Author Affiliations
Abstract
Background: Integrating nursing theory with clinical skills ensures safe patient care. However, interns face theory-practice gaps due to limited supervision, heavy workload, resource shortages, and psychological stress, particularly in low-resource government hospitals.
Aim: This study aimed to evaluate the individual, institutional, and environmental barriers affecting the integration of nursing knowledge and clinical skills into clinical practice among nursing interns at Saidu Group of Teaching Hospital (SGTH), Swat, and to examine the association between these barriers and theory–practice integration.
Methodology: The study was a quantitative analytical cross-sectional study and involved 147 nursing interns in SGTH, Swat. The data were gathered through a validated self-administered questionnaire that consisted of demographics, theory-practice integration, and barriers (individual, institutional, and environmental), which were analyzed using descriptive statistics and Chi-square tests.
Results: Most of the interns were males (76.2%) and those with an average age of 24-26 (46.3%). There were moderate to high barriers: individual (86.4%), institutional (87.7%), and environmental (89.1%). The majority of interns (60.5%) identified a gap between theory and practice, and stress and the use of trial-and-error techniques were observed. The chi-square test indicated that perceived barriers were significantly related to theory-practice integration (χ² = 29.84, df = 4, p = 0.001), with more barriers being associated with less knowledge and skills integration.
Conclusion: Individual, institutional, and environmental barriers hinder the application of nursing knowledge in practice. Targeted interventions, structured supervision, improved resources, and mentorship programs are essential to bridge the theory–practice gap, enhance clinical competence, and ensure patient safety.
Keywords
Nursing interns, Theory-practice gap, Clinical skills, Barriers, Integration, Patient safety, Tertiary care.
Introduction
Nursing knowledge is the theoretical knowledge gained through formal education, whereas clinical skills are the practical and psychomotor skills that are necessary in providing care to the patient. The real healthcare setting, in which the nursing interns can put into practice the acquired knowledge and skills, is clinical practice.[1] Among nurses, new entrants are nursing interns who are undertaking supervised clinical training. The barriers are factors that discourage effective application of theory in practice, including organizational, educational, and personal barriers. Nursing knowledge and clinical skills must be integrated to provide safe, competent, and evidence-based nursing care.[2]
One of the issues that has been reported frequently in the literature of nursing education is the difficulty in incorporating nursing knowledge and clinical expertise into practice. Studies have revealed that a large proportion of nursing interns are struggling with the internship.[3] It has been argued that nearly half of all nursing interns throughout the world report a discernible theory-practice gap. The problem is greater in the hospitals of the public sector, in which the workload is significant.[4] The absence of supervision and inappropriate learning material are also causes of high rates of this problem. This is an irreparable gap with negative implications for nursing performance and patient outcomes.[5]
A nursing internship is one of the important stages of the development of a professional during which theoretical knowledge should be demonstrated in effective clinical practice. Some of the tasks that the nursing interns are required to undertake during this time include patient assessment, medication administration, and general care of the patient. Low confidence and clinical competence are caused by the lack of knowledge and skills integration in the internship process.[6] Many interns are unable to apply classroom learning to clinical situations. Once it is not addressed at the initial stages, this challenge can be furthered to practice. Training internships are therefore necessary to develop qualified nurses.[7]
The level of clinical competence in nursing interns depends on the final determinants in clinical learning environments.[8] Government tertiary care hospitals are typically overcrowded, have high turnover, and lack equipment. This makes it impossible to have supervised practice and practical learning. The nursing interns can be sent to do menial duties without adequate instructions and clarifications. The absence of skills learning reduces confidence and competence levels. Such working conditions hinder practical learning and work development.[9]
Clinical learning entails supervision and mentorship, which are essential components. Seasoned nurses and clinical instructors have to give nursing interns continuous guidance, feedback, and support. The role of patient care is normally imposed on the seniors of government hospitals. This much work limits the supervision and teaching time.[10] Lack of mentorship programs. Lack of skills development is also not addressed with proper mentorship programs. There is a detrimental effect on learning outcomes and professional confidence due to a lack of proper supervision.[11]
The variables of education are significant in the integration of the knowledge of nursing and clinical competencies. The lack of connectivity between the learning programs in the academic world and in clinical practices puzzles the nursing interns.[12] The reduction of readiness to work in real clinical situations is the result of the short-term simulation training in academic programs. Absence of clinical exposure in the learning process suppresses the learning of skills. Theoretical knowledge is possible for nursing interns who are not sure about how to perform procedures. This kind of disparity is a cause of the endemic theory-practice gap.[13]
This has psychological problems that are important as a hindrance to the effective integration of nursing knowledge and skills. It is usual that nursing interns are plagued by anxiety, fear of doing something wrong, and self-doubt.[14] Clinical environments are also stressful due to psychological problems. This is because interns will not want to perform procedures on their own, as they stand the risk of being criticized or negatively evaluated. Emotional stress promotes low motivation to learn and low decision-making ability. These are not only factors that influence learning but also have a negative impact on patient care[15]
The clinical learning experiences require interpersonal relationships within healthcare teams. The absence of effective communication between nursing students and senior staff members inhibits the opportunities in clarifications and mentoring.[16] The hierarchical working structures can dishearten the interns from asking questions. Lack of support and respect for each other reduces active participation in the care of patients. The attitude of the healthcare staff is not supportive and affects learning negatively. Without good relationships at work, the integration of the skills cannot be achieved.[17]
Organizational and administrative factors, which bring barriers to nursing interns, exist as well. Indecision in the role and the duties results in confusion during clinical practice. The interns are also exposed to a lack of orientation programs that help them to know what to expect at the clinics.[18] Lacking standard policies on internships affects the learning uniformity. Learning materials and equipment are not easily available, and restrict the acquisition of the skills. Without the support of the organization, clinical training is impossible.[19]
