Author Affiliations
Abstract
Background: Musculoskeletal injuries are common in emergency departments (EDs), necessitating effective referrals to orthopedic services to optimize patient care and resource management. The appropriateness of these referrals is crucial for ensuring that patients receive necessary interventions while minimizing unnecessary consultations that can burden healthcare resources.
Methodology: A retrospective audit was conducted over three months, from January to March 2023, at Omdurman Teaching Hospital, focusing on the emergency room (ER).
Results: A total of 1,854 patients were referred to orthopedic services, with a mean age of 35.2 years (range 18-85). The nature of injuries included fractures (53.3%), soft tissue injuries (26.7%), dislocations (13.3%), and other injuries (6.7%). Of the referred patients, 66.8% required orthopedic intervention, with 93.7% of fracture referrals appropriate, while only 49.9% of soft tissue injuries warranted intervention, indicating potential over-referral in this category.
Conclusion: The audit underscores the effectiveness of emergency room (ER) referrals to orthopedic services, particularly for fractures and dislocations. However, the unnecessary referral of soft tissue injuries indicates the need for improved training and clearer referral guidelines
Keywords
Emergency room, Orthopedic referrals, Musculoskeletal injuries, Audit, Patient care.
Introduction
Musculoskeletal injuries represent a significant portion of cases seen in EDs, accounting for a substantial number of visits each year. These injuries can range from minor sprains and strains to complex fractures and dislocations, necessitating a wide spectrum of medical interventions.[3] Effective management of these injuries often requires timely and appropriate referrals to orthopedic services, as early intervention can significantly influence patient outcomes and recovery trajectories. However, the decision to refer patients can be complex and is influenced by various factors, including the experience of the ER staff, the availability of orthopedic specialists, and existing referral protocols.
The objective of this audit was to evaluate the referral patterns from the ER to orthopedic services at Dr. Ammar Altayb unit in Omdurman Teaching Hospital. By assessing the number of referrals against the actual need for orthopedic intervention, this audit seeks to identify discrepancies that may exist between the volume of referrals and the appropriateness of those referrals. Understanding these patterns is crucial for enhancing the efficiency of healthcare delivery and ensuring that patients receive the most suitable care in a timely manner.
Background: The increasing incidence of musculoskeletal injuries in emergency settings necessitates a thorough understanding of referral practices.[4] Factors contributing to the rise in these injuries include increased participation in sports, higher rates of road traffic accidents, and an aging population more susceptible to falls and fractures. As such, EDs are often the first point of contact for patients with musculoskeletal complaints, making it essential for ER physicians to have a clear understanding of when to refer patients to orthopedic specialists.
Effective referrals can enhance patient outcomes by ensuring that individuals receive timely and appropriate interventions, which can lead to reduced complications, shorter recovery times, and improved quality of life. Additionally, optimizing referral practices can help reduce waiting times for necessary interventions, thereby improving overall patient satisfaction and resource utilization within the healthcare system. Conversely, inappropriate referrals can lead to increased healthcare costs, unnecessary strain on orthopedic services, and delays in treatment for patients who genuinely require surgical or specialized care.
In many cases, the lack of standardized referral protocols contributes to variability in referral patterns, leading to either over-referral or under-referral of patients. Over-referral can overwhelm orthopedic services, creating backlogs and delaying care for those in need, while under-referral may result in inadequate treatment for patients who require specialized intervention. This audit aims to assess the appropriateness of ER referrals to orthopedic services, identify areas for improvement, and ultimately contribute to the development of clearer referral guidelines that can enhance the quality of care provided to patients at Dr. Ammar Altayb unit.
By examining the existing referral patterns and comparing them to established best practices, this audit will provide valuable insights into the effectiveness of current practices and highlight opportunities for targeted interventions. The findings will not only inform local practices but may also contribute to broader discussions on improving referral systems in emergency medicine, ultimately benefiting patient care and resource management across the healthcare continuum.
Methodology
Study design: A retrospective audit was conducted over three months (January to March 2023) at Omdurman Teaching Hospital, focusing on the ER department.
Setting: The audit was performed at the Dr. Ammar Altayb unit, which serves a diverse population with varying degrees of musculoskeletal injuries.
Inclusion criteria: All patients referred to the orthopedic clinic during the study period.
Exclusion criteria: Patients discharged without referral, those already under orthopedic care, and patients under 18 years of age.
