Author Affiliations
Abstract
Background: Awareness of patient care standards is essential for ensuring safe and effective nursing practice. Active participation in clinical nursing rounds helps undergraduate nursing students develop practical skills, strengthen professional competence, and apply theoretical knowledge in real clinical settings. Limited research exists in Pakistan examining the relationship between students’ knowledge of patient care protocols and their level of participation in clinical nursing rounds.
Aim: The study aimed to assess the knowledge of patient care protocols and participation levels in clinical nursing rounds among undergraduate nursing students and to examine the relationship between knowledge and participation.
Methodology: A descriptive cross-sectional study was conducted among 235 third-year undergraduate nursing students at Saidu Teaching Hospital, Swat. Data were collected using a structured self-administered questionnaire covering demographic information, knowledge of patient care protocols, and participation in clinical rounds. Descriptive statistics summarized demographic characteristics, knowledge levels, and participation. The Chi-square test was used to determine the association between knowledge and participation, with statistical significance set at p < 0.05.
Results: Most participants were male (82%) and aged 20–22 years (60%). Students were distributed across medical (29.8%), surgical (25.5%), emergency (25.5%), and specialty wards (19.1%). Knowledge assessment showed that 50.2% had average knowledge, 29.8% good knowledge, and 20% poor knowledge. Participation in clinical rounds was moderate in 45.1%, high in 29.8%, and low in 25.1%. A significant association was found between knowledge and participation (χ² = 45.62, p < 0.001).
Conclusion: Improving knowledge of patient care protocols may enhance student participation in clinical nursing rounds and contribute to better clinical competence.
Keywords
Undergraduate nursing students, Patient care protocols, Clinical participation, Nursing education, Clinical rounds.
Introduction
The key words that are core in this study are undergraduate nursing students, patient care protocols, clinical nursing rounds, nursing knowledge, active participation, and a tertiary care hospital. Patient care protocols are defined as evidence-based, standardized guidelines that aim at providing care that is safe, effective, and consistent in all healthcare institutions. Nursing knowledge constitutes the mental ability, clinical cognizance, and examination of theoretical concepts by nursing students in the process of providing care to a patient. Clinical nursing rounds are designed clinical experiences where nursing students are involved in assessing patients, planning their care, and communicating with disciplines under the guidance of a supervisor.[1] Active participation means active engagement in clinical activity, decision-making, and interaction with the patient during such rounds. Patient safety and professional growth of nursing students are facilitated by the necessity to ensure patient care protocols adherence during clinical rounds.[2]
The quality of healthcare delivery is mostly determined by the level at which the healthcare professionals, such as nursing students during clinical training, follow the laid-down patient care protocols. Globally and regionally, issues have been raised about the gaps in the knowledge of patient care protocol among nursing students and how this information can be applied in clinical practice.[3] According to the reports of developing nations, inappropriate knowledge of standardized care guidelines is one of the factors that lead to poor clinical performance of nursing students. Lack of adequate supervision, clinical exposure, and inconsistency in educational standards further enlarge this disparity. These issues are especially pronounced in tertiary care hospitals with high complexity of patients and workload.[4]
One of the most significant learning experiences among undergraduate nursing students is clinical nursing rounds. In rounds, students are supposed to combine theoretical and practical skills as they offer patient-centered care.[5] Active involvement in rounds improves critical thinking, communication, and clinical competence. Nevertheless, those students who have a low level of understanding of the patient care procedures tend to show passive attendance, lack of confidence, and lack of clinical interaction. This impacts their educational performance and results in the poor quality of patient care provided under supervision.[6]
Among the main points of patient care protocols, it is possible to mention infection control, administration of medications, patient safety, documentation control, and ethical standards. These guidelines can be viewed as the basis of safe nursing practice. Lack of knowledge or adherence to such directions could lead to clinical errors, decision-threatening patient safety, and ineffective professional growth. The undergraduate nursing students should thus be able to have proper protocol knowledge to be able to actively and safely engage in clinical rounds.[7] In tertiary care hospitals, patients are usually present with complicated medical conditions that need a keen observation of the guidelines of care. The nursing students who are on rotation in such settings get to experience high-acuity cases requiring good clinical judgment. Students who have no proper knowledge of protocols might become confused and be reluctant to participate in activities of patient care. This results in watching and not acting, which restricts learning and growth of a profession.[8]
Clinical instructors and nursing educators are crucial to closing the theory-practice gap. Although there are well-organized programs, the clinical teaching strategies have inconsistencies in implementation. Clinical environments of high patient-instructor ratios, insufficient number of instructors, and turnover of patients decrease the chances of supervision on an individual basis. Consequently, students might not be well guided to use patient care protocols when rounding. This is a condition that affects the level of confidence and participation among students in a negative way.[9,10] Patient safety is a worldwide medical issue, and nursing students are being acknowledged as an essential part of the healthcare team. Mistakes connected with the failure to follow the prescribed protocols during clinical training may lead to the occurrence of poor patient outcomes. Participation in the rounds as knowledge based is paramount to mitigate the avoidable risks. Skilled mentoring through active participation enhances responsibility, vigilance, and safety-related practices among nursing students.[11]
