Author Affiliations
Abstract
The progressive corneal disorder known as keratoconus results in the cornea becoming weaker and appearing conical. Because of this, the cornea’s structural integrity is compromised, which puts afflicted people at risk for acute corneal hydrops. It is characterized by pain and sudden loss of vision due to a rupture in Descemet’s membrane (the cornea’s deepest layer). It typically strikes in the second decade of life and impacts people of all racial and gender identities. 54 per 100,000 is the estimated prevalence in the general population. This paper describes a case of this uncommon cause of sudden visual loss and an illustration of Munson’s sign, an advanced keratoconus-related V-shaped protrusion of the lower eyelid upon downward gaze. The goal is to draw attention to Munson’s sign, which can be used to diagnose keratoconus quickly and easily in a patient.
Keywords
Keratoconus, Munson’s sign, Cornea, Acute corneal hydrops, Vision, Contact lens
Introduction
Keratoconus, which refers to a protrusion of the cornea resembling a cone, is a term derived from the Greek words keras (horn) and konos (cone). A condition called keratoconus causes the cornea to gradually curve, changing from a symmetrical dome to an asymmetric cone shape. This leads to a shift in eyeglasses and decreased visual acuity [1]. The middle of the 19th century saw the discovery of this disorder. Keratoconus is a non-inflammatory condition that causes the cornea to thicken; it typically affects both sides in 96% of cases but can also develop asymmetrically. Although bilateral keratoconus occurs in most cases, its severity and progression are asymmetric [1,2]. An obvious feature of Munson’s sign is a downward-pointing V-shaped indentation of the lower eyelid. Indicators of severe keratoconus include a positive Munson’s sign. Relating to genetic and environmental factors, keratoconus is a common ectatic disorder affecting the cornea. The characteristic feature of this eye condition is a localized, non-inflammatory thinning of the central corneal stroma, which frequently results in bilateral, asymmetric corneal distortion and anterior protrusion. The symptoms of keratoconus usually appear in the second decade of life or during adolescence. They usually worsen over the course of the following two decades before stabilizing. Corneal scarring and edema may worsen vision loss in extreme situations. Clinical manifestations of keratoconus vary with its severity [3,4]. Eye care professionals can now diagnose corneal ectasia far earlier than they could in the past, thanks to advancements in corneal topography and the development of corneal tomography [5]. The advancements in contact lens technology and keratoconus surgery have improved clinical management [6].
This medical case report aimed to report the clinical manifestations, imaging study, and management of Munson’s sign in a Keratoconus patient.
Case Presentation
A 32-year-old female visited the physician’s office with a complaint of the sudden onset of vision loss associated with epiphora (watery eye) and pain in the left eye. She also reported experiencing frequent itching and watering of the left eye for the past six months. The patient has no significant past medical history; however, her family history revealed that her father had keratoconus. She has a history of smoking half a pack of cigarettes daily and reports no alcohol consumption or illicit drug use.
On examination, her vital signs, including temperature, blood pressure, blood glucose, body mass index (BMI), and pulse rate, were within normal limits. Ophthalmologic examination (Figure 1) revealed a V-shaped protrusion of the left lower eyelid, corneal opacification, and decreased visual acuity. The patient was further diagnosed with acute corneal hydrops (ACH).
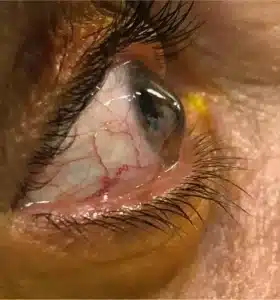
Figure 1: Munson’s sign in a Keratoconus patient
Case Management
She was prescribed cyclopentolate drops, erythromycin ointment, sodium chloride 5% drops, brimonidine drops, and an eye shield without patching. She was also instructed to avoid rubbing her eyes. She was scheduled for a follow-up appointment with an ophthalmologist in one week. After one visit, an ophthalmic examination was carried out using optical coherence tomography (OCT) imaging. After diagnosis, the patient’s vision was corrected using rigid gas permeable (RGP) contact lenses that rest on the sclera, or white portion of the eye, as opposed to the cornea, known as scleral lenses. They have a larger diameter. After treatment, the patient was advised to follow up in 6 months. These lenses have the potential to provide nearly excellent corrected vision.
Discussion
The prevalence and incidence rates of keratoconus have been estimated to be between 0.2 and 4,790 per 100,000 persons and 1.5 and 25 per 100,000 persons/year, respectively, with the highest prevalence and incidence rates typically occurring in 20- to 30-year-olds. Epidemiological studies show substantial global variation in these rates [7]. In moderate to advanced cases, a frequently observed sign is the presence of Fleischer’s ring encircling the base of the corneal cone, resulting from the accumulation of iron deposits. Another distinctive feature is Vogt’s striae, which are fine vertical lines caused by compression of Descemet’s membrane. As the condition advances, many patients develop Munson’s sign, characterized by a protrusion of the lower eyelid upon downward gaze due to corneal bulging. Severe keratoconus may lead to corneal hydrops, marked by acute stromal edema and stromal scarring due to breaks in Descemet’s membrane [8].
