Author Affiliations
Abstract
Cytomegalovirus (CMV) is a common human herpesvirus that can lead to a variety of clinical manifestations. We report the case of a 40-year-old previously healthy male who presented with a one-week history of easy bruising, fatigue, and pallor. Physical examination revealed multiple petechiae on both lower limbs. The patient’s platelet count was significantly low. Given the clinical presentation and absence of other clear etiologies, a thorough workup was initiated, including viral serologies. Testing revealed a positive result for cytomegalovirus (CMV) IgG, suggesting acute CMV infection. Further investigation confirmed CMV-induced thrombocytopenia, with viral DNA detected in the patient’s blood. The patient started antiviral therapy with ganciclovir and pulse therapy of methylprednisolone. Over the following week, platelet counts gradually improved, and the patient’s symptoms of fatigue and easy bruising resolved. These cases highlight the importance of considering CMV as a potential cause of thrombocytopenia, particularly in patients with nonspecific symptoms like bruising and petechiae. Early diagnosis is critical for effective management, which includes antiviral therapy and supportive care. Clinicians should be aware that CMV-induced thrombocytopenia can occur in immunocompetent individuals, and prompt intervention can lead to favorable outcomes.
Keywords
Cytomegalovirus, Thrombocytopenia, Immunocompetent patient, Low platelets count, Treatment and management.
Introduction
Cytomegalovirus (CMV) is known to cause thrombocytopenia, a condition characterized by low platelet counts. Although more commonly associated with immunocompromised patients, CMV-induced thrombocytopenia can also occur in immunocompetent individuals.[1] Cytomegalovirus (CMV) infection can cause thrombocytopenia through multiple mechanisms, including bone marrow suppression, immune-mediated destruction, and increased platelet consumption.[2]. This case report details the presentation of CMV-induced thrombocytopenia in a previously healthy patient, underscoring the importance of considering CMV in the differential diagnosis of thrombocytopenia.
Case Presentation
Case Report-1
A 40-year-old otherwise healthy male presented with a 1-week history of easy bruising, fatigue, and epistaxis. Patient also developed rash on Bilateral lower limbs and was found to have enlarged liver and spleen. Three months back, the patient had an episode of bloody diarrhea for 1 week, which was treated with homeopathic medications of unknown origin at home. Initial laboratory tests revealed a platelet count of 18,000/µL (normal range: 150,000–450,000/µL). The patient had no recent travel history or known exposure to infectious agents.
Location: The location of this case report is Advanced International Hospital (AIH), G-8 Markaz, Islamabad, Pakistan. AIH is a 200-bedded tertiary care hospital in central Islamabad, Pakistan.
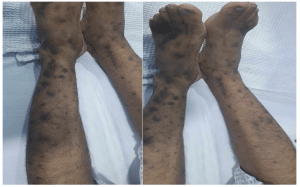
Figure 1: Rashes on bilateral lower limbs
Diagnostic evaluation: Initial differential diagnoses included idiopathic thrombocytopenic purpura (ITP), viral infections, and bone marrow disorders. A comprehensive workup included a complete blood count, peripheral blood smear, and specific viral serologies. The peripheral blood smear was notable for a few giant platelets and no evidence of atypical cells. Bone marrow biopsy was offered but refused by the patient.
Serological testing revealed positive CMV IgG antibodies, with the CMV polymerase chain reaction (PCR) facility not available at that time, showing previous CMV infection. Other infectious causes and autoimmune conditions were ruled out.
Case Report-2
A recent case report highlighted a 34-year-old immunocompetent patient who presented with isolated thrombocytopenia. The patient exhibited a platelet count of 80,000/µL without any significant bleeding or other symptoms. Initial investigations, including peripheral blood smear and bone marrow biopsy, did not reveal any underlying hematological malignancy. The patient’s CMV serology showed positive IgM and IgG antibodies, suggesting a recent or active CMV infection. Further diagnostic work-up confirmed CMV infection as the likely etiology of thrombocytopenia.
Diagnostic considerations: Diagnosing CMV-induced thrombocytopenia involves a combination of clinical, serological, and sometimes molecular tests:
- Serology: CMV IgM and IgG antibodies help confirm recent or active infection.
- Molecular testing: PCR for CMV DNA in blood or other tissues can provide definitive evidence of active CMV infection.
- Bone marrow biopsy: Although not always necessary, a bone marrow biopsy can help rule out other causes of thrombocytopenia and assess the direct effects on megakaryocytes.
It is essential to distinguish CMV-induced thrombocytopenia from other potential causes, including autoimmune disorders, hematological malignancies, and other infections. A thorough evaluation of clinical history and laboratory findings is crucial for accurate diagnosis.[3]
Case Management
Case Report-1
The patient was treated with supportive care, including monitoring of platelet counts and symptomatic management of bleeding symptoms. Patient was started on Injectable methylprednisolone pulse therapy, i.e, 1 gm IV for 03 consecutive days, along with Injectable Ganciclovir 5mg/kg q12 hourly. Patient platelet counts improved gradually over the next few days and improved to above 1,00,000/uL. Patient was then shifted to oral prednisolone along with oral valganciclovir 900mg q12 hourly and was discharged home to come for follow-up. During his follow-up, he experienced weight gain of 5.6kg in 1 month. Apart from that, the patient did not develop any significant side effects from the medications. The patient was given intravenous ganciclovir first due to its ready availability and relative cost-effectiveness. The patient was later switched to oral valganciclovir due to his inability to afford continued hospital admission. It was easier for the patient to take oral tablets home. Renal function tests and complete blood count were regularly monitored on his follow-ups, and he was followed up for 3 months with no signs of relapse.