Psychological and educational processes also determine the student’s involvement in clinical rounds. Students who possess a deeper theoretical background are more confident, and they also ask appropriate questions and they also engage in clinical activities more independently. Conversely, poor students tend to keep to themselves in fear of committing a mistake. This strengthens passive learning habits and compromises competency building.[12] One of the challenges that has been associated with undergraduate nursing education in developing healthcare systems is the lack of resources, simulation facilities, and unequal clinical exposure. There is a continual tendency to focus on emergency and acute care competencies and pay less attention to the overall reinforcement of patient care guidelines. This gap causes ongoing knowledge gaps among nursing students.[13,14]
Saidu Teaching Hospital is a clinical setting with a significant population of patients who are mainly based in various districts, hence a heavy patient workload and complexity of care provided. These limits are supposed to be within the bounds of nursing students. The proper understanding of patient care procedures will help the students to quickly adjust to the environment of high-paced work and participate in the clinical rounds. Absence of knowledge can, however, undermine learning and patient safety.[15] Research literature shows that the extent of knowledge among nursing students can play a significant role in determining their clinical outcomes and involvement. Students who achieve academically better and have more structured clinical guidance demonstrated favorable results regarding participation in nursing rounds. On the other hand, a lack of knowledge restrains practical engagement and the empowerment of decision-making. Local research is needed to detect gaps in institutional settings.[16]
There are also cultural and institutional influences that influence the involvement of students during rounds. Students who lack confidence may not be encouraged to question and take independent action in hierarchical clinical settings. Knowledge can empower students to manage these barriers through promoting evidence-based conversations and advocacy for the patient. Optimization of protocol knowledge leads to professional communication and patient-centered care.[17] Research based on assessment offers necessary baseline information on curriculum assessment and clinical teaching refinements. Insight into the relationship between the knowledge and engagement of the students would enable the teachers to develop specific interventions. This type of data assures the creation of competency-based education and clinical training programs.[18]
Saidu Teaching Hospital, Swat, has a large tertiary care facility and an important clinical training facility for undergraduate nursing students. The challenging clinical setting demands that the students have sufficient knowledge and actively participate in the care of the patient. Assessing the correlation between patient care protocols knowledge and involvement in clinical nursing rounds is important in determining the gaps in education. The results of this research will inform nursing educators, administrators, and policymakers to enhance their efforts in clinical training, patient safety, and outcomes of nursing education.[19]
Methodology
The research design used in this study was a descriptive cross-sectional research design aimed at investigating the relationship between the knowledge of patient care protocols among undergraduate nursing students and their involvement in clinical nursing rounds. The study took place at Swat Saidu Teaching Hospital, which is a tertiary care institution offering full medical and surgical services and a significant clinical training facility to nursing students. The sample population consisted of third-year students in the undergraduate nursing (BS Nursing) degree program who had clinical rotations at the time when the sample was collected. Students who were actively involved in patient care activities could participate. The individuals who missed during the clinical postings, declined to participate, or were not studying in the fourth year were not included in the study. There were 235 students who were involved. The population of 600 students was estimated, and the Raosoft sample size calculator was used with a 95% confidence interval, 5% margin of error, and a population of 600 students. Participants were recruited based on a convenience sampling method, and they had to satisfy the inclusion criteria and be available during the time of data collection.
Data collection procedure: The permission to collect data was granted by the Nursing Superintendent of Saidu Teaching Hospital before collecting data. The required Ethical Review Committee gave ethical approval. The structured questionnaire was used in the collection of data to help in the determination of the knowledge of the students on patient care protocols, as well as the use of a participation scale to determine the level of involvement of the students in the clinical nursing rounds. The questionnaire was properly applied by the researcher and the trained research assistants, face-to-face, to promote clarity and consistency. The subjects received information on the aim of the research, confidence, anonymity, and voluntary consent to participate. Each participant signed an informed consent form that was written. The students were given ample time to fill out the questionnaire, and help was given in case of difficulty, especially in answering questions. Questionnaires were completed, and the reviews were carried out immediately to ensure that the questionnaires were complete and accurate.