Consanguinity and a positive family history of keratoconus are believed to contribute to its incidence. Consequently, this case can be reclassified as a familial instance of keratoconus. In familial cases of keratoconus, it is increasingly evident that the condition follows a Mendelian inheritance pattern, where specific genetic mutations play a causative role. Furthermore, environmental factors have emerged as potential contributors to keratoconus, including contact lens usage, habitual eye rubbing, magnesium deficiency, and ocular atopy. A growing body of evidence notably supports a potential link between atopic conditions and keratoconus [9,10].
From a pathological perspective, individuals with keratoconus who also exhibit signs of atopy demonstrate corneal topographic and pachymetric characteristics distinct from those without atopy. The itching associated with atopic conditions might lead to increased eye rubbing, potentially contributing to the development of keratoconus. Due to the highly asymmetric nature of corneal shape distortion and stromal thinning in keratoconus, vision correction with spectacles and conventional spherical or toric soft contact lenses is suboptimal, primarily effective only in the early stages of keratoconus [11,6].
Genetic and environmental factors play a role in the pathogenesis of kidney cancer. The understanding of its epidemiology and etiology has advanced significantly. Our understanding of the pathophysiology of keratoconus has been advanced. It will continue to be enhanced by recently developed genetic technologies such as whole-exome or genome sequencing and genome-wide association technologies. Eventually, this information will help develop targeted therapies, better early diagnostics, and possibly even a better prognosis [12,13].
Custom-designed soft contact lenses incorporating aberration-controlled designs may offer some control over the primary aberrations associated with keratoconus, such as coma and spherical aberration. For moderate-to-advanced keratoconus, the primary modalities for vision correction are rigid gas permeable contact lenses and scleral lenses. These lenses serve as the cornerstone of treatment. Their principal advantage is creating a tear pool between the lens and the cornea, effectively neutralizing ocular aberrations linked to keratoconus ectasia. Consequently, they have the potential to provide nearly excellent corrected vision [14,15].
Weed et al [16] conducted a prospective longitudinal clinical study in 200 eyes of patients with keratoconus, 1% of patients used soft contact lens, 6.4% used hybrid lenses, and 2% used scleral lens. In this study, keratoconic subjects achieved very good Snellen visual acuity (97%, > or =6/9) and wore rigid contact lenses (90.6%) for more than 12 hours per day (81%), seven days a week (91%). Most corneas (71%) showed evidence of corneal staining; however, only a small proportion of participants reported significant issues with discomfort (18%), hyperemia (16%), or lens dislodging (4%). The primary reason (79%) for undergoing penetrating keratoplasty (PKP) was poor visual acuity. This procedure is typically performed later in life, about ten years after diagnosis. Four percent of eyes progressed to PKP during the study period. Postoperatively, only 9.5% of eyes did not require any form of visual correction.
Rashid et al [17] examined records of 254 keratoconus patients. 75% of the patients were between the ages of 6 and 25, with a mean age of 20.97 ± 11.13 years (range, 6-84 years). Males made up the majority (59.8%). The most frequent complaints were contact lens intolerance (11.8%), blurred vision (50%), poor visual acuity with spectacles (33.5%), and others (unspecified). The majority of cases were classified as severe (71%), moderate (22.9%), and mild (6.2%). The average best-corrected visual acuity (BCVA) was 6.11 ± 0.23. An optical correction was given in 98% of the cases; 34.6% of those cases involved glasses, 31.1% involved gas-permeable lenses, and the remaining cases involved both. In 16.5% of cases, a keratoplasty referral was justified.
Conclusion
In the past, keratoconus was a bilateral, asymmetric ocular disease and was thought to be noninflammatory, but in the present, it has been linked to ocular inflammation. It usually begins to manifest in the second and third decades of life and continues until the end of the fourth decade. The illness impacts both sexes and all ethnicities. This case demonstrates that Munson’s sign in keratoconus patients is associated with a V-shaped protrusion of the lower eyelid upon downward gaze. RGP contact lenses or scleral lenses can well manage this clinical condition.
References
- Gordon-Shaag A, Millodot M, Shneor E. The epidemiology and etiology of keratoconus. Epidemiology. 2012;70(1):7-15. The epidemiology and etiology of keratoconus.