Patient safety is directly related to nursing interns’ competence. Poor integration of knowledge and skills improves the likelihood of medication errors, inappropriate infection control precaution and a lack of patient assessment. The patients may be placed in danger by interns whose level of clinical competence is low. Successful integration prevents unwanted adverse incidents. Good nursing services increase patient satisfaction and health outcomes. Patient safety is therefore a priority of clinical training strengthening.[20]
Other problems that influence nursing education in the low- and middle-income countries are through the healthcare systems. Resource limitations increase the obstacles to learning because of insufficient staffing and training resources. Most of the nursing interns might be left working under pressure with minimal support. Modern medical equipment is not readily available, thus constraining skills practice. These problems continue to widen the theory practice divided into clinical practice. The systemic barriers to nursing education should be addressed.[21]
The tertiary care hospitals operated by the Swat government face a large and diverse population, to which they provide healthcare services. The shortage of sufficient staff and massive patient load led to working under difficult circumstances. The nursing interns in such hospitals have a number of learning challenges. The culture and work dynamics also have an extra impact on the experience of clinical training. Poor clinical education does not allow skills development. One should build the perception of local impediments to improve the experiences of an internship.[22]
There have been few local studies on the impediments to incorporating nursing knowledge and clinical skills in Swat. Lack of evidence that is context-related limits the proper policy development. Determining obstacles will help teachers and administrators to enhance training courses. Clinical education and supervision can be strengthened with the help of evidence-based interventions. Enhanced training internships lead to better competence and quality of patient care. The research fills a gap in the field of nursing education research.[23]
Methodology
The study design was a quantitative analytic cross-sectional research design to determine the obstacles to implementing nursing knowledge and clinical skills into practice among nursing interns in a government tertiary care hospital in Swat. The participants of the study were nursing interns who were receiving clinical training in the course of the study in various units, including medical-surgical, emergency, pediatrics, and obstetrics/gynecology. The overall sample size of 147 nursing interns was used. This sample was calculated with G+Power software (version 3.1.9.7) of a chi-square test, where the medium effect size (w = 0.30), the level of significance (0.05), the power (0.80), and the number of degrees of freedom (4) were used. Another 10% was added to consider the possible non-response. A convenience sampling method was employed in selecting the participants in accordance with pre-determined inclusion and exclusion criteria.
Data collection procedure: The study was approved by the Graduate Committee of the respective nursing institution, and then the nursing administration of the hospital gave its consent. Respondents were well informed about the objective of the study, and informed consent was signed and handed in writing before data collection. The information was gathered through a self-administered and validated questionnaire in five parts with closed-ended questions on a 3-point Likert scale. The reliability of the instrument was evaluated through a pilot study done on 25 nursing interns. The alpha value of Cronbach was 0.731, which is an acceptable internal consistency. There were both positive and negative worded items, as well as reverse coding, where necessary, to ensure that it was accurate.
Data analysis procedure: The Statistical Package of Social Sciences (SPSS) version 25.0 was used to enter and analyze the data. Demographic variables, as well as perceived barriers, were summarized using descriptive statistics: frequencies and percentages. The number of predominant barriers was established based on the percentage of participants who chose to agree. The barriers were grouped into low, moderate, and high based on set percentages. The chi-square test was employed to analyze the relationships between theory-practice integration and individual, institutional, and environmental obstacles. A p-value of below 0.05 was said to be statistically significant. Findings were tabulated and presented in figures.
Results
Demographic characteristics of nurses: The demographic characteristics of the nursing interns (n = 147) revealed that the majority were male (76.2%), while females comprised 23.8% of the sample, indicating a higher representation of males in the internship program. Most participants were aged between 24 and 26 years (46.3%), followed by 21–23 years (37.4%), and a smaller proportion were above 26 years (16.3%), showing a predominantly young workforce. All interns were enrolled in the GBSN program (100%). Regarding the duration of internship, most were in the 9–12 months period (76.2%), while fewer were in the 6–9 months (13.7%) and 3–6 months (10.1%) phases. The distribution across clinical rotations was fairly even, with the highest representation in medical (19.0%) and emergency (17.0%) units, followed by surgical (17.7%), gynecology/obstetrics (16.3%), ICU (13.6%), pediatric (12.2%), and other areas (4.1%). In terms of previous clinical experience, 40.1% had prior experience, whereas the majority (59.9%) had no prior exposure, highlighting variability in practical exposure among interns. These characteristics provide a comprehensive overview of the sample and context for analyzing the barriers to integration of nursing knowledge and clinical skills.
| Variable | Category | Frequency (n) | Percentage (%) |
| Gender | Male | 112 | 76.2 |
| Female | 35 | 23.8 | |
| Age (years) | 21–23 | 55 | 37.4 |
| 24–26 | 68 | 46.3 | |
| Above 26 | 24 | 16.3 | |
| Program | GBSN | 147 | 100 |
| Current month of internship | 4-6 months | 15 | 10.1 |
| 7-9 months | 20 | 13.7 | |
| 10-12 months | 112 | 76.2 | |
| Area of rotation | Medical | 28 | 19.0 |
| Surgical | 26 | 17.7 | |
| ICU | 20 | 13.6 | |
| Emergency | 25 | 17.0 | |
| Gyne/Obs | 24 | 16.3 | |
| Pediatric | 18 | 12.2 | |
| Other | 6 | 4.1 | |
| Previous clinical experience | Yes | 59 | 40.1 |
| No | 88 | 59.9 |
Table 1: Demographic characteristics of nursing interns
The results regarding theory–practice integration among nursing interns revealed that slightly more than half of the participants (51.0%) reported applying most of the skills learned in the classroom during their clinical duties, while 27.2% were neutral and 21.8% disagreed. A majority of 60.5% perceived a gap between theory and clinical practice, indicating challenges in translating academic knowledge into real-life patient care. Over half of the interns (51.7%) reported feeling stressed when performing skills independently, highlighting the psychological impact of clinical responsibilities. Most participants (59.2%) stated that they make clinical decisions based on their theoretical knowledge, demonstrating some level of effective integration. Around 51.0% felt that their academic learning prepared them well for clinical situations, whereas 30.6% were neutral and 18.4% disagreed. A considerable proportion (42.9%) admitted depending on trial and error rather than academic knowledge, suggesting occasional reliance on experiential learning. These findings reflect that while nursing interns are partially able to integrate theory into practice, gaps, stress, and dependence on non-academic approaches still exist. Overall, the data indicate moderate theory–practice integration with areas that require further support and structured guidance.