Data analysis procedure: The data collected were coded and keyed into statistical package of the Social Sciences (SPSS) version 26 to be analyzed. Demographic characteristics, knowledge scores, and levels of participation were summarized using descriptive statistics and the frequencies, percentages, means, and standard deviations. To establish a relationship between the knowledge of patient care protocols and involvement in clinical nursing rounds, inferential analysis was conducted with the help of the chi-square test. The statistical significance was set at less than 0.05p-value.
Results
Demographic characteristics of participants: The demographic composition of 235 undergraduate students of nursing who participated in the study. Most of the participants were male (82 %), and female students were also 18 % of the sample. The largest percentage of students (60 %) belonged to the age group of 20-22 years, then there was 34.9 % of students belonging to the age group of 23-25 years, and 5.1 % of students who were above 25 years. The distribution of clinical rotations was relatively equal, as 29.8% of them were in medical wards, 25.5% in surgical wards, 25.5% in emergency units, and 19.1% in specialty wards. This distribution is used to represent the representation of students in various wards and ages. Knowledge of demographics is necessary to place the knowledge and participation results in perspective. These features give grounds to examine possible correlations of student profiles and clinical engagement.
| Variable | Category | Frequency (n) | Percentage (%) |
| Gender | Male | 193 | 82 |
| Female | 42 | 18 | |
| Age (years) | 20–22 | 141 | 60 |
| 23–25 | 82 | 34.9 | |
| >25 | 12 | 5.1 | |
| Clinical rotation area | Medical Ward | 70 | 29.8 |
| Surgical Ward | 60 | 25.5 | |
| Emergency Unit | 60 | 25.5 | |
| Specialty Wards | 45 | 19.1 |
Table 1: Demographic characteristics of participants
The level of knowledge of patient care protocols among undergraduate nursing students is found in Figure 1. Most of the students (50.2%) had average knowledge, with only 29.8 of them scoring good knowledge. A lesser percentage (20) of the participants was classified as possessing poor knowledge. This implies that most of the students are moderately familiar with patient care protocols, yet few of them are particularly good at this matter. Knowledge assessment is important because it can affect clinical performance and involvement. These findings point to improvement in areas of educational and clinical training programs. The table gives a good idea of the level of knowledge distribution among the study population.
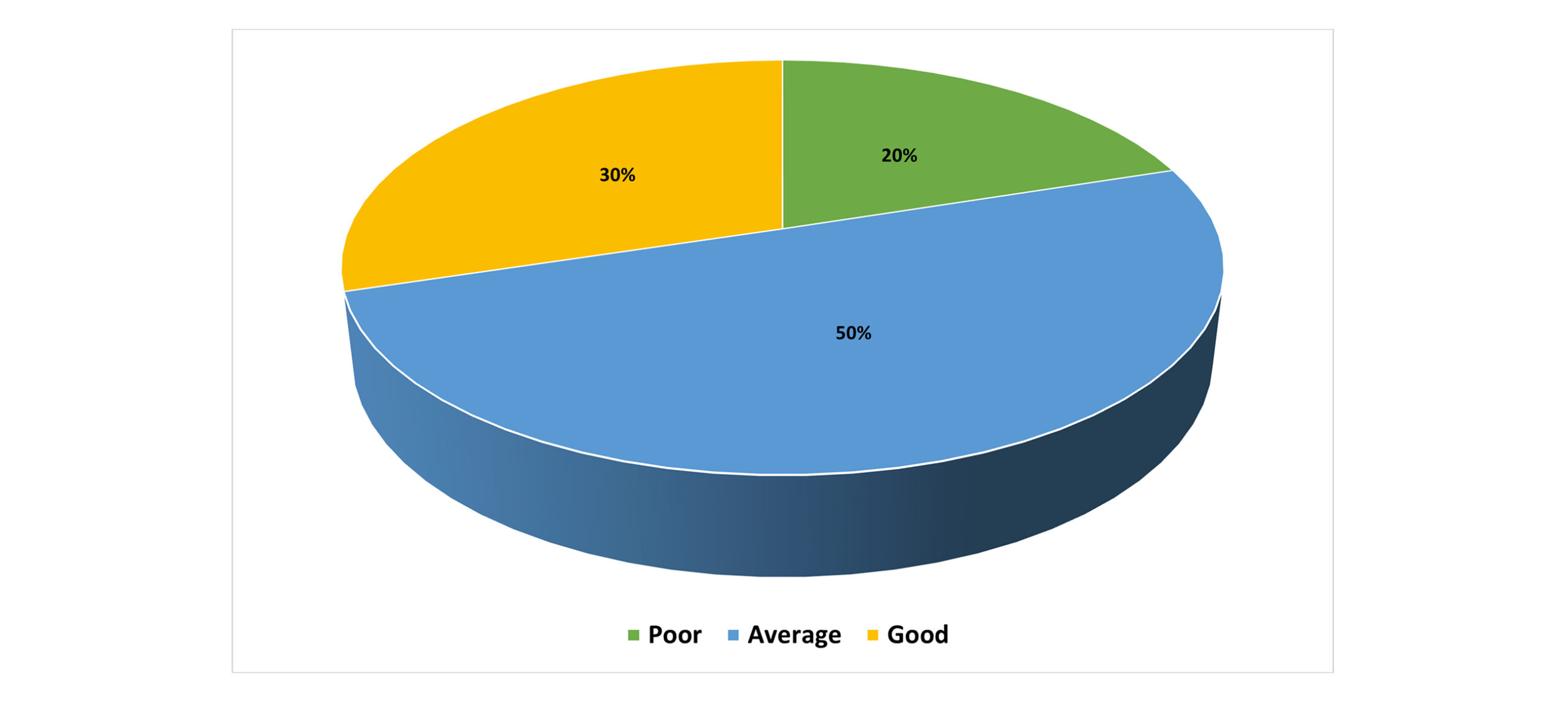
Figure 1: Knowledge of patient care protocols (n = 235)
Table 2 represents the rate of student participation in clinical nursing rounds. The highest percentage of students (45.1) expressed moderate participation, after which 29.8% expressed high-level participation. A lower percentage (25.1) showed low attendance in the clinical rounds. These results suggest that, although the majority of students practice clinically on the moderate level, there are quite a number of less active students who can influence the outcomes of learning. Involvement is crucial in the development of skills, professional competency, and awareness of the patient care protocols. The findings are an insight into how clinically engaged the students are during rotations. They are also used to form an evaluation of the association with levels of knowledge.