- Hawkes E, Nanavaty MA. Eye rubbing and keratoconus: a literature review. Int J Kerat Ect Cor Dis. 2015;3(2):118-121. Eye rubbing and keratoconus: a literature review
- Santodomingo-Rubido J, Carracedo G, Suzaki A, Villa-Collar C, Vincent SJ, Wolffsohn JS. Keratoconus: An updated review. Cont Lens Anterior Eye. 2022;45(3):101559. doi.10.1016/j.clae.2021.101559. PubMed | Crossref | Google Scholar
- Borchert GA, Tan J. Munson’s Sign in Keratoconus. N Engl J Med. 2023;389(10):939. doi.10.1056/NEJMicm2300297 PubMed | Crossref | Google Scholar
- Martínez-Abad A, Piñero DP. New perspectives on the detection and progression of keratoconus. J Cataract Refract Surg. 2017;43(9):1213-1227. doi.10.1016/j.jcrs.2017.07.021 PubMed | Crossref | Google Scholar
- Loukovitis E, Kozeis N, Gatzioufas Z, et al. The proteins of keratoconus: A literature review exploring their contribution to the pathophysiology of the disease. Adv Ther. 2019;36(9):2205-2222. doi.10.1007/s12325-019-01026-0 PubMed | Crossref | Google Scholar
- Hwang S, Lim DH, Chung TY. Prevalence and incidence of keratoconus in South Korea: A nationwide population-based study. Am J Ophthalmol. 2018;192:56-64. doi.10.1016/j.ajo.2018.04.027PubMed
- Khaled ML, Helwa I, Drewry M, et al. Molecular and histopathological changes associated with keratoconus. Biomed Res Int. 2017;2017:7803029. doi.10.1155/2017/7803029 PubMed | Crossref | Google Scholar
- Santodomingo-Rubido J, Carracedo G, Suzaki A, Villa-Collar C, Vincent SJ, Wolffsohn JS. Keratoconus: An updated review. Cont Lens Anterior Eye. 2022;45(3):101559. doi.10.1016/j.clae.2021.101559 PubMed | Crossref | Google Scholar
- Rabinowitz YS. Keratoconus. Surv Ophthalmol. 1998;42(4):297-319. doi.10.1016/s0039-6257(97)00119-7 PubMed | Crossref | Google Scholar
- Brookes NH, Loh IP, Clover GM, Poole CA, Sherwin T. Involvement of corneal nerves in the progression of keratoconus. Exp Eye Res. 2003;77(4):515-524. doi.10.1016/s0014-4835(03)00148-9 PubMed | Crossref | Google Scholar
- Gordon-Shaag A, Millodot M, Shneor E, Liu Y. The genetic and environmental factors for keratoconus. Biomed Res Int. 2015;2015:795738 doi.10.1155/2015/795738 PubMed | Crossref
- Millodot M, Shneor E, Albou S, Atlani E, Gordon-Shaag A. Prevalence and associated factors of keratoconus in Jerusalem: a cross-sectional study. Ophthalmic Epidemiol. 2011;18(2):91-97. doi.10.3109/09286586.2011.560747 PubMed | Crossref | Google Scholar
- McMonnies CW. Eye rubbing type and prevalence including contact lens ‘removal-relief’ rubbing. Clin Exp Optom. 2016;99(4):366-372. doi.10.1111/cxo.12343 PubMed | Crossref | Google Scholar
- Lim L, Lim EWL. Current perspectives in the management of keratoconus with contact lenses. Eye (Lond). 2020;34(12):2175-2196. doi.10.1038/s41433-020-1065-z PubMed | Crossref | Google Scholar
- Weed KH, Macewen CJ, McGhee CN. The Dundee University Scottish Keratoconus Study II: A prospective study of optical and surgical correction. Ophthalmic Physiol Opt. 2007;27(6):561-567. doi.10.1111/j.1475-1313.2007.00524.x PubMed | Crossref | Google Scholar
- Rashid ZA, Millodot M, Evans KS. Characteristics of keratoconic patients attending a specialist contact lens clinic in Kenya. Middle East Afr J Ophthalmol. 2016;23(4):283-287. doi.10.4103/0974-9233.194074
PubMed | Crossref | Google Scholar
Acknowledgments
Not applicable
Funding
Not applicable
Author Information
Corresponding Author:
Raziya Begum Sheikh
Independent Researcher, Department of Content
medtigo India Pvt Ltd, Pune, India
Email: raziya.pharma@gmail.com
Co-Author:
T Sindhoori
Independent Researcher, Department of Content
medtigo India Pvt Ltd, Pune, India
Authors Contributions
All patient-related data were collected by Dr. Sindhoori. Raziya Begum Sheikh contributed to the writing of the manuscript, including the original draft preparation and subsequent review and editing to refine the final version.
Informed Consent
Not applicable
Conflict of Interest Statement
This case report is based on a clinical case published in the “Cases” section of medtigo.com. The authors declare no conflicts of interest related to this publication.
Guarantor
Not applicable
DOI
Cite this Article
Begum RS, T Sindhoori. A 32-Year-Old Female with Sudden Onset of Vision Loss. medtigo J Med. 2024;2(1):e3062211. doi:10.63096/medtigo3062211 Crossref