| Statement | Disagree n (%) | Neutral n (%) | Agree n (%) |
| Apply most classroom skills during clinical duties | 32 (21.8) | 40 (27.2) | 75 (51.0) |
| There is a difference between theory and practice | 20 (13.6) | 38 (25.9) | 89 (60.5) |
| Feel stressed performing skills independently | 25 (17.0) | 46 (31.3) | 76 (51.7) |
| Make clinical decisions based on theoretical knowledge | 19 (12.9) | 41 (27.9) | 87 (59.2) |
| Academic learning is well-prepared for clinical situations | 27 (18.4) | 45 (30.6) | 75 (51.0) |
| Depending on trial and error rather than academic knowledge | 35 (23.8) | 49 (33.3) | 63 (42.9) |
Table 2: Theory-practice integration among nursing interns
The findings on individual barriers among nursing interns indicate that slightly more than half of the participants (51.7%) reported low confidence when applying their knowledge during patient care, while 27.9% were neutral and 20.4% disagreed. Similarly, 51.7% of interns felt anxious while performing clinical skills, reflecting the psychological challenges faced in real clinical settings. More than half (55.8%) reported effective communication with patients, though a notable proportion remained neutral (30.6%) or disagreed (13.6%). About 51.0% hesitated to perform skills due to fear of making mistakes, demonstrating that apprehension can limit practical application. A majority (64.6%) expressed motivation to apply their academic knowledge in clinical practice, indicating willingness despite barriers. Nearly half of the interns (49.0%) managed their time effectively during clinical duties, while the rest faced challenges in time management. These results suggest that individual barriers, including confidence, anxiety, fear of errors, and time management, moderately affect the integration of theoretical knowledge into practice. Overall, personal factors play a significant role in shaping interns’ ability to implement their learned skills in clinical settings.
| Statement | Disagree n (%) | Neutral n (%) | Agree n (%) |
| Low confidence in applying knowledge | 30 (20.4) | 41 (27.9) | 76 (51.7) |
| Feel anxious during skill application | 25 (17.0) | 46 (31.3) | 76 (51.7) |
| Communicate effectively with patients | 20 (13.6) | 45 (30.6) | 82 (55.8) |
| Hesitate due to fear of mistakes | 28 (19.0) | 44 (29.9) | 75 (51.0) |
| Motivated to apply academic knowledge | 15 (10.2) | 37 (25.2) | 95 (64.6) |
| Manage time effectively during clinical duties | 27 (18.4) | 48 (32.7) | 72 (49.0) |
Table 3: Individual barriers
The results regarding institutional barriers among nursing interns revealed several challenges affecting the integration of theoretical knowledge into clinical practice. A majority of interns (55.8%) reported that nursing supervisors rarely provided supervision during clinical procedures, while 25.2% were neutral and 19.0% disagreed. More than half (61.2%) indicated that the lack of equipment hindered their ability to perform clinical skills, reflecting resource-related constraints. Only 42.9% felt that proper orientation was provided for new interns, with 32.7% neutral and 24.5% disagreeing. Similarly, 42.2% reported sufficient learning resources, such as models and charts, were available, while the remainder indicated neutral (30.6%) or inadequate resources (27.2%). About 49.7% received adequate feedback on their performed skills, showing a moderate level of guidance. Lastly, 42.2% acknowledged the availability of special training programs for practical learning, suggesting gaps in structured institutional support. Overall, institutional factors, including supervision, equipment, orientation, feedback, and training programs, moderately influenced the application of nursing knowledge into practice among interns.
| Statement | Disagree n (%) | Neutral n (%) | Agree n (%) |
| A nursing supervisor rarely provides supervision | 28 (19.0) | 37 (25.2) | 82 (55.8) |
| Lack of equipment hinders skill performance | 22 (15.0) | 35 (23.8) | 90 (61.2) |
| Proper orientation provided for new interns | 36 (24.5) | 48 (32.7) | 63 (42.9) |
| Sufficient learning resources available | 40 (27.2) | 45 (30.6) | 62 (42.2) |
| Adequate feedback on skills | 30 (20.4) | 44 (29.9) | 73 (49.7) |
| Special training programs are available | 35 (23.8) | 50 (34.0) | 62 (42.2) |
Table 4: Institutional barriers
The findings related to environmental barriers indicate several factors affecting the nursing interns’ ability to integrate knowledge and skills into clinical practice. More than half of the participants (55.8%) agreed that they had enough opportunities to practice their skills, whereas 27.2% were neutral and 17.0% disagreed. A majority (57.1%) reported that improper documentation by staff could lead to mistakes, reflecting systemic challenges. Around 62.6% of interns perceived staff nurses as cooperative during skill performance, showing positive interpersonal support. However, nearly half (49.7%) noted that the overflow of visitors reduced space for performing procedures, and 47.0% indicated that high patient assignments hindered skill application. Most interns (59.9%) agreed that the clinical environment was safe for performing skills, suggesting overall adequate safety. Overall, environmental factors such as space, patient load, staff cooperation, and safety moderately influenced the ability of interns to apply theoretical knowledge in practice.