| Participation level | Frequency (n) | Percentage (%) |
| Low | 59 | 25.1 |
| Moderate | 106 | 45.1 |
| High | 70 | 29.8 |
Table 2: Participation in clinical nursing rounds (n = 235)
Table 3 indicates the correlation between the knowledge that the students have of patient care protocols and their attendance during clinical nursing rounds. The chi-square test showed that the relationship was statistically significant (2 = 45.62, p < 0.001). Good knowledge was more likely to engage in participation than poor knowledge, as 32 out of the 70 students were high in participation. The average knowledge students were the ones who participated moderately, with poor knowledge students being the largest contributors to the low participation category. These findings suggest that knowledge has a great impact on involvement in clinical practice. The results highlight the need to increase knowledge and turn participation and clinical competencies into a priority. The table gives us grounds to believe that there is a positive correlation between knowledge and clinical engagement as hypothesized in the study.
| Knowledge level | Low participation | Moderate participation | High participation | Total (n) |
| Poor | 35 | 12 | 0 | 47 |
| Average | 20 | 60 | 38 | 118 |
| Good | 4 | 34 | 32 | 70 |
| Total (n) | 59 | 106 | 70 | 235 |
Chi-square test: χ² = 45.62, p < 0.001
Table 3: Association between knowledge and participation in clinical nursing rounds
Discussion
The current research was conducted on the association between patient care protocol knowledge and attendance of clinical nursing rounds in undergraduate nursing students. The demographic profile showed that most of the respondents were male and were between 20 and 22 years old. This preponderance of young pupils would be consistent with other reports that have stated that early adult nursing pupils would constitute the highest proportion in clinical training plans by enrolling in nursing schools in Pakistan and other third-world nations.[20] The gender balance, however, is the opposite of international data, in which female students tend to be a larger proportion, which is caused by sociocultural disparity in nursing education and workforce setup.[21] Knowledge assessment showed that the majority of students had average knowledge of patient care protocols, and a lower proportion of students had good scores of knowledge assessment. This is in line with the findings of other literature carried out in the same tertiary care environment, whereby moderate levels of knowledge were prevalent among undergraduates in the nursing field, which points to the lack of theoretical training or the insufficient transfer of classroom knowledge into clinical practice. This study showed a lower ratio of poor knowledge among students compared to some of the past research, indicating that there are recent changes in the curriculum and organized clinical experience, which might improve baseline knowledge.[22]
All students engaged in clinical nursing rounds differently, with the majority showing moderate participation. This observation is also supported by the past literature, where undergraduate students tend to exhibit partial involvement in clinical activities, without confidence in their experience, fear of error, or strong guidance.[23,24] This tendency is also confirmed by the literature conducted in more resource-rich environments, where high active participation was observed, which can be explained by improved student-to-preceptor ratio and programmed mentorship.