Case Report-2
The management of CMV-induced thrombocytopenia typically focuses on treating the underlying CMV infection. In present immunocompetent patients, treatment often involves:
- Supportive care: Regular monitoring of platelet counts and symptomatic management as needed.
- Antiviral therapy: In cases of severe CMV infection or significant symptoms, antiviral medications such as ganciclovir or foscarnet may be considered
For immunocompromised patients or those with severe manifestations, more aggressive antiviral treatment may be necessary, and consultation with an infectious disease specialist is recommended.
Discussion
CMV-induced thrombocytopenia is a rare but important consideration in patients presenting with unexplained thrombocytopenia. This case supports previous reports that CMV can cause thrombocytopenia in immunocompetent individuals, often presenting with nonspecific symptoms such as bruising and fatigue.[4,5] The management of CMV-induced thrombocytopenia includes antiviral therapy and platelet support, with good outcomes typically seen in immunocompetent patients when treatment is initiated promptly. Early recognition is crucial for favorable outcomes, and clinicians should consider CMV in the differential diagnosis of thrombocytopenia in patients with no obvious etiology.[6]
Thrombocytopenia in CMV infection is hypothesized to result from multiple mechanisms, including:
- Direct viral cytopathic effects: On bone marrow progenitor cells, leading to decreased platelet production.
- Immune-mediated destruction: via anti-platelet antibodies or molecular mimicry.
- Splenic sequestration: Due to CMV-induced splenomegaly, leading to increased platelet clearance.[7]
The differential diagnosis of thrombocytopenia includes ITP, drug-induced thrombocytopenia, disseminated intravascular coagulation (DIC), and other viral infections.[8] In these cases, CMV was identified as the causative factor due to the presence of viremia and the exclusion of other etiologies.
Conclusion
CMV-induced thrombocytopenia, though rare, is a key consideration in isolated thrombocytopenia. Early diagnosis through clinical evaluation, serological, and molecular testing is essential for effective management and to prevent unnecessary treatments. These cases highlight the importance of including CMV in thrombocytopenia workups. Further research is needed to enhance treatment strategies and achieve long-term remission.
References
- Echcharii N, Chekhlabi N, Dini N. A Case of Cytomegalovirus Infection With Severe Thrombocytopenia in an Infant Who Was Successfully Managed With Antiviral Therapy. Cureus. 2022;14(10):e30640. doi:10.7759/cureus.30640
PubMed | Crossref | Google Scholar - Sachdev PS, Blacker D, Blazer DG, et al. Classifying neurocognitive disorders: the DSM-5 approach. Nat Rev Neurol. 2014;10(11):634-642. doi:10.1038/nrneurol.2014.181
PubMed | Crossref | Google Scholar - Kotton CN, Kumar D, Caliendo AM, et al. The Third International Consensus Guidelines on the Management of Cytomegalovirus in Solid-organ Transplantation. Transplantation. 2018;102(6):900-931. doi:10.1097/TP.0000000000002191
PubMed | Crossref | Google Scholar - Jameson JL, Fauci AS, Kasper DL, et al, eds. Harrison’s Manual of Internal Medicine. 20th ed. McGraw-Hill Education; 2018.
Harrison’s Principles of Internal Medicine, 21e | AccessMedicine | McGraw Hill Medical - Maita H, Tonosaki K, Ozawa A, et al. Severe thrombocytopenia caused by cytomegalovirus infection in an immunocompetent adult: A case report. SAGE Open Med Case Rep. 2024;12:2050313X241266766. doi:10.1177/2050313X241266766
PubMed | Crossref | Google Scholar - Choi YL, Kim JA, Jang KT, et al. Characteristics of cutaneous cytomegalovirus infection in non-acquired immune deficiency syndrome, immunocompromised patients. Br J Dermatol. 2006;155(5):977-982. doi:10.1111/j.1365-2133.2006.07456.x
PubMed | Crossref | Google Scholar - van der Poll T, van de Veerdonk FL, Scicluna BP, Netea MG. The immunopathology of sepsis and potential therapeutic targets. Nat Rev Immunol. 2017;17(7):407-420. doi:10.1038/nri.2017.36
PubMed | Crossref | Google Scholar - Kuriakose D, Xiao Z. Pathophysiology and Treatment of Stroke: Present Status and Future Perspectives. Int J Mol Sci. 2020;21(20):7609. doi:10.3390/ijms21207609
PubMed | Crossref | Google Scholar
Acknowledgments
Not reported
Funding
Not reported
Author Information
Corresponding Author:
Waleed Zahoor
Department of Emergency Medicine
Advanced International Hospital, Islamabad, Pakistan
Email: waleedzahoor21@yahoo.com
Co-Authors:
Ahmad Naseer, Hamid Zafar Ansari
Department of Internal Medicine
Advanced International Hospital, Islamabad, Pakistan
Amina Azhar
Department of Cardiology
Advanced International Hospital, Islamabad, Pakistan
Authors Contributions
Waleed Zahoor was responsible for writing the case report, obtaining consent, and seeing the patient during the initial presentation. Ahmad Naseer managed the patient as the primary consultant, monitored his progress, and devised the treatment plan. Hamid Zafar Ansari conducted the literature review and monitored the patient during his 3-day admission phase. Amina Azhar contributed to the literature review and assisted in writing the case report.
Ethical Approval
The ethical committee of Advanced International Hospital has approved this case report on January 01, 2025. Consent from the patient was obtained.
Conflict of Interest Statement
Not reported
Guarantor
None
DOI
Cite this Article
Waleed Z, Ahmad N, Hamid ZA, Amina A. Cytomegalovirus Induced Thrombocytopenia in an Immunocompetent Patient. medtigo J Med. 2025;3(1):e30623139. doi:10.63096/medtigo30623139 Crossref









