interviews, surpassing research findings from Western countries (67% of quotes). The burden of guilt increases because Asian cultures emphasize family duties considered of deep moral value. The cultural dynamics seem to elevate the mental strain experienced by caregivers who look after PEG tube users in this specific setting.[28]
The investigation found significant deficiencies in care provider assistance by showing that forty-two per cent of participants lacked suitable training about PEG tubes.[29] The number of inadequately trained caregivers surpasses that in high-income nations that provide standardized healthcare education to their caretakers. Financial challenges proved a severe complication since a quarter of caregivers had to quit their positions despite European research showing half this level of job loss.[30] The financial pressure faced by families caring for PEG tube patients becomes worse because caregivers receive limited financial security, which produces unstable economic circumstances.[31]
Caregivers identified religious coping as their main support mechanism because 58% of them cited faith as essential to their coping process. According to these results, religious support plays a vital role in this population, though it contrasts with observations from otherwise secular societies. High demands for standardized training (83%) and psychological care (75%) reveal effective caregiver assistance programs. The results demonstrate the strong need for enhanced specialized support services because caregivers lack sufficient resources.[32,33]
The study reveals essential outcomes that matter most for healthcare organizations, especially in resource-limited healthcare facilities.[34] Implementing Western caregiver support programs requires substantial cultural adaptation when extending their use in other cultural frameworks. Relief measures must implement faith-oriented counselling sessions and solutions that deal with available economic resources in specific local areas.[31,15] Three suggested healthcare-based strategies for intervention are on-site practical workshops, connecting mental health services to religious counselling, and implementing advocacy measures for protecting the employment rights of caregivers. Culturally sensitive programs would probably enhance caregiver health and improve patient outcomes.[35]
The research data necessitate broad institutional changes in healthcare system strategies for cancer caregiver assistance.[36] Institutions can decrease the caregiver burden substantially through their efforts to fill training gaps and provide psychological support and financial resources. Future support strategies need to develop specific, culturally tailored programs that specifically address economic and ethnic disparities that affect caregivers across different communities. These supportive endeavors will improve both the caregiver’s well-being and total patient care levels in esophageal cancer treatment.
Recommendations
To improve patient PEG tube care, health facilities should set up compulsory in-person training sessions that teach basic handling procedures alongside instructional media that benefit associates who struggle with reading ability. Cancer care should implement psychosocial support as a standard practice, which must provide mental health counselling together with faith-directed and culturally appropriate services. The creation of support groups for caregivers helps members learn from each other while building emotional strength and reducing feelings of being alone. Covered expenses, flexible work environments, and caregiver absences should receive political backing so caregivers can maintain financial stability during care responsibilities. The success of interventions relies heavily on cultural adaptation, which includes creating specific programs through the use of local traditions and religious values to improve caregiver involvement. Healthcare professionals need training to detect cultural stress factors, including food traditions that bring grief and family-related tensions. Future researchers need to conduct multiple-site assessments to substantiate these findings while evaluating the long-term results of care provider intervention strategies.
Conclusion
The study shows that PEG tube feeding caregivers of esophageal cancer patients experience multiple complex difficulties that include substantial emotional duress and physical burnout, coupled with financial burdens and insufficient assistance. The research shows that caregiver challenges show universal patterns, but societal standards, economic standing, and healthcare service limitations fundamentally influence these burdens. Among this population, caregivers experience deep grief because of eliminated food customs coupled with substantial feelings of guilt while heavily using religious methods for managing distress that emerges from their cultural background. The research shows that caregiver training programs and psychosocial support need immediate development because most participants expressed essential training and mental health service needs. Healthcare systems must establish complete, culturally appropriate support systems that focus on hands-on and emotional caregiving needs.