The chi-square test showed that there was a statistically significant connection between knowledge and attendance of clinical rounds, suggesting that students whose knowledge was higher were more inclined towards being active. The above finding also affirms the theory that knowledge enables students to engage in the care of patients with confidence, which was also established by Al-Kandari et al.[10] who concluded that well-informed students were more active in clinical decision-making. Other researchers, however, observed less significant associations, which they attribute to low participation in the study due to external influences, including workload, ward environment, and preceptor attitudes, indicating that knowledge is not necessarily a complete predictor of engagement.[25,26]
Clinical rotation area comparison showed that the performance of the students in medical wards was slightly higher than in comparison to specialty wards. This is in line with research findings, which state that students in general care type settings usually get more chances to view routine practices and actively contribute to patient care, but specialty wards can have highly complicated interventions that do not provide chances to the students to practically participate. On the other hand, a few studies have revealed that partaking of specialized jurisdictions may augment involvement of highly motivated students, with emphasis on the role played by personal initiative and preceptor encouragement.[27]
The findings of this paper stress the relevance of combining knowledge acquisition with clinical practice. Past studies point to the fact that structured teaching methods, including case-based learning, simulation games, and guided bedside education, are effective in boosting retention of knowledge and clinical engagement.[28] This supports the importance of curricula that are theory-practice based so that students are not simply able to learn the knowledge but can easily apply it in patient care.
The average knowledge and engagement rates are indicative of the fact that students are rather competent but can be improved. South Asian based studies on nursing programs also showed similar results regarding students’ skills to translate theoretical knowledge into practical skills that were related to insufficient supervision, high patient-to-student ratio, and time spent on clinical rotation. These gaps should be closed through an ongoing faculty development program and through the introduction of mentorship programs to assist the students throughout clinical rounds.
The results also highlight the two-way contact between participation and knowledge. Kaddoura et al.[29] Note that those students who are actively involved in clinical rounds are more likely to consolidate their knowledge based on observations, practice, and feedback to form a positive learning cycle. On the other hand, low-knowledge students can evade active participation, and hence, learning and acquisition of clinical confidence can be restricted. This interdependence underscores the importance of concomitant approaches that have the effect of augmenting knowledge and clinical involvement.[30]
The percentage of students who attain high knowledge and participation in this study is moderate in comparison to international studies. In those nations that have developed nursing education systems, greater proportions of students show high levels of knowledge and involvement, which is attributed to the organization of clinical supervision, a smaller number of students on one ward, and a regular evaluation of clinical competence.[31] These comparisons imply that knowledge and participation depend heavily on educational and institutional conditions, such as support of the faculty, ward environment, and availability of learning resources.
On balance, the results of the study stress that active involvement in the clinical nursing rounds can be encouraged only by increasing the awareness of patient care protocols. Specific educational activities, organized mentoring, and clinical exposure can enhance the confidence and interest of students. The findings have an implication to nursing teachers and hospital managers who need to design conducive learning environments that promote cognitive and practical competence, which eventually lead to better patient care outcomes.
Recommendations: Nursing teachers are advised to use specific strategies to enhance the knowledge of patient care procedures among students with the help of systematic teaching, simulations, and case studies.
- Clinical mentorship systems are to be strengthened in order to mentor students throughout the rotations and promote proactive activities and the acquisition of practical skills.
- To ensure that there is sufficient supervision and learning experience in all the clinical units, such as specialty wards, hospitals, and training institutions, the staff should maintain adequate student-preceptor ratios.
- Knowledge and clinical engagement evaluation should be performed periodically to determine students who require further assistance and evaluate the efficiency of educational practices.