| Statement | Disagree n (%) | Neutral n (%) | Agree n (%) |
| Enough opportunities to practice skills | 25 (17.0) | 40 (27.2) | 82 (55.8) |
| Improper documentation may cause mistakes | 22 (15.0) | 41 (27.9) | 84 (57.1) |
| Staff nurses cooperate during skill performance | 20 (13.6) | 35 (23.8) | 92 (62.6) |
| Overflow of visitors reduces space for procedures | 28 (19.0) | 46 (31.3) | 73 (49.7) |
| High patient assignment hinders skill application | 30 (20.4) | 48 (32.7) | 69 (47.0) |
| An environment safe for performing skills | 18 (12.2) | 41 (27.9) | 88 (59.9) |
Table 5: Environmental barriers
The overall prevalence of barriers to integrating nursing knowledge and clinical skills among nursing interns was assessed across individual, institutional, and environmental domains. For individual barriers, 13.6% of participants reported low barriers, 46.3% reported moderate barriers, and 40.1% experienced high barriers, indicating a substantial proportion faced personal challenges such as low confidence, anxiety, and time management issues. Regarding institutional barriers, 12.2% reported low, 44.2% moderate, and 43.5% high barriers, highlighting organizational challenges like inadequate supervision, lack of equipment, and insufficient training programs. Environmental barriers were reported as low by 10.9%, moderate by 45.6%, and high by 43.5%, reflecting external constraints such as limited practice opportunities, overcrowding, high patient load, and safety concerns. These results suggest that moderate to high barriers are prevalent among nursing interns, with institutional and environmental factors slightly more pronounced than individual barriers.
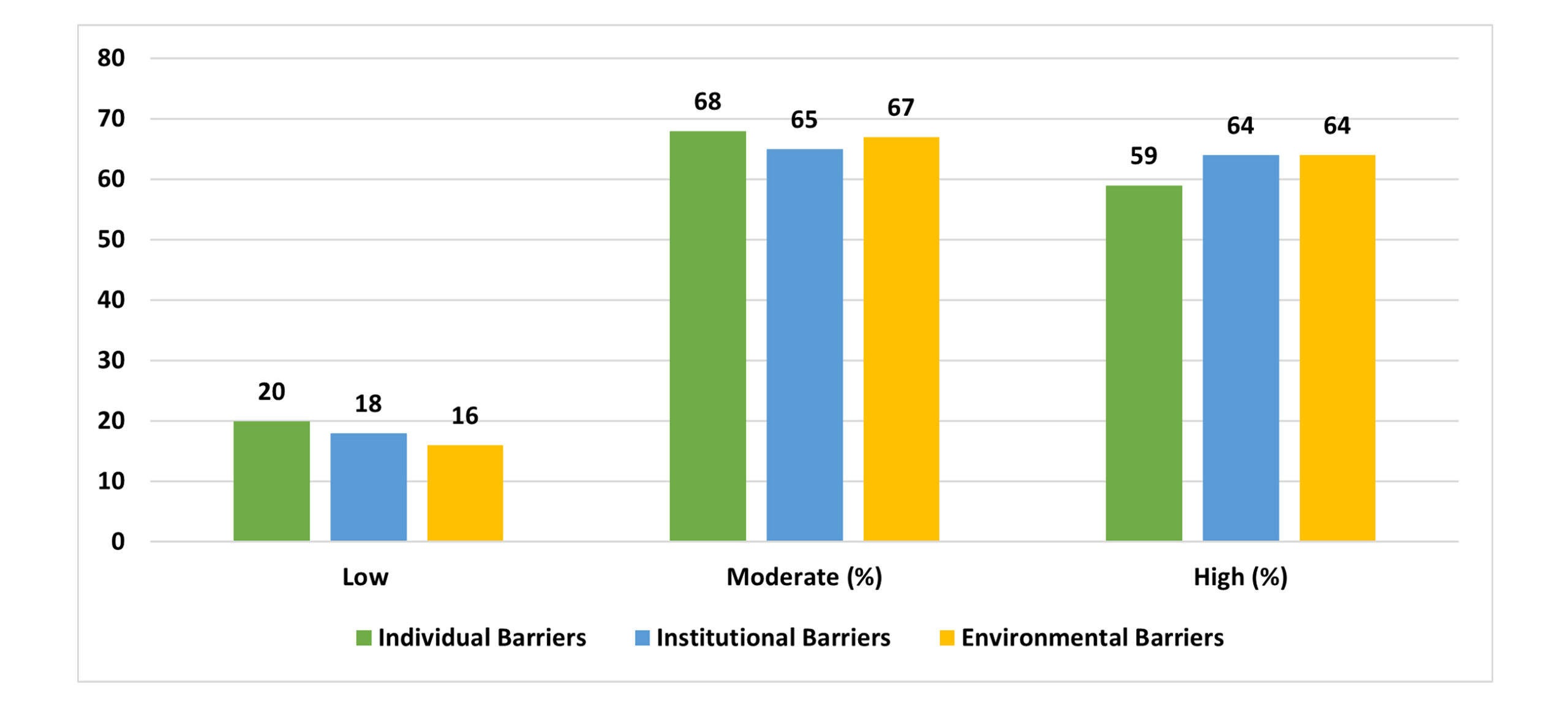
Figure 1: Prevalence of barriers based on agreement
The crosstabulation of perceived barriers and theory–practice integration among 147 nursing interns at SGTH Swat showed that interns experiencing low barriers mostly reported low integration of nursing knowledge and clinical skills into practice, with 56.3% in the low integration category. Those facing moderate barriers were predominantly in the moderate integration group (62.5%), while interns with high barriers largely fell into the high integration category (62.8%). The overall distribution indicates that higher perceived barriers are associated with greater challenges in applying theoretical knowledge to clinical practice. The Chi-square test confirmed a statistically significant association between perceived barriers and theory–practice integration (χ² = 29.84, df = 4, p = 0.001). This suggests that the intensity of barriers—whether individual, institutional, or environmental—has a meaningful impact on the interns’ ability to implement learned skills. The findings highlight the importance of addressing barriers to improve the practical application of knowledge. Interventions targeting high-barrier areas could enhance clinical competence and confidence among nursing interns. The results provide evidence for administrators and educators to focus on supportive strategies that bridge the theory–practice gap.