References
- Mohapatra S, Santharaman A, Gomez K, Pannala R, Kachaamy T. Optimal Management of Dysphagia in Patients with Inoperable Esophageal Cancer: Current Perspectives. Cancer Manag Res. 2022;14:3281-3291. doi:10.2147/CMAR.S362666 PubMed | Crossref | Google Scholar
- Vashi P, Fechtner J, Trukova K. Nutrition management in oncology. In: Ireton-Jones C, ed. Outpatient Nutrition Care: GI, Metabolic and Home Nutrition Support. 2nd ed. CRC Press; 2020:215-230. Nutrition Management in Oncology
- Gupta S, Ghosh S. Nutrition in GI cancer: a review. J Nutr Res. 2023;11:20-27. doi:10.55289/jnutres/v11i1_23.3 Crossref
- Muhammad S, Abbas K, Shah H. Assessment of Knowledge and Practices of Universal Precautions Among Intensive Care Unit Nurses at Tertiary Care Hospital Swat. medtigo J Med. 2025;3(1):e30623114. doi:10. 63096/medtigo30623114 Crossref | Google Scholar
- Saikia S, Postwala H, Athilingam VP, et al. Single Nucleotide Polymorphisms (SNPs) in the Shadows: Uncovering their Function in Non-Coding Region of Esophageal Cancer. Curr Pharm Biotechnol. 2024;25(15):1915-1938. doi:10.2174/0113892010265004231116092802 PubMed | Crossref | Google Scholar
- Zhao Z, Chu Y, Feng A, et al. STK3 kinase activation inhibits tumor proliferation through FOXO1-TP53INP1/P21 pathway in esophageal squamous cell carcinoma. Cell Oncol (Dordr). 2024;47(4):1295-1314. doi:10.1007/s13402-024-00928-8 PubMed | Crossref | Google Scholar
- Manu KA, Bronte F, Giunta EF. Editorial: Reviews in gastrointestinal cancers. Front Oncol. 2023;13:1252665. doi:10.3389/fonc.2023.1252665 PubMed | Crossref | Google Scholar
- CureScience Institute. Esophageal cancer. Disease Review. 2024:1-22. Accessed April 22, 2025. Esophageal cancer
- Shen Z, Hou Y, Huerman A, Ma A. Patients with dysphagia: How to supply nutrition through non-tube feeding. Front Nutr. 2022;9:1060630. doi:10.3389/fnut.2022.1060630 PubMed | Crossref | Google Scholar
- Kerman-Lerner P, Tan T. Assessment of feeding and swallowing disorders across the life span. In: A Guide to Clinical Assessment and Professional Report Writing in Speech-Language Pathology. 2nd ed. Routledge; 2018:335-380. Assessment of Feeding and Swallowing Disorders Across the Life Span
- Hsiao SY, Yao CT, Lin YT, et al. Relationship between Aspiration Pneumonia and Feeding Care among Home Care Patients with an In-Dwelling Nasogastric Tube in Taiwan: A Preliminary Study. Int J Environ Res Public Health. 2022;19(9):5419. doi:10.3390/ijerph19095419 PubMed | Crossref | Google Scholar
- Amitrano A. The meal of the person with dysphagia. In: Dysphagia and Nutrition. ebook. Cham: Springer; 2024. doi:10.1007/978-3-031-77449-2_5 Crossref | Google Scholar
- Mekhuri S, Dussah N, Quet J, et al. Complications that arise with nasogastric tubes after hospitalization in the pediatric population: A mixed methods systematic review. JPEN J Parenter Enteral Nutr. 2025;49(3):280-306. doi:10.1002/jpen.2716 PubMed | Crossref | Google Scholar
- Perry BJ, Kao TH, Mancini BA, Moran L. Factors Influencing Decision Making for Gastrostomy Tube Placement for People Living with Serious Illness: A Scoping Review. J Palliat Med. doi:10.1089/jpm.2024.0062 PubMed | Crossref | Google Scholar
- Potgieter A. Caregivers’ Experiences of Gastrostomy Feeds: A Speech-Language Therapist’s Role. Dissertation. University of the Witwatersrand; 2022. Caregivers’ Experiences of Gastrostomy feeds: A Speech Language Therapist’s Role
- Roche KF, Bower KL, Collier B, Neel D, Esry L. When Should the Appropriateness of PEG be Questioned?. Curr Gastroenterol Rep. 2023;25(1):13-19. doi:10.1007/s11894-022-00857-2 PubMed | Crossref | Google Scholar