- The nursing curriculum must combine theoretical learning with practical clinical learning and focus on the relationship between theoretical learning and practical involvement.
- Training and updating patient care protocols should be conducted through workshops and refreshing to promote competency and confidence among the undergraduate nursing students.
- The best investigation ought to be conducted in order to investigate other variables of clinical participation, like motivation, ward environment, preceptor support, among others, in order to come up with a multifaceted approach to enhancing participation among students.
- Nursing education policymakers ought to leverage evidence-based practices with a view to enriching the knowledge of patients, as well as practical competence, thus guaranteeing the provision of quality care to their patients.
Conclusion
The research outcomes were that out of the 235-3rd year undergraduate nursing students, most of them were male and between 20 and 22 years of age, with students being spread out in the medical, surgical, emergency, and specialty wards. The majority of the participants possessed average knowledge on how to care for the patient, with a smaller proportion possessing good knowledge, and a minority had poor knowledge. The number of students involved in clinical nursing rounds was mostly medium in association, and a small number of students had high and low involvement. The correlation between knowledge and participation was statistically significant, whereby students who had better knowledge had higher chances of participating actively in clinical practice. These results emphasize the importance of knowledge in promoting clinical involvement and competency. Improving the areas of education, clinical supervision, and on-the-job exposure would reinforce knowledge, as well as proactive exposure, which will eventually lead to better nursing practice and quality care of patients during clinical rotations.
References
- Levett-Jones T, Andersen P, Bogossian F, et al. A cross-sectional survey of nursing students’ patient safety knowledge. Nurse Educ Today. 2020;88:104372. doi:10.1016/j.nedt.2020.104372
PubMed | Crossref | Google Scholar - Vaismoradi M, Tella S, A Logan P, Khakurel J, Vizcaya-Moreno F. Nurses’ Adherence to Patient Safety Principles: A Systematic Review. Int J Environ Res Public Health. 2020;17(6):2028. doi:10.3390/ijerph17062028
PubMed | Crossref | Google Scholar - McCloughen A, Levy D, Johnson A, Nguyen H, McKenzie H. Nursing students’ socialisation to emotion management during early clinical placement experiences: A qualitative study. J Clin Nurs. 2020;29(13-14):2508-2520. doi:10.1111/jocn.15270
PubMed | Crossref | Google Scholar - Slemon A, Jenkins E, Bungay V, Brown H. Undergraduate students’ perspectives on pursuing a career in mental health nursing following practicum experience. J Clin Nurs. 2020;29(1-2):163-171. doi:10.1111/jocn.15074
PubMed | Crossref | Google Scholar - Karttunen M, Sneck S, Jokelainen J, Elo S. Nurses’ self-assessments of adherence to guidelines on safe medication preparation and administration in long-term elderly care. Scand J Caring Sci. 2020;34(1):108-117. doi:10.1111/scs.12712
PubMed | Crossref | Google Scholar - Motsaanaka MN, Makhene A, Ally H. Student nurses’ experiences regarding their clinical learning opportunities in a public academic hospital in Gauteng province, South Africa. Health SA. 2020;25:1217. doi:10.4102/hsag.v25i0.1217
PubMed | Crossref | Google Scholar - Dobrowolska B, Chiappinotto S, Cabrera E, et al. Correction: Changes and continuities in undergraduate nursing education during and after COVID-19: a European comparative study from the perspective of health science. BMC Med Educ. 2025;25(1):1165. doi:10.1186/s12909-025-07731-5
PubMed | Crossref | Google Scholar - Chávez-Valenzuela P, Kappes M, Sambuceti CE, Díaz-Guio DA. “Challenges in the implementation of inter-professional education programs with clinical simulation for health care students: A scoping review”. Nurse Educ Today. 2025;146:106548. doi:10.1016/j.nedt.2024.106548