| Perceived barriers | Theory-practice integration | |||
| Low n (Row %) | Moderate n (Row %) | High n (Row %) | Total n (%) | |
| Low barriers | 18 (56.3) | 10 (31.3) | 4 (12.5) | 32 (100) |
| Moderate barriers | 12 (16.7) | 45 (62.5) | 15 (20.8) | 72 (100) |
| High barriers | 4 (9.3) | 12 (27.9) | 27 (62.8) | 43 (100) |
| Total | 34 (23.1) | 67 (45.6) | 46 (31.3) | 147 (100) |
| Chi-Square Test | χ² = 29.84 | df = 4 | p = 0.001 | |
Table 6: Association between perceived barriers and theory-practice integration among nursing interns
Discussion
The results of the present study suggested that there were numerous obstacles in incorporating theoretical knowledge and clinical skills into practice by nursing interns at SGTH Swat. Individual barriers like poor confidence, fear, and reluctance to carry out procedures were common, with 40.1% of interns indicating that they had high perceived individual barriers. This is in line with what prior research indicates, that nursing students and interns tend to have psychological obstacles, such as fear of errors and self-efficacy, which hinder the application of theoretical knowledge in clinical practice.[24] Clinical practice anxiety was observed to lower skills performance, and the ability to make decisions, and this could be the reason as to why almost half of the participants reported intermediate obstacles that influenced their practice.[25]
In this study, barriers at the institutional level were also very important. Absence of supervision, learning resources, feedback, and special training programs were identified as barriers, and 43.5% of interns saw high institutional barriers. These results aligned with studies conducted in resource-constrained hospital environments, where patient-to-nurse ratios, inadequate equipment, and low levels of mentoring hindered the effectiveness of clinical learning among nursing students. Conversely, researchers in institutions with more resources reported fewer perceived institutional barriers since they had a well-organized orientation, sufficient supervision, and available training modules.[26] This underlines the influence of hospital structure and management assistance on realistic skills assimilation.
The high barriers were reported to be environmental barriers such as overcrowded wards, ineffective documentation, high patient assignment, and lack of practice opportunities, and these factors were conditions reported by 43.5% of interns. The findings are reflective of the research done in other developing countries in the same tertiary care setting, where environmental factors have a major implication on the practical implementation of nursing knowledge.[27] Physical and organizational barriers that may restrict the safe and confident ability to execute procedures are a common problem in such environments for interns. In contrast, there is research evidence in urban or well-equipped hospitals where appropriate clinical space, controllable patient load, and staff supportive behavior improve skill applicability.[28]
The general dominance of the medium barriers of all types shows that the majority of the interns are faced with a set of challenges that cannot be explained by a single aspect. Approximately 45 to 46% of study participants complained about moderate individual, institutional, and environmental barriers. The same result was also observed in a study that was carried out in Pakistan and other low- and middle-income countries where a combination of personal, organizational, and environmental factors collectively influenced clinical competence in nursing interns.[29] The combination of these obstacles highlights the complexity of integrating theory and practice and the necessity of complex interventions.
As far as theory-practice integration is concerned, the research found that interns who had low perceived barriers showed greater knowledge and skills integration. As an example, 56.3% low barriers interns said that there were low integration problems when high barriers had higher integration problems with 62.8% having high integration problems. This is in line with the past literature, which indicates that lower barriers, such as increased confidence and enhanced supervision, are related to improved clinical performance.[30] The correlation between barriers and integration was found to be statistically significant (χ 2 = 29.84, df = 4, p = 0.001), which implies a high level of association between the perceived barriers and the application of practical skills.
Another issue that was noted in the study was that individual factors, specifically confidence and anxiety, were directly related to theory-practice integration. Highly anxious or lowly confident interns were less apt to work out skills on their own and tended to use trial-and-error methods. The same results were observed by Tiwari et al., who stated that the nursing students with low self-efficacy were reluctant towards skill performance, resulting in decreased competence and dependency on supervision.[31] This stresses the necessity of having psychological support, mentorship, and learning by simulation to enhance confidence and skill execution.
The institutional factors, such as the absence of supervision and scarcity of resources, were essential impediments to ensuring that knowledge gets into practice. Lack of mentorship and training materials was reported by interns to decrease their capacity to transfer theory into actual patient care. The findings are in agreement with the studies conducted in South Asia and Africa, which documented that institutional support, including preceptor guidance and practical workshops, is a significant way of enhancing clinical competence.[32] On the other hand, hospitals that had well-organized mentoring programs and skill laboratories had more skill integration among interns.[33] This highlights the importance of the administrative policies and organizational support in clinical education.