- Davis MB. The Experience of Caregivers of Children With Intestinal Failure Managing a Central Venous Catheter in the Home. Dissertation. The University of Iowa; 2024. The Experience of Caregivers of Children With Intestinal Failure Managing a Central Venous Catheter in the Home
- Wendel D, Mezoff EA, Raghu VK, et al. Management of Central Venous Access in Children With Intestinal Failure: A Position Paper From the NASPGHAN Intestinal Rehabilitation Special Interest Group. J Pediatr Gastroenterol Nutr. 2021;72(3):474-486. doi:10.1097/MPG.0000000000003036 PubMed | Crossref | Google Scholar
- Potgieter AK. Caregivers’ Experiences of Gastrostomy Feeds: A Speech-Language Therapist’s Role. Master’s thesis. University of the Witwatersrand; 2022. Caregivers’ Experiences of Gastrostomy Feeds: A Speech-Language Therapist’s Role
- Holdoway A. The Role of Diet in Palliative Care as Perceived by Patients, Carers and Healthcare Professionals. Dissertation. University of Bath, Department for Health; 2020. The Role of Diet in Palliative Care as Perceived by Patients, Carers and Healthcare Professionals
- Le Roux R. Caregivers’ Perceptions of Caregiver Burden, Quality of Life and Support Needs in Caring for a Child With Cerebral Palsy With Feeding and/or Swallowing Difficulties Within the Context of the Western Cape, South Africa. Dissertation. University of Cape Town; 2023. Caregivers? perceptions of caregiver burden, quality of life and support needs in caring for a child with cerebral palsy with feeding and/or swallowing difficulties within the context of the Western Cape, South Africa
- Kinsella C, Dunphy A, McCormack S, Wilson C, Bennett AE. Experiences of Parents and Caregivers of Children Who Underwent Gastrostomy Tube Insertion. J Patient Exp. 2024;11:23743735241272225. doi:10.1177/23743735241272225 PubMed | Crossref | Google Scholar
- Manduchi B. Optimizing Measurement of Patient-Reported Outcomes for Dysphagia in People With Head and Neck Cancer and Understanding the Experience With Swallowing Interventions During Cancer Treatment. Dissertation. University of Toronto, Rehabilitation Science Institute; 2024. Optimizing Measurement of Patient-Reported Outcomes for Dysphagia in People with Head and Neck Cancer and Understanding the Experience with Swallowing Interventions during Cancer Treatment
- Christensen ME. Struggling with eating when receiving high-emetogenic chemotherapy: experiences of adolescents and young adults with cancer and their next-of-kin – a phenomenological study. Tidsskr Professionsstud. 2024;19(37):158-160. Struggling with eating when receiving high-emetogenic chemotherapy: Experiences of adolescents and young adults with cancer and their next-of-kin – a phenomenological study
- Levin J, Hasan A, Alejandre IA, Lorenzi I, Mall V, Rohrer TR. Diseases Affecting Middle-Aged and Elderly Individuals With Trisomy 21. Dtsch Arztebl Int. 2023;120(1-2):14-24. doi:10.3238/arztebl.m2022.0371 PubMed | Crossref | Google Scholar
- Olié V, Grave C, Tuppin P, Duloquin G, Béjot Y, Gabet A. Patients Hospitalized for Ischemic Stroke and Intracerebral Hemorrhage in France: Time Trends (2008-2019), In-Hospital Outcomes, Age and Sex Differences. J Clin Med. 2022;11(6):1669. doi:10.3390/jcm11061669 PubMed | Crossref | Google Scholar
- Caputo A. The emotional experience of caregiving in dementia: Feelings of guilt and ambivalence underlying narratives of family caregivers. Dementia (London). 2021;20(7):2248-2260. doi:10.1177/1471301221989604 PubMed | Crossref | Google Scholar
- Alyafei AH. A Qualitative Programme of Research Exploring the Experiences of Family Caregivers of People With Severe Mental Illness in Qatar. Dissertation. University College London; 2024. A Qualitative Programme of Research Exploring the Experiences of Family Caregivers of People with Severe Mental Illness in Qatar