PubMed | Crossref | Google Scholar - Chaudhary S, Singh AL. Impact of self-directed learning strategy, an innovative method in nursing undergraduates: Study protocol for a randomized controlled trial. PLoS One. 2025;20(7):e0325300. doi:10.1371/journal.pone.0325300
PubMed | Crossref | Google Scholar - Wang L, He LH, Wan JH. Implementation of a guideline-based clinical practice teaching model to enhance learning and thinking abilities in undergraduate nursing students. BMC Nurs. 2025;24(1):572. doi:10.1186/s12912-025-03183-w
PubMed | Crossref | Google Scholar - Longhini J, Kabir ZN, Waldréus N, et al. Development of an instrument to measure the attitudes and skills of undergraduate nursing students in caring for family caregivers: An international multi-method study. Nurse Educ Today. 2025;151:106738. doi:10.1016/j.nedt.2025.106738
PubMed | Crossref | Google Scholar - Becking-Verhaar F, Pelzer F, Van Noort H, et al. Evaluating Nurses’ Perspectives on the Acceptability and Practicality of Comfort Rounding for Personalised Nutritional and Mobility Care in Surgical Wards: A Mixed-Methods Feasibility Study. J Adv Nurs. 2025. doi:10.1111/jan.70462
PubMed | Crossref | Google Scholar - Byerly LK, Floren LC, Yukawa M. Fostering Interprofessional Geriatric Patient Care Skills for Health Professions Students Through a Nursing Facility-Based Immersion Rotation. MedEdPORTAL. 2020;16:11059. doi:10.15766/mep_2374-8265.11059
PubMed | Crossref | Google Scholar - Ullah M, Ullah R, Hussain F, et al. Perceptions and Satisfaction of Nursing Students During Clinical Training: A Study from Swat, Pakistan. J Health Wellness Community Res. 2025;3(13):e1065. doi:10.61919/ejz2bt74
Crossref | Google Scholar - Ahlstrom L, Holmberg C. A comparison of three interactive examination designs in active learning classrooms for nursing students. BMC Nurs. 2021;20(1):59. doi:10.1186/s12912-021-00575-6
PubMed | Crossref | Google Scholar - Koldestam M, Broström A, Petersson C, Knutsson S. Model for Improvements in Learning Outcomes (MILO): Development of a conceptual model grounded in caritative caring aimed to facilitate undergraduate nursing students’ learning during clinical practice (Part 1). Nurse Educ Pract. 2021;55:103144. doi:10.1016/j.nepr.2021.103144
PubMed | Crossref | Google Scholar - Cantero-López N, González-Chordá VM, Valero-Chillerón MJ, et al. Attitudes of Undergraduate Nursing Students towards Patient Safety: A Quasi-Experimental Study. Int J Environ Res Public Health. 2021;18(4):1429. doi:10.3390/ijerph18041429
PubMed | Crossref | Google Scholar - Becking-Verhaar F, Pelzer F, Van Noort H, et al. Evaluating Nurses’ Perspectives on the Acceptability and Practicality of Comfort Rounding for Personalised Nutritional and Mobility Care in Surgical Wards: A Mixed-Methods Feasibility Study. J Adv Nurs. 2025. doi:10.1111/jan.70462
PubMed | Crossref | Google Scholar - Xu J, Chen X, Zeng Y, Tang J, Long Y, Li L. Mapping patient safety competency in undergraduate nursing interns: Insights from a latent profile analysis. Nurse Educ Today. 2025;153:106813. doi:10.1016/j.nedt.2025.106813
PubMed | Crossref | Google Scholar - de Goumoëns V, Lefrançois LE, Forestier A, et al. Bachelor nursing competencies to care for children in hospital and home settings: A Delphi study. Nurse Educ Today. 2025;145:106487. doi:10.1016/j.nedt.2024.106487
PubMed | Crossref | Google Scholar - Ryan ELJ, Jackson D, Woods C, Usher KJ. Pre-registration nursing students’ perceptions and experience of intentional rounding: A cross-sectional study. Nurse Educ Pract. 2020;42:102691. doi:10.1016/j.nepr.2019.102691
PubMed | Crossref | Google Scholar - Cieślak I, Jaworski M, Panczyk M, et al. Exploring the association between combined formal and informal educational approaches and cultural intelligence among undergraduate nursing students: A cross-sectional study. Nurse Educ Today. 2025;146:106537. doi:10.1016/j.nedt.2024.106537
PubMed | Crossref | Google Scholar - Beigzadeh A, Yamani N, Bahaadinbeigy K, Adibi P. Challenges and strategies of clinical rounds from the perspective of medical students: A qualitative research. J Educ Health Promot. 2021;10:6. doi:10.4103/jehp.jehp_104_20