Also, the theory-practice integration was very dependent on environmental factors. Patient loads and overcrowding, as well as non-cooperative staff, were reported to restrict the practice opportunities and lower the learning effectiveness. Similar research in low-resource environments indicates that environmental stress factors have a direct effect on the capacity of interns to apply classroom knowledge to clinical skills.[34] On the other hand, in a setting where patients are assigned carefully, there is enough space, and staff members are working together creates effective learning and application of skills.[35] These results imply that a supportive clinical environment has to be developed to help in narrowing the theory-practice gap.
The research found that a large percentage of interns had a high perceived barrier regardless of moderate exposure to clinical practice. According to previous studies, integration can be supported by the length of the internship and preceding clinical learning experiences, but institutional and environmental obstacles can still lead to the cancellation of exposure gains.[36] This means that the number of clinical hours is not enough without the consideration of factors that discourage interns in terms of their learning and confidence.
On the comparison of the findings with the foreign research, it was found that nursing interns in developed nations have fewer obstacles because of superior supervision, resources, and well-organized mentorship initiatives.[37] On the contrary, interns in the developing world, like in the SGTH context, face multi-dimensional obstacles that hinder the process of acquiring and implementing skills.[38] These comparisons show that the systemic and contextual aspects contribute to the formation of the clinical education outcomes and underline the necessity to develop interventions on the local level.
The research also proved that individual, institutional, and environmental barriers should be addressed simultaneously in order to enhance theory-practice integration. The existing literature demonstrates that simulation-based training, clinical mentorship, feedback sessions, and organizational support programs are the types of interventions that increase the level of skills application in nurses among students and interns.[39] The adoption of the approaches of this nature in SGTH may result in better integration of theoretical knowledge into practical care.
Recommendations:
- The nursing administration is supposed to introduce structured mentorship and supervision programs to support the interns through clinical practice.
- To improve real skills acquisition, hospitals are supposed to offer sufficient learning materials, such as skill labs, models, and visual aids.
- Training sessions in the form of simulation should be introduced to enhance confidence and decrease anxiety, as well as bridge the gap between theory and practice.
- Time management in work and the best placement of patients should be done in order to give interns adequate time to practice.
- Supervision, good performance evaluation, and continuous feedback should be given to facilitate learning results.
- Policymakers in nursing education need to develop context-based interventions to overcome individual, institutional, and environmental impediments.
- Future studies are needed to determine the efficacy of educational and organizational interventions in enhancing theory-practice integration.
Conclusion
The paper has found that SGTH Swat nursing interns experience serious challenges in the application of theoretical knowledge and clinical expertise to clinical practice. The report also established individual, institutional, and environmental obstacles such as low confidence, anxiety, and hesitation, lack of supervision, inadequate resources in learning, and insufficient feedback as contributing factors, and high patient load, overcrowding, and lack of practice opportunities, among others, as being significant. The findings showed that these barriers hurt the implementation of classroom learning by the interns in clinical practice, and there was a high statistically significant difference between perceived barriers and theory-practice integration (χ² = 29.84, df = 4, p = 0.001). In general, the results point to the importance of the specific intervention aimed at enhancing the clinical learning environment, support, and resources of nursing interns.
References
- Amini A, Bayat R, Amini K. Barriers to clinical education from the perspective of nursing students in Iran: An integrative review. Archives of Pharmacy Practice. 2020;11(1):73-79.
Barriers to Clinical Education from the Perspective of Nursing Students in Iran: An Integrative Review - Unadkat MB, Mbuba CK, Ngugi AK, Kamya D. Self-reported knowledge, attitudes, practices and barriers in use of evidence-based medicine among resident physicians in Kenya: a mixed methods study. BMC Med Educ. 2021;21(1):537. doi:10.1186/s12909-021-02974-4
PubMed | Crossref | Google Scholar - Chua GP. Challenges Confronting the Practice of Nursing in Singapore. Asia Pac J Oncol Nurs. 2020;7(3):259-265. doi:10.4103/apjon.apjon_13_20
PubMed | Crossref | Google Scholar - Arora S, Rege S, Bhate-Deosthali P, et al. Knowledge, attitudes, and practices of health care providers trained in responding to violence against women: a pre- and post-intervention study. BMC Public Health. 2021;21(1):1973. doi:10.1186/s12889-021-12042-7
PubMed | Crossref | Google Scholar - Rajdev K, Loghmanieh N, Farberov MA, Demissie S, Maniatis T. Are Health-Care Providers Well Prepared in Providing Optimal End-of-Life Care to Critically Ill Patients? A Cross-Sectional Study at a Tertiary Care Hospital in the United States. J Intensive Care Med. 2020;35(10):1080-1094. doi:10.1177/0885066618811794