Data collection: Data were collected from hospital records, including:
- Patient demographics (age, gender)
- Nature of injuries (fractures, soft tissue injuries, dislocations, others)
- Final assessments by the orthopedic department regarding the need for intervention
Data analysis: Descriptive statistics were used to analyze the data, comparing the number of referrals with the number of patients requiring orthopedic intervention.
Results
During the study period, a total of 1,854 patients were referred to orthopedic services. The mean age of the patients was 35.2 years, with a demographic distribution comprising 68% male and 32% female. The nature of injuries among the referred patients varied, with fractures being the most common, accounting for 988 cases (53.3%). Soft tissue injuries followed, comprising 495 cases (26.7%), while dislocations represented 247 cases (13.3%). Other injuries accounted for 124 cases (6.7%).
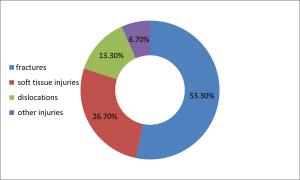
Figure 1: The nature of injuries included fractures, soft tissue injuries, dislocations, and other injuries
Upon orthopedic assessment, it was determined that 1,238 patients (66.8%) required intervention, while 616 patients (33.2%) did not require any orthopedic intervention. The appropriateness of referrals was analyzed, revealing that a significant majority of fracture referrals were justified, with 926 cases (93.7%) requiring intervention. In contrast, only 49.9% of the soft tissue injury referrals warranted orthopedic intervention, indicating a notable discrepancy in this category. For dislocations, 189 cases (76.5%) were deemed appropriate for intervention, while 64 cases (51.6%) of other injuries also required further orthopedic care. These findings highlight both the effectiveness and the areas for improvement in the current referral practices from the ED to orthopedic services.
| ER orthopedics referrals | Frequency | Percent (%) | |
| Appropriateness of referrals | Fractures requiring intervention | 926 | 93.7 |
| Soft tissue injuries requiring intervention | 247 | 49.9 | |
| Dislocations requiring intervention | 189 | 76.5 | |
| Other injuries requiring intervention | 64 | 51.6 | |
| Orthopedic assessment | Patients requiring intervention | 1238 | 66.8 |
| Patients not requiring intervention | 616 | 33.2 | |
Table 1: The distribution of the patients according to their ER orthopedics referrals (n=1854)
Discussion
The findings of this audit indicate that while most referrals for fractures and dislocations were appropriate, a substantial proportion of soft tissue injuries were referred unnecessarily. Specifically, only 49.9% of soft tissue injury referrals warranted orthopedic intervention, suggesting a potential over-referral in this category. This discrepancy highlights the need for enhanced training for ER staff in accurately identifying injuries that may not necessitate orthopedic intervention.
The results aligned with similar audits conducted in various EDs, which have reported comparable trends in referral patterns. For instance, a study found that while fracture referrals were predominantly appropriate, a significant percentage of soft tissue injuries were also referred unnecessarily.[5] Their findings suggested that a lack of standardized referral protocols contributed to this issue, echoing the need for clearer guidelines in our own audit.
Moreover, a study emphasized the importance of education for ER physicians regarding musculoskeletal injuries.[6] They found that targeted training programs significantly improved the accuracy of referrals, leading to a reduction in unnecessary consultations. This suggests that implementing similar educational initiatives at Dr. Ammar Altayb’s unit could enhance the competency of ER staff in managing musculoskeletal injuries, thereby optimizing referral practices.
In addition, a retrospective analysis highlighted that inappropriate referrals not only strain orthopedic services but also delay care for patients who genuinely require intervention.[4] Their research demonstrated that improving the knowledge base of ER personnel regarding injury assessment could lead to more judicious referrals and better allocation of resources. This is particularly relevant in our context, where the high volume of referrals could overwhelm orthopedic services if not managed appropriately.
Furthermore, a systematic review reported that EDs often face challenges in distinguishing between injuries that require orthopedic intervention and those that can be managed conservatively.[3] The review underscored the necessity for ongoing education and the development of referral protocols, which could mitigate the risk of unnecessary referrals.
In summary, our audit’s findings underscore the effectiveness of ER referrals for fractures and dislocations while revealing a critical gap in the management of soft tissue injuries. To address this, we recommend implementing structured training programs for ER physicians, developing clear referral guidelines, and conducting regular audits to monitor referral practices. By learning from similar audits and their recommendations, we can enhance the quality of care provided at Dr. Ammar Altayb’s unit and ensure that patients receive timely and appropriate orthopedic interventions.