PubMed | Crossref | Google Scholar - Marcellus L, Jantzen D, Humble R, Sawchuck D, Gordon C. Characteristics and processes of the dedicated education unit practice education model for undergraduate nursing students: a scoping review. JBI Evid Synth. 2021;19(11):2993-3039. doi:10.11124/JBIES-20-00462
PubMed | Crossref | Google Scholar - Singh K, Alomari AMA, Sayed HMA, et al. Barriers and Solutions to the Gap Between Theory and Practice in Nursing Services: A Systematic Review of Qualitative Evidence. Nurs Forum. 2024;2024:7522900. doi:10.1155/2024/7522900
Crossref | Google Scholar - Salberg J, Ramklint M, Öster C. Nursing and medical students’ experiences of interprofessional education during clinical training in psychiatry. J Interprof Care. 2022;36(4):582-588. doi:10.1080/13561820.2021.1928028
PubMed | Crossref | Google Scholar - Bowles W, Buck J, Brinkman B, Hixon B, Guo J, Zehala A. Academic-clinical nursing partnership use an evidence-based practice model. J Clin Nurs. 2022;31(3-4):335-346. doi:10.1111/jocn.15710
PubMed | Crossref | Google Scholar - Marcellus L, Jantzen D, Humble R, Sawchuck D, Gordon C. Characteristics and processes of the dedicated education unit practice education model for undergraduate nursing students: a scoping review. JBI Evid Synth. 2021;19(11):2993-3039. doi:10.11124/JBIES-20-00462
PubMed | Crossref | Google Scholar - Rutledge CM, Gustin T. Preparing nurses for roles in telehealth: now is the time! OJIN: The Online Journal of Issues in Nursing. 2021;26(1):Manuscript 3. doi:10.3912/OJIN.Vol26No01Man03
Crossref | Google Scholar - Liu N, Zheng Z, Liao J, Li J, Yang Z, Lai X. The Effectiveness of Student-Led Ward Round Training on Knowledge Acquisition, Critical Thinking Ability, and Self-Confidence of Acute Upper Gastrointestinal Bleeding for Nursing Students. Adv Med Educ Pract. 2023;14:21-30. doi:10.2147/AMEP.S381760
PubMed | Crossref | Google Scholar - Roustaei Z, Sadeghi N, Azizi A, Eghbalian M, Karsidani SD. The effect of regular nursing rounds on patients’ comfort and satisfaction, and violence against nurses in surgical ward. Heliyon. 2023;9(7):e17708. doi:10.1016/j.heliyon.2023.e17708
PubMed | Crossref | Google Scholar
Acknowledgments
The authors would like to express their sincere gratitude to Dr. Shah Hussain, Principal/Associate Professor, Janbar College of Nursing, Swat, for his invaluable supervision, guidance, and support throughout the course of this study.
Funding
This research did not receive any specific grant from funding agencies in the public, commercial, or not-for-profit sectors.
Author Information
Corresponding Author:
Junaid Khan
Department of Nursing
Malakand College of Nursing, Swat, Pakistan
Email: drjunaidkhan03@gmail.com
Co-Authors:
Abdur Rahman, Awais Akhtar, Muhammad Suliman Khan, Barkat Ali Khan, Jawad Ahmad, Shah Fahad, Muhammad Zakir, Safyan Ali, Usman Khan
Department of Nursing
Malakand College of Nursing, Swat, Pakistan
Mumtaz Ali Khan
Department of Nursing
Malakand College of Nursing, Swat, Pakistan
Shah Hussain
Department of Nursing
Janbar College of Nursing, Swat, Pakistan
Authors Contributions
Junaid Khan, Abdul Rahman, Awais Akhtar, and Muhammad Suliman Khan contributed to data collection and data analysis. Muhammad Zakir, Barkat Ali Khan, and Jawad Ahmad were responsible for data collection and literature review. And USMAN KHAN, Shah Fahad, Safyan Ali, contributed to data collection and data organization. Dr. Shah Hussain and Mumtaz Ali Khan were responsible for the interpretations.
Ethical Approval
Ethical approval was obtained from the Saidu Teaching Hospital, Swat (Ref No: SGTH/IRB/2026/25).
Conflict of Interest Statement
The authors declare that there is no conflict of interest.
Guarantor
Junaid Khan is the guarantor of this study and takes full responsibility for the integrity of the data and the accuracy of the data analysis.
DOI
Cite this Article
Rahman A, Khan J, Akhtar A, et al. Association Between Undergraduate Nursing Students’ Knowledge of Patient Care Protocols and their Active Participation in Clinical Nursing Rounds at Saidu Teaching Hospital, Swat. medtigo J Med. 2026;4(1):e3062424. doi:10.63096/medtigo3062424 Crossref