PubMed | Crossref | Google Scholar - Crowley T, Mokoka E, Geyer N. Ten years of nurse-initiated antiretroviral treatment in South Africa: A narrative review of enablers and barriers. South Afr J HIV Med. 2021;22(1):1196. doi:10.4102/sajhivmed.v22i1.1196
PubMed | Crossref | Google Scholar - Abd Elrahman AM, Eid NM, Safaan SM. Study of nursing interns’ needs through their practical competency self-evaluation. Menoufia Nurs J. 2021;6(1):73-90. doi:10.21608/menj.2021.169892
Crossref | Google Scholar - Liu F, Weng H, Xu R, et al. Nursing Interns’ Attitudes Toward, Preferences for, and Use of Diabetes Virtual Simulation Teaching Applications in China: National Web-Based Survey. JMIR Mhealth Uhealth. 2021;9(9):e29498. doi:10.2196/29498
PubMed | Crossref | Google Scholar - Nyondo-Mipando AL, Woo Kinshella ML, Bohne C, et al. Barriers and enablers of implementing bubble Continuous Positive Airway Pressure (CPAP): Perspectives of health professionals in Malawi. PLoS One. 2020;15(2):e0228915. doi:10.1371/journal.pone.0228915
PubMed | Crossref | Google Scholar - Agom DA, Onyeka TC, Iheanacho PN, Ominyi J. Barriers to the Provision and Utilization of Palliative Care in Africa: A Rapid Scoping Review. Indian J Palliat Care. 2021;27(1):3-17. doi:10.4103/IJPC.IJPC_355_20
PubMed | Crossref | Google Scholar - Hense H, Harst L, Küster D, Walther F, Schmitt J. Implementing longitudinal integrated curricula: Systematic review of barriers and facilitators. Med Educ. 2021;55(5):558-573. doi:10.1111/medu.14401
PubMed | Crossref | Google Scholar - Xu Z, Liang X, Zhu Y, et al. Factors associated with potentially inappropriate prescriptions and barriers to medicines optimisation among older adults in primary care settings: a systematic review. Fam Med Community Health. 2021;9(4):e001325. doi:10.1136/fmch-2021-001325
PubMed | Crossref | Google Scholar - Fryk JJ, Tong S, Marshall C, et al. Knowledge, attitudes and practices of healthcare workers within an Australian tertiary hospital to managing high-consequence infectious diseases. Infect Dis Health. 2021;26(2):95-103. doi:10.1016/j.idh.2020.10.002
PubMed | Crossref | Google Scholar - Gulliver L, Brooks H, Kinniburgh L, Aburn R, Stodart J, Rudland J. Health professional education and practice in preventing and controlling infections in New Zealand: a review to inform strategies for enhancing practitioner competencies and patient safety. Integr Healthc J. 2020;2(1):e000034. doi:10.1136/ihj-2019-000034
PubMed | Crossref | Google Scholar - Abd El-Hay SA, Abed Allah AK. Effect of implementing training module on competence of internship nursing students performance regarding needle stick and sharp injuries safety issues. Tanta Sci Nurs J. 2020;19(1):152-180. doi:10.21608/tsnj.2020.131943
Crossref | Google Scholar - Bosire EN, Mendenhall E, Norris SA, Goudge J. Patient-Centred Care for Patients With Diabetes and HIV at a Public Tertiary Hospital in South Africa: An Ethnographic Study. Int J Health Policy Manag. 2021;10(9):534-545. doi:10.34172/ijhpm.2020.65
PubMed | Crossref | Google Scholar - Moreljwab MH, Mokhtar AMF, Idress EA, et al. Challenges and Difficulties During the Nursing Internship Program Using 5 Domains: A Cross-Sectional Study. Adv Med Educ Pract. 2025;16:341-355. doi:10.2147/AMEP.S466735
PubMed | Crossref | Google Scholar - Ali I, Ahmad K, Ara N, Ahmad S, Noreen S, Ali S. Explore issues and barriers to internship among graduating students in nursing institutes in Khyber Pakhtunkhwa. NurSearcher (J Nurs Midwifery Sci). 2025;5(2):14-23. doi:10.54393/nrs.v5i2.157
Crossref | Google Scholar - Hobenu KA, Adefuye AO, Naab F, Nyoni CN. Clinical education in undergraduate nursing in Ghana: a gap analysis. BMC Nurs. 2025;24(1):562. doi:10.1186/s12912-025-03167-w
PubMed | Crossref | Google Scholar - Hmwe N, Lei C. Nursing internship in pre-registration nursing education programs: A scoping review. Open Nurs J. 2025;19:e18744346372837. doi:10.2174/0118744346372837250307075300
Crossref | Google Scholar - Mramel M, El Alaoui M, El Janati Idrissi R. Barriers to clinical learning skills development among midwifery students and newly qualified midwives in Morocco: A qualitative study. Belitung Nurs J. 2024;10(2):160-168. doi:10.33546/bnj.3163
PubMed | Crossref | Google Scholar - Kumari C, Mahim, Kaushal S, Saini D, Gupta A, Garg HK, Mohan B. Research and evidence-based medical practice: Attitude of MBBS & nursing students and technical staff towards it. Eksplorium. 2025;46(2):1185-1192. doi:10.54393/eksplorium.v46i2.375
Research and evidence-based medical practice: Attitude of MBBS & nursing students and technical sta… - Cai H, Wu Q, Wang P. The influence of workplace experience and professional education on enhancing empathy among doctors, nurses and healthcare students: A comparative cross-sectional study. Int J Nurs Stud. 2026;173:105275. doi:10.1016/j.ijnurstu.2025.105275
PubMed | Crossref | Google Scholar - Alodhialah AM. Exploring the influence of organizational culture on evidence-based practice adoption among nurses in tertiary hospitals: a qualitative study. BMC Nurs. 2025;24(1):1029. doi:10.1186/s12912-025-03647-z
PubMed | Crossref | Google Scholar - Nyalapa MW, Gombachika BT, Gundo R, Chepuka L. Barriers and facilitators in the acquisition of diabetes knowledge among tertiary-care nurses in central and southern Malawi: an exploratory-descriptive qualitative study. BMC Health Serv Res. 2024;24(1):1604. doi:10.1186/s12913-024-12081-x