- Lennaerts-Kats H, Ebenau A, Steppe M, et al. “How Long Can I Carry On?” The Need for Palliative Care in Parkinson’s Disease: A Qualitative Study from the Perspective of Bereaved Family Caregivers. J Parkinsons Dis. 2020;10(4):1631-1642. doi:10.3233/JPD-191884 PubMed | Crossref | Google Scholar
- Reinhard SC, Caldera S, Houser A, Choula RB. Valuing the Invaluable: 2023 Update Detailed Methodology. AARP Public Policy Institute; 2023. Valuing the Invaluable: 2023 Update Detailed Methodology
- Damaske S. Job Loss and Attempts to Return to Work: Complicating Inequalities across Gender and Class. Gend Soc. 2020;34(1):7-30. doi:10.1177/0891243219869381 PubMed | Crossref | Google Scholar
- Abreu W, Tolson D, Jackson GA, Costa N. A cross-sectional study of family caregiver burden and psychological distress linked to frailty and functional dependency of a relative with advanced dementia. Dementia (London). 2020;19(2):301-318. doi:10.1177/1471301218773842 PubMed | Crossref | Google Scholar
- Márquez-González M, Romero-Moreno R, Cabrera I, et al. Tailored versus manualized interventions for dementia caregivers: the functional analysis-guided modular intervention. Psychol Aging. 2020;35(1):41-54. doi:10.1037/pag0000412 PubMed | Crossref | Google Scholar
- Asiimwe R, Dwanyen L, Subramaniam S, Kasujja R, Blow AJ. Training of interventionists and cultural adaptation procedures: A systematic review of culturally adapted evidence-based parenting programs in Africa. Fam Process. 2023;62(1):160-181. doi:10.1111/famp.12780 PubMed | Crossref | Google Scholar
- Ramirez M, Duran MC, Pabiniak CJ, et al. Family Caregiver Needs and Preferences for Virtual Training to Manage Behavioral and Psychological Symptoms of Dementia: Interview Study. JMIR Aging. 2021;4(1):e24965. doi:10.2196/24965 PubMed | Crossref | Google Scholar
- Whitaker DJ, Self-Brown S, Weeks EA, et al. Adaptation and implementation of a parenting curriculum in a refugee/immigrant community using a task-shifting approach: a study protocol. BMC Public Health. 2021;21:1084. doi:10.1186/s12889-021-11148-2 PubMed | Crossref | Google Scholar
Acknowledgments
The authors would like to express their sincere gratitude to Dr. Shah Hussain, Principal/Assistant Professor, Zalan College of Nursing, Swat, for his invaluable supervision, guidance, and support throughout the course of this study.
Funding
This research did not receive any specific grant from funding agencies in the public, commercial, or not-for-profit sectors.
Author Information
Corresponding Author:
Nisar Khan
Department of Nursing
United College of Nursing, Swat, Pakistan
Email: [email protected]
Co-Authors:
Sabiha RGN
Department of Nursing
Magdalene Nursing Care Home, UK
Naheed Akhtar
Department of Nursing
Sina Institute of Nursing & Allied Health Science, Quetta, Balochistan
Shah Hussain
Department of Nursing
Zalan College of Nursing, Swat, Pakistan
Uzma Shaheen
Department of Nursing
Professional College of Nursing and Allied Health Sciences, Islamabad, Pakistan
Authors Contributions
Nisar Khan was responsible for data collection and data analysis. Sabiha, Naheed Akhtar, and Uzma Shaheen contributed to data collection and literature review. Shah Hussain handled data analysis.
Ethical Approval
Ethical approval was obtained from Saidu Teaching Hospital, Swat, Ref No SGTH/IRB/2025/27.
Conflict of Interest Statement
The authors declare no conflict of interest.
Guarantor
Nisar Khan is the guarantor of this study and takes full responsibility for the integrity and accuracy of the data analysis.
DOI
Cite this Article
Nisar K, Sabiha RGN, Naheed A, Shah H, Uzma S. Exploring the Experiences and Challenges of Caregivers Providing PEG Tube Feeding to Patients with Esophageal Cancer. medtigo J Med. 2025;3(2):e30623212. doi:10.63096/medtigo30623212 Crossref