Recommendations for future audits: Future audits should assess the impact of implemented changes on referral practices and expand to include patient outcomes post-intervention. This will provide a comprehensive evaluation of the effectiveness of referrals and inform strategies to improve the management of musculoskeletal injuries in emergency settings.[7]
Conclusion
This audit highlights the effectiveness of ER referrals to orthopedic services, particularly for fractures and dislocations. However, the unnecessary referral of soft tissue injuries points to a need for improved training and clearer referral guidelines. Recommendations include ongoing education for ER physicians, the establishment of referral protocols, and regular audits to refine referral practices and enhance patient care.
References
- Morris DM, Gordon JA. The role of the emergency department in the care of homeless and disadvantaged populations. Emerg Med Clin North Am. 2006;24(4):839-848. doi:10.1016/j.emc.2006.06.011
PubMed | Crossref | Google Scholar - Pan T, Kish AJ, Hennrikus WL. Referral patterns to a pediatric orthopedic clinic: pediatric orthopedic surgeons are primary care musculoskeletal medicine physicians. J Pediatr Orthop B. 2022;31(6):613-618. doi:10.1097/BPB.0000000000000979 PubMed | Crossref | Google Scholar
- Browne GJ, Barnett PLj. Common sports-related musculoskeletal injuries presenting to the emergency department. J Paediatr Child Health. 2016;52(2):231-236. doi:10.1111/jpc.13101 PubMed | Crossref | Google Scholar
- Schoenfeld AJ, Belmont PJ Jr, See AA, Bader JO, Bono CM. Patient demographics, insurance status, race, and ethnicity as predictors of morbidity and mortality after spine trauma: a study using the National Trauma Data Bank. Spine J. 2013;13(12):1766-1773. doi:10.1016/j.spinee.2013.03.024 PubMed | Crossref | Google Scholar
- Chartier LB, Masood S, Choi J, et al. A blueprint for building an emergency department quality improvement and patient safety committee. CJEM. 2022;24(2):195-205. doi:10.1007/s43678-021-00252-2
PubMed | Crossref | Google Scholar - Silverman ARC, Broome JN, Jarvis RC 3rd, Plassche GC, Kirschenbaum IH. Using Emergency Department Data to Inform Specialty Strategy: Analyzing the Distribution of 13,777 Consecutive Immediate Orthopaedic Consults in an Urban Community Emergency Department. J Am Acad Orthop Surg Glob Res Rev. 2020;4(2):e20.00005. doi:10.5435/JAAOSGlobal-D-20-00005 PubMed | Crossref | Google Scholar
- Hurwitz S. Evidence-based medicine in orthopaedic surgery–a way to the future. Iowa Orthop J. 2003;23:61-65. Evidence-Based Medicine in Orthopaedic Surgery – A Way to the Future
Acknowledgments
We would like to thank the staff at Dr. Ammar Altayb unit and Omdurman Teaching Hospital for their support in conducting this audit.
Funding
The work had no special funding.
Author Information
Corresponding Author:
Mohammad Khalid
Department of Orthopedics
University of Bahri, College of Medicine, Khartoum, Sudan
Email: mohhak@live.com
Co-Authors:
Sondos Elnair, Hesham Salama, Mahmoud Abdelrahman, Ahmed Elawad, Ahmed Ahmed, Rawan Hassan, Esra Yagoub, Elzahra Elsamani, Razan Khalid, Mohamed Mihaimeed, Wafa Yousif
Department of Orthopedics
Omdurman Teaching Hospital, Sudan
Ammar Awad
Department of Orthopedics
Ahfad University for Women, Omdurman, Sudan
Authors Contributions
All authors have equal contributions to the article in all sections.
Ethical Approval
This clinical audit was conducted in the Orthopaedic Department of Omdurman Teaching Hospital following approval from the Hospital Administration, Emergency department, orthopedic department, and the Local Ethics Committee. The study adhered to ethical principles in accordance with:
- Patient confidentiality – All patient data were anonymized, with no identifiable information disclosed.
- No informed consent required – Since this was a retrospective audit using existing records without patient intervention, individual consent was waived by the ethics committee.
- Data Protection – Data was securely stored and accessed only by authorized audit team members.
The audit was conducted solely for quality improvement purposes, with no commercial interest involved.
Conflict of Interest Statement
The authors declare no conflicts of interest.
DOI
Cite this Article
Khalid M, Elnair S, Salama H, et al. Audit on Patient Referrals by ER Doctors vs. Orthopedic Intervention Needs at Dr. Ammar Altayb Unit, Omdurman Teaching Hospital. medtigo J Med. 2025;3(1):e30623141. doi:10.63096/medtigo30623141 Crossref