PubMed | Crossref | Google Scholar - Mohd Nawawi MH, Ibrahim MI. Nurses’ perceptions of patient handoffs and predictors of patient handoff perceptions in tertiary care hospitals in Kelantan, Malaysia: a cross-sectional study. BMJ Open. 2024;14(8):e087612. doi:10.1136/bmjopen-2024-087612
PubMed | Crossref | Google Scholar - Gao X, Gu Z, Huang Y, Li H, Xi X. Investigation on pharmaceutical care barriers perceived by clinical pharmacists in secondary and tertiary hospitals in China. Heliyon. 2024;10(19):e35192. doi:10.1016/j.heliyon.2024.e35192
PubMed | Crossref | Google Scholar - Waterworth CJ, Smith F, Kiefel-Johnson F, Pryor W, Marella M. Integration of rehabilitation services in primary, secondary, and tertiary levels of health care systems in low- and middle-income countries: a scoping review. Disabil Rehabil. 2024;46(25):5965-5976. doi:10.1080/09638288.2024.2317422
PubMed | Crossref | Google Scholar - Pu Y, Xie H, Fu L, et al. Self-efficacy as a mediator in the relationship between clinical learning environment and core nursing competence of intern nursing students: a multicentre cross-sectional study. BMJ Open. 2025;15(5):e094858. doi:10.1136/bmjopen-2024-094858
PubMed | Crossref | Google Scholar - Xu Y, Tang Y, Wang M, et al. Midwives perspectives of barriers and facilitators for the practice of promoting women’s positive childbirth experience in China: A qualitative study. Women Birth. 2025;38(1):101867. doi:10.1016/j.wombi.2025.101867
PubMed | Crossref | Google Scholar - Abou Hashish EA, Alnajjar H. Digital proficiency: assessing knowledge, attitudes, and skills in digital transformation, health literacy, and artificial intelligence among university nursing students. BMC Med Educ. 2024;24(1):508. doi:10.1186/s12909-024-05482-3
PubMed | Crossref | Google Scholar - Abubakari A, Gross J, Asamoah E. Barriers to delivery of culturally competent care among nurses: A multi-center cross-sectional study in a resource-limited setting. Int J Africa Nurs Sci. 2024;20:100705. doi:10.1016/j.ijans.2024.100705
Crossref | Google Scholar - Alsadaan N, Ramadan OME. Barriers and facilitators in implementing evidence-based practice: a parallel cross-sectional mixed methods study among nursing administrators. BMC Nurs. 2025;24(1):403. doi:10.1186/s12912-025-03059-z
PubMed | Crossref | Google Scholar - Wu J, Wang Y, Ye J, Wen H, Song X. Barriers to early career development for Chinese nurses with master’s degrees: A qualitative study. Nurse Educ Pract. 2025;84:104339. doi:10.1016/j.nepr.2025.104339
PubMed | Crossref | Google Scholar - Bahari G, Alharbi F, Alharbi O. Facilitators of and barriers to success in nursing internship programs: A qualitative study of interns’ and faculty members’ perspectives. Nurse Educ Today. 2022;109:105257. doi:10.1016/j.nedt.2021.105257
PubMed | Crossref | Google Scholar - Nigussie Bolado G, Ataro B, Agana A, et al. Internship challenges encountered by nursing students: A qualitative study conducted at the highest institutions in Ethiopia. Nurs Res Pract. 2023;2023:425836. doi:10.2147/NRR.S425836
Crossref | Google Scholar - Tan X, He Y, Zeng Y, Tang J, Huang Y, Sun M. Facilitators and barriers of African postgraduate nursing students’ adaptation to internship: A qualitative study. Nurse Educ Today. 2022;119:105534. doi:10.1016/j.nedt.2022.105534
PubMed | Crossref | Google Scholar - Wang Y, Huang Y, Zheng R, Yue X, Dong F. Intern nursing students’ perceived barriers to providing end-of-life care for dying cancer patients in a death taboo cultural context: A qualitative study. Asia Pac J Oncol Nurs. 2023;10(4):100210. doi:10.1016/j.apjon.2023.100210
PubMed | Crossref | Google Scholar - Wang T, Tan JB, Liu XL, Zhao I. Barriers and enablers to implementing clinical practice guidelines in primary care: an overview of systematic reviews. BMJ Open. 2023;13(1):e062158. doi:10.1136/bmjopen-2022-062158
PubMed | Crossref | Google Scholar
Acknowledgments
The authors would like to express their sincere gratitude to Dr. Shah Hussain, Principal/Associate Professor, Janbar, College of Nursing, Swat, for his invaluable supervision, guidance, and support throughout the course of this study.
Funding
This research did not receive any specific grant from funding agencies in the public, commercial, or not-for-profit sectors.
Author Information
Corresponding Author:
Nasar Mian
Department of Nursing
National College of Nursing, Swat, Pakistan
Email: nasarmian819@gmail.com
Co-Authors:
Sayed Saqib Shah, Syed Azlan Shah, Akhtar Ali, Irshad Muhmmad, Hasnain Nawab, Ikram Shah, Syed Zaid Salim, Rahimullah
Department of Nursing
National College of Nursing, Swat, Pakistan
Shah Hussain
Department of Nursing
Janbar College of Nursing, Swat, Pakistan
Authors Contributions
Nasar Mian, Sayed Saqib Shah, and Syed Azlan Shah contributed to data collection and data analysis. Irshad Muhammad and Hasnain Nawab contributed to data collection and literature review. Ikram Shah, Syed Zaid Salim, and Rahimullah contributed to data collection and data organization. Akhtar Ali and Shah Hussain contributed to the analysis and interpretation.
Ethical Approval
Ethical Approval was obtained from the Saidu Teaching Hospital, Swat, Ref No SGTH/IRB/2026/16
Conflict of Interest Statement
The authors declare that there is no conflict of interest.
Guarantor
Nasar Mian is the guarantor of this study and takes full responsibility for the integrity of the data and the accuracy of the data analysis.
DOI
Cite this Article
Mian N, Shah SS, Shah SA, et al. Barriers to Integrating Nursing Knowledge and Clinical Skills into Clinical Practice Among Nursing Interns at the Government tertiary care hospital, Swat. medtigo J Med. 2026;4(1):e3062422. doi:10.63096/medtigo3062422 Crossref









